Abstract
Background
There is no level 1a evidence regarding the best technique for skin closure at loop ileostomy reversal. The aim of this study was to evaluate whether purse-string skin closure (PSC) is associated with lower surgical site infection (SSI) rates as compared to linear skin closure (LC).
Methods
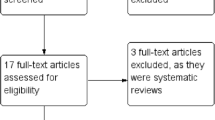
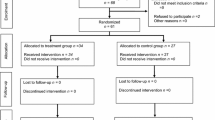
EMBASE, MEDLINE, Pubmed, Cochrane Library, Web of Science, and CINAHL databases were systematically searched. PSC was defined as a circumferential subcuticular suture leaving a small circular skin defect allowing for free drainage, granulation, and epithelialization. In LC, the wound edges were approximated side to side with or without drainage. The primary endpoint was SSI rate. Secondary endpoints included operating time, length of hospital stay, wound healing time, and incisional hernia rates.
Study selection
Inclusion criterion was any observational or experimental study comparing PSC to LC in patients undergoing ostomy reversal.
Results
Twenty studies (6 experimental and 14 observational) totaling 1812 patients (826 PSC and 986 LC) were included. SSI rates were significantly lower statistically and clinically in patients with PSC [OR (95% CI) = 0.14 (0.09, 0.21); p < 0.0001; NNT = 6] in the meta-analysis of all studies. The subgroup analysis of randomized trials [OR (95% CI) = 0.10 (0.04, 0.21); p < 0.0001; NNT = 6] as well as the analysis of randomized trials including patients with loop ileostomy only [OR (95% CI) = 0.12 (0.05, 0.28); p < 0.0001; NNT = 5] confirmed this finding.
Conclusions
This meta-analysis found that PSC was associated with significantly decreased rates of SSI in patients undergoing loop ileostomy reversal.







Similar content being viewed by others
References
Bax TW, McNevin MS (2007) The value of diverting loop ileostomy on the high-risk colon and rectal anastomosis. Am J Surg 193(5):585–587
Nagle DA (2013) Toward better understanding of readmissions for physiologic complications of ileostomy. Dis Colon Rectum 56(8):933–934
Kaidar-Person O, Person B, Wexner DS (2005) Complications of construction and closure of temporary loop ileostomy. J Am Coll Surg 201(5):759–773
Herrle F, Sandra-Petrescu F, Weiss C, Post S, Runkel N, Kienle P (2016) Quality of life and timing of stoma closure in patients with rectal cancer undergoing low anterior resection with diverting stoma: a multicenter longitudinal observational study. Dis Colon Rectum 59(4):281–290
Sutton CD, Williams N, Marshall LJ, Lloyd G, Thomas WM (2002) A technique for wound closure that minimizes sepsis after stoma closure. ANZ J Surg 72(10):766–767
Perez RO, Habr-Gama A, Seid VE et al (2006) Loop ileostomy morbity: timing of closure matters. Dis Colon Rectum 49(10):1539–1545
Hackam DJ, Rotsein OD (1995) Stoma closure and wound infection: an evaluation of risk factors. Can J Surg 38(2):144–148
Pan HD, Wang L, Peng YF et al (2015) Subcutaneous vacuum drains reduce surgical site infection after primary closure of defunctioning ileostomy. Int J Colorectal Dis 20(7):977–982
Uchino M, Hirose K, Toshihiro B, Chohno T, Takesue Y, Ikeuchi H (2016) Randomized controlled trial of prophylactic negative-pressure wound therapy at ostomy closure for the prevention of delayed wound healing and surgical site infection in patients with ulcerative colitis. Dig Surg 33(6):449–454
Banerjee A (1997) Pursestring skin closure after stoma reversal. Dis Colon Rectum 40(8):993–994
Li LT, Hicks SC, Davila JA, Kao LS, Berger RL, Arita NA, Lian MK (2014) Circular closure is associated with the lowest rate of surgical site infection following stoma reversal: a systematic review and multiple treatment meta-analysis. Colorectal Dis 16(6):406–416
McCartan DP, Burke JP, Walsh SR, Coffey JC (2013) Purse-string approximation is superior to primary skin closure following stoma reversal: a systematic review and meta-analysis. Tech Coloproctol 17(4):345–351
Higgins JP, Green S (2011) Cochrane handbook for systematic reviews of interventions, vol 4. Wiley, London
Moher D, Liberati A, Tetzlaff J et al (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8:336–341
Stroup DF, Berlin JA, Morton SC et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283(15):2008–2012
Horan TC, Gaynes RP, Martone WJ et al (1992) CDC definitions of nosocomial surgical site infections, 1992: a modification of CDC definitions of surgical wound infections. Infect Control Hosp Epidemiol 13:606–608
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13
Higgins JP, Thompson SG, Deeks JJ et al (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Cook RJ, Sackett DL (1995) The number needed to treat: a clinically useful measure of treatment effect. BMJ 310(6977):452–454
Altman DG (1998) Confidence intervals for the number needed to treat. BMJ 317(7168):1309–1312
Sureshkumar S, Jubel K, Ali MS et al (2018) Comparing surgical site infection and scar cosmesis between conventional linear skin closure versus purse-string skin closure in stoma reversal—a randomized controlled trial. Cureus 10(2):e2181
