Abstract
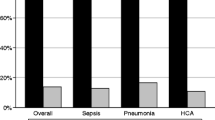
We conducted a retrospective matched cohort study to examine the impact of isolation of multi-drug-resistant (MDR) Acinetobacter baumannii on patient outcomes. Cases from whom MDR A. baumannii was isolated in a clinical culture (n = 118) were compared with controls from whom MDR A. baumannii was not isolated (n = 118). Cases and controls were matched according to ward, calendar month of hospitalization, and duration of hospitalization before culture. The following outcomes were compared in multivariable analysis: in-hospital mortality, length of stay, need for mechanical ventilation, and functional status at discharge. MDR A. baumannii was determined to be a pathogen in 72% of cases. In 36% of cases, the patient died, versus 21% of controls (odds ratio [OR] 2.21, 95% confidence interval [CI] 1.17–4.16, P = 0.014). Median length of stay for surviving cases was 17 days, versus 11 for surviving controls (multiplicative effect 1.55, 95% CI 0.99–2.44, P = 0.057). Fifty-two percent of cases required mechanical ventilation, versus 25% of controls (OR 3.72, 95% CI 1.91–7.25, P<0.001); 60% of surviving cases were discharged with reduced functional status, versus 38% of controls (OR 4.4, 95% CI 1.66–11.61, P = 0.003). In multivariable analysis, clinical isolation of MDR A. baumannii remained a significant predictor of mortality (OR 6.23, 95% CI 1.31–29.5, P = 0.021), need for mechanical ventilation (OR 7.34, 95% CI 2.24–24.0, P<0.001), and reduced functional status on discharge (OR 7.93, 95% CI 1.1–56.85, P = 0.039). Thus, MDR A. baumannii acquisition is associated with severe adverse outcomes, including increased mortality, need for mechanical ventilation, and reduced functional status.
Similar content being viewed by others
References
Seifert H, Strate A, Pulverer G (1995) Nosocomial bacteremia due to Acinetobacter baumannii. Clinical features, epidemiology, and predictors of mortality. Medicine (Baltimore) 74:340–349
Getchell-White SI, Donowitz LG, Groschel DH (1989) The inanimate environment of an intensive care unit as a potential source of nosocomial bacteria: evidence for long survival of Acinetobacter calcoaceticus. Infect Control Hosp Epidemiol 10:402–407
Wendt C, Dietze B, Dietz E, Ruden H (1997) Survival of Acinetobacter baumannii on dry surfaces. J Clin Microbiol 35:1394–1397
Gales AC, Jones RN, Forward KR, Linares J, Sader HS, Verhoef J (2001) Emerging importance of multidrug-resistant Acinetobacter species and Stenotrophomonas maltophilia as pathogens in seriously ill patients: geographic patterns, epidemiological features, and trends in the SENTRY Antimicrobial Surveillance Program (1997–1999). Clin Infect Dis 32 Suppl 2:S104–S113
Falagas ME, Bliziotis IA, Siempos II (2006) Attributable mortality of Acinetobacter baumannii infections in critically ill patients: a systematic review of matched cohort and case-control studies. Crit Care 10:R48
National Nosocomial Infections Surveillance (NNIS) (1996) National Nosocomial Infections Surveillance (NNIS) report, data summary from October 1986–April 1996, issued May 1996. A report from the National Nosocomial Infections Surveillance (NNIS) System. Am J Infect Control 24:380–388
Corbella X, Montero A, Pujol M, Domínguez MA, Ayats J, Argerich MJ, et al (2000) Emergence and rapid spread of carbapenem resistance during a large and sustained hospital outbreak of multiresistant Acinetobacter baumannii. J Clin Microbiol 38:4086–4095
