Abstract
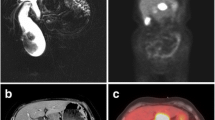
Neuroendocrine carcinoma of the gallbladder is an uncommon disease. We present the case of a 45-year-old woman with a mass located in the gallbladder, whose diagnosis was based on contrast-enhanced ultrasound and magnetic resonance imaging. The tumor involved the liver and retroperitoneum, and was histopathologically confirmed by liver biopsy as a neuroendocrine tumor grade 3. The patient received chemotherapy with good response, followed by surgery with cholecystectomy and partial hepatectomy.


Similar content being viewed by others
References
Lawrence B, Gustafsson BI, Chan A, et al. The epidemiology of gastroenteropancreatic neuroendocrine tumors. Endocrinol Metab Clin North Am. 2011;40:1–18.
Frilling A, Modlin IM, Kidd M, et al. for the Working Group on Neuroendocrine Liver Metastases. Recommendations for management of patients with neuroendocrine liver metastases. Lancet Oncol 2014;15:e8–21. www.thelancet.com/oncology.
John BJ, Davidson BR. Treatment options for unresectable neuroendocrine liver metastases. Expert Rev Gastroenterol Hepatol. 2012;6:357–69.
Albores-Saavedra J, Henson DE. Tumors of the Gallbladder and Extrahepatic Bile ducts. Radiographics. 2002;22:387–413.
Hamilton SR, Aaktonen LA. Pathology and genetics, tumors of the digestive system. WHO. 2000;214–6.
Jamali M, Chetty R. Predicting prognosis in gastroentero-pancreatic neuroendocrine tumors: an overview and the value of Ki-67 immunostaining. Endocr Pathol. 2008;19:282–8.
Dhall D, Mertens R, Bresee C, et al. Ki-67 proliferative index predicts progression-free survival of patients with well differentiated ileal neuroendocrine tumors. Hum Pathol. 2012;43:489–95.
Eltawil KM, Gustafsson BI, Kidd M, et al. Neuroendocrine tumors of the gallbladder: an evaluation and reassessment of management strategy. J Clin Gastroenterol. 2010;44:687–95.
Iwao M, Nakamura M, Enjoji M, et al. Primary hepatic carcinoid tumor: case report and review of 53 cases. Med Sci Monit. 2001;7:746–50.
Albores-Saavedra J, Molberg K, Henson DE. Unusual malignant epithelial tumors of the gallbladder. Semin Diagn Pathol. 1996;13:326–38.
Maitra A, Tascilar M, Hruban RH, et al. Small cell carcinoma of the gallbladder. A clinicopathologic, immunohistochemical, and molecular pathology study of 12 cases. Am J Surg Pathol. 2001;25:595–601.
Yamamoto M, Nakajo S, Miyoshi N, et al. Endocrine cell carcinoma (Carcinoid) of the gallbladder. Am J Surg Pathol. 1989;13:292–302.
Bosl GJ, Yagoda A, Camara LL. Malignant carcinoid of the gallbladder: third reported case and review of the literature. J Surg Oncol. 1980;13:215–22.
Komminoth P, Arnold R, Capella C, et al. Neuroendocrine neoplasms of the gallbladder and extrahepatic bile ducts. In: Bosman FT, Carneiro F, Hruban RH, et al., editors. WHO Classification of Tumours of the Digestive System. Lyon: IARC Press; 2010. p. 274–6.
Lepage C, Ciccolallo L, De Angelis R, et al. European disparities in malignant digestive endocrine tumours survival. Int J Cancer. 2010;126:2928–34.
Albores-Saavedra J, Nadji M, Henson DE, et al. Intestinal metaplasia of the gallbladder: a morphologic and immunocytochemical study. Hum Pathol. 1986;17:614–20.
Papotti M, Cassoni P, Sapino A, et al. Large cell neuroendocrine carcinoma of the gallbladder: report of two cases. Am J Surg Pathol. 2000;24:1424–8.
Wakiyama S, Yoshimura K, Shimada M, et al. Heterotopic gastric mucosa in a gallbladder with an anomalous union of the pancreatobiliary duct: a case report. Hepatogastroenterology. 1998;45:1488–91.
Modlin IM, Lye KD, Kidd M. A 5-Decade Analysis of 13,715 Carcinoid Tumors. Cancer. 2003;97:934–59.
McDermott EW, Guduric B, Brennan MF. Prognostic variables in patients with gastrointestinal carcinoid tumours. Br J Surg. 1994;81:1007–9.
Rindi G, D’Adda T, Froio E, et al. Prognostic factors in gastrointestinal endocrine tumors. Endocr Pathol. 2007;18:145–9.
