Abstract
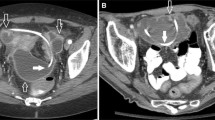
This study aims to review the imaging findings of distal (thoracic and abdominal) complications related to ventriculo-peritoneal (VP), ventriculo-pleural (VPL), and ventriculo-atrial (VA) cerebrospinal fluid (CSF) shunt catheter placement. Institution review board-approved single-center study of patients with thoracic and abdominal CSF catheter-related complications on cross-sectional imaging examinations over a 14-year period was performed. Clinical presentation, patient demographics, prior medical history, and subsequent surgical treatment were recorded. The presence or absence of CSF catheter-related infection and/or acute hydrocephalus on cross-sectional imaging was also recorded. There were 81 distal CSF catheter-related complications identified on 47 thoracic or abdominal imaging examinations in 30 patients (age 5–80 years, mean 39.3 years), most often on CT (CT = 42, MRI = 1, US = 4). Complications included 38 intraperitoneal and 11 extraperitoneal fluid collections. Extraperitoneal collections included nine abdominal wall subcutaneous (SC) pseudocysts associated with shunt migration and obesity, an intrapleural pseudocyst, and a breast pseudocyst. There were also two large VPL-related pleural effusions, a fractured catheter in the SC tissues, and a large VA shunt thrombus within the right atrium. Ten patients (33.3 %) had culture-positive infection from CSF or shunt catheter samples. Ten patients (33.3 %) had features of temporally related acute or worsening hydrocephalus on neuroimaging. In four of these patients, the detection of thoracic and abdominal complications on CT preceded and predicted the findings of acute hydrocephalus on cranial imaging. Thoracic and abdominal complications of CSF shunts, as can be identified on CT, include shunt infection and/or obstruction, may be both multiple and recurrent, and may be predictive of concurrent acute intracranial problems.









Similar content being viewed by others
References
Wallace AN, McConathy J, Menias CO et al (2014) Imaging evaluation of CSF shunts. AJR Am J Roentgenol 202:38–53. doi:10.2214/AJR.12.10270
Küpeli E, Yilmaz C, Akçay S (2010) Pleural effusion following ventriculopleural shunt: case reports and review of the literature. Ann Thorac Med 5:166–170. doi:10.4103/1817-1737.65048
Goeser CD, McLeary MS, Young LW (1998) Diagnostic imaging of ventriculoperitoneal shunt malfunctions and complications. Radiographics 18:635–651. doi:10.1148/radiographics.18.3.9599388
Vernet O, Rilliet B (2001) Late complications of ventriculoatrial or ventriculoperitoneal shunts. Lancet 358:1569–1570. doi:10.1016/S0140-6736(01)06670-3
Bergsneider M, Egnor MR, Johnston M et al (2006) What we don’t (but should) know about hydrocephalus. J Neurosurg 104:157–159. doi:10.3171/ped.2006.104.3.157
Nfonsam V, Chand B, Rosenblatt S et al (2008) Laparoscopic management of distal ventriculoperitoneal shunt complications. Surg Endosc 22:1866–1870. doi:10.1007/s00464-007-9728-4
Chung J-J, Yu J-S, Kim JH et al (2009) Intraabdominal complications secondary to ventriculoperitoneal shunts: CT findings and review of the literature. AJR Am J Roentgenol 193:1311–1317. doi:10.2214/AJR.09.2463
Blount JP, Campbell JA, Haines SJ (1993) Complications in ventricular cerebrospinal fluid shunting. Neurosurg Clin N Am 4:633–656
Vinchon M, Fichten A, Delestret I, Dhellemmes P (2003) Shunt revision for asymptomatic failure: surgical and clinical results. Neurosurgery 52:347–353, discussion 353–6
Dabdoub CB, Dabdoub CF, Chavez M et al (2014) Abdominal cerebrospinal fluid pseudocyst: a comparative analysis between children and adults. Childs Nerv Syst 30:579–589. doi:10.1007/s00381-014-2370-2
Browd SR, Ragel BT, Gottfried ON, Kestle JRW (2006) Failure of cerebrospinal fluid shunts: part I: obstruction and mechanical failure. Pediatr Neurol 34:83–92. doi:10.1016/j.pediatrneurol.2005.05.020
Rainov N, Schobess A, Heidecke V, Burkert W (1994) Abdominal CSF pseudocysts in patients with ventriculo-peritoneal shunts report of fourteen cases and review of the literature. Acta Neurochir (Wien) 127:73–78
Ohba S, Kinoshita Y, Tsutsui M et al (2012) Formation of abdominal cerebrospinal fluid pseudocyst. Neurol Med Chir (Tokyo) 52:838–842
Aparici-Robles F, Molina-Fabrega R (2008) Abdominal cerebrospinal fluid pseudocyst: a complication of ventriculoperitoneal shunts in adults. J Med Imaging Radiat Oncol 52:40–43. doi:10.1111/j.1440-1673.2007.01909.x