Alvandipour M, Gharedaghi B, Khodabakhsh H, Karami MY (2016) Purse-string versus linear conventional skin wound closure of an ileostomy: a randomized clinical trial. Ann Coloproctol 32(4):144–149
Camacho-Mauries D, Rodriguez-Díaz JL, Salgado-Nesme N, González QH, Vergara-Fernández O (2013) Randomized clinical trial of intestinal ostomy takedown comparing pursestring wound closure vs conventional closure to eliminate the risk of wound infection. Dis Colon Rectum 56(2):205–211
Dusch N, Goranova D, Herrle F, Niedergethmann M, Kienle P (2013) Randomized controlled trial: comparison of two surgical techniques for closing the wound following ileostomy closure: purse string vs direct suture. Colorectal Dis 15(8):1033–1040
Habbe N, Hannes S, Liese J, Woeste G, Bechstein WO, Strey C (2014) The use of purse-string skin closure in loop ileostomy reversals leads to lower wound infection rates—a single high-volume centre experience. Int J Colorectal Dis 29(6):709–714
Juratli MA, Nour-Eldin NA, Ackermann H et al (2018) Purse-string closure technique reduces the incidence of incisional hernias following the reversal of temporary ileostomy. Int J Colorectal Dis 33:973–977
Klink CD, Wunschmann M, Binnebosel M et al (2013) Influence of skin closure technique on surgical site infection after loop ileostomy reversal: retrospective cohort study. Int J Surg 11(10):1123–1125
Lee JR, Kim YW, Sung JJ et al (2011) Conventional linear versus purse-string skin closure after loop ileostomy reversal: comparison of wound infection rates and operative outcomes. J Korean Soc Coloproctol 27(2):58–63
Lee JT, Marquez TT, Clerc D et al (2014) Pursestring closure of the stoma site leads to fewer wound infections: results from a multicenter randomized controlled trial. Dis Colon Rectum 57(11):1282–1289
Li LT, Brahmbhatt R, Hicks SC, Davila JA, Berger DH, Liang MK (2014) Prevalence of surgical site infection at the stoma site following four skin closure techniques: a retrospective cohort study. Dig Surg 31(2):73–78
Marquez TT, Christoforidis D, Abraham A, Madoff RD, Rothenberger DA (2010) Wound infection following stoma takedown: primary skin closure versus subcuticular purse-string suture. World J Surg 34(12):2877–2882
Milanchi S, Nasseri Y, Kidner T, Fleshner P (2009) Wound infection after ileostomy closure can be eliminated by circumferential subcuticular wound approximation. Dis Colon Rectum 52(3):469–474
Mirbagheri N, Dark J, Skinner S (2013) Factors predicting stomal wound closure infection rates. Tech Coloproctol 17(2):215–220
O’Leary DP, Carter M, Wijewardene D et al (2017) The effect of purse-string approximation versus linear approximation of ileostomy reversal wounds on morbidity rates and patient satisfaction: the ‘STOMA’ trial. Tech Coloproctol 21(11):863–868
Reid K, Pockney P, Pollitt T, Draganic B, Smith SR (2010) Randomized clinical trial of short-term outcomes following purse-string versus conventional closure of ileostomy wounds. Br J Surg 97(10):1511–1517
Suh YJ, Park JW, Kim YS, Park SC, Oh JH (2014) A beneficial effect of purse-string skin closure after ileostomy takedown: a retrospective cohort study. Int J Surg 12(6):615–620
Wada Y, Miyoshi N, Ohue M et al (2015) Comparison of surgical techniques for stoma closure: a retrospective study of purse-string skin closure versus conventional skin closure following ileostomy and colostomy reversal. Mol Clin Oncol 3(3):619–622
Yamamoto M, Tanaka K, Masubuchi S et al (2018) Risk factors for surgical site infection after stoma closure comparison between pursestring wound closure and conventional linear wound closure: propensity score matching analysis. Am J Surg 215(1):58–61
Yoon SI, Bae SM, Namgung H, Park DG (2015) Clinical trial on the incidence of wound infection and patient satisfaction after stoma closure: comparison of two skin closure techniques. Ann Coloproctol 31(1):29–33
Younis J, Chowdhury Y, Scott HJ (2011) Purse-string closure versus conventional primary linear closure of ileostomy wounds. Colorectal Dis 13(Supp5):87
Zhou P, Hrabe J, Byrn J (2016) A retrospective, single-institution review of loop ileostomy reversal outcomes. Ostomy Wound Manag 62(8):22–33
Hseih MC, Kuo LT, Chi CC, Huang WS, Chin CC (2015) Pursestring closure versus conventional primary closure following stoma reversal to reduce surgical site infection rate: a meta-analysis of randomized controlled trials. Dis Colon Rectum 61(2):808–815
Funding
None.
Author information
Authors and Affiliations
Contributions
MG, RB: Intellectual concept and design of the work. MG, HL, AC, AD, NZ, and RB: Acquisition, analysis, or interpretation of the data. MG, HL, AC, AD, NZ, and RB: Drafting the manuscript. MG, HL, AC, AD, NZ, and RB: Revising and final approval of the submitted version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gachabayov, M., Lee, H., Chudner, A. et al. Purse-string vs. linear skin closure at loop ileostomy reversal: a systematic review and meta-analysis. Tech Coloproctol 23, 207–220 (2019). https://doi.org/10.1007/s10151-019-01952-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-019-01952-9