Jung EM, Ross CJ, Rennert J, et al. Characterization of microvascularization of liver tumor lesions with high resolution linear ultrasound and contrast enhanced ultrasound (CEUS) during surgery: first results. Clin Hemorheol Microcirc. 2010;46:89–99.
Rickes S, Ocran KW, Gerstenhauer G, et al. Evaluation of diagnostic criteria for liver metastases of adenocarcinomas and neuroendocrine tumours at conventional ultrasound, unenhanced power Doppler sonography and echoenhanced ultrasound. Dig Dis. 2004;22:81–6.
d’Assignies G, Fina P, Bruno O, et al. High sensitivity of diffusion weighted MR imaging for the detection of liver metastases from neuroendocrine tumors: comparison with T2-weighted and dynamic gadolinium-enhanced MR imaging. Radiology. 2013; 268:390–99.
Frilling A, Sotiropoulos GC, Radtke A, et al. The impact of 68 Ga-DOTATOC positron emission tomography/computed tomography on the multimodal management of patients with neuroendocrine tumors. Ann Surg. 2010;252:850–6.
Ruf J, Heuck F, Schiefer J, et al. Impact of multiphase 68 Ga-DOTATOC-PET/CT on therapy management in patients with neuroendocrine tumors. Neuroendocrinology. 2010;91:101–9.
Elias D, Lefevre JH, Duvillard P, et al. Hepatic metastases from neuroendocrine tumors with a “thin slice” pathological examination: they are many more than you think. Ann Surg. 2010;251:307–10.
Bajetta E, Ferrari L, Martinetti A, et al. Chromogranin A, neuron specific enolase, carcinoembryonic antigen, and hydroxyindole acetic acid evaluation in patients with neuroendocrine tumors. Cancer. 1999;86:858–65.
Seregni E, Ferrari L, Bajetta E, et al. Clinical significance of blood chromogranin A measurement in neuroendocrine tumours. Ann Oncol. 2001;12:S69–72.
Soga J. Primary endocrinomas (carcinoid and variant neoplasm) of the gallbladder. A Statistical evaluation of 138 reported cases. J Exp Clin Cancer Res. 2001;22:5–15.
Pavel M, Baudin E, Couvelard A, et al. ENETS Consensus Guidelines for the management of patients with liver and other distant metastases from neuroendocrine neoplasms of foregut, midgut, hindgut, and unknown primary. Neuroendocrinology. 2012;95:157–76.
Sarmiento JM, Heywood G, Rubin J, et al. Surgical treatment of neuroendocrine metastases to the liver: a plea for resection to increase survival. J Am Coll Surg. 2003;197:29–37.
Elias D, Lasser P, Ducreux M, et al. Liver resection (and associated extrahepatic resections) for metastatic well-differentiated endocrine tumors: a 15-year single center prospective study. Surgery. 2003;133:375–82.
Glazer ES, Tseng JF, Al-Refaie W, et al. Long-term survival after surgical management of neuroendocrine hepatic metastases. HPB (Oxford). 2010;12:427–33.
Iype S, Mirza TA, Propper DJ. Neuroendocrine tumours of the gallbladder: three cases and a review of the literature. Postgrad Med J. 2009;85:213–8.
Mitry E, Baudin E, Ducreux M, et al. Treatment of poorly differentiated neuroendocrine tumours with etoposide and cisplatin. Br J Cancer. 1999;81:1351–5.
Moertel CG, Kvols LK, O’Connell MJ, et al. Treatment of neuroendocrine carcinomas with combined etoposide and cisplatin. Evidence of major therapeutic activity in the anaplastic variants of these neoplasms. Cancer. 1991;68:227–32.
Mezi S, Petrozza V, Schillaci O. Neuroendocrine tumors of the gallbladder: a case report and review of the literature. J Med Case Rep. 2011;5:334.
Modlin IM, Oberg K, Chung DC, et al. Gastroenteropancreatic neuroendocrine tumours. Lancet Oncol. 2008;9:61–72.
Acknowledgments
Liliana Chiorean thanks Doctor Mark Kidd from Yale University, USA, for his kind guidance and advice during manuscript preparation.
Conflict of interest
There are no financial or other relations that could lead to a conflict of interest.
Ethical standards
This article does not contain any studies with human or animal subjects performed by any of the authors.
Informed consent
Written informed consent was obtained from the patient for the publication of this manuscript and any accompanying images.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Chiorean, L., Bartos, A., Pelau, D. et al. Neuroendocrine tumor of gallbladder with liver and retroperitoneal metastases and a good response to the chemotherapeutical treatment. J Med Ultrasonics 42, 271–276 (2015). https://doi.org/10.1007/s10396-014-0585-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-014-0585-1