Anderson CM, Sorrells DL, Kerby JD (2003) Intra-abdominal pseudocysts as a complication of ventriculoperitoneal shunts: a case report and review of the literature. Curr Surg 60:338–340. doi:10.1016/S0149-7944(03)00029-1
Burchianti M, Cantini R (1988) Peritoneal cerebrospinal fluid pseudocysts: a complication of ventriculoperitoneal shunts. Childs Nerv Syst 4:286–290
Pathi R, Sage M, Slavotinek J, Hanieh A (2004) Abdominal cerebrospinal fluid pseudocyst. Australas Radiol 48:61–63. doi:10.1111/j.1440-1673.2004.01245.x
Gaskill SJ, Marlin AE (1989) Pseudocysts of the abdomen associated with ventriculoperitoneal shunts: a report of twelve cases and a review of the literature. Pediatr Neurosci 15:23–26, discussion 26–7
Grunebaum M, Ziv N, Kornreich L et al (1988) The sonographic signs of the peritoneal pseudocyst obstructing the ventriculo-peritoneal shunt in children. Neuroradiology 30:433–438
Kim TY, Stewart G, Voth M et al (2006) Signs and symptoms of cerebrospinal fluid shunt malfunction in the pediatric emergency department. Pediatr Emerg Care 22:28–34
Briggs JR, Hendry GM, Minns RA (1984) Abdominal ultrasound in the diagnosis of cerebrospinal fluid pseudocysts complicating ventriculoperitoneal shunts. Arch Dis Child 59:661–664
Coley BD, Shiels WE, Elton S et al (2004) Sonographically guided aspiration of cerebrospinal fluid pseudocysts in children and adolescents. AJR Am J Roentgenol 183:1507–1510. doi:10.2214/ajr.183.5.1831507
Balakrishnan V, Jeanmonod R (2014) Two episodes of ventriculoperitoneal shunt migration in a patient with idiopathic intracranial hypertension. Case Rep Emerg Med 2014:280793–3. doi:10.1155/2014/280793
Sugerman H, Windsor A, Bessos M, Wolfe L (1997) Intra-abdominal pressure, sagittal abdominal diameter and obesity comorbidity. J Intern Med 241:71–79
Morrison JF, Sung KE, Bergman AM et al (2010) A novel solution to reduce the complications of distal shunt catheter displacement associated with obesity. J Neurosurg 113:1314–1316. doi:10.3171/2010.6.JNS10300
Sahuquillo J, Arikan F, Poca MA et al (2008) Intra-abdominal pressure: the neglected variable in selecting the ventriculoperitoneal shunt for treating hydrocephalus. Neurosurgery 62:143–149. doi:10.1227/01.NEU.0000311071.33615.E1, discussion 149–50
Nakahara K, Shimizu S, Oka H et al (2009) Migration of the distal end of a ventriculoperitoneal shunt into the abdominal wall in an obese patient: case report. Neurol Med Chir (Tokyo) 49:490–492
Nagasaka T, Inao S, Ikeda H et al (2010) Subcutaneous migration of distal ventriculoperitoneal shunt catheter caused by abdominal fat pad shift—three case reports. Neurol Med Chir (Tokyo) 50:80–82
Simon TD, Hall M, Riva-Cambrin J et al (2009) Infection rates following initial cerebrospinal fluid shunt placement across pediatric hospitals in the United States Clinical article. J Neurosurg Pediatr 4:156–165. doi:10.3171/2009.3.PEDS08215
George R, Leibrock L, Epstein M (1979) Long-term analysis of cerebrospinal fluid shunt infections. A 25-year experience. J Neurosurg 51:804–811. doi:10.3171/jns.1979.51.6.0804
Esposito C, Porreca A, Gangemi M et al (1998) The use of laparoscopy in the diagnosis and treatment of abdominal complications of ventriculo-peritoneal shunts in children. Pediatr Surg Int 13:352–354
Di Rocco C, Marchese E, Velardi F, Di Rocco C, Marchese E, Velardi F (1994) A survey of the first complication of newly implanted CSF shunt devices for the treatment of nontumoral hydrocephalus. Cooperative survey of the (1991–1992) Education Committee of the ISPN. Childs Nerv Syst 10:321–327
Browd SR, Gottfried ON, Ragel BT, Kestle JRW (2006) Failure of cerebrospinal fluid shunts: part II: overdrainage, loculation, and abdominal complications. Pediatr Neurol 34:171–176. doi:10.1016/j.pediatrneurol.2005.05.021
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
IRB statement
The institutional review board approved this retrospective study and waived the need for informed consent.
Rights and permissions
About this article
Cite this article
Bolster, F., Fardanesh, R., Morgan, T. et al. Cross-sectional imaging of thoracic and abdominal complications of cerebrospinal fluid shunt catheters. Emerg Radiol 23, 117–125 (2016). https://doi.org/10.1007/s10140-015-1368-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-015-1368-8