Abstract
The aim of this study was to investigate the effects of low-level red laser on tissue repair in rats submitted to second-degree burn, evaluating if the timing of laser treatment influences the healing process. The animals had their backs shaved and divided as follows: control group (n = 12)—rats burned and not irradiated, early laser group (n = 12)—rats burned and irradiated from day 1 after injury for five consecutive days, and late laser group (n = 14)—rats burned and irradiated from day 4 after injury for five consecutive days. Laser irradiation was according to a clinical protocol (20 J/cm2, 100 mW, continuous wave emission mode, 660 nm) as recommended by the laser device manufacturer. Half of the animals were sacrificed 10 days after burn, and the other animals were sacrificed 21 days after burn. The late laser group accelerated wound contraction 10 and 21 days after burn. The late laser group accelerated reepithelialization 18 days after burn. The late laser group increases the granulation tissue 10 and 21 days after burn. Both irradiated groups increased type III collagen expression and TGF-β 21 days after burn. Both irradiated groups increased macrophage and myofibroblast numbers 10 days after burn and decreased 21 days after. Low-level red laser exposure contributes to the process of tissue repair of second-degree burns, but the intervention during proliferative phase is crucial in the final outcome of the repair process.




Similar content being viewed by others
References
Peck MD (2011) Epidemiology of burns throughout the world. Part I: distribution and risk factors. Burns 37:1087–1100
American burn association Online. http://www.ameriburn.org/resources_factsheet.php. 2012
Gurtner GC, Werner S, Barrandon Y, Longaker MT (2008) Wound repair and regeneration. Nature 453:314–321
Singer AJ, Clark RA (1999) Cutaneous wound healing. N Engl J Med 341:738–746
Nunez SC, Franca CM, Silva DF, Nogueira GE, Prates RA, Ribeiro MS (2013) The influence of red laser irradiation timeline on burn healing in rats. Lasers Med Sci 28:633–641
Zhang X, Liu L, Wei X, Tan YS, Tong L, Chang R, Ghanamah MS, Reinblatt M, Marti GP, Harmon JW, Semenza GP (2010) Impaired angiogenesis and mobilization of circulating angiogenic cells in HIF-1alpha heterozygous-null mice after burn wounding. Wound Repair Regen 18:193–201
Abrahamse H (2012) Regenerative medicine, stem cells, and low-level laser therapy: future directives. Photomed Laser Surg 30:681–682
Karu TI (2010) Multiple roles of cytochrome c oxidase in mammalian cells under action of red and IR-A radiation. IUBMB Life 62:607–610
da Silva JP, da Silva MA, Almeida AP, Lombardi Junior I, Matos AP (2010) Laser therapy in the tissue repair process: a literature review. Photomed Laser Surg 28:17–21
Meireles GC, Santos JN, Chagas PO, Moura AP, Pinheiro AL (2008) Effectiveness of laser photobiomodulation at 660 or 780 nanometers on the repair of third-degree burns in diabetic rats. Photomed Laser Surg 26:47–54
Vasheghani MM, Bayat M, Rezaei F, Bayat A, Karimipour M (2008) Effect of low-level laser therapy on mast cells in second degree burns in rats. Photomed Laser Surg 26:1–5
Gupta A, Daí T, Hamblin MR (2014) Effect of red and near-infrared wavelengths on low-level laser (light) therapy-induced healing of partial-thickness dermal abrasion in mice. Lasers Med Sci 29:257–265
Goncalves RV, Novaes RD, Cupertino Mdo C, Moraes B, Leite JP, Peluzio Mdo C, Pinto MV, da Matta SL (2013) Time-dependent effects of low-level laser therapy on the morphology and oxidative response in the skin wound healing in rats. Lasers Med Sci 28:383–390
