Abstract
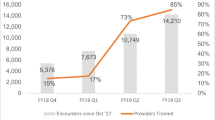
This clinical demonstration project used facilitation to implement VA Video to Home (VTH) to deliver evidence-based psychotherapies to underserved rural Veterans, to increase access to mental health care. Participants were Veterans seeking mental health treatment at “Sonny” Montgomery Veterans Affairs Medical Center in Jackson, MS, and/or its six community-based outpatient clinics. Measures included patient encounter and demographic data, patient and provider interviews, reach, effectiveness, adoption, implementation, and maintenance (RE-AIM) factors, measures of fidelity to manualized evidence-based psychotherapies (EBPs), and qualitative interviews. The project was deemed feasible; 93 (67 men, 26 women, including 77 rural, 16 urban) patients received weekly EBPs via VTH. Nearly half were Black (n = 46), 36 of whom (78.3%) were also rural. Fifty-three (48.4%) were Operation Enduring Freedom/Operation Iraqi Freedom Veterans. Ages varied widely, from 20 to 79 years. Primary diagnoses included posttraumatic stress disorder (41), depressive disorders (22), anxiety disorders (nine), insomnia (eight), chronic pain (eight), and substance use disorder (five). Fifteen clinicians were trained to deliver eight EBPs via VTH. Growth in number of Veterans treated by telehealth was 10.12 times and mental health visits were 7.34 times greater than the national annual average of growth for telehealth at VHA facilities. Illustrative examples and qualitative data from both patients and providers suggested overall satisfaction with VTH. This demonstrates the benefits of VTH for increasing access to mental health treatment for rural patients and advantages of an implementation facilitation strategy using an external facilitator. Continuing research should clarify whether certain patients are more likely to participate than others and whether certain EBPs are more easily delivered with VTH than others.


Similar content being viewed by others
References
Acierno, R., Gros, D. F., Ruggiero, I. J., Hernandez-Tejada, M. A., Knapp, R. G., Lejuez, C. W., et al. (2016). Behavioral activation and therapeutic exposure for posttraumatic stress disorder: a noninferiority trial of treatment delivered in person versus home-based telehealth. Depression and Anxiety, 33(5), 415–423.
Acierno, R., Knapp, R., Tuerk, P., Gilmore, A. K., Lejuez, C., Ruggiero, K., et al. (2017). A non-inferiority trial of prolonged exposure for posttraumatic stress disorder: in person versus home-based telehealth. Behaviour Research and Therapy, 89, 57–65.
Buzza, C., Ono, S. S., Turvey, C., Wittrock, S., Noble, M., Reddy, G., et al. (2011). Distance is relative: unpacking a principal barrier in rural healthcare. Journal of General Internal Medicine, 26(Supp l2), 648–654.
Carroll, K. M., Ball, S. A., Martino, S., Nich, C., Babuscio, T. A., Nuro, K. F., et al. (2008). Computer-assisted delivery of cognitive-behavioral therapy for addiction: a randomized trial of CBT4CBT. The American Journal of Psychiatry, 165(7), 881–888.
Chard, K. M., Schumm, J. A., Owens, G. P., & Cottingham, S. M. (2010). A comparison of OEF and OIF Veterans and Vietnam Veterans receiving cognitive processing therapy. Journal of Traumatic Stress, 23(1), 25–32.
Craske, M. G., Rose, R. D., Lang, A. J., Welch, S. S., Campbell-Sills, L., Sullivan, G., et al. (2009). Computer assisted delivery of cognitive behavior therapy for anxiety disorders in primary care settings. Depression and Anxiety, 26, 235–242.
Cucciare, M. A., Curran, G. M., Craske, M. G., Abraham, T., McCarthur, M. B., Marchant-Miros, K., et al. (2016). Assessing fidelity of cognitive behavioral therapy in rural VA clinics: design of a randomized implementation effectiveness (hybrid type III) trial. Implementation Science, 11(1), 65.
Cully, J. A., Jameson, J. P., Phillips, L. L., Kunik, M. E., & Fortney, J. A. (2010). Use of psychotherapy by rural and urban Veterans. Journal of Rural Health, 26(3), 225–233.