Go ES, Urban C, Burns J, Kreiswirth B, Eisner W, Mariano N, et al (1994) Clinical and molecular epidemiology of Acinetobacter infections sensitive only to polymyxin B and sulbactam. Lancet 344:1329–1332
Landman D, Quale JM, Mayorga D, Adedeji A, Vangala K, Ravishankar J, et al (2002) Citywide clonal outbreak of multiresistant Acinetobacter baumannii and Pseudomonas aeruginosa in Brooklyn, NY: the preantibiotic era has returned. Arch Intern Med 162:1515–1520
Davis KA, Moran KA, McAllister CK, Gray PJ (2005) Multidrug-resistant Acinetobacter extremity infections in soldiers. Emerg Infect Dis 11:1218–1224
MMWR (2004) Acinetobacter baumannii infections among patients at military medical facilities treating injured U.S. service members, 2002–2004. MMWR Morb Mortal Wkly Rep 53:1063–1066
Aarabi B (1987) Comparative study of bacteriological contamination between primary and secondary exploration of missile head wounds. Neurosurgery 20:610–616
Heath CH OC, Lee RC, Pearman JW, McCullough C, Christiansen KJ (2003) A review of the Royal Perth Hospital Bali experience: an infection control perspective. Australian Infect Control 2:43–54
Maegele M, Gregor S, Steinhausen E, Bouillon B, Heiss MM, Perbix W, et al (2005) The long-distance tertiary air transfer and care of tsunami victims: injury pattern and microbiological and psychological aspects. Crit Care Med 33:1136–1140
Oncul O, Keskin O, Acar HV, Küçükardali Y, Evrenkaya R, Atasoyu EM, et al (2002) Hospital-acquired infections following the 1999 Marmara earthquake. J Hosp Infect 51:47–51
Paul M, Weinberger M, Siegman-Igra Y, Lazarovitch T, Ostfeld I, Boldur I, et al (2005) Acinetobacter baumannii: emergence and spread in Israeli hospitals 1997–2002. J Hosp Infect 60:256–60
Abbo A, Navon-Venezia S, Hammer-Muntz O, Krichali T, Siegman-Igra Y, Carmeli Y (2005) Multidrug-resistant Acinetobacter baumannii. Emerg Infect Dis 11:22–9
Acar JF (1997) Consequences of bacterial resistance to antibiotics in medical practice. Clin Infect Dis 24 Suppl 1:S17–S18
Cohen ML (1992) Epidemiology of drug resistance: implications for a post-antimicrobial era. Science 257:1050–1055
Schwaber MJ, Navon-Venezia S, Kaye KS, Ben-Ami R, Schwartz D, Carmeli Y (2006) Clinical and economic impact of bacteremia with extended-spectrum-beta-lactamase-producing Enterobacteriaceae. Antimicrob Agents Chemother 50:1257–1262
Beck-Sague CM, Jarvis WR, Brook JH, Culver DH, Potts A, Gay E, et al (1990) Epidemic bacteremia due to Acinetobacter baumannii in five intensive care units. Am J Epidemiol 132:723–733
Wisplinghoff H, Perbix W, Seifert H (1999) Risk factors for nosocomial bloodstream infections due to Acinetobacter baumannii: a case-control study of adult burn patients. Clin Infect Dis 28:59–66
Cisneros JM, Reyes MJ, Pachón J, Becerril B, Caballero FJ, García-Garmendía JL, et al (1996) Bacteremia due to Acinetobacter baumannii: epidemiology, clinical findings, and prognostic features. Clin Infect Dis 22:1026–1032
Blot S, Vandewoude K, Colardyn F (2003) Nosocomial bacteremia involving Acinetobacter baumannii in critically ill patients: a matched cohort study. Intensive Care Med 29:471–475
Falagas ME, Kopterides P, Siempos II (2006) Attributable mortality of Acinetobacter baumannii infection among critically ill patients. Clin Infect Dis 43:389–390
Fournier PE, Richet H (2006) The epidemiology and control of Acinetobacter baumannii in health care facilities. Clin Infect Dis 42:692–699
Kaye KS, Engemann JJ, Mozaffari E, Carmeli Y (2004) Reference group choice and antibiotic resistance outcomes. Emerg Infect Dis 10:1125–1128
