Summary
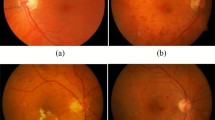
The three-dimensional ultrastructure of glomerular basement membrane (GBM) in streptozotocin (STZ)-induced diabetic rats was examined by quickfreezing and deep-etching method. In three layers of the GBM of control rats, the outer and inner layers were formed by files of perpendicular fibrils, which connected the epithelial or endothelial cell surfaces with meshwork structures of the middle layer. In the diabetic rats, the inner layer was diffusely enlarged and the meshwork structure of the middle layer became markedly irregular due to the rupture of fine fibrils and thickening of material adherent to the fibrils. These ultrastructural changes correspond to those of subendothelial oedema, lamellation of lamina densa and fluffy material in the GBM, as revealed on conventional ultra-thin sections. It is suggested that the initial morphological change of STZ-induced diabetic nephropathy is disruption of matrix fibrils in the GBM, seemingly indicating a disturbance of size and/or charge barriers.
Similar content being viewed by others
References
Anderson S, Rennke HG, Garcia DL, Brenner BM (1989) Short and long term effects on antihypertensive therapy in the diabetic rat. Kidney Int 36: 526–536
Boushey HA, Warnock DG, Smith LH (1986) The pathogenesis and prevention of diabetic nephropathy. West J Med 145: 222–227
Chakrabarti S, Ma N, Sima AAF (1989) Reduced number of anionic sites is associated with glomerular basement membrane thickening in the diabetic BB-rat. Diabetologia 32: 826–828
Chakrabarti S, Ma N, Sima AAF (1991) Anionic sites in diabetic basement membranes and their possible role in diffusion barrier abnormalities in the BB-rat. Diabetologia 34: 301–306
Chavers BM, Bilous RW, Ellis EN, Steffes MW, Mauer SM (1989) Glomerular lesions and urinary albumin excretion in type I diabetes without overt proteinuria. N Engl J Med 320: 966–970
Churg J, Sobin LH (1982) Diabetic glomerulosclerosis. In: Renal disease classification and atlas of glomerular disease. Igaku-Shoin, Tokyo, pp 226–239
Cooper ME, Allen TJ, Macmillan, P, Bach L, Jermus G, Doyle AE (1988) Genetic hypertension accelerates nephropathy in the streptozotocin diabetic rat. Am J Hypertens 1: 5–10
Deckert T, Feldt-Rasmussen B, Djurup R, Deckert M (1988) Glomerular size and charge selectivity in insulin-dependent diabetes mellitus. Kidney Int 33: 100–106
Friedman S, Jones III HW, Golbetz HV, Lee JA, Little HL, Myers BD (1983) Mechanisms of proteinuria in diabetic nephropathy II. A study of the size-selective glomerular filtration barrier. Diabetes 32: 40–46
Heuser JE, Kirschner MW (1980) Filament organization revealed in platinum replicas of freeze-dried cytoskeletons. J Cell Biol 86: 212–234
Hirose K, Østerby R, Nozawa M, Gundersen HJG (1982) Development of glomerular lesions in experimental long-term diabetes in the rat. Kidney Int 21: 689–695
Inomata S, Oosawa Y, Itoh M, Inoue M, Masamune O (1987) Analysis of urinary proteins in diabetes mellitus—with reference to the relationship between microalbuminuria and diabetic renal lesions. J Jpn Diabetes Soc 30: 429–435
Koda Y, Maruyama Y, Ogino S, Hayashi H, Nishi S, Saito T, Ueno H, Arakawa M (1991) Early mesangiolysis and monocyte influx observed in diabetic glomerulosclerosis: relation to nodule formation. Jpn J Nephrol 33: 33–42
Mauer SM, Steffes MW, Ellis EN, Sutherland DER, Brown DM, Goetz FC (1984) Structural-functional relationships in diabetic nephropathy. J Clin Invest 74: 1143–1155
Mogensen CE (1987) Microalbuminuria as a predictor of clinical diabetic nephropathy. Kidney Int 31: 673–689
Mogensen CE, Christensen CK, Vittinghus E (1983) The stages in diabetic renal disease. With emphasis on the stage of incipient diabetic nephropathy. Diabetes 32: 64–78
