Abstract
Purpose
There is conflicting data regarding visfatin in gestational diabetes mellitus (GDM). The aim of the present study was to compare serum visfatin levels between patients with GDM and subjects with normal pregnancy and to evaluate its relationship with dietary intake and components of insulin-resistance syndrome.
Methods
Thirty-five patients with GDM (aged 31 ± 0.8 years, BMI = 29.6) and 35 age- and body mass index-matched healthy pregnant women (aged 29 ± 0.7 years, BMI = 28.6) between 24 and 28 weeks of gestation were studied. In addition to anthropometric and dietary intake assessments, measurements of fasting plasma levels of visfatin, glucose, insulin, hemoglobin A1c (HbA1c) and lipid profile were performed for all subjects.
Results
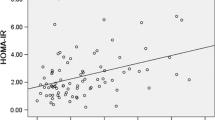
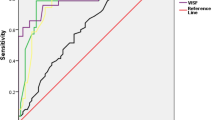
Plasma visfatin levels were significantly lower in pregnant women with GDM compared to healthy subjects (5.29 ± 0.47 vs. 7.76 ± 0.53, p = 0.001). After adjustment for age, maternal gestational age, body mass index, and macronutrients intake, GDM remained the independent predictor of serum visfatin concentrations (β = −1.2, p = 0.001). Serum visfatin levels were significantly correlated with log HbA1c values (r = −0.24, p = 0.03), even after adjustment for age and body mass index (β = −6.45, p = 0.05). No associations between visfatin and other parameters of the insulin-resistance syndrome as well as macronutrient intake were detectable.
Conclusions
Plasma visfatin concentrations are lower in patients with GDM and related to glycemic control reflected by HbA1c. Furthermore, visfatin does not seem to be correlated with dietary intake in pregnant women.
Similar content being viewed by others
References
Metzger BE, Coustan DR (1998) Summary and recommendations of the Fourth International Workshop-Conference on Gestational Diabetes Mellitus. The Organizing Committee. Diabetes Care 21(Suppl 2):B161–B167
Dabelea D, Snell-Bergeon JK, Hartsfield CL et al (2005) Increasing prevalence of gestational diabetes mellitus (GDM) over time and by birth cohort: Kaiser Permanente of Colorado GDM Screening Program. Diabetes Care 28:579–584
Yudkin JS (2003) Adipose tissue, insulin action and vascular disease: inflammatory signals. Int J Obes Relat Metab Disord 27(Suppl 3):S25–S28
Fantuzzi G (2005) Adipose tissue, adipokines, and inflammation. J Allergy Clin Immunol 115:911–919 quiz 920
Fukuhara A, Matsuda M, Nishizawa M et al (2005) Visfatin: a protein secreted by visceral fat that mimics the effects of insulin. Science 307:426–430
Song HK, Lee MH, Kim BK et al (2008) Visfatin: a new player in mesangial cell physiology and diabetic nephropathy. Am J Physiol Renal Physiol 295:F1485–F1494
Haider DG, Schaller G, Kapiotis S et al (2006) The release of the adipocytokine visfatin is regulated by glucose and insulin. Diabetologia 49:1909–1914
Revollo JR, Korner A, Mills KF et al (2007) Nampt/PBEF/Visfatin regulates insulin secretion in beta cells as a systemic NAD biosynthetic enzyme. Cell Metab 6:363–375
Filippatos TD, Randeva HS, Derdemezis CS et al (2010) Visfatin/PBEF and atherosclerosis-related diseases. Curr Vasc Pharmacol 8:12–28
Chan TF, Chen YL, Lee CH et al (2006) Decreased plasma visfatin concentrations in women with gestational diabetes mellitus. J Soc Gynecol Investig 13:364–367
Haider DG, Handisurya A, Storka A et al (2007) Visfatin response to glucose is reduced in women with gestational diabetes mellitus. Diabetes Care 30:1889–1891
