Abstract
Sepsis and other acute injuries such as severe trauma, extensive burns, or major surgeries, are usually followed by a period of marked immunosuppression. In particular, while lymphocytes play a pivotal role in immune response, their functions and numbers are profoundly altered after severe injuries. Apoptosis plays a central role in this process by affecting immune response at various levels. Indeed, apoptosis-induced lymphopenia duration and depth have been associated with higher risk of infection and mortality in various clinical settings. Therapies modulating apoptosis represent an interesting approach to restore immune competence after acute injury, although their use in clinical practice still presents several limitations. After briefly describing the apoptosis process in physiology and during severe injuries, we will explore the immunological consequences of injury-induced lymphocyte apoptosis, and describe associations with clinically relevant outcomes in patients. Therapeutic perspectives targeting apoptosis will also be discussed.
Similar content being viewed by others
Introduction
Severe injuries, i.e. mainly sepsis, trauma, burns, and major surgeries, represent a real public health challenge. For example, sepsis, recently redefined as a life-threatening organ dysfunction caused by the dysregulation of the host response to an infectious process [1], represents a burden of more than 5 million deaths per year in the world [2]. In high-income countries, its incidence is estimated to 437 per 100.000 person-years in the last decade, and related hospital mortality to 17%. The most severe form of sepsis, septic shock, affects 270 per 100.000 person-years, of which more than 25% will die [2]. Healthcare-associated infections (HAI) develop in 13% of septic patients and are responsible for 11% of the observed mortality [3].
Relative to severe traumas (violence, traffic accidents), extensive burns are less frequent, with an incidence of 10 per 100.000 person-years in France in 2011, relative mortality is as high as 50% [4]. Severely burn patients are particularly susceptible to HAI, which occurrence also increases length of stay and associated costs [5, 6].
Advances in anesthesia and critical care medicine have led to the development of increasingly invasive surgical procedures. Surgeries aiming at removing invading tumors—for example esophagectomy, cystectomy, gastrectomy, pancreaticoduodenectomy—are common nowadays in high-income countries. Almost one-third of patients undergoing such highly invasive procedures develop postoperative sepsis [7]. Moreover, this complication is independently associated with long-term mortality [7]. In addition, development of infection after pancreaticoduodenectomy results in a 32% increase in total hospital costs [8]. After spine surgery, postoperative deep wound infections causes more than a doubling of related costs [9].
Although these severe injuries represent a large number of patients worldwide at high risk of death and/or HAI, the burden of injury-induced immunosuppression occurring in these patients has largely been under-recognized. Indeed, it is now well established that these severe injuries induce marked immune dysfunctions [10]. Such immune alterations have been extensively explored within the last decade in severe septic syndromes. However, it is now clear that they also occur after other acute aggressions. The resulting immunosuppression is believed to be responsible for a large part of delayed deaths after injury, as it favors viral reactivations and HAI [11, 12]. The pathophysiology of the so-called “post-aggressive immunosuppression” involves both innate and adaptive immune responses [10]. Among various alterations, lymphocyte loss is a major cause for immunosuppression and apoptosis has been proposed as the main mechanism for lymphocyte death in sepsis and other injuries [13–15]. This review focuses on the consequences of lymphocyte apoptosis in critically ill patients after injuries and examines future therapeutic opportunities.
Apoptosis in sepsis
Apoptosis as an immunosuppressive process
Apoptosis is hypothesized to participate in the immunosuppressive process, details of which will be discussed below. Apoptosis is known to play a major role in physiology, from the embryo implantation and development to the turnover of adult tissues, as well as the selection of T cells during their maturation [16–18]. Apoptosis in cells can be induced through two main pathways. The extrinsic pathway is triggered by the binding of inducers to cell surface receptors, such as Fas, leading to subsequent caspase-8 activation. The intrinsic “mitochondrial” pathway is driven by upsetting the delicate balance between the products of pro- and anti-apoptotic genes of the Bcl-2 superfamily (B cell lymphoma 2), and by stress-induced noxious stimuli. This latter pathway is a known activator of caspase-9. Both pathways involve a common end-point, leading to caspase-3 activation and DNA fragmentation. Cross-talks exist between these two pathways, primarily through tBid, the truncated form of Bid (Bcl-2 homology domain 3 interacting-domain death agonist), causing the release of cytochrome c, endonuclease G, and Smac (second mitochondrial activator of caspases) [19, 20]. Both pathways are involved in sepsis-induced apoptosis [21–23].
Apoptosis in sepsis and immunological consequences
Apoptosis affects multiple cell types during sepsis [15]. Clinical evidences of apoptosis in splenocytes and intestinal epithelial cells were first observed in an autopsy study of adult patients who died from sepsis [13]. Similar results were later obtained in a pediatric cohort of sepsis-induced multiple organ failure [24]. Finally, the almost ubiquity of apoptosis process during sepsis was demonstrated in murine models [25, 26]. Neutrophils represent an exception, as their apoptosis is transitory decreased after septic shock, which could participate in the major neutrophilia observed in septic patients [27].
It is now admitted that some innate immune cells such as dendritic cells, as well as cells from the adaptive immune system, especially lymphocytes, are depleted due to apoptosis early after sepsis onset [28–30]. In addition, many studies both in mice and patients showed that sepsis-induced apoptosis is driven either by extrinsic or intrinsic pathways [21–23]. Finally, post-mortem studies in septic shock patients showed that such apoptotic process occurs not only in circulating cells, but also in solid organs [14].
There are two major consequences of the apoptotic process during sepsis. First, as mentioned before, apoptotic cells present anti-inflammatory properties and induce immunological tolerance [31, 32]. For example, it has been shown that their phagocytosis inhibits pro-inflammatory cytokines production by macrophages, while increasing anti-inflammatory factors release [33]. This is concordant with observations made in sepsis, since a shift from pro- to anti-inflammatory cytokine production has been observed in monocytes from septic patients versus healthy donors [34]. Similarly, the interaction between IL-10-producing apoptotic cells and antigen-presenting cells promotes a shift towards a Th2 polarization of the immune response [35, 36]. Such shift towards Th2 cytokine production has been described after septic shock and is predictive of fatal outcome [37, 38]. Induction of FoxP3+ (forkhead box P3) regulatory T cells (Tregs) also contributes to the depressed immune response induced by apoptotic elements [39]. In elderly patients suffering from sepsis, Inoue et al. demonstrated a decrease in immunocompetent CD4+ CD28+ T cells, whereas regulatory CD4+ CD25+ FoxP3+ and immunosuppressive PD-1+ (programmed cell death 1) T cells were increased [40]. Likewise, work from our lab revealed that septic shock patients present an increased percentage of regulatory T cells, the magnitude of which seems to be associated with more intense immunoparalysis and poorer outcomes [41]. This was not due to Tregs proliferation, but rather related to the lowering of effector CD4+ T cells numeration, suggesting that Tregs may not be susceptible to apoptosis during sepsis [42]. In addition, recent data indicate that Tregs could induce CD4+ effector T cells apoptosis through a TGF-β1 (transforming growth factor, beta 1) signal, therefore increasing the anti-inflammatory response in a negative feedback loop [43].
The anti-inflammatory effect of apoptosis alters clinical outcomes. A study from Prof. Hotchkiss’ team showed that, in rats, administration of apoptotic splenocytes before induction of peritonitis decreased interferon-gamma (IFN-γ) production and worsened animal survival, as compared to the transfer of necrotic splenocytes [44].