Myers BD (1990) Pathophysiology of proteinuria in diabetic glomerular disease. J Hypertens 8: S 41–46
Nakamura Y, Myers BD (1988) Charge selectivity of proteinuria in diabetic glomerulopathy. Diabetes 37: 1202–1211
Naramoto A, Ohno S, Itoh N, Shibata N, Nakazawa K, Takami H, Duan H-J, Kasahara H, Shigematsu H (1991a) Ultrastructure of matriceal changes in chronic phase of Masugi nephritis by quick-freezing and deep-etching method. Virchows Arch [A] 418: 51–59
Naramoto A, Ohno S, Nakazawa K, Takami H, Itoh N, Shigematsu H (1991b) Three-dimensional ultrastructure of glomerular injury in serum sickness nephritis using the quick-freezing and deep-etching method. Virchows Arch [A] 418: 185–192
Ohno S (1985) Immunocytochemical study on the cytoplasmic side of cell membranes infected with vesicular stomatitis virus by quick-freezing and deep-etching replica method. Histochemistry 82: 565–575
Østerby R (1988) Glomerular abnormalities in early and late stages of experimental diabetes: models for diabetic nephropathy? Frontiers in diabetes research. Lessons from animal diabetes. John Libbey, London, pp 522–527
Østerby R, Brekke IB, Gunderson HJG, Jorgensen HE, Lokkegaard H, Mogensen CE, Nyberg G, Parving HH, Westberg G (1984) Quantitative studies of glomerular ultrastructure in human and experimental diabetes. Appl Pathol 2: 205–211
Østerby R, Parving HH, Hommel E, Jorgensen HE, Lokkegaard H (1990) Glomerular structure and function in diabetic nephropathy. Early to advanced stages. Diabetes 39: 1057–1063
Rasch R (1979) Prevention of diabetic glomerulopathy in streptozotocin diabetic rats by insulin treatment. Glomerular basement membrane thickness. Diabetologia 16: 319–324
Rosenstock J, Raskin P (1986) Early diabetic nephropathy: assessment and potential therapeutic interventions. Diabetes Care 9: 529–545
Saito Y, Kida H, Takeda S, Yoshimura M, Yokoyama H, Koshino Y, Hattori N (1988) Mesangiolysis in diabetic glomeruli: its role in the formation of nodular lesions. Kidney Int 34: 389–396
Schuler JW, Kalichaman D, Hoedemaeker J, Molenaar I (1978) The use of polyethyleneimine for demonstration of anionic sites in basement membranes and collagen fibrils. J Histochem Cytochem 26: 688–689
Shimomura H, Spiro RG (1987) Studies on macromolecular component of human glomerular basement membrane and alterations in diabetes. Decreased levels of heparan sulfate proteoglycan and laminin. Diabetes 36: 374–381
Steffes MW, Østerby R, Chavers B, Mauer SM (1989) Perspectives in diabetes. Mesangial expansion as a central mechanism for loss of kidney function in diabetic patients. Diabetes 38: 1077–1081
Takami H, Naramoto A, Shigematsu H, Ohno S (1991) Ultrastructure of glomerular basement membrane by quick-freeze and deep-etch methods. Kidney Int 39: 659–664
Templeton DM (1989) Retention of glomerular basement membrane-proteoglycans accompanying loss of anionic site staining in experimental diabetes. Lab Invest 61: 202–211
Vehaskari VM, Root ER, Germuth FG, Robson AM (1982) Glomerular charge and urinary protein excretion: effects of systemic and intrarenal polycation infusion in the rat. Kidney Int 22: 127–135
Viberti GC, Wiseman MJ (1986) The kidney in diabetes: significance of the early abnormalities. Clin Endocrinol Metab 15: 753–782
Weil III R, Nozawa M, Koss M, Weber C, Reemts K, Mcintosh R (1976) The kidney in streptozotocin diabetic rats Arch Pathol Lab Med 100: 37–49
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Moriya, T., Ohno, S., Nakazawa, K. et al. Ultrastructural study of glomerular basement membrane in diabetic rats by quick-freezing and deep-etching method. Virchows Archiv B Cell Pathol 64, 107–114 (1993). https://doi.org/10.1007/BF02915102
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF02915102