Abstract
Objectives
To evaluate the outcomes of enhanced recovery after surgery (ERAS) implementation in a gynaecological oncology centre.
Method
Non-randomised control trial, evaluating morbidity outcomes, before and after implementation of ERAS programme. All consecutive major gynaecological oncology operations performed during two specified periods were included. Data were collected prospectively for a study group in the initial 7.5 months of ERAS implementation and compared with a consecutive historic control group from the exact same period, the year before. Patients’ characteristics and perioperative outcomes were compared. Further analysis stratified abdominal and laparoscopic surgery.
Results
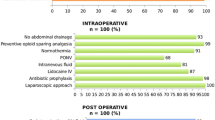
In total, 265 cases identified; 99 patients followed ERAS and 99 historic controls, managed with a traditional peri-operative approach, the exact same period the year before (vulval surgery excluded, 67 cases). Groups were comparable in demographics and co-morbidities (age, BMI, ASA, WHO), level of surgery and 30 days post-operative complication (grading Clavien-Dindo classification) and readmission rates (p > 0.05). Overall, the post-operative length of hospital stay (LOS) was significantly reduced for patients who followed ERAS (4.29 ± 2.78 days versus 7.23 ± 5.68 days, p < 0.001). Stratification to subgroups was based on the type of surgery, abdominal versus laparoscopic. Those who underwent abdominal surgery and followed ERAS benefited the maximum (LOS: 5.09 ± 2.74 days versus 8.70 ± 5.75, p < 0.001)
Conclusions
ERAS programme is feasible and safe in Gynae-oncology. In this study, there was a reduction of 3.61 (SE: 0.78, CI 95 %) days in the total LOS, in major abdominal Gynae-oncology surgery (level 3 and 4) without affecting complication or readmission rates.
Similar content being viewed by others
References
NHS Enhanced Recovery Partnership. Fulfilling the potential: a better journey for patients and a better deal for the nhs. Leicester; NHS Improvement; 2012
NHS Improvement (2012) My role and my responsibilities in helping to improve my recovery. NHS England, Redditch. http://www.improvement.nhs.uk/documents/er_my_role.pdf. Accessed 23 Nov 2014
Preoperative tests, the use of routine preoperative tests for elective surgery, NICE Clinical Guidelines, No. 3, National Collaborating Centre for Acute Care (UK). London: National Collaborating Centre for Acute Care (UK); 2003 Jun. http://www.ncbi.nlm.nih.gov/books/NBK48488/. Accessed 23 Nov 2014
Gizzo S, Ancona E, Saccardi C, Patrelli TS, Berretta R, Anis O et al (2013) Radical trachelectomy: the first step of fertility preservation in young women with cervical cancer (review). Oncol Rep 30(6):2545–2554. doi:10.3892/or.2013.2736
Gizzo S, Burul G, Di Gangi S, Lamparelli L, Saccardi C, Nardelli GB et al (2013) LigaSure vessel sealing system in vaginal hysterectomy: safety, efficacy and limitations. Arch Gynecol Obstet 288(5):1067–1074. doi:10.1007/s00404-013-2857-1
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Lidder P, Thomas S, Fleming S, Hosie K, Shaw S, Lewis S (2013) A randomized placebo controlled trial of preoperative carbohydrate drinks and early postoperative nutritional supplement drinks in colorectal surgery. Colorectal Dis 15(6):737–745
Gouvas N, Tan E, Windsor A, Xynos E, Tekkis P (2009) Fast-track vs standard care in colorectal surgery: a meta-analysis update. Int J Colorectal Dis 24:1119–1131
Varadha K, Neal K, Dejong C, Fearon K, Ljungqvist O, Lobo D (2010) The enhanced recovery after surgery (ERAS) pathway for patients undergoing major elective open colorectal surgery: a meta-analysis of randomized controlled trials. Clin Nutr 29:434–440
Guenaga KF, Matos D, Wille-Jørgensen P (2011) Mechanical bowel preparation for elective colorectal surgery. Cochrane Database Syst Rev 9:CD001544
Kehlet H (2008) Fast-track colorectal surgery. Lancet 371:791–793
Gadducci A, Cosio S, Spirito N, Genazzani AR (2010) The perioperative management of patients with gynaecological cancer undergoing major surgery: a debated clinical challenge. Crit Rev Oncol Hematol 73(2):126–140
Kalogera E, Bakkum-Gamez J, Jankowski C, Trabuco E, Lovely J, Dhanorker S et al (2013) Enhanced Recovery in Gynecologic Surgery. Obestet Gynaecol 122:319–328