The second major consequence of apoptosis on the immune response after sepsis is the resultant massive cell loss observed in patients. While it has been described for other cell types such as dendritic cells [29], this phenomenon represents the principle cause of the severe sepsis-induced lymphopenia. This is illustrated by a study conducted in a University Hospital, which showed that, among all causes of admission, sepsis was the first etiology responsible for lymphopenia in all-cause hospitalized patients [45]. Such apoptosis-induced lymphopenia is pronounced in sepsis, since most septic patients present with <0.8 G/L absolute lymphocyte count and <0.3 G/L CD4+ lymphocytes [46]. Apoptosis-induced lymphopenia will be detailed in the next subchapter.
Apoptosis-induced lymphopenia in sepsis
Clinical demonstration
Numerous studies have investigated the occurrence of apoptosis in lymphocytes after sepsis by using different technical approaches. First, cell morphology is modified during apoptosis. This can be assessed by microscopy, showing fragmented and compacted nuclei. Cell shrinkage can also be revealed by a decrease in side and forward scatter on flow cytometric analyses, although this is largely nonspecific and rarely used in clinical studies [15]. The apoptotic signal is normally too low to be detected in healthy cells. In damaged cells, such signal is increased and might be detected and quantified by forward scatter analysis [47, 48]. Second, markers such as annexin-V, 7-AAD (7-aminoactinomycine D), APO2.7 (a protein confined to the mitochondrial membrane) [49], caspases [50, 51], among others, can be stained to assess apoptosis by flow cytometry. For example, Le Tulzo et al. showed that annexin-V staining was increased on circulating lymphocytes of sepsis and septic shock patients [52]. Similarly, Inoue et al. showed that polymicrobial sepsis induced higher percentage of caspase-3-positive splenocytes in rapidly-aging than in wild type mice [51].
Western-blot can also be used to detect caspases [53], Bid, FADD (Fas-associated protein with death domain) [54], Bcl-2, Bax (Bcl-2 associated X protein) [55], HMGβ1 (high-mobility group box 1), NFκB (nuclear factor, kappa B) [56], as well as ELISA to measure cytochrome-c concentrations [57, 58]. Such techniques have been used by Tinsley et al. and Guo et al. to demonstrate the increased thymocyte apoptosis in mice upon cecal ligature and punction-induced sepsis [53, 57].
DNA fragmentation occurring during the late stages of apoptosis can be detected by the TUNEL (terminal-deoxynucleotidyl-transferasemediated dUTP nick-end labeling) assay [59, 60]. When apoptotic, cells are detected as TUNEL-positive by flow cytometry. In mice after cecal ligature and punction (CLP), Unsinger et al. showed an increased percentage of TUNEL-positive CD3+ splenocytes [61], while Zou et al. found TUNEL-positive cells in thymus, spleen, and liver [50].
Studies of mRNA expression emphasized the intense modulation of gene expression during sepsis, particularly those of Bcl-2 superfamily genes. For example, the pro-apoptotic genes Bim (Bcl-2-like protein 11), Bak (Bcl-2 antagonist/killer), Bid and Fas were upregulated in septic shock patients [62, 63]. On the contrary, anti-apoptotic genes like Bcl-2 and Bcl-xl (B cell lymphoma-extra-large) were downregulated during severe sepsis [62]. These modulations in apoptosis-regulating genes may be cell-specific [64].
Overall, Le Tulzo et al. showed that lymphocyte apoptosis was increased by fivefold in septic shock patients versus controls, and by more than twofold versus other critically ill patients [52]. This major apoptotic process leads to severe lymphopenia (absolute lymphocyte count <0.5 G/L), which affects 25–63% of septic shock patients [65].
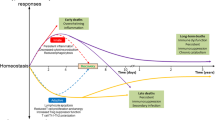
Although apoptosis results in a major decrease of lymphocyte absolute count right after the onset of septic shock [65], these alterations have been suspected to be specific to some lymphocyte subtypes. Especially, while apoptosis of CD4+ effector T cells has repeatedly been showed to be increased during sepsis not only in circulating blood cells but also in lymphoid organs, data concerning CD8+ T cells are still a subject of debate. For example, Hotchkiss et al. showed a caspase-9 mediated deletion of B and CD4+ T cells but not CD8+ or NK cells in septic patients [28]. Conversely, in a study by Le Tulzo et al. lymphopenia affected both CD4+ and CD8+ T cells subsets [52]. This is consistent with observations by Roger et al. of an enhanced apoptosis in CD4+ and CD8+ T cells during the early phase of human sepsis [66]. Poles apart, studies described that Tregs are resistant to sepsis-induced apoptosis and present pro-apoptotic effects on effector cells [67]. Overall, this strongly suggests that apoptosis favors sepsis-induced immunosuppression (Fig. 1).
Role of lymphocyte apoptosis in injury-induced immunosuppression. The initial acute injury (lightning) triggers complex pro and anti-inflammatory concomitant immune responses. Imbalance between both sides results in immunosuppression, leading to unfavorable outcomes. Lymphocyte apoptosis limits pro-inflammatory response and favors the global anti-inflammatory resultant. HAI healthcare-associated infections, Tregs regulatory T lymphocytes
Association with clinical outcomes
Numerous observational studies in clinical practice identified an association between sepsis-induced lymphopenia and poor outcomes in septic patients. For example, Chung et al. observed that the presence of severe lymphopenia at intensive care unit (ICU) admission of septic shock patients was associated with a 3.5-fold increased risk of death at day 28 [65]. In addition, persistence of this severe lymphopenia over time was also associated with poor prognosis. Drewry et al. showed that persistent lymphopenia on day 4 after the onset of sepsis predicted 28-day and 1-year survival [68]. Similarly, in children with multiple organ failure, prolonged lymphopenia for >7 days was also independently associated with an increased risk of death [24]. In fact, failure to recover a normal non-apoptotic lymphocyte count seems to be associated with higher mortality in septic shock patients [52].
Such association with increased mortality was also observed for other apoptosis markers. For example, in severe sepsis patients, caspase-cleaved cytokeratin-18 fragments concentration was higher in non-survivors than in survivors. In addition, in patients with sepsis-induced hepatic dysfunction, a higher level of total cytokeratin-18 at the onset of septic syndrome was also predictive for survival [69]. In a cohort of 87 septic patients, non-survivors of septic shock also presented higher levels of apoptosis markers (APO2.7 on leukocytes and lymphocytes, and 7-AAD and annexin V on monocytes) at admission to the emergency department, compared to survivors [49]. Moreover, proportion of APO2.7-positive lymphocytes predicted mortality with the same performances than lactacidemia [49].
Similar associations were observed between prolonged lymphopenia and increased risk of subsequent nosocomial infections after severe sepsis in children and adult patients [24, 68]. A pro-apoptotic gene expression pattern, with increased Bid and decreased Bcl-2 mRNA, was identified in children to predict the development of HAI after pediatric ICU admission. This was accompanied by an upregulation of anti-inflammatory cytokines gene expression [70].
Apoptosis-induced lymphopenia in other, non-septic, acute injuries
In other clinical settings and in unselected critical care patients, severe lymphopenia has been frequently observed in association with the development of injury-induced immunoparalysis and HAI [71].
Trauma
Lymphocyte apoptosis occurs early after severe trauma and is usually highest at day 3 after the injury [30, 72]. In addition, patients with higher injury severity score (ISS) exhibit more pronounced lymphopenia than less severely injured patients [30]. Lymphocyte subsets are differentially affected—CD4+ and NK T lymphocytes number is reduced, whereas CD8+ T cell number does not seem to exhibit important variations [73]. Severity of lymphopenia is associated with an increased risk of subsequent major infection or death [72]. Gouel-Chéron et al. showed that the CD4+ lymphocytes count at day 3 was lower in those patients who developed subsequent sepsis, relative to those who remained uninfected [74]. This was also observed by Heffernan et al. in a cohort of >2400 severely injured (ISS >15) patients. In this study, persistent lymphopenia over the first 4 days was independently associated with a higher risk of mortality and with an increased hospital length of stay [75].
