Abstract
Background and aims
Ileo pouch anal anastomosis (IPAA) is the standard restorative procedure for patients with ulcerative colitis and familial adenomatous polyposis, but its pros and cons have not been explored in depth. This study analyzed the long-term complications such as incontinence and sexual dysfunction after IPAA.
Patients and methods
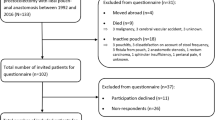
Netherlands Society for Crohn’s disease and Ulcerative Colitis) A questionnaire on complications, sexual dysfunction, and continence was sent to all 137 members of the Netherlands Society for Crohn’s disease and Ulcerative Colitis who had IPAA; the questionnaire was returned by 111. Results of the questionnaire were compared with those of a meta-analysis on pooled incidences of complications after IPAA, as previously performed and reported.
Results
Pelvic sepsis was reported by 15.3% of respondents. The reported incidence of sexual dysfunction (19.8%), passive incontinence (23.4%), and soiling (39.3%) was significantly higher than that in the meta-analysis. Nevertheless, 90% of the population was satisfied with the results of the IPAA.
Conclusion
This study underlines that the operation itself, freeing patients of their disease, provides the major satisfaction and improvement of quality of life, even when patients have pouch-related complications such as sexual dysfunction and some degree of fecal incontinence.
Similar content being viewed by others
Reference
Hueting WE, Buskens E, van der Tweel I, Gooszen HG, van Laarhoven CJHM (2001) Ileo pouch anal anastomosis: meta analysis on results and complications of 44 studies with 9435 patients. Colorectal Dis 3 [Suppl 1]:19
Laarhoven CJ van et al (1999) Ileoneorectal anastomosis: early clinical results of a restorative procedure for ulcerative colitis and familial adenomatous polyposis without formation of an ileoanal pouch. Ann Surg 230:750–757
Andriesse GI et al (2001) Functional results and visceral perception after ileo neo-rectal anastomosis in patients: a pilot study. Gut 48:683–689
Vaizey CJ, Carapeti E, Cahill JA, Kamm MA (1999) Prospective comparison of faecal incontinence grading systems. Gut 44:77–80
Metcalf AM, Dozois RR, Kelly KA (1986) Sexual function in women after proctocolectomy. Ann Surg 204:624–627
Damgaard B, Wettergren A, Kirkegaard P (1995) Social and sexual function following ileal pouch-anal anastomosis. Dis Colon Rectum 38:286–289
Pescatori M, Anastasio G, Bottini C, Mentasti A (1992) New grading and scoring for anal incontinence. Evaluation of 335 patients. Dis Colon Rectum 35:482–487
Jorge JM, Wexner SD (1993) Etiology and management of fecal incontinence. Dis Colon Rectum 36:77–97
Steens J et al (2000) Limited influence of pouch function on quality of life after ileal pouch-anal anastomosis. Hepatogastroenterology 47:746–750
van Duijvendijk P et al (2000) Quality of life after total colectomy with ileorectal anastomosis or proctocolectomy and ileal pouch-anal anastomosis for familial adenomatous polyposis. Br J Surg 87:590–596
Dunker MS, Bemelman WA, Slors JF, van Duijvendijk P, Gouma DJ (2001) Functional outcome, quality of life, body image, and cosmesis in patients after laparoscopic-assisted and conventional restorative proctocolectomy: a comparative study. Dis Colon Rectum 44:1800–1807
Jimmo B, Hyman NH (1998) Is ileal pouch-anal anastomosis really the procedure of choice for patients with ulcerative colitis? Dis Colon Rectum 41:41–5
Acknowledgements
The authors are indebted to Erik Buskens, MD, of the Julius Center for General Practice and Patient-Oriented Research, for his critical comments and suggestions on the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hueting, W.E., Gooszen, H.G. & van Laarhoven, C.J.H.M. Sexual function and continence after ileo pouch anal anastomosis: a comparison between a meta-analysis and a questionnaire survey. Int J Colorectal Dis 19, 215–218 (2004). https://doi.org/10.1007/s00384-003-0543-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-003-0543-7