Abstract
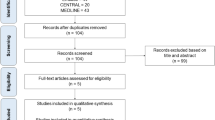
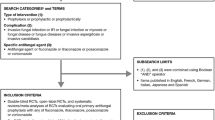
A systematic review and meta-analysis was performed to evaluate the benefits and harms of antifungal prophylaxis in liver transplant recipients. Ten randomised trials comparing any prophylactic antifungal regimen with no antifungal agent or with another antifungal regimen were identified from Medline, EMBASE, the Cochrane Library, and other sources. Together, the studies included a total of 1,106 patients. In general, results were consistent across trials despite clinical and methodological heterogeneity. Antifungal prophylaxis did not reduce total mortality (RR 0.84, 95% CI: 0.54–1.3). Fluconazole prophylaxis reduced invasive fungal infections by about 75% (RR 0.28, 95% CI: 0.13–0.57). Although fewer data on prophylactic itraconazole and liposomal amphotericin B were available, indirect comparisons and three direct comparative trials suggested similar efficacy. Fluconazole prophylaxis did not significantly increase colonisation or infection with azole-resistant fungi, although data were limited. A subgroup analysis suggested a dose and duration effect. In conclusion, fluconazole prophylaxis significantly reduces invasive fungal infections in liver transplant recipients and should be instituted in patients at increased risk in the early postoperative period.



Similar content being viewed by others
References
Beck-Sague C, Jarvis WR (1993) Secular trends in the epidemiology of nosocomial fungal infections in the United States, 1980–1990. J Infect Dis 167:1247–1251
Jarvis WR (1995) Epidemiology of nosocomial fungal infections, with emphasis on Candida species. Clin Infect Dis 20:1526–1530
Singh N (2000) Antifungal prophylaxis for solid organ transplant recipients: seeking clarity amidst controversy. Clin Infect Dis 31:545–553
Paya CV (1993) Fungal infections in solid-organ transplantation. Clin Infect Dis 16:677–688
Nieto-Rodriguez JA, Kusne S, Manez R, Irish W, Linden P, Magnone M, Wing EJ, Fung JJ, Starzl TE (1996) Factors associated with the development of candidemia and candidemia-related death among liver transplant recipients. Ann Surg 223:70–76
Husain S, Tollemar J, Dominguez EA, Baumgarten K, Humar A, Paterson DL, Wagener MM, Kusne S, Singh N (2003) Changes in the spectrum and risk factors for invasive candidiasis in liver transplant recipients: prospective, multicenter, case-controlled study. Transplantation 75:2023–2029
Paterson DL, Singh N (1999) Invasive aspergillosis in transplant recipients. Medicine 78:123–138
Lin S-J, Schranz J, Teutsch SM (2001) Aspergillosis case-fatality rate: systematic review of the literature. Clin Infect Dis 32:358–366
Kanda Y, Yamamoto R, Chizuka A, Hamaki T, Suguro M, Arai C, Matsuyama T, Takezako N, Miwa A, Kern W, Kami M, Akiyama H, Hirai H, Togawa A (2000) Prophylactic action of oral fluconazole against fungal infection in neutropenic patients. A meta-analysis of 16 randomized, controlled trials. Cancer 89:1611–1625
Bow EJ, Laverdiere M, Lussier N, Rotstein C, Cheang MS, Ioannou S (2002) Antifungal prophylaxis for severely neutropenic chemotherapy patients. A meta analysis of randomized-controlled clinical trials. Cancer 94:3230–3246
Glasmacher A, Prentice AG, Gorschluter M, Engelhart S, Hahn C, Djulbegovic B, Schmidt-Wolf IG (2003) Itraconazole prevents invasive fungal infections in neutropenic patients treated for hematologic malignancies: evidence from a meta-analysis of 3,597 patients. J Clin Oncol 21:4615–4626