Surgery
Major surgical procedures also affect adaptive immune response. First, various hypnotic drugs, either intravenous agents or inhaled halogenated gases, depressed the suppressor/cytotoxic lymphocyte ratio in mice, and decreased survival in a CLP model of sepsis [76]. In dogs, lymphopenia could be observed after induction of general anesthesia with thiopental, and a higher percentage of apoptotic cells was measured in animals undergoing laparotomy compared to those anesthetized but not operated [77]. In humans, pre-operative lymphopenia was associated with a 50% rise in post-operative infections [78]. Post-operative lymphocyte apoptosis observed after esophagectomy could have been induced by monocytes [79]. The intensity of lymphocyte apoptosis in the post-operative period is associated with the invasiveness of the surgical procedure. For example, surgery-induced lymphopenia was more pronounced after esophagectomy than after colorectal cancer surgery [80], whereas lymphopenia did not occur after minor surgical procedures [81]. Post-operative lymphopenia was also more common after open surgery than after laparoscopy [80]. Moreover, lymphocytes from pre-operatively lymphopenic patients exhibited increased expressions of apoptosis markers such as annexin-V and caspase-3, compared with non-lymphopenic patients [78]. T cell co-stimulatory receptor CD28 expression on T cells was markedly suppressed after major scheduled abdominal surgery, while Tregs were not affected [82]. Considering emergency intra-abdominal surgery, the lymphocyte count was shown to be decreased during the first week in non-survivors, and persistent lymphopenia was independently associated with a 3.5 fold increase in hospital mortality [83].
Burns
Following extensive burns, the total number of T lymphocytes is also drastically reduced [84]. In a murine model, depletion of lymphoid organs lasted over 2 months post-burn injury [85]. In a rat model of burns and subsequent infection, helper T cells appeared to be selectively depleted in infected animals compared to burn but non-infected ones [86]. In burn patients, a profound lymphopenia has been observed as well. While CD4+ lymphocytes are systematically affected, CD8+ count is not always reduced following thermal injury [87, 88]. Again, in this clinical context, Tregs are elevated versus controls. Moreover, their percentage is higher in non-survivors and in patients who will develop nosocomial sepsis [89].
Therapeutic perspectives
Considering the major links between injury-induced lymphocyte apoptosis and deleterious clinical outcomes, numerous therapeutic strategies aiming at restoring normal lymphocyte numbers and decreasing apoptosis have been evaluated both in animal models and ex vivo in patients’ cells.
Animal models
Many therapies have been proposed to limit lymphocyte apoptosis and its consequences during sepsis. Most of them have shown promising results, mainly in rodents. In a CLP model of polymicrobial sepsis, transgenic mice with overexpression of Bcl-2 in T lymphocytes were totally resistant to T cell apoptosis in thymus and spleen, but also developed less B cell apoptosis [90]. Moreover, mice with Bcl-2 overexpression had a lower mortality after sepsis [90, 91]. Similarly, overexpression of Bcl-xl, another anti-apoptotic gene of the Bcl-2 superfamily, reduced thymus and spleen T and B cell apoptosis as well and improved survival of septic mice [92]. As apoptosis involves many genes and pathways, they represent as many targets for gene expression modulation and putative therapeutic interventions. For example, overexpression of Akt in thymocytes and peripheral T cells of transgenic mice also decreased CD4+ T cell apoptosis via a non-Bcl-2-mediated mechanism, and improved survival in a CLP model [93]. However, to date, gene therapy appears difficult to implement in patients, and these reports rather demonstrate the interest of apoptosis modulation in sepsis than represent real ready-to-use therapies.
The balance in apoptosis regulation by Bcl-2 genes superfamily can also be modulated by antiapoptotic peptides, conjugated to permeation peptides derived from HIV-1 TAT (human immunodeficiency virus-1 trans-activator of transcription) basic domain to allow cell penetration. In vivo administration of TAT-BH4 (Bcl-2 homology domain 4) to septic mice decreased T and B cell apoptosis in splenocytes, and seemed to prevent also thymus and circulating blood T cell apoptosis [92].
Modulation can also take place at the translational level with small interfering RNAs (siRNA). Pre-treatment of mice with siRNA targeting Bim, a pro-apoptotic member of the Bcl-2 superfamily, resulted in a decrease in B and T cell apoptosis after CLP. It also conferred survival advantage to sepsis to pre-treated animals [94]. One major limitation of pre-treatment is its non-feasibility in clinical settings. However, post-exposure treatment with Fas and caspase-8 siRNA also suppressed sepsis-induced apoptosis in spleen and liver and improved mice survival after CLP [95].
Caspases are involved in both extrinsic and intrinsic apoptosis pathways. Anti-caspase therapies may therefore block sepsis-induced lymphocyte apoptosis. The broad-spectrum caspase inhibitor z-VAD-FMK (carbobenzoxy-valyl-alanyl-aspartyl-[O-ethyl]-fluoromethylketone) demonstrated its capacity to prevent lymphocyte apoptosis in spleen and thymus in a dose-dependent manner, and prevented mice death in a CLP model [91]. Another broad-spectrum caspase inhibitor, VX-166, lowered lymphocyte apoptosis and improved CLP mice survival [96]. Similar beneficial results on CD4+ and CD8+ T lymphocyte apoptosis and animal survival were obtained with the polycaspase inhibitor M-920 and the selective caspase-3 inhibitor M-791 [97].
An elegant therapeutic perspective is represented by protease inhibitors initially designed against HIV. Indeed, this class of antiretroviral agents is known to decrease HIV-induced CD4+ and CD8+ T cell apoptosis [98]. In a mice CLP model, pre-treatment with nelfinavir boosted by ritonavir prevented splenic and thymic lymphocyte apoptosis, increased tumor necrosis factor-alpha (TNF-α) and decreased IL-6 and IL-10 production. Moreover, it improved mice survival to sepsis, and this beneficial effect was preserved, although diminished, in case of post-CLP introduction of protease inhibitors [99]. Nelfinavir/ritonavir combination also showed its capacity to reduce apoptosis of multiple cell types in various diseases rodent models. Its modus operandi is located at the mitochondrial membrane level—inhibiting the loss of mitochondrial transmembrane potential by preventing the mitochondrial permeability transition pore complex adenine nucleotide translocator subunit pore function [100]. It should by highlighted that the beneficial effects of protease and caspase inhibitors are clearly mediated by lymphocytes, as Rag1−/− mice (recombination-activating gene 1), animals lacking functional lymphocytes, did not benefit these therapies [97, 99].
Post-aggressive immunoparalysis is characterized by an increased expression of co-inhibitory receptors on immune cells surface. Blockade of these receptors improves survival in experimental fungal sepsis [101], and is already used in human cancer, a condition with sepsis-like immunological defects [102]. In a mice CLP model, anti-PD-1 antibody inhibited apoptosis, thus preventing sepsis-induced lymphocyte depletion, and improved animal survival [103]. Similarly, blockade of PD-1 ligand by anti-PD-L1 antibody prevented T and B lymphocyte apoptosis in blood, spleen and thymus, enhanced bacterial clearance, and decreased mortality [104]. Inhibition of CTLA-4 (cytotoxic T lymphocyte associated protein 4), another co-inhibitory receptor, also decreased splenic T lymphocyte apoptosis in experimental polymicrobial sepsis [105].
