Abstract
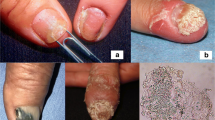
Onychomycosis is a common fungal infection affecting nails. The primary cause for onychomycosis is dermatophytes, while Candida species have emerged as second-line pathogens. Onychomycosis due to Candida (candidal onychomycosis) is increasingly found in individuals having defective immunity consequential to aging, diabetes mellitus, vascular diseases, HIV infection and drug therapies such as immunosuppressives and broad-spectrum antibiotics. Breached local immunity at the nail complex due to trauma, chronic exposure to moisture and chemicals including smoke, detergents, soap, etc., also contribute to candidal onychomycosis. Adhesion, filamentation, secretion of extracellular enzymes and the development of antifungal resistance are some of the virulence mechanisms of Candida species associated with onychomycosis. Diagnosis of onychomycosis depends on history and clinical examination, direct microscopic investigation, mycological culture and histopathology. Restoration of immune defenses, elimination of fungi using appropriate drug therapy and improvement of nail hygiene with the removal of predisposing factors are key aspects in the management of candidal onychomycosis.


Similar content being viewed by others
Abbreviations
- CMC:
-
Chronic mucocutaneous candidiasis
- HIV:
-
Human immunodeficiency virus
- KOH:
-
Potassium hydroxide
- PAS:
-
Periodic acid Schiff
References
Veer P, Patwardhan NS, Damle AS. Study of onychomycosis: prevailing fungi and pattern of infection. Indian J Med Microbiol. 2007;25:53–6. doi:10.4103/0255-0857.31063.
Vélez A, Linares MJ, Fenández-Roldán JC, Casal M. Study of onychomycosis in Córdoba, Spain: prevailing fungi and pattern of infection. Mycopathologia. 1997;137:1–8. doi:10.1023/A:1006874303991.
Loo DS. Onychomycosis in the elderly: drug treatment options. Drugs Aging. 2007;24:293–302. doi:10.2165/00002512-200724040-00003.
Lange M, Roszkiewicz J, Szczerkowska-Dobosz A, Jasiel-Walikowska E, Bykowska B. Onychomycosis is no longer a rare finding in children. Mycoses. 2006;49:55–9. doi:10.1111/j.1439-0507.2005.01186.x.
Gupta AK, Taborda P, Taborda V, Gilmour J, Rachlis A, Salit I, et al. Epidemiology and prevalence of onychomycosis in HIV positive individuals. Int J Dermatol. 2000;39:746–53. doi:10.1046/j.1365-4362.2000.00012.x.
Surjushe A, Kamath R, Oberai C, Saple D, Thakre M, Dharmshale S, et al. A clinical and mycological study of onychomycosis in HIV infection. Indian J Dermatol Venereol Leprol. 2007;73:397–401. doi:10.4103/0378-6323.35751.
Jesudanam TM, Rao GR, Lakshmi DJ, Kumari GR. Onychomycosis: a significant medical problem. Indian J Dermatol Venereol Leprol. 2002;68:326–9.
Chi CC, Wang SH, Chou MC. The causative pathogens of onychomycosis in southern Taiwan. Mycoses. 2005;48:413–20. doi:10.1111/j.1439-0507.2005.01152.x.
Foster KW, Ghannoum MA, Elewski BE. Epidemiologic surveillance of cutaneous fungal infection in the United States from 1999 to 2002. J Am Acad Dermatol. 2004;50:748–52. doi:10.1016/S0190-9622(03)02117-0.
Das S, Goyal R, Bhattacharya SN. Laboratory based epidemiological study of superficial fungal infections. J Dermatol. 2007;34:248–53. doi:10.1111/j.1346-8138.2007.00262.x.
Kirkpatrick CH, Rich RR, Bennett JE. Chronic mucocutaneous candidiasis: model-building in cellular immunity. Ann Intern Med. 1971;74:955–78.
Kirkpatrick CH. Chronic mucocutaneous candidiasis. Pediatr Infect Dis J. 2001;20:197–206. doi:10.1097/00006454-200102000-00017.
Tosti A, Piraccini BM, Lorenzi S, D’Antuono A. Candida onychomycosis in HIV infection. Eur J Dermatol. 1998;8:173–4.
Clegg HW, Prose NS, Greenberg DN. Nail dystrophy in congenital cutaneous candidiasis. Paediatr Dermatol. 2003;20:342–4. doi:10.1046/j.1525-1470.2003.20415.x.
Kwok YKC, Tay YK, Goh CL, Kamarudin A, Koh MT, Seow CS. Epidemiology and in vitro activity of antimycotics against candidal vaginal/skin/nail infections in Singapore. Int J Dermatol. 1998;37:145–9. doi:10.1046/j.1365-4362.1998.00038.x.
Vella Zahra L, Gatt P, Boffa MJ, Borg E, Mifsud E, Scerri L, et al. Characteristics of superficial mycoses in Malta. Int J Dermatol. 2003;42:265–71. doi:10.1046/j.1365-4362.2003.01789.x.