Lewandowski KC, Stojanovic N, Press M et al (2007) Elevated serum levels of visfatin in gestational diabetes: a comparative study across various degrees of glucose tolerance. Diabetologia 50:1033–1037
Krzyzanowska K, Krugluger W, Mittermayer F et al (2006) Increased visfatin concentrations in women with gestational diabetes mellitus. Clin Sci 110:605–609
Akturk M, Altinova AE, Mert I et al (2008) Visfatin concentration is decreased in women with gestational diabetes mellitus in the third trimester. J Endocrinol Invest 31:610–613
Telejko B, Kuzmicki M, Zonenberg A et al (2009) Visfatin in gestational diabetes: serum level and mRNA expression in fat and placental tissue. Diabetes Res Clin Pract 84:68–75
de Luis DA, Aller R, Gonzalez Sagrado M et al (2010) Serum visfatin concentrations are related to dietary intake in obese patients. Ann Nutr Metab 57:265–270
ACOG Practice Bulletin (2001) Clinical management guidelines for obstetrician-gynecologists Number 30, September 2001 (replaces Technical Bulletin Number 200, December 1994). Gestational diabetes. Obstet Gynecol 98:525–538
Carpenter MW, Coustan DR (1982) Criteria for screening tests for gestational diabetes. Am J Obstet Gynecol 144:768–773
Matthews DR, Hosker JP, Rudenski AS et al (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28:412–419
Ma Y, Cheng Y, Wang J et al (2010) The changes of visfatin in serum and its expression in fat and placental tissue in pregnant women with gestational diabetes. Diabetes Res Clin Pract 90:60–65
Coskun A, Ozkaya M, Kiran G et al (2010) Plasma visfatin levels in pregnant women with normal glucose tolerance, gestational diabetes and pre-gestational diabetes mellitus. J Matern Fetal Neonatal Med 23:1014–1018
Morgan SA, Bringolf JB, Seidel ER (2008) Visfatin expression is elevated in normal human pregnancy. Peptides 29:1382–1389
Katwa LC, Seidel ER (2009) Visfatin in pregnancy: proposed mechanism of peptide delivery. Amino Acids 37:555–558
Berndt J, Kloting N, Kralisch S et al (2005) Plasma visfatin concentrations and fat depot-specific mRNA expression in humans. Diabetes 54:2911–2916
Li L, Yang G, Li Q et al (2006) Changes and relations of circulating visfatin, apelin, and resistin levels in normal, impaired glucose tolerance, and type 2 diabetic subjects. Exp Clin Endocrinol Diabetes 114:544–548
Toruner F, Altinova AE, Bukan N et al (2009) Plasma visfatin concentrations in subjects with type 1 diabetes mellitus. Horm Res 72:33–37
Marcinkowska M, Lewandowski KC, Lewinski A et al (2007) Visfatin levels do not change after the oral glucose tolerance test and after a dexamethasone-induced increase in insulin resistance in humans. Endokrynol Pol 58:188–194
Lorente-Cebrian S, Bustos M, Marti A et al (2009) Eicosapentaenoic acid stimulates AMP-activated protein kinase and increases visfatin secretion in cultured murine adipocytes. Clin Sci (Lond) 117:243–249
Wen Y, Wang HW, Wu J et al (2006) Effects of fatty acid regulation on visfatin gene expression in adipocytes. Chin Med J (Engl) 119:1701–1708
Acknowledgments
This research has been supported by Tehran University of Medical Sciences and Health services grant. Also, we would like to thank obstetrics clinic staff of the Arash hospital, Tehran University of Medical Sciences, Tehran, Iran.
Conflict of interest
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rezvan, N., Hosseinzadeh-Attar, M.J., Masoudkabir, F. et al. Serum visfatin concentrations in gestational diabetes mellitus and normal pregnancy. Arch Gynecol Obstet 285, 1257–1262 (2012). https://doi.org/10.1007/s00404-011-2156-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-011-2156-7