In a murine peritonitis model, recombinant IL-7 (rhIL-7) increased splenic T lymphocyte count, probably due to the blockade of CD4+ and CD8+ spleen T cell apoptosis induced by rhIL-7 [106]. The same team observed similar increases in splenocytes count in rhIL-7-treated mice (versus septic untreated animals) after a double-hit model of sepsis, with a CLP followed by Candida albicans injection 4 days later. In this last study, rhIL-7 also restored IFN-γ production by CD8+ splenocytes [107]. In another study using a classic CLP model, rhIL-7 resulted in increased Bcl-2 expression in naive and effector memory CD4+ and CD8+ splenocytes as early as 3 h after treatment onset [108]. Taken together, these results suggest that the above described effects of rhIL-7 could be related to its anti-apoptotic effects.
Other therapies, such as IL-15 [109], IL-33 [110], and agonistic anti-CD40 receptor antibody [111] have shown benefits on lymphocyte apoptosis and survival in mice models of sepsis.
Efficacy on human blood ex vivo
Encouraging results have been obtained in mice, but human cells may react in a slightly different manner than predicted by animal experiments. Evidence of anti-apoptotic effects of the previously mentioned treatments in human cells is still scarce. In human T lymphocytes co-cultured in vitro with Escherichia coli, apoptosis was reduced by anti-apoptotic peptides TAT-Bcl-xl and TAT-BH4 in a dose-dependent manner [92].
In human lung epithelial cells, which are also subject to sepsis-induced apoptosis, kallistatin attenuated apoptosis via down-regulating Fas/Fas-ligand signaling, reactive oxygen species formation and subsequent NF-κB activation [112]. Limiting lung cell apoptosis may prevent sepsis-induced acute lung injury and acute respiratory distress syndrome.
Co-inhibitory receptors blockade also demonstrated interesting ex vivo results in septic shock patients’ blood. Chang et al. showed that anti-PD-1 and anti-PD-L1 antibodies decreased lymphocyte apoptosis and increased IFN-γ and IL-2 production [113].
Finally, work from our lab revealed that rhIL-7 was able to restore normal functions of lymphocytes purified from septic shock patients’ blood. Sepsis-induced decreases in lymphocyte proliferation and IFN-γ production were corrected by rhIL-7. Furthermore, rhIL-7 increased Bcl-2 protein expression, suggesting that the induced improvements observed might be, at least partially, related to an anti-apoptotic effect [114].
Limitations
Although attractive, therapeutic strategies aiming to modulate or block apoptosis may present several limitations in patients. First, apoptosis is a physiological process that is necessary for cell homeostasis [115]. It may also be a physiological response to the initial hyper-inflammation in sepsis, counterbalancing it by its anti-inflammatory consequences. Moreover, caspases also have other non-apoptotic functions, especially on cell proliferation and differentiation of B and T cells [15]. Therefore, blockade of apoptosis could induce serious adverse events. Consistently, a study in mice with cancer showed that prevention of apoptosis by overexpression of Bcl-2 increases mortality in a pneumonia model [116]. In another study, mice deficient for MyD88—an important element in response to pathogens, linking cell surface receptors to intracellular signaling pathways—had a worsened survival to CLP despite lower sepsis-induced apoptosis [117].
Moreover, lymphocyte apoptosis and apoptosis-induced lymphopenia occur quickly after the onset of sepsis [49]. Consequently, it may not be possible in clinical settings to initiate apoptosis blockade in such a short time-frame. Therefore, treating the consequences of lymphocyte apoptosis rather than apoptosis itself may represent an interesting and feasible alternative. As mentioned previously, one of the most promising therapies to boost lymphocyte number and functions in sepsis is rhIL-7 [114]. This therapy restores T cell functions, trafficking capacities to infected loci, and improves survival in experimental sepsis [106]. Recently, the complementary effects of rhIL-7 and anti-PD-1 therapies in septic mice have highlighted the possible benefit of a combined treatment in septic patients [118]. Two clinical trials testing the capacity of rhIL-7 to restore immune functions of septic patients—IRIS-7A (NCT02797431) and IRIS-7B (NCT02640807)—are currently recruiting.
Conclusion
Apoptosis-induced lymphopenia is a common process during sepsis and severe injuries, such as burns, major surgeries, and trauma. This process begins early after the onset of the causative injury. Lymphopenia severity and duration are associated with poor clinical outcomes, i.e. subsequent infections and higher mortality rates. Apoptosis is one of the leading causes of injury-associated lymphopenia, and participates directly and indirectly in injury-induced immunoparalysis. Many therapies targeting apoptosis have shown promising effects on immunological parameters and survival in animal models of severe injury. Apoptosis modulation represents an exciting field for critically ill patients’ treatment research, although the consequences of apoptosis blockade in patients deserve additional investigations. To date, recombinant human IL-7 represents an interesting therapy, as it may counterbalance the consequences of lymphocyte apoptosis in severely injured patients.
Abbreviations
- 7-AAD:
-
7-Aminoactinomycine D
- Bak:
-
Bcl-2 antagonist/killer
- Bax:
-
Bcl-2 associated X protein
- Bcl-2:
-
B cell lymphoma 2
- Bcl-xl:
-
B cell lymphoma-extra-large
- Bid:
-
Bcl-2 homology domain 3 interacting-domain death agonist
- Bim:
-
Bcl-2-like protein 11
- CD:
-
Cluster of differentiation
- CLP:
-
Cecal ligature and punction
- CTLA-4:
-
Cytotoxic T lymphocyte associated protein 4
- ELISA:
-
Enzyme-linked immunosorbent assay
- FADD:
-
Fas-associated protein with death domain
- FoxP3:
-
Forkhead box P3
- HAI:
-
Healthcare-associated infections
- HIV-1 TAT:
-
Human immunodeficiency virus-1 trans-activator of transcription
- HMGβ1:
-
High-mobility group box 1
- ICU:
-
Intensive care unit
- IFN-γ:
-
Interferon-gamma
- IL:
-
Interleukin
- ISS:
-
Injury severity score
- MyD88:
-
Myeloid differentiation primary response gene 88
- NFκB:
-
Nuclear factor, kappa B
- NK:
-
Natural killer
- PD-1:
-
Programmed cell death
- PD-L1:
-
PD-1 ligand
- Rag1:
-
Recombination-activating gene 1