Playford EG, Webster AC, Sorrell TC, Craig JC (2006) Antifungal agents for preventing fungal infections in non-neutropenic critically-ill and surgical patients: systematic review and meta-analysis of randomised clinical trials. J Antimicrob Chemother 57:628–638
Pappas PG, Rex JH, Sobel JD, Filler SG, Dismukes WE, Walsh TJ, Edwards JE (2004) Guidelines for treatment of candidiasis. Clin Infect Dis 38:161–189
Paya CV (2002) Prevention of fungal infection in transplantation. Transplant Infect Dis 4:46–51
Sobel JD, Rex JH (2001) Invasive candidiasis: turning risk into a practical prevention policy? Clin Infect Dis 33:187–190
Higgins J, Green S (2005) Highly sensitive search strategies for identifying reports of randomized controlled trials in MEDLINE. Cochrane handbook for systematic reviews of interventions 4.2.5; Section 4. The Cochrane Library, issue no. 3. Wiley, Chichester, UK
Lefebvre C, McDonald S (1996) Development of a sensitive search strategy for reports of randomized controlled trials in EMBASE. In: Proceedings of the 4th International Cochrane Colloquium. Cochrane Collaboration, Adelaide, Australia, Abstract no. 33
Higgins J, Green S (2005) Assessment of study quality. Cochrane handbook for systematic reviews of interventions 4.2.5 (updated May 2005); Section 6. The Cochrane Library, issue no. 3. Wiley, Chichester, UK
Ascioglu S, Rex JH, de Pauw B, Bennett JE, Bille J, Crokaert F, Denning DW, Donnelly JP, Edwards JE, Erjavec Z, Fiere D, Lortholary O, Maertens J, Meis JF, Patterson TF, Ritter J, Selleslang D, Shah PM, Stevens DA, Walsh TJ (2002) Defining opportunistic invasive fungal infections in immunocompromised patients with cancer and hemopoietic stem cell transplants: an international consensus. Clin Infect Dis 34:7–14
Higgins PT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Rossi SJ, Ferguson M, Gortesky S, Gelhoi A, Schroeder T, Hano D (1995) A randomised prospective trial of fluconazole vs. nystatin/clotrimazole for fungal prophylaxis in liver transplant recipients. In: Proceedings of the 14th Annual Meeting of the American Society of Transplant Physicians, Chicago, IL, p 149
Meyers B, Papanicolaou G, Chodoff L, Sheiner P, Miller C, Mendelson M, Shlasko NB (1997) A double-blind prospective controlled trial of fluconazole (F) vs. placebo in the prevention of fungal infections in patients undergoing orthotopic liver transplantation (OLT). In: Program and abstracts of the 37th ICAAC, American Society for Microbiology, Toronto, Abstract no. J57
Hadley S, Daly J, Pappas P, Kauffman CA, Rabkin J, Yao J, Schuster MG, Karchmer AW (2003) A randomized double-blind trial comparing AmBisome (AMB) and fluconazole (FL) in high-risk liver transplant recipients (LTR) for prevention of invasive fungal infection (IFI). In: Proceedings of the 41st Annual Meeting of the Infectious Diseases Society of America, San Diego, Abstract no. 133
Lumbreras C, Cuervas-Mons V, Jara P, del Palacio A, Turrion VS, Barrios C, Moreno E, Noriega AR, Paya CV (1996) Randomized trial of fluconazole versus nystatin for the prophylaxis of Candida infection following liver transplantation. J Infect Dis 174:583–588
Sharpe MD, Ghent C, Grant D, Horbay GLA, McDougal J, Colby WD (2003) Efficacy and safety of itraconazole prophylaxis for fungal infections after orthotopic liver transplantation: a prospective, randomized, double-blind study. Transplantation 76:977–983
Winston DJ, Busuttil RW (2002) Randomized controlled trial of oral itraconazole solution versus intravenous/oral fluconazole for prevention of fungal infections in liver transplant recipients. Transplantation 74:688–695