de Moraes JM, de Oliveira E, Mendonca D, Moura VB, Oliveira MA, Afonso CL, Vinaud MC, Bachion MM, de Souza Lino R Jr (2013) Anti-inflammatory effect of low-intensity laser on the healing of third-degree burn wounds in rats. Lasers Med Sci 28:1169–1176
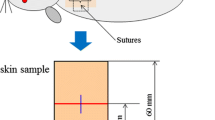
Venter NG, Monte-Alto-Costa A, Marques RG (2014) A new model for the standardization of experimental burn wounds. Burns. doi:10.1016/j.burns.2014.08.002
Reddy GK (2004) Photobiological basis and clinical role of low-intensity lasers in biology and medicine. J Clin Laser Med Surg 22:141–150
Fonseca AS, Geller M, Bernardo Filho M, Valenca SS, de Paoli F (2012) Low-level infrared laser effect on plasmid DNA. Lasers Med Sci 27:121–130
Farahani RM, Kloth LC (2008) The hypothesis of ‘biophysical matrix contraction’: wound contraction revisited. Int Wound J 5:477–482
Li J, Chen J, Kirsner R (2007) Pathophysiology of acute wound healing. Clin Dermatol 25:9–18
Broughton G 2nd, Janis JE, Attinger CE (2006) Wound healing: an overview. Plast Reconstr Surg 117:1e-S–32e-S
Fiorio FB, Albertini R, Leal-Junior EC, de Carvalho PT (2014) Effect of low-level laser therapy on types I and III collagen and inflammatory cells in rats with induced third-degree burns. Lasers Med Sci 29:313–319
Wong VW, Gurtner GC, Longaker MT (2013) Wound healing: a paradigm for regeneration. Mayo Clin Proc 88:1022–1031
Boo S, Dagnino L (2013) Integrins as modulators of transforming growth factor beta signaling in dermal fibroblasts during skin regeneration after injury. Adv Wound Care (New Rochelle) 2:238–246
dos Santos SA, Alves AC, Leal-Junior EC, Albertini R, Vieira Rde P, Ligeiro AP, Junior JA, de Carvalho PT (2014) Comparative analysis of two low-level laser doses on the expression of inflammatory mediators and on neutrophils and macrophages in acute joint inflammation. Lasers Med Sci 29:1051–1058
Alves AC, Vieira R, Leal-Junior E, dos Santos S, Ligeiro AP, Albertini R (2013) Effect of low-level laser therapy on the expression of inflammatory mediators and on neutrophils and macrophages in acute joint inflammation. Arthritis Res Ther 15:R116
Mirza R, DiPietro LA, Koh TJ (2009) Selective and specific macrophage ablation is detrimental to wound healing in mice. Am J Pathol 175:2454–2462
Lucas T, Waisman A, Ranjan R, Roes J, Krieg T, Muller W (2010) Differential roles of macrophages in diverse phases of skin repair. J Immunol 184:3964–3977
Jetten N, Roumans N, Gijbels MJ, Romano A, Post MJ, de Winther MP (2014) Wound administration of M2-polarized macrophages does not improve murine cutaneous healing responses. PLoS One 9:e102994
Chiarotto GB, Neves LM, Esquisatto MA, do Amaral ME, Dos Santos GM, Mendonça FA (2014) Effects of laser irradiation (670-nm InGaP and 830-nm GaAlAs) on burn of second degree in rats. Lasers Med Sci 29:1685–1693
de Vasconcelos Catao MH, Nonaka CF, de Albuquerque RL Jr, Bento PM, de Oliveira Costa R. (2014) Effects of red laser, infrared, photodynamic therapy, and green LED on the healing process of third-degree burns: clinical and histological study in rats. Lasers Med Sci 30(1):421-428
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Trajano, E.T.L., da Trajano, L.A., dos Santos Silva, M.A. et al. Low-level red laser improves healing of second-degree burn when applied during proliferative phase. Lasers Med Sci 30, 1297–1304 (2015). https://doi.org/10.1007/s10103-015-1729-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-015-1729-2