- rhIL-7:
-
Recombinant IL-7
- siRNA:
-
Small interfering RNAs
- Smac:
-
Second mitochondrial activator of caspases
- TAT-BH4:
-
Trans-activator of transcription-Bcl-2 homology domain 4
- TGF-β1:
-
Transforming growth factor, beta 1
- Th2:
-
T helper 2
- TNF-α:
-
Tumor necrosis factor-alpha
- Tregs:
-
Regulatory T cells
- TUNEL:
-
Terminal-deoxynucleotidyl-transferasemediated dUTP nick-end labeling
- z-VAD-FMK:
-
Carbobenzoxy-valyl-alanyl-aspartyl-[O-ethyl]-fluoromethylketone
References
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, Bellomo R, Bernard GR, Chiche JD, Coopersmith CM, Hotchkiss RS, Levy MM, Marshall JC, Martin GS, Opal SM, Rubenfeld GD, van der Poll T, Vincent JL, Angus DC (2016) The third international consensus definitions for sepsis and septic shock (Sepsis-3). J Am Med Assoc 315:801–810
Fleischmann C, Scherag A, Adhikari NKJ, Hartog CS, Tsaganos T, Schlattmann P, Angus DC, Reinhart K, International Forum of Acute Care Trialists (2016) Assessment of global incidence and mortality of hospital-treated sepsis. Current estimates and limitations. Am J Respir Crit Care Med 193:259–272
van Vught LA, Klein Klouwenberg PMC, Spitoni C, Scicluna BP, Wiewel MA, Horn J, Schultz MJ, Nürnberg P, Bonten MJM, Cremer OL, van der Poll T, MARS Consortium (2016) Incidence, risk factors, and attributable mortality of secondary infections in the intensive care unit after admission for sepsis. J Am Med Assoc 315:1469–1479
Pasquereau A, Thélot B (2014) Hospitalisations pour brûlures à partir des données du programme de médicalisation des systèmes d’information. France métropolitaine 2011 et évolution depuis 2008 (French). http://www.sfetb.org/docs/2014/plaq_brulures_2014_bat.pdf. Accessed 1 Aug 2016
Oncul O, Yüksel F, Altunay H, Açikel C, Celiköz B, Cavuşlu S (2002) The evaluation of nosocomial infection during 1-year-period in the burn unit of a training hospital in Istanbul, Turkey. Burns 28:738–744
Brusselaers N, Monstrey S, Snoeij T, Vandijck D, Lizy C, Hoste E, Lauwaert S, Colpaert K, Vandekerckhove L, Vogelaers D, Blot S (2010) Morbidity and mortality of bloodstream infections in patients with severe burn injury. Am J Crit Care 19:e81–e87
Mokart D, Giaoui E, Barbier L, Lambert J, Sannini A, Chow-Chine L, Brun JP, Faucher M, Guiramand J, Ewald J, Bisbal M, Blache JL, Delpero JR, Leone M, Turrini O (2016) Postoperative sepsis in cancer patients undergoing major elective digestive surgery is associated with increased long-term mortality. J Crit Care 31:48–53
Santema TB, Visser A, Busch ORC, Dijkgraaf MGW, Goslings JC, Gouma DJ, Ubbink DT (2015) Hospital costs of complications after a pancreatoduodenectomy. HPB (Oxford) 17:723–731
Kuhns BD, Lubelski D, Alvin MD, Taub JS, McGirt MJ, Benzel EC, Mroz TE (2015) Cost and quality of life outcome analysis of postoperative infections after subaxial dorsal cervical fusions. J Neurosurg Spine 22:381–386
Hotchkiss RS, Monneret G, Payen D (2013) Sepsis-induced immunosuppression: from cellular dysfunctions to immunotherapy. Nat Rev Immunol 13:862–874
Hotchkiss RS, Monneret G, Payen D (2013) Immunosuppression in sepsis: a novel understanding of the disorder and a new therapeutic approach. Lancet Infect Dis 13:260–268
Venet F, Lukaszewicz AC, Payen D, Hotchkiss R, Monneret G (2013) Monitoring the immune response in sepsis: a rational approach to administration of immunoadjuvant therapies. Curr Opin Immunol 25:477–483
Hotchkiss RS, Swanson PE, Freeman BD, Tinsley KW, Cobb JP, Matuschak GM, Buchman TG, Karl IE (1999) Apoptotic cell death in patients with sepsis, shock, and multiple organ dysfunction. Crit Care Med 27:1230–1251
Hotchkiss RS, Tinsley KW, Karl IE (2003) Role of apoptotic cell death in sepsis. Scand J Infect Dis 35:585–592
Hotchkiss RS, Nicholson DW (2006) Apoptosis and caspases regulate death and inflammation in sepsis. Nat Rev Immunol 6:813–822
Kerr JF, Wyllie AH, Currie AR (1972) Apoptosis: a basic biological phenomenon with wide-ranging implications in tissue kinetics. Br J Cancer 26:239–257
Cohen JJ, Duke RC, Fadok VA, Sellins KS (1992) Apoptosis and programmed cell death in immunity. Annu Rev Immunol 10:267–293
Alison MR, Sarraf CE (1992) Apoptosis: a gene-directed programme of cell death. J R Coll Physicians Lond 26:25–35
Madesh M, Antonsson B, Srinivasula SM, Alnemri ES, Hajnóczky G (2002) Rapid kinetics of tBid-induced cytochrome c and Smac/DIABLO release and mitochondrial depolarization. J Biol Chem 277:5651–5659
van Loo G, Schotte P, van Gurp M, Demol H, Hoorelbeke B, Gevaert K, Rodriguez I, Ruiz-Carrillo A, Vandekerckhove J, Declercq W, Beyaert R, Vandenabeele P (2001) Endonuclease G: a mitochondrial protein released in apoptosis and involved in caspase-independent DNA degradation. Cell Death Differ 8:1136–1142
Ayala A, Perl M, Venet F, Lomas-Neira J, Swan R, Chung CS (2008) Apoptosis in sepsis: mechanisms, clinical impact and potential therapeutic targets. Curr Pharm Des 14:1853–1859
Hotchkiss RS, Osmon SB, Chang KC, Wagner TH, Coopersmith CM, Karl IE (2005) Accelerated lymphocyte death in sepsis occurs by both the death receptor and mitochondrial pathways. J Immunol 174:5110–5118
Chang KC, Unsinger J, Davis CG, Schwulst SJ, Muenzer JT, Strasser A, Hotchkiss RS (2007) Multiple triggers of cell death in sepsis: death receptor and mitochondrial-mediated apoptosis. FASEB J 21:708–719
Felmet KA, Hall MW, Clark RSB, Jaffe R, Carcillo JA (2005) Prolonged lymphopenia, lymphoid depletion, and hypoprolactinemia in children with nosocomial sepsis and multiple organ failure. J Immunol 174:3765–3772
Hiramatsu M, Hotchkiss RS, Karl IE, Buchman TG (1997) Cecal ligation and puncture (CLP) induces apoptosis in thymus, spleen, lung, and gut by an endotoxin and TNF-independent pathway. Shock 7:247–253
Hotchkiss RS, Swanson PE, Cobb JP, Jacobson A, Buchman TG, Karl IE (1997) Apoptosis in lymphoid and parenchymal cells during sepsis: findings in normal and T and B cell-deficient mice. Crit Care Med 25:1298–1307
Tamayo E, Gómez E, Bustamante J, Gómez-Herreras JI, Fonteriz R, Bobillo F, Bermejo-Martín JF, Castrodeza J, Heredia M, Fierro I, Álvarez FJ (2012) Evolution of neutrophil apoptosis in septic shock survivors and nonsurvivors. J Crit Care 27(415):e1–e11
Hotchkiss RS, Tinsley KW, Swanson PE, Schmieg RE, Hui JJ, Chang KC, Osborne DF, Freeman BD, Cobb JP, Buchman TG, Karl IE (2001) Sepsis-induced apoptosis causes progressive profound depletion of B and CD4+ T lymphocytes in humans. J Immunol 166:6952–6963