Gunduz T, Metin DY, Sacar T, Hilmioglu S, Baydur H, Inci R, et al. Onychomycosis in primary school children: association with socioeconomic conditions. Mycoses. 2006;49:431–3. doi:10.1111/j.1439-0507.2006.01268.x.
Koklu E, Gunes T, Kurtoglu S, Gokoglu S, Koklu S. Onychomycosis in a premature infant caused by Candida parapsilosis. Pediatr Dermatol. 2007;24:155–6. doi:10.1111/j.1525-1470.2007.00365.x.
Chun DK, Lee UH, Park HS, Choi JC. Onychomycosis in a premature infant caused by Candida tropicalis. J Eur Acad Dermatol Venereol. 2004;18:617–8. doi:10.1111/j.1468-3083.2004.01018.x.
Figueiredo VT, de Assis Santos D, Resende MA, Hamdan JS. Identification and in vitro antifungal susceptibility testing of 200 clinical isolates of Candida spp. responsible for fingernail infections. Mycopathologia. 2007;164:27–33. doi:10.1007/s11046-007-9027-6.
Samaranayake LP. Introduction and historical aspects. In: Samaranayake LP, MacFarlane TW, editors. Oral candidosis. London: Butterworth & Co. (Publishers) Ltd; 1990. p. 1–9.
Daniel CRIII, Gupta AK, Daniel MP, Sullivan S. Candida infection of the nail: role of Candida as a secondary pathogen. Int J Dermatol. 1998;37:904–7. doi:10.1046/j.1365-4362.1998.00473.x.
Güleç AT, Demirbilek M, Seçkin D, Can F, Saray Y, Sarifakioglu E, et al. Superficial fungal infections in 102 renal transplant recipients: a case–control study. J Am Acad Dermatol. 2003;49:187–92. doi:10.1067/S0190-9622(03)00861-2.
Hube B, Naglik J. Extracellular hydrolases. In: Calderone RA, editor. Candida and candidiasis. Washington, DC: ASM Press; 2002. p. 107–22.
Jayatilake JAMS, Samaranayake YH, Samaranayake LP. An ultrastructural and a cytochemical study of candidal invasion of reconstituted human oral epithelium. J Oral Pathol Med. 2005;34:240–6. doi:10.1111/j.1600-0714.2005.00307.x.
Jayatilake JA, Samaranayake YH, Samaranayake LP. A comparative study of candidal invasion in rabbit tongue mucosal explants and reconstituted human oral epithelium. Mycopathologia. 2008;165:373–80. doi:10.1007/s11046-008-9096-1.
Ray TL, Payne CD. Comparative production and rapid purification of Candida acid proteinase from protein-supplemented cultures. Infect Immun. 1990;58:508–14.
Dorschner RA, Lopez-Garcia B, Massie J, Kim C, Gallo RL. Innate immune defense of the nail unit by antimicrobial peptides. J Am Acad Dermatol. 2004;50:343–8. doi:10.1016/j.jaad.2003.09.010.
Lu Q, Jayatilake JAMS, Samaranayake LP, Jin LJ. Hyphal invasion of Candida albicans inhibits the expression of human β-defensins in experimental oral candidiasis. J Invest Dermatol. 2006;126:2049–56. doi:10.1038/sj.jid.5700346.
Morris-Jones R, Gomez BL, Diez S, Uran M, Morris-Jones SD, Casadevall A, et al. Synthesis of melanin pigment by Candida albicans in vitro and during infection. Infect Immun. 2005;73:6147–50. doi:10.1128/IAI.73.9.6147-6150.2005.
Elewski BE. Onychomycosis: pathogenesis, diagnosis, and management. Clin Microbiol Rev. 1998;11:415–29.
Parlak AH, Goksugur N, Karabay O. A case of melanonychia due to Candida albicans. Clin Exp Dermatol. 2006;31:398–400. doi:10.1111/j.1365-2230.2006.02115.x.
Rockwell PG. Acute and chronic paronychia. Am Fam Physician. 2001;63:1113–6.
Baran R, Hay RJ, Tosti A, Haneke E. A new classification of onychomycosis. Br J Dermatol. 1998;139:567–71. doi:10.1046/j.1365-2133.1998.02449.x.
Roberts DT, Taylor WD, Boyle J. Guidelines for treatment of onychomycosis. Br J Dermatol. 2003;148:402–10. doi:10.1046/j.1365-2133.2003.05242.x.
El Sayed F, Ammoury A, Haybe RF, Dhaybi R. Onychomycosis in Lebanon: a mycological survey of 772 patients. Mycoses. 2006;49:216–9. doi:10.1111/j.1439-0507.2006.01224.x.
Liu J, Lei P. Histopathologic and scanning electron microscope examination of the nail and hair in chronic mucocutaneous candidiasis. J Am Acad Dermatol. 2003;49:154–6. doi:10.1067/mjd.2003.335.
Ungpakorn R. Mycoses in Thailand: current concerns. Nippon Ishinkin Gakkai Zasshi. 2005;46:81–6.
Warshaw EM, Nelson D, Carver SM, Zielke GR, Webster N, Lederle FA, et al. A