Abstract
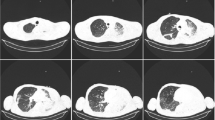
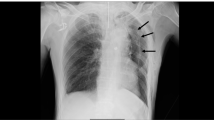
Two patients with refractory hypoxemia due to unilateral lung atelectasis were treated with differential lung ventilation (DLV) through a Robertshaw-type, double-lumen tracheostomy tube. DLV was applied using two non-synchronized ventilators and maintained for 6 and 3 days, respectively. Ventilator settings were chosen in accord to the clinical, laboratory and chest X-rays results. Particularly, tidal volume and PEEP were set to avoid excessively high alveolar pressure and to obtain the highest possible value of compliance. We investigated the mechanical properties of the two lungs separately by measuring airway pressure and compliance of each lung before the beginning of DLV and at 0, 5, 24, and 48 h after. Initially we observed in both patients very low values of compliance (7–9 cm H2O/I) and a significant level of PEEPi (12–8 cm H2O) of the diseased lung, whereas PEEPi in the healthy lung was negligible. The clinical improvement was assessed by sequential chest X-rays and by significant improvement of arterial blood gas and PaO2/FiO2 ratios and was associated with a progressive increase of compliance (24–22 cm H2O/I) and by a fall of PEEPi levels (5–4 cm H2O) of the diseased lung. We also observed an improvement of S\(\bar v\)O2, O2AVI, PVRI and\(\dot Q\)va/\(\dot Q\)t values (Case 1). The tracheostomy tube used to apply DLV was very reliable, allowing easy nursing care and selective bronchial aspirations. We conclude that DLV is a very useful technique in unilateral lung pathology, and it can be a life saving procedure in selected patients, by supplying volume and PEEP more efficiently to the affected lung.
Article PDF
Similar content being viewed by others
References
Katz JA, Ozanne GM, Zinne SE, Fairley HB (1981) Time course and mechanism of lung-volume increase with PEEP in acute pulmonary failure. Anesthesiology 54:9–16
Baehrendtz S, Hedenstierna G (1984) Differential ventilation and selective positive endexpiratory pressure: effects on patient with acute bilateral lung disease. Anesthestology 61:511–517
Hedenstierna G, McCarty G, Bergstrom M (1976) Airway closure during mechanical ventilation. Anesthesiology 44:114–123
McIntyre RW, Laws AK, Ramachandran PR (1969) Positive expiratory pressure plateau: improved gas exchange during mechanical ventilation. Can Anaesth Soc J 16:477–486
Falke KJ, Pontoppidan H, Kumar S, Leigh DE, Gaffn B, Laver MB (1972) Ventilation with end-expiratory pressure in acute lung disease. J Clin Invest 51:2315–2323
Baehrendtz S, Santesson J, Bindslev I, Hedensterna G, Matell G (1983) Differential ventilation in acute bilateral lung disease. Influence on gas exchange and central haemodynamics. Acta Anaesthesiol Scand 27:270–277
Kumar A, Pontoppidan H, Falke K, Wilson R, Laver MB (1973) Pulmonary barotrauma during mecharical ventilation. Crit Care Med 1:181–186
West JB, Dallery CT, Naimark A (1964) Distribution of blood flow in isolated lung: relation to vascular and alveolar pressures. J Appl Physiol 19:713–724
Geiger K (1983) Differential lung ventilation. In: European advances in intensive care medicine. Anesthesiol Clin 21:83–96
Siegel JH, Stoklosa JC, Borg U, Wiles CE (1985) Quantification of asymmetric lung pathophysiology as a guide to the use of simultaneous independent lung ventilation in posttraumatic and septic adult respiratory distress syndrome. Am Surg 202:425–437
Gottfried SB, Higgs BD, Rossi A, Carb F, Meugeot PM, Calverly PMA, Zocchi L, Milic-Emili J (1985) Interrupter technique for measurement of respiratory mechanics in anesthetized humans. J Appl Physiol 59:647–652
Gottfried SB, Rossi A, Higgs BD, Calverley PMA, Zocchi L, Bozic C, Milic-Emili J (1985) Noninvasive determination of respiratory system mechanics during mechanical ventilation for acute respiratory failure. Am Rev Respir Dis 131:414–420