Hotchkiss RS, Tinsley KW, Swanson PE, Grayson MH, Osborne DF, Wagner TH, Cobb JP, Coopersmith C, Karl IE (2002) Depletion of dendritic cells, but not macrophages, in patients with sepsis. J Immunol 168:2493–2500
Hotchkiss RS, Schmieg RE, Swanson PE, Freeman BD, Tinsley KW, Cobb JP, Karl IE, Buchman TG (2000) Rapid onset of intestinal epithelial and lymphocyte apoptotic cell death in patients with trauma and shock. Crit Care Med 28:3207–3217
Griffith TS, Yu X, Herndon JM, Green DR, Ferguson TA (1996) CD95-induced apoptosis of lymphocytes in an immune privileged site induces immunological tolerance. Immunity 5:7–16
Henson PM, Bratton DL (2013) Antiinflammatory effects of apoptotic cells. J Clin Invest 123:2773–2774
Fadok VA, Bratton DL, Konowal A, Freed PW, Westcott JY, Henson PM (1998) Macrophages that have ingested apoptotic cells in vitro inhibit proinflammatory cytokine production through autocrine/paracrine mechanisms involving TGF-beta, PGE2, and PAF. J Clin Invest 101:890–898
Astiz M, Saha D, Lustbader D, Lin R, Rackow E (1996) Monocyte response to bacterial toxins, expression of cell surface receptors, and release of anti-inflammatory cytokines during sepsis. J Lab Clin Med 128:594–600
Voll RE, Herrmann M, Roth EA, Stach C, Kalden JR, Girkontaite I (1997) Immunosuppressive effects of apoptotic cells. Nature 390:350–351
Gao Y, Herndon JM, Zhang H, Griffith TS, Ferguson TA (1998) Antiinflammatory effects of CD95 ligand (FasL)-induced apoptosis. J Exp Med 188:887–896
Ono S, Ueno C, Aosasa S, Tsujimoto H, Seki S, Mochizuki H (2001) Severe sepsis induces deficient interferon-gamma and interleukin-12 production, but interleukin-12 therapy improves survival in peritonitis. Am J Surg 182:491–497
Gogos CA, Drosou E, Bassaris HP, Skoutelis A (2000) Pro-versus anti-inflammatory cytokine profile in patients with severe sepsis: a marker for prognosis and future therapeutic options. J Infect Dis 181:176–180
Kushwah R, Wu J, Oliver JR, Jiang G, Zhang J, Siminovitch KA, Hu J (2010) Uptake of apoptotic DC converts immature DC into tolerogenic DC that induce differentiation of Foxp3+ Treg. Eur J Immunol 40:1022–1035
Inoue S, Suzuki-Utsunomiya K, Okada Y, Taira T, Iida Y, Miura N, Tsuji T, Yamagiwa T, Morita S, Chiba T, Sato T, Inokuchi S (2013) Reduction of immunocompetent T cells followed by prolonged lymphopenia in severe sepsis in the elderly. Crit Care Med 41:810–819
Monneret G, Debard AL, Venet F, Bohe J, Hequet O, Bienvenu J, Lepape A (2003) Marked elevation of human circulating CD4+ CD25+ regulatory T cells in sepsis-induced immunoparalysis. Crit Care Med 31:2068–2071
Venet F, Pachot A, Debard AL, Bohé J, Bienvenu J, Lepape A, Monneret G (2004) Increased percentage of CD4+ CD25+ regulatory T cells during septic shock is due to the decrease of CD4+ CD25− lymphocytes. Crit Care Med 32:2329–2331
Luan Y, Yin C, Qin Q, Dong N, Zhu X, Sheng Z, Zhang Q, Yao Y (2015) Effect of regulatory T cells on promoting apoptosis of T lymphocyte and its regulatory mechanism in sepsis. J Interferon Cytokine Res 35:969–980
Hotchkiss RS, Chang KC, Grayson MH, Tinsley KW, Dunne BS, Davis CG, Osborne DF, Karl IE (2003) Adoptive transfer of apoptotic splenocytes worsens survival, whereas adoptive transfer of necrotic splenocytes improves survival in sepsis. Proc Natl Acad Sci USA 100:6724–6729
Castelino DJ, McNair P, Kay TW (1997) Lymphocytopenia in a hospital population–what does it signify? Aust N Z J Med 27:170–174
Venet F, Davin F, Guignant C, Larue A, Cazalis MA, Darbon R, Allombert C, Mougin B, Malcus C, Poitevin-Later F, Lepape A, Monneret G (2010) Early assessment of leukocyte alterations at diagnosis of septic shock. Shock 34:358–363
Banfalvi G, Klaisz M, Ujvarosi K, Trencsenyi G, Rozsa D, Nagy G (2007) Gamma irradiation induced apoptotic changes in the chromatin structure of human erythroleukemia K562 cells. Apoptosis 12:2271–2283
Banfalvi G (2014) Apoptotic agents inducing genotoxicity-specific chromatin changes. Apoptosis 19:1301–1316
Kung CT, Su CM, Chang HW, Cheng HH, Hsiao SY, Tsai TC, Tsai NW, Wang HC, Su YJ, Lin WC, Cheng BC, Chang YT, Chiang YF, Lu CH (2015) The prognostic value of leukocyte apoptosis in patients with severe sepsis at the emergency department. Clin Chim Acta 438:364–369
Zou L, Chen HH, Li D, Xu G, Feng Y, Chen C, Wang L, Sosnovik DE, Chao W (2015) Imaging lymphoid cell death in vivo during polymicrobial sepsis. Crit Care Med 43:2303–2312
Inoue S, Sato T, Suzuki-Utsunomiya K, Komori Y, Hozumi K, Chiba T, Yahata T, Nakai K, Inokuchi S (2013) Sepsis-induced hypercytokinemia and lymphocyte apoptosis in aging-accelerated Klotho knockout mice. Shock 39:311–316
Le Tulzo Y, Pangault C, Gacouin A, Guilloux V, Tribut O, Amiot L, Tattevin P, Thomas R, Fauchet R, Drénou B (2002) Early circulating lymphocyte apoptosis in human septic shock is associated with poor outcome. Shock 18:487–494
Tinsley KW, Cheng SL, Buchman TG, Chang KC, Hui JJ, Swanson PE, Karl IE, Hotchkiss RS (2000) Caspases-2, -3, -6, and -9, but not caspase-1, are activated in sepsis-induced thymocyte apoptosis. Shock 13:1–7
Clark JA, Clark AT, Hotchkiss RS, Buchman TG, Coopersmith CM (2008) Epidermal growth factor treatment decreases mortality and is associated with improved gut integrity in sepsis. Shock 30:36–42
Zhao L, An R, Yang Y, Yang X, Liu H, Yue L, Li X, Lin Y, Reiter RJ, Qu Y (2015) Melatonin alleviates brain injury in mice subjected to cecal ligation and puncture via attenuating inflammation, apoptosis, and oxidative stress: the role of SIRT1 signaling. J Pineal Res 59:230–239
Li L, Hu BC, Chen CQ, Gong SJ, Yu YH, Dai HW, Yan J (2013) Role of mitochondrial damage during cardiac apoptosis in septic rats. Chin Med J (Engl) 126:1860–1866
Guo RF, Huber-Lang M, Wang X, Sarma V, Padgaonkar VA, Craig RA, Riedemann NC, McClintock SD, Hlaing T, Shi MM, Ward PA (2000) Protective effects of anti-C5a in sepsis-induced thymocyte apoptosis. J Clin Invest 106:1271–1280
Messaris E, Memos N, Chatzigianni E, Kataki A, Nikolopoulou M, Manouras A, Albanopoulos K, Konstadoulakis MM, Bramis J (2008) Apoptotic death of renal tubular cells in experimental sepsis. Surg Infect 9:377–388
Gavrieli Y, Sherman Y, Ben-Sasson SA (1992) Identification of programmed cell death in situ via specific labeling of nuclear DNA fragmentation. J Cell Biol 119:493–501