Davis, J. J., Walter, K. H., Chard, K. M., Parkinson, R. B., & Houston, W. S. (2013). Treatment adherence in cognitive processing therapy for combat-related PTSD with history of mild TBI. Rehabilitation Psychology, 58(1), 36–42.
Friedman, S. A., Phibbs, C. S., Schmitt, S. K., Hayes, P. M., Herrera, L., & Frayne, S. M. (2011). New women Veterans in the VHA: a longitudinal profile. Womens Health Issues, 21(4 suppl), S103–S111.
Gilmore, A. K., Davis, M. T., Grubaugh, A., Resnick, H., Birks, A., Denier, C., et al. (2016). “Do you expect me to receive PTSD care in a setting where most of the other patients remind me of the perpetrator?”: home-based telemedicine to address barriers to care unique to military sexual trauma and Veterans affairs hospitals. Contemporary Clinical Trials, 48, 59–64.
Gros, D. F., Veronee, K., Strachan, M., Ruggiero, K. J., & Acierno, R. (2011a). Managing suicidality in home-based telehealth. Journal of Telemedicine and Telecare, 17(6), 332–335.
Gros, D. F., Yoder, M., Tuerk, P. W., Lozano, B. E., & Acierno, R. (2011b). Exposure therapy for PTSD delivered to Veterans via telehealth: predictors of treatment completion and outcome and comparison to treatment delivered in person. Behavior Therapy, 42(2), 276–283.
Gros, D. F., Morland, L. A., Greene, C. J., Acierno, R., Strachan, M., Egede, L. E., et al. (2013). Delivery of evidence-based psychotherapy via video telehealth. Journal of Psychopathology and Behavioral Assessment, 35(4), 506–521.
Gros, D. F., Lancaster, C. L., López, C. M., & Acierno, R. (2016). Treatment satisfaction of home-based telehealth versus in-person delivery of prolonged exposure for combat-related PTSD in Veterans. Journal of Telemedicine and Telecare. [Epub ahead of print, September 26, 2016]. https://doi.org/10.1177/1357633X16671096.
Harvey, G., & Kitson, A. (2015). Implementing evidence-based practice in healthcare: a facilitation guide. London: Routledge, Taylor & Francis Group.
Hilty, D. M., Ferrer, D. C., Parish, M. B., Johnston, B., Callahan, E. J., & Yellowlees, P. M. (2013). The effectiveness of telemental health: a 2013 review. Telemedicine and e-Health, 19(6), 444–454.
Hilty, D. M., Chan, S., Hwang, T., Wong, A., & Bauer, A. M. (2017). Advances in mobile mental health: opportunities and implementation for the spectrum of e-mental health services. mHealth, 3(34), 3–18.
Hsieh, H. F., & Shannon, S. E. (2005). Three approaches to qualitative content analysis. Qualitative Health Research, 15(9), 1277–1288.
Jeffreys, M. D., Reinfeld, C., Nair, P. V., Garcia, H. A., Mata-Galan, E., & Rentz, T. O. (2014). Evaluating treatment of posttraumatic stress disorder with cognitive processing therapy and prolonged exposure therapy in a VHA specialty clinic. Journal of Anxiety Disorders, 28(1), 108–114.
Karlin, B. E., & Cross, G. (2014). From the laboratory to the therapy room. National dissemination and implementation of evidence-based psychotherapies in the U.S. Department of Veterans Affairs health care system. American Psychologist, 69(11), 19–33.
Kirchner, J. E., Ritchie, M. J., Pitcock, J. A., Parker, L. E., Curran, G. M., & Fortney, J. C. (2014). Outcomes of a partnered facilitation strategy to implement primary care mental health. Journal of General Internal Medicine, 29(Suppl 4), S904–S912.
Lindsay, J. A., Kauth, M. R., Hudson, S., Martin, L. A., Ramsey, D. J., Daily, L., et al. (2015). Implementation of video telehealth to improve access to evidence-based psychotherapy for posttraumatic stress disorder. Telemedicine and e-Health, 21, 6. https://doi.org/10.1089/tmj.2014.0114.