Carlon GC, Ray C, Klein R, Goldiner PI, Miodownik S (1978) Criteria for selective positive end-expiratory pressure and independent synchronized ventilation of each lung. Chest 74:501–507
Kanarek DJ, Shannon DC (1975) Adverse effect of positive end expiratory pressure on pulmonary perfusion and arterial oxygenation. Am Rev Respir Dis 112:457
Kvetan V, Carlon GC, Howland WS (1982) Acute pulmonary failure in asymmetric lung disease: approach to management. Crit Care Med 10:114
Carlon GC, Kahn R, Howland WS, Baron R, Romaker J (1978) Acute life threatening ventilation-perfusion inequality: an indication for independent lung ventilation. Crit Care Med 6:380–383
Zandstra DF, Stoutenbeek ChP, Bams JL (1989) Monitoring lung mechanics and airway pressures during differential lung ventilation (DLV) with emphasis on weaning from DLV. Intensive Care Med 15:458–463
Hillman KM, Barber JD (1980) Asynchronous independent lung ventilation (AILV). Crit Care Med 8:390–395
Hurst JM, De Haven CB, Bronson RD (1985) Comparison of conventional mechanical ventilation and synchronous independent lung ventilation (SILV) in the treatment of unilateral lung injury. J Trauma 25:766–768
Crimi G, Conti G, Candiani A, Antonelli M, Bufi M, Mattia C, Gasparetto A (1987) Clinical use of continous positive airway pressure in the treatment of unilateral acute lung injury. Intensive Care Med 13:416–418
Powner DJ, Eross B, Grenvik A (1977) Differential lung ventilation with PEEP in the treatment of unilateral pneumonia. Crit Care Med 5:170–172
Rivara D, Bourgain JL, Rieuf P, Horf A, Lemaire F (1979) Differential ventilation in unilateral lung disease: effects on respiratory mechanics and gas exchange. Intensive Care Med 5:189–191
Glass DD, Tonnesen AS, Gabel JC, Arens JF (1976) Therapy of unilateral pulmonary insufficiency with a double lumen endotracheal tube. Crit Care Med 4:323
Feeley TW, Keating D, Nishimura T (1988) Independent lung ventilation using high-frequency ventilation in the management of a bronchopleural fistula. Anesthesiology 69:420–422
Wendt M, Hachenberg T, Winde G, Lawin P (1989) Dffferential ventilation with low-flow CPAP and CPPV in the treatment of unilateral chest trauma. Intensive Care Med 15:209–211
Zandstra DF, Stoutenbeek CP (1987) Treatment of massive unilateral pulmonary embolism by differential lung ventilation. Intensive Care Med 13:422–424
Frostell C, Blomqvist H, Nilsson JA, Grenrot C, Baehrendtz S, Hedenstierna G (1984) Differential ventilation with selective Peep in bilateral lung disease. Intensive Care Med 10:265–267
Rossi A, Gottfried SB, Zocchi L, Higgs BD, Lennox S, Calverley PMA, Begin P, Grassino A, Milic-Emili J (1985) Measurement of static compliance of the total respiratory system in patients with acute respiratory failure during mechanical ventilation. Am Rev Respir Dis 131:672–677
Wright PE, Marini JJ, Bernard GR (1989) In vitro versus in vivo comparison of endotracheal tube airflow resistance. Am Rev Respir Dis 140:10–16
Rossi A, Santos C, Roca J, Torres A, Felez MA, Rodriguez Roisin R (1992) Effects of intrinsic PEEP on ventilation-perfusion mismatching in mechnically ventilated patients with acute or chronic airway obstruction. Am Rev Respir Dis 145:A76
Muneyuki M, Konishi K, Horiguchi R, Tsujimoto S, Saito M, Sakakura S, Konishi A (1983) Effects of alternating lung ventilation on cardiopulmonary functions in dogs. Anesthesiology, 58: 353–356
Baehrendtz S, Hedenstierna G (1984) Differential ventilation and selective endexpiratory pressure: effects on patients with acute bilateral lung disease. Anesthesiology 61:511–517
Rommelsheim K (1985) Ein neuer doppellumiger Tracheostomietube zur Langzeitanwendung. Anaesth. Intensivther Notfallmed 20:342–344
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Alberti, A., Valenti, S., Gallo, F. et al. Differential lung ventilation with a double-lumen tracheostomy tube in unilateral refractory atelectasis. Intensive Care Med 18, 479–484 (1992). https://doi.org/10.1007/BF01708585
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01708585