Kyrylkova K, Kyryachenko S, Leid M, Kioussi C (2012) Detection of apoptosis by TUNEL assay. Methods Mol Biol 887:41–47
Unsinger J, Kazama H, McDonough JS, Griffith TS, Hotchkiss RS, Ferguson TA (2010) Sepsis-induced apoptosis leads to active suppression of delayed-type hypersensitivity by CD8 + regulatory T cells through a TRAIL-dependent mechanism. J Immunol 184:6766–6772
Weber SU, Schewe JC, Lehmann LE, Müller S, Book M, Klaschik S, Hoeft A, Stüber F (2008) Induction of Bim and Bid gene expression during accelerated apoptosis in severe sepsis. Crit Care 12:R128
Turrel-Davin F, Guignant C, Lepape A, Mougin B, Monneret G, Venet F (2010) Upregulation of the pro-apoptotic genes BID and FAS in septic shock patients. Crit Care 14:R133
Hoogerwerf JJ, van Zoelen MA, Wiersinga WJ, van’t Veer C, de Vos AF, de Boer A, Schultz MJ, Hooibrink B, de Jonge E, van der Poll T (2010) Gene expression profiling of apoptosis regulators in patients with sepsis. J Innate Immun 2:461–468
Chung KP, Chang HT, Lo SC, Chang LY, Lin SY, Cheng A, Huang YT, Chen CC, Lee MR, Chen YJ, Hou HH, Hsu CL, Jerng JS, Ho CC, Huang MT, Yu CJ, Yang PC (2015) Severe lymphopenia is associated with elevated plasma interleukin-15 levels and increased mortality during severe sepsis. Shock 43:569–575
Roger PM, Hyvernat H, Ticchioni M, Kumar G, Dellamonica J, Bernardin G (2012) The early phase of human sepsis is characterized by a combination of apoptosis and proliferation of T cells. J Crit Care 27:384–393
Cabrera-Perez J, Condotta SA, Badovinac VP, Griffith TS (2014) Impact of sepsis on CD4 T cell immunity. J Leukoc Biol 96:767–777
Drewry AM, Samra N, Skrupky LP, Fuller BM, Compton SM, Hotchkiss RS (2014) Persistent lymphopenia after diagnosis of sepsis predicts mortality. Shock 42:383–391
Hofer S, Brenner T, Bopp C, Steppan J, Lichtenstern C, Weitz J, Bruckner T, Martin E, Hoffmann U, Weigand MA (2009) Cell death serum biomarkers are early predictors for survival in severe septic patients with hepatic dysfunction. Crit Care 13:R93
Peronnet E, Nguyen K, Cerrato E, Guhadasan R, Venet F, Textoris J, Pachot A, Monneret G, Carrol ED (2016) Evaluation of mRNA biomarkers to identify risk of hospital acquired infections in children admitted to paediatric intensive care unit. PloS One 11:e0152388
Rajan G, Sleigh JW (1997) Lymphocyte counts and the development of nosocomial sepsis. Intensive Care Med 23:1187
Cheadle WG, Pemberton RM, Robinson D, Livingston DH, Rodriguez JL, Polk HC (1993) Lymphocyte subset responses to trauma and sepsis. J Trauma 35:844–849
Menges T, Engel J, Welters I, Wagner RM, Little S, Ruwoldt R, Wollbrueck M, Hempelmann G (1999) Changes in blood lymphocyte populations after multiple trauma: association with posttraumatic complications. Crit Care Med 27:733–740
Gouel-Chéron A, Venet F, Allaouchiche B, Monneret G (2012) CD4+ T lymphocyte alterations in trauma patients. Crit Care 16:432
Heffernan DS, Monaghan SF, Thakkar RK, Machan JT, Cioffi WG, Ayala A (2012) Failure to normalize lymphopenia following trauma is associated with increased mortality, independent of the leukocytosis pattern. Crit Care 16:R12
Hansbrough JF, Zapata-Sirvent RL, Bartle EJ, Anderson JK, Elliott L, Mansour MA, Carter WH (1985) Alterations in splenic lymphocyte subpopulations and increased mortality from sepsis following anesthesia in mice. Anesthesiology 63:267–273
Yamada R, Tsuchida S, Hara Y, Tagawa M, Ogawa R (2002) Apoptotic lymphocytes induced by surgical trauma in dogs. J Anesth 16:131–137
Edwards MR, Sultan P, del Arroyo AG, Whittle J, Karmali SN, Moonesinghe SR, Haddad FS, Mythen MG, Singer M, Ackland GL (2015) Metabolic dysfunction in lymphocytes promotes postoperative morbidity. Clin Sci 129:423–437
Kono K, Takahashi A, Iizuka H, Fujii H, Sekikawa T, Matsumoto Y (2001) Effect of oesophagectomy on monocyte-induced apoptosis of peripheral blood T lymphocytes. Br J Surg 88:1110–1116
Nishiguchi K, Okuda J, Toyoda M, Tanaka K, Tanigawa N (2001) Comparative evaluation of surgical stress of laparoscopic and open surgeries for colorectal carcinoma. Dis Colon Rectum 44:223–230
Sasajima K, Inokuchi K, Onda M, Miyashita M, Okawa KI, Matsutani T, Takubo K (1999) Detection of T cell apoptosis after major operations. Eur J Surg 165:1020–1023
Albertsmeier M, Quaiser D, von Dossow-Hanfstingl V, Winter H, Faist E, Angele MK (2015) Major surgical trauma differentially affects T cells and APC. Innate Immun 21:55–64
Vulliamy PE, Perkins ZB, Brohi K, Manson J (2015) Persistent lymphopenia is an independent predictor of mortality in critically ill emergency general surgical patients. Eur J Trauma Emerg Surg. doi:10.1007/s00068-015-0585-x
Barlow Y (1994) T lymphocytes and immunosuppression in the burned patient: a review. Burns 20:487–490
Organ BC, Antonacci AC, Chiao J, Chiao J, Kumar A, de Riesthal HF, Yuan L, Black D, Calvano SE (1989) Changes in lymphocyte number and phenotype in seven lymphoid compartments after thermal injury. Ann Surg 210:78–89
Burleson DG, Mason AD, Pruitt BA (1988) Lymphoid subpopulation changes after thermal injury and thermal injury with infection in an experimental model. Ann Surg 207:208–212
Maldonado MD, Venturoli A, Franco A, Nunez-Roldan A (1991) Specific changes in peripheral blood lymphocyte phenotype from burn patients. Probable origin of the thermal injury-related lymphocytopenia. Burns 17:188–192
Lebedev MY, Sholkina MN, Utkina TM, Vilkov SA, Korablev SB, Golubcova NV, Baryshnikov AY, Novikov VV (2001) Immunophenotype of peripheral blood lymphocytes in patients with burns. Russ J Immunol 6:47–54
Huang LF, Yao YM, Dong N, Yu Y, He LX, Sheng ZY (2010) Association between regulatory T cell activity and sepsis and outcome of severely burned patients: a prospective, observational study. Crit Care 14:R3
Hotchkiss RS, Swanson PE, Knudson CM, Chang KC, Cobb JP, Osborne DF, Zollner KM, Buchman TG, Korsmeyer SJ, Karl IE (1999) Overexpression of Bcl-2 in transgenic mice decreases apoptosis and improves survival in sepsis. J Immunol 162:4148–4156
Hotchkiss RS, Tinsley KW, Swanson PE, Chang KC, Cobb JP, Buchman TG, Korsmeyer SJ, Karl IE (1999) Prevention of lymphocyte cell death in sepsis improves survival in mice. Proc Natl Acad Sci USA 96:14541–14546
Hotchkiss RS, McConnell KW, Bullok K, Davis CG, Chang KC, Schwulst SJ, Dunne JC, Dietz GPH, Bähr M, McDunn JE, Karl IE, Wagner TH, Cobb JP, Coopersmith CM, Piwnica-Worms D (2006) TAT-BH4 and TAT-Bcl-xL peptides protect against sepsis-induced lymphocyte apoptosis in vivo. J Immunol 176:5471–5477