Tortorano AM, Viviani MA, Pagano A, Paone G, Gridelli B, Breda G, Langer M (1995) Candida colonization in orthotopic liver transplantation: fluconazole versus oral amphotericin B. J Mycol Med 5:21–24
Winston DJ, Pakrasi A, Busuttil RW (1999) Prophylactic fluconazole in liver transplant recipients. A randomized, double-blind, placebo-controlled trial. Ann Intern Med 131:729–737
Tollemar J, Hockerstedt K, Ericzon BG, Jalanko H, Ringden O (1995) Prophylaxis with liposomal amphotericin B (AmBisome) prevents fungal infections in liver transplant recipients: long-term results of a randomized, placebo-controlled trial. Transplant Proc 27:1195–1198
Biancofiore G, Bindi ML, Baldassarri R, Romanelli AM, Catalano G, Filipponi F, Vagelli A, Mosca F (2002) Antifungal prophylaxis in liver transplant recipients: a randomized placebo-controlled study. Transplant Int 15:341–347
Ruskin JD, Wood RP, Bailey MR, Whitmore CK, Shaw BW (1992) Comparative trial of oral clotrimazole and nystatin for oropharyngeal candidiasis prophylaxis in orthotopic liver transplant patients. Oral Surg Oral Med Oral Pathol 74:567–571
Fung JJ (2002) Fungal infection in liver transplantation. Transplant Infect Dis 4:18–23
Collins LA, Samore MH, Roberts MS, Luzzati R, Jenkins RL, Lewis WD, Karchmer AW (1994) Risk factors for invasive fungal infections complicating orthotopic liver transplantation. J Infect Dis 170:644–652
Patel R, Portela D, Badley AD, Harmsen WS, Larson-Keller JJ, Ilstrup DM, Keating MR, Wiesner RH, Krom RA, Paya CV (1996) Risk factors of invasive Candida and non-Candida fungal infections after liver transplantation. Transplantation 62:926–934
George MJ, Snydman DR, Werner BG, Griffith J, Falagas ME, Dougherty NN, Rubin RH (1997) The independent role of cytomegalovirus as a risk factor for invasive fungal disease in orthotopic liver transplant recipients. Am J Med 103:106–113
Singh N, Avery RK, Munoz P, Pruett TL, Alexander B, Jacobs R, Tollemar JG, Dominguez EA, Yu CM, Paterson DL, Husain S, Kusne S, Linden P (2003) Trends in risk profiles for and mortality associated with invasive aspergillosis among liver transplant recipients. Clin Infect Dis 36:46–52
Law D, Moore CB, Wardle HM, Ganguli LA, Keaney MGL, Denning DW (1994) High prevalence of antifungal resistance in Candida spp. from patients with AIDS. J Antimicrob Chemother 34:659–668
Johnson EM, Warnock DW, Luker J, Porter SR, Scully C (1995) Emergence of azole drug resistance in Candida species from HIV-infected patients receiving prolonged fluconazole therapy for oral candidosis. J Antimicrob Chemother 35:103–114
Nguyen MH, Peacock JE Jr, Morris AJ, Tanner DC, Nguyen ML, Snydman DR, Wagener MM, Rinaldi MG, Yu VL (1996) The changing face of candidemia: emergence of non-Candida albicans species and antifungal resistance. Am J Med 100:617–623
Abi-Said D, Anaissie E, Uzun O, Raad I, Pinzcowski H, Vartivarian S (1997) The epidemiology of hematogenous candidiasis caused by different Candida species. Clin Infect Dis 24:1122–1128
Fortun J, Lopez-San Roman A, Velasco JJ, Sanchez-Sousa A, de Vicente E, Nuno J, Quereda C, Barcena R, Monge G, Candela A, Honrubia A, Guerrero A (1997) Selection of Candida glabrata strains with reduced susceptibility to azoles in four liver transplant patients with invasive candidiasis. Eur J Clin Microbiol Infect Dis 16:314–318
Gleason TG, May AK, Caparelli D, Farr BM, Sawyer RG (1997) Emerging evidence of selection of fluconazole-tolerant fungi in surgical intensive care units. Arch Surg 132:1197–1201
Johansen HK, Gotzsche PC (1999) Problems in the design and reporting of trials of antifungal agents encountered during meta-analysis. JAMA 282:1752–1759