Minig L, Biffi R, Zanagnolo V, Attanasio A, Beltrami C, Bocciolone L et al (2009) Reduction of postoperative complication rate with the use of early oral feeding in gynecologic oncologic patients undergoing major surgery: a randomized controlled trial. Ann Surg Oncol 16:3101–3110
Carter J (2012) Fast-track surgery in gynaecology and gynaecologic oncology: a review of a rolling clinical audit. ISRN Surg. 2012:368014
Chase DM, Lopez S, Nguyen CN, Pugmire GA, Monk BJ (2008) A clinical pathway for postoperative management and early patient discharge, does it work in gynecologic oncology? Am J Obstet Gynecol 199(541):e1–e7
Gustafsson UO, Hausel J, Thorell A, Ljungqvist O, Soop M, Nygren J (2011) Enhanced recovery after surgery study group. adherence to the enhanced recovery after surgery protocol and outcomes after colorectal cancer surgery. Arch Surg 146(5):571–577
Gerardi MA, Santillan A, Meisner B, Zahurak ML, Diaz Montes TP, Giuntoli RL II et al (2008) A clinical pathway for patients undergoing primary cytoreductive surgery with rectosigmoid colectomy for advanced ovarian and primary peritoneal cancers. Gynecol Oncol 108:282–286
Charoenkwan K, Phillipson G, Vutyavanich T (2007) Early versus delayed (traditional) oral fluids and food for reducing complications after major abdominal gynaecologic surgery. Cochrane Database Syst Rev 4:CD004508
Smith I, Kranke P, Murat I, Smith A, O’Sullivan G, Søreide E, Spies C, in’t Veld B (2011) European society of anaesthesiology. perioperative fasting in adults and children: guidelines from the european society of anaesthesiology. Eur J Anaesthesiol 28(8):556–569
Abbas SM, Hill AG (2008) Systematic review of the literature for the use of oesophageal Doppler monitor for fluid replacement in major abdominal surgery. Anaesthesia 63:44–51
Sinclair S, James S, Singer M (1997) Intraoperative intravascular volume optimisation and length of hospital stay after repair of proximal femoral fracture: randomised controlled trial. BMJ 315:909–912
Noblett SE, Watson DS, Huong H, Davison B, Hainsworth PJ, Horgan AF (2006) Pre-operative oral carbohydrate loading in colorectal surgery: a randomized controlled trial. Colorectal Dis 8:563–569
Nelson R, Edwards S, Tse B (2007) Prophylactic nasogastric decompression after abdominal surgery. Cochrane Database Syst Rev 3:CD004929
Borendal Wodlin N, Nilsson L, Kjølhede P, GASPI study group (2011) The impact of mode of anaesthesia on postoperative recovery from fast-track abdominal hysterectomy: a randomised clinical trial. BJOG 308:118–299
Carli F, Clemente A (2014) Regional anesthesia and enhanced recovery after surgery. Minerva Anestesiol 80(11):1228–1233
Kristensen B, Rasmussen Y, Agerlin M, Topp M, Weincke M, Kehlet H (2011) Local infiltration analgesia in urogenital prolapse surgery: a prospective randomized, double-blind, placebo-controlled study. Acta Obstet Gynecol Scand 90:1121–1125
Rockall TA, Demartines N (2014) Laparoscopy in the era of enhanced recovery. Best Pract Res Clin Gastroenterol 28(1):133–142
Berretta R, Gizzo S, Noventa M, Marrazzo V, Franchi L, Migliavacca C et al (2015) Quality of life in patients affected by endometrial cancer: comparison among laparotomy, laparoscopy and vaginal approach. Pathol Oncol Res 21(3):811–816. doi:10.1007/s12253-014-9895-2
Lv D, Wang X, Shi G (2010) Perioperative enhanced recovery programmes for gynaecological cancer patients. Cochrane Database Syst Rev 6:CD008239
Sjetne IS, Krogstad U, Odegard S, Engh ME (2009) Improving quality by introducing enhanced recovery after surgery in a gynaecological department: consequences for ward nursing practice. Qual Saf Health Care 18:236–240
Acknowledgments
The authors would like to acknowledge the valuable help of Margaret Ryan and Julie Kiernan (Clinical Nurse Specialists) in the successful implementation of the programme.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All patients participating in the study provided informed consent to participate in the ERAS implementation programme and approval has been granted from the Hospital Committee as part of clinical audit to review and present our data.
Funding
No funding was obtained to perform data collection, analysis and presentation of this study.
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Myriokefalitaki, E., Smith, M. & Ahmed, A.S. Implementation of enhanced recovery after surgery (ERAS) in gynaecological oncology. Arch Gynecol Obstet 294, 137–143 (2016). https://doi.org/10.1007/s00404-015-3934-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-015-3934-4