Bommhardt U, Chang KC, Swanson PE, Wagner TH, Tinsley KW, Karl IE, Hotchkiss RS (2004) Akt decreases lymphocyte apoptosis and improves survival in sepsis. J Immunol 172:7583–7591
Schwulst SJ, Muenzer JT, Peck-Palmer OM, Chang KC, Davis CG, McDonough JS, Osborne DF, Walton AH, Unsinger J, McDunn JE, Hotchkiss RS (2008) Bim siRNA decreases lymphocyte apoptosis and improves survival in sepsis. Shock 30:127–134
Wesche-Soldato DE, Chung CS, Lomas-Neira J, Doughty LA, Gregory SH, Ayala A (2005) In vivo delivery of caspase-8 or Fas siRNA improves the survival of septic mice. Blood 106:2295–2301
Weber P, Wang P, Maddens S, Wang PS, Wu R, Miksa M, Dong W, Mortimore M, Golec JMC, Charlton P (2009) VX-166: a novel potent small molecule caspase inhibitor as a potential therapy for sepsis. Crit Care 13:R146
Hotchkiss RS, Chang KC, Swanson PE, Tinsley KW, Hui JJ, Klender P, Xanthoudakis S, Roy S, Black C, Grimm E, Aspiotis R, Han Y, Nicholson DW, Karl IE (2000) Caspase inhibitors improve survival in sepsis: a critical role of the lymphocyte. Nat Immunol 1:496–501
Phenix BN, Angel JB, Mandy F, Kravcik S, Parato K, Chambers KA, Gallicano K, Hawley-Foss N, Cassol S, Cameron DW, Badley AD (2000) Decreased HIV-associated T cell apoptosis by HIV protease inhibitors. AIDS Res Hum Retroviruses 16:559–567
Weaver JGR, Rouse MS, Steckelberg JM, Badley AD (2004) Improved survival in experimental sepsis with an orally administered inhibitor of apoptosis. FASEB J 18:1185–1191
Weaver JGR, Tarze A, Moffat TC, Lebras M, Deniaud A, Brenner C, Bren GD, Morin MY, Phenix BN, Dong L, Jiang SX, Sim VL, Zurakowski B, Lallier J, Hardin H, Wettstein P, van Heeswijk RPG, Douen A, Kroemer RT, Hou ST, Bennett SAL, Lynch DH, Kroemer G, Badley AD (2005) Inhibition of adenine nucleotide translocator pore function and protection against apoptosis in vivo by an HIV protease inhibitor. J Clin Invest 115:1828–1838
Chang KC, Burnham CA, Compton SM, Rasche DP, Mazuski RJ, McDonough JS, Unsinger J, Korman AJ, Green JM, Hotchkiss RS (2013) Blockade of the negative co-stimulatory molecules PD-1 and CTLA-4 improves survival in primary and secondary fungal sepsis. Crit Care 17:R85
Hotchkiss RS, Moldawer LL (2014) Parallels between cancer and infectious disease. N Engl J Med 371:380–383
Brahmamdam P, Inoue S, Unsinger J, Chang KC, McDunn JE, Hotchkiss RS (2010) Delayed administration of anti-PD-1 antibody reverses immune dysfunction and improves survival during sepsis. J Leukoc Biol 88:233–240
Zhang Y, Zhou Y, Lou J, Li J, Bo L, Zhu K, Wan X, Deng X, Cai Z (2010) PD-L1 blockade improves survival in experimental sepsis by inhibiting lymphocyte apoptosis and reversing monocyte dysfunction. Crit Care 14:R220
Inoue S, Bo L, Bian J, Unsinger J, Chang K, Hotchkiss RS (2011) Dose-dependent effect of anti-CTLA-4 on survival in sepsis. Shock 36:38–44
Unsinger J, McGlynn M, Kasten KR, Hoekzema AS, Watanabe E, Muenzer JT, McDonough JS, Tschoep J, Ferguson TA, McDunn JE, Morre M, Hildeman DA, Caldwell CC, Hotchkiss RS (2010) IL-7 promotes T cell viability, trafficking, and functionality and improves survival in sepsis. J Immunol 184:3768–3779
Unsinger J, Burnham CAD, McDonough J, Morre M, Prakash PS, Caldwell CC, Dunne WM, Hotchkiss RS (2012) Interleukin-7 ameliorates immune dysfunction and improves survival in a 2-hit model of fungal sepsis. J Infect Dis 206:606–616
Kasten KR, Prakash PS, Unsinger J, Goetzman HS, England LG, Cave CM, Seitz AP, Mazuski CN, Zhou TT, Morre M, Hotchkiss RS, Hildeman DA, Caldwell CC (2010) Interleukin-7 (IL-7) treatment accelerates neutrophil recruitment through gamma delta T cell IL-17 production in a murine model of sepsis. Infect Immun 78:4714–4722
Inoue S, Unsinger J, Davis CG, Muenzer JT, Ferguson TA, Chang K, Osborne DF, Clark AT, Coopersmith CM, McDunn JE, Hotchkiss RS (2010) IL-15 prevents apoptosis, reverses innate and adaptive immune dysfunction, and improves survival in sepsis. J Immunol 184:1401–1409
Li S, Zhu FX, Zhao XJ, An YZ (2016) The immunoprotective activity of interleukin-33 in mouse model of cecal ligation and puncture-induced sepsis. Immunol Lett 169:1–7
Schwulst SJ, Grayson MH, DiPasco PJ, Davis CG, Brahmbhatt TS, Ferguson TA, Hotchkiss RS (2006) Agonistic monoclonal antibody against CD40 receptor decreases lymphocyte apoptosis and improves survival in sepsis. J Immunol 177:557–565
Lin WC, Chen CW, Huang YW, Chao L, Chao J, Lin YS, Lin CF (2015) Kallistatin protects against sepsis-related acute lung injury via inhibiting inflammation and apoptosis. Sci Rep 5:12463
Chang K, Svabek C, Vazquez-Guillamet C, Sato B, Rasche D, Wilson S, Robbins P, Ulbrandt N, Suzich J, Green J, Patera AC, Blair W, Krishnan S, Hotchkiss R (2014) Targeting the programmed cell death 1: programmed cell death ligand 1 pathway reverses T cell exhaustion in patients with sepsis. Crit Care 18:R3
Venet F, Foray AP, Villars-Méchin A, Malcus C, Poitevin-Later F, Lepape A, Monneret G (2012) IL-7 restores lymphocyte functions in septic patients. J Immunol 189:5073–5081
Jin Z, El-Deiry WS (2005) Overview of cell death signaling pathways. Cancer Biol Ther 4:139–163
Fox AC, Breed ER, Liang Z, Clark AT, Zee-Cheng BR, Chang KC, Dominguez JA, Jung E, Dunne WM, Burd EM, Farris AB, Linehan DC, Coopersmith CM (2011) Prevention of lymphocyte apoptosis in septic mice with cancer increases mortality. J Immunol 187:1950–1956
Peck-Palmer OM, Unsinger J, Chang KC, Davis CG, McDunn JE, Hotchkiss RS (2008) Deletion of MyD88 markedly attenuates sepsis-induced T and B lymphocyte apoptosis but worsens survival. J Leukoc Biol 83:1009–1018
Shindo Y, Unsinger J, Burnham CA, Green JM, Hotchkiss RS (2015) Interleukin-7 and anti-programmed cell death 1 antibody have differing effects to reverse sepsis-induced immunosuppression. Shock 43:334–343
Acknowledgements
This work was supported by Hospices Civils de Lyon (France).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare they have no conflict of interest related to this manuscript. All authors are employees of Hospices Civils de Lyon and Lyon 1 University (Lyon, France).
Rights and permissions
About this article
Cite this article
Girardot, T., Rimmelé, T., Venet, F. et al. Apoptosis-induced lymphopenia in sepsis and other severe injuries. Apoptosis 22, 295–305 (2017). https://doi.org/10.1007/s10495-016-1325-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10495-016-1325-3