Smith GD, Egger M (1998) Meta-analysis: unresolved issues and future developments. BMJ 316:221–225
Cook DJ, Guyatt GH, Ryan G, Clifton J, Buckingham L, Willan A, McIlroy W, Oxman AD (1993) Should unpublished data be included in meta-analyses? Current convictions and controversies. JAMA 269:2749–2753
Thornton A, Lee P (2000) Publication bias in meta-analysis: its causes and consequences. J Clin Epidemiol 53:207–216
Sterling TD, Rosenbaum WL, Weinkam JJ (1995) Publication decisions revisited: the effects of the outcome of statistical tests on the decision to publish and vice versa. Am Statician 49:108–112
Scherer RW, Dickersin K, Langenberg P (1994) Full publication of results initially presented in abstracts. A meta-analysis. JAMA 272:158–162
Schultz K, Chambers I, Hayes R, Altman D (1995) Empirical evidence of bias. Dimensions of methodological quality associated with estimates of treatment effects in controlled trials. JAMA 273:408–412
Ascioglu S, de Pauw BE, Donnelly JP, Collette L (2001) Reliability of clinical research on invasive fungal infections: a systematic review of the literature. Med Mycol 39:35–40
Egger M, Dickersin K, Davey Smith G (2001) Problems and limitations in conducting systematic reviews. In: Egger M, Davey Smith G, Altman DG (eds) Systematic reviews in health care. Meta-analysis in context. BMJ Publishing Group, London, pp 43–68
Egger M, Davey Smith G, O’Rourke K (2001) Rationale, potentials, and promise of systematic reviews. In: Egger M, Davey Smith G, Altman D (eds) Systematic reviews in health care. Meta-analysis in context. BMJ Publishing Group, London, pp 3–22
Deeks JJ, Altman DG, Bradburn MJ (2001) Statistical methods for examining heterogeneity and combining results from several studies in meta-analysis. In: Egger M, Davey Smith G, Altman DG (eds) Systematic reviews in health care. Meta-analysis in context. BMJ, London, pp 285–312
Karchmer AW, Pappas P, Merion R, Cloud G, Hadley S, Rabkin J, Schuster MG, Andes D, Kauffman C, Delaney J, Daly J, Kusne S, Alexander B (2002) Invasive fungal infection in liver transplant recipients (LTR) considered at low risk. In: Proceedings of the Infectious Diseases Society of America 40th Annual Meeting, Chicago, IL, 24–27 October 2002, Abstract no. 16
Acknowledgements
The authors gratefully acknowledge the assistance provided by Narelle Willis, Cochrane Renal Group coordinator, and by study authors who responded to our enquiries for additional information. The helpful suggestions of the anonymous reviewers are also gratefully acknowledged. This review is an updated version of that published in the Cochrane Library (Issue 3, 2004), which will be periodically updated.
Author information
Authors and Affiliations
Corresponding author
Additional information
Potential conflicts of interest: E.G.P. is a member of the Mycology Interest Group of the Australasian Society for Infectious Diseases, which is sponsored by Gilead, Pfizer, and Merck. T.C.S. has advisory board involvement with Pfizer, Merck, and Gilead, has received unrelated project funding from Pfizer, Merck, and Gilead, and is a member of the Mycology Interest Group of the Australasian Society for Infectious Diseases, which is sponsored by Gilead, Pfizer, and Merck.
Rights and permissions
About this article
Cite this article
Playford, E.G., Webster, A.C., Sorrell, T.C. et al. Systematic review and meta-analysis of antifungal agents for preventing fungal infections in liver transplant recipients. Eur J Clin Microbiol Infect Dis 25, 549–561 (2006). https://doi.org/10.1007/s10096-006-0182-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-006-0182-3