Mott, J. M., Grubbs, K. M., Sansgiry, S., Fortney, J. C., & Cully, J. A. (2014a). Psychotherapy utilization among rural and urban Veterans from 2007-2010. The Journal of Rural Health, 31, 235–243.
Mott, J. M., Mondragon, S., Hundt, N. E., Beason-Smith, M., Grady, R. H., & Teng, E. J. (2014b). Characteristics of US Veterans who begin and complete prolonged exposure and cognitive processing therapy for PTSD. Journal of Traumatic Stress, 27(3), 265–273.
Office of Health Policy, Office of the Assistant Secretary for Planning and Evaluations. (2016). Report to Congress: e-health and telemedicine. Washington, DC: Department of Health and Human Services.
Ritchie, M. J., Dollar, K. M., Miller, C. J., Oliver, K. A., Smith, J. L., Lindsay, J. A., et al. (2017). Using implementation facilitation to improve care in the Veterans Health Administration (version 2). Veterans Health Administration, Quality Enhancement Research Initiative (QUERI) for Team-Based Behavioral Health. Available at: https://www.queri.research.va.gov/tools/implementation/Facilitation-Manual.pdf.
Schnurr, P. P., Friedman, M. J., Engel, C. C., Foa, E. B., Shea, M. T., Chow, B. K., et al. (2007). Cognitive behavioral therapy for posttraumatic stress disorder in women. Journal of the American Medical Association, 297(8), 820–830.
Strachan, M., Gros, D. F., Ruggiero, K. J., Lejuez, C. W., & Acierno, R. (2012). An integrated approach to delivering exposure-based treatment for symptoms of PTSD and depression in OIF/OEF Veterans: preliminary findings. Behavior Therapy, 43(3), 560–569.
Tuckson, R. V., Edmunds, M., & Hodgkins, M. L. (2017). Special report: telehealth. New England Journal of Medicine, 377(16), 1585–1592.
U. S. Department of Health and Human Services. (2003). Achieving the promise: transforming mental health care in America. Washington, D.C.
Virginia Tech College of Agriculture and Life Sciences. (n.d.). Reach effectiveness adoption implementation (RE-AIM). RE-AIM.org. http://re-aim.org/. Accessed 6 June 2017.
Whealin, J. M., Seibert-Hatalsky, A., Howell, J. W., & Tsai, J. (2015). E-mental health preferences of Veterans with and without probable posttraumatic stress disorder. Journal of Rehabilitation Research & Development, 52(6), 725–738.
Wykes, T., & Brown, M. (2016). Over promised, over-sold and underperforming?—e-health in mental health (editorial). Journal of Mental Health, 25(1), 1–4.
Yuen, E. K., Gros, D. F., Price, M., Zeigler, S., Tuerk, P. W., Foa, E. B., et al. (2015). Randomized controlled trial of home-based telehealth versus in-person prolonged exposure for combat-related PTSD in veterans: preliminary results. Journal of Clinical Psychology, 71(6), 500–512.
Acknowledgments
The authors would like to thank Mona Ritchie, PhD, MSW, and JoAnn Kirchner, MD, for implementation facilitation training and mentoring; and Rhonda Johnson, PhD, BC-FNP, BC-ANP, and Mr. John Peters for assistance and expertise in providing telehealth services.
Funding
This work is the result of a grant from the VA Office of Rural Health, N16-FY15Q1-S1-P01392 (4440), to Jan Lindsay, support by the VA South Central Mental Illness Research, Education and Clinical Center, and use of resources and facilities at the Houston VA HSR&D Center for Innovations in Quality, Effectiveness and Safety (CIN13-413). The opinions expressed are those of the authors and not necessarily those of the Department of Veterans Affairs, the U.S. Government or Baylor College of Medicine.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Lindsay, J.A., Hudson, S., Martin, L. et al. Implementing Video to Home to Increase Access to Evidence-Based Psychotherapy for Rural Veterans. J. technol. behav. sci. 2, 140–148 (2017). https://doi.org/10.1007/s41347-017-0032-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41347-017-0032-4