Abstract
Objective
To evaluate the feasibility of implementing a program of controlled non-heart beating organ donation, in patients undergoing the withdrawal of intensive care treatment.
Design and setting
Prospective observational study. Medical and Surgical ICUs in a tertiary university hospital.
Patients
Consecutive patients younger than 70 years dying in the ICU after treatment withdrawal for dire neurological prognosis.
Measurements and results
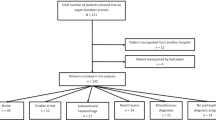
We analyzed prospectively collected data from the ICU clinical information system. Seventy-three of 516 ICU deaths (13%) were identified, equally distributed among traumatic, stroke, and anoxic brain injury. The management and the course in these three diagnostic categories were similar. All patients underwent withdrawal of mechanical ventilation and half were extubated. Median time to death was of 4.8 h (IQR 1.4–11.5). In 70% of cases the patient received analgesia and 30% sedation. Such treatment was not related to earlier death. Hypotension was observed in 50% of patients during the 30 min preceding cardiac death.
Conclusions
With our current management of terminal patients controlled non-heart beating organ procedure may be difficult due to the duration and variability of the dying process. This observation suggests that we can perform better by evaluating this process moreclosely.

Similar content being viewed by others
References
Daar AS (2004) Non-heart-beating donation: ten evidence-based ethical recommendations. Transplant Proc 36:1885–1887
Kootstra G (1995) Statement on non-heart-beating donor programs. Transplant Proc 27:2965
Truog RD, Robinson WM (2003) Role of brain death and the dead-donor rule in the ethics of organ transplantation. Crit Care Med 31:2391–2396
Brook NR, Waller JR, Richardson AC, Andrew Bradley J, Andrews PA, Koffman G, Gok M, Talbot D, Nicholson ML (2004) A report on the activity and clinical outcomes of renal non-heart beating donor transplantation in the United Kingdom. Clin Transpl 18:627–633
Bell MDD (2005) Non-heartbeating organ donation: clinical process and fundamental issues. Br J Anaesth 94:474–478
Sudhindran S, Pettigrew GJ, Drain A, Shrotri M, Watson CJ, Jamieson NV, Bradley JA (2003) Outcome of transplantation using kidneys from controlled (Maastricht category 3) non-heart-beating donors. Clin Transpl 17:93–100
Revelly JP, Imperatori L, Maravic P, Schaller MD, Chioléro RL (2005) Are terminally ill patients dying in the ICU suitable for non-heart beating organ donation? Intensive Care Med 31:S156
Vallotton M (2004) Care of patients in the end of life. Medical-ethical guidelines of the Swiss Academy of Medical Sciences. http://www.samw.ch/content/Richtlinien/e_RL_Lebensende.pdf
Sprung CL, Cohen SL, Sjokvist P, Baras M, Bulow HH, Hovilehto S, Ledoux D, Lippert A, Maia P, Phelan D, Schobersberger W, Wennberg E, Woodcock T, Group Ethicus Study (2003) End-of-life practices in European intensive care units: the Ethicus Study. JAMA 290:790–797
Bell MDD (2003) Non-heart beating organ donation: old procurement strategy-new ethical problems. J Med Ethics 29:176–181
Mayer SA, Kossoff SB (1999) Withdrawal of life support in the neurological intensive care unit. Neurology 52:1602–1609
Azoulay E, Pochard F, Kentish-Barnes N, Chevret S, Aboab J, Adrie C, Annane D, Bleichner G, Bollaert PE, Darmon M, Fassier T, Galliot R, Garrouste-Orgeas M, Goulenok C, Goldgran-Toledano D, Hayon J, Jourdain M, Kaidomar M, Laplace C, Larché J, Liotier J, Papazian L, Poisson C, Reignier J, Saidi F, Schlemmer B (2005) Risk of post-traumatic stress symptoms in family members of intensive care unit patients. Am J Respir Crit Care Med 171:987–994
Author information
Authors and Affiliations
Corresponding author
Additional information
René Chioléro and Luca Imperatori are members of the SwissFoundation to Support Organ Donation.
Electronic Supplementary Material
Rights and permissions
About this article
Cite this article
Revelly, JP., Imperatori, L., Maravic, P. et al. Are terminally ill patients dying in the ICU suitable for non-heart beating organ donation?. Intensive Care Med 32, 708–712 (2006). https://doi.org/10.1007/s00134-006-0116-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-006-0116-7