Carmeli Y, Eliopoulos GM, Samore MH (2002) Antecedent treatment with different antibiotic agents as a risk factor for vancomycin-resistant Enterococcus. Emerg Infect Dis 8:802–807
Clinical and Laboratory Standards Institute (2005) Performance standards for antimicrobial susceptibility testing; fifteenth informational supplement. M100S15. Clinical and Laboratory Standards Institute, Wayne, Pa., USA
Garner JS, Jarvis WR, Emori TG, Horan TC, Hughes JM (1988) CDC definitions for nosocomial infections. Am J Infect Control 16:128–140
McCabe WR, Jackson GG (1962) Gram-negative bacteremia. Arch Intern Med 110:847–855
Carmeli Y, Troillet N, Karchmer AW, Samore MH (1999) Health and economic outcomes of antibiotic resistance in Pseudomonas aeruginosa. Arch Intern Med 159:1127–1132
Schwaber MJ, Carmeli Y (2006) Antimicrobial resistance and patient outcomes: the hazards of adjustment. Crit Care 10:164
Falagas ME, Kopterides P (2006) Risk factors for the isolation of multi-drug-resistant Acinetobacter baumannii and Pseudomonas aeruginosa: a systematic review of the literature. J Hosp Infect 64:7–15
Harbarth S, Garbino J, Pugin J, Romand JA, Lew D, Pittet D (2003) Inappropriate initial antimicrobial therapy and its effect on survival in a clinical trial of immunomodulating therapy for severe sepsis. Am J Med 115:529–535
Falagas ME, Kasiakou SK, Rafailidis PI, Zouglakis G, Morfou P (2006) Comparison of mortality of patients with Acinetobacter baumannii bacteraemia receiving appropriate and inappropriate empirical therapy. J Antimicrob Chemother 57:1251–1254
Navon-Venezia S, Ben-Ami R, Carmeli Y (2005) Update on Pseudomonas aeruginosa and Acinetobacter baumannii infections in the healthcare setting. Curr Opin Infect Dis 18:306–313
Sunenshine RH, Wright MO, Maragakis LL, Harris AD, Song X, Hebden J, et al (2007) Multidrug-resistant Acinetobacter infection mortality rate and length of hospitalization. Emerg Infect Dis 13:97–103
Paterson DL, Ko WC, Von Gottberg A, Mohapatra S, Casellas JM, Goossens H, et al (2004) Antibiotic therapy for Klebsiella pneumoniae bacteremia: implications of production of extended-spectrum beta-lactamases. Clin Infect Dis 39:31–37
Zimhony O, Chmelnitsky I, Bardenstein R, Goland S, Hammer Muntz O, Navon Venezia S, Carmeli Y (2006) Endocarditis caused by extended-spectrum-beta-lactamase-producing Klebsiella pneumoniae: emergence of resistance to ciprofloxacin and piperacillin-tazobactam during treatment despite initial susceptibility. Antimicrob Agents Chemother 50:3179–3182
Fournier PE, Vallenet D, Barbe V, Audic S, Ogata H, Poirel L, et al (2006) Comparative genomics of multidrug resistance in Acinetobacter baumannii. PLoS Genet 2:e7
Diep BA, Carleton HA, Chang RF, Sensabaugh GF, Perdreau-Remington F (2006) Roles of 34 virulence genes in the evolution of hospital- and community-associated strains of methicillin-resistant Staphylococcus aureus. J Infect Dis 193:1495–1503
Sahly H, Aucken H, Benedi VJ, Forestier C, Fussing V, Hansen DS, et al (2004) Increased serum resistance in Klebsiella pneumoniae strains producing extended-spectrum beta-lactamases. Antimicrob Agents Chemother 48:3477–3482
Acknowledgments
This study was funded by a grant from the United States-Israel Binational Science Foundation. The Foundation had no role in the design or conduct of any aspect of the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Abbo, A., Carmeli, Y., Navon-Venezia, S. et al. Impact of multi-drug-resistant Acinetobacter baumannii on clinical outcomes. Eur J Clin Microbiol Infect Dis 26, 793–800 (2007). https://doi.org/10.1007/s10096-007-0371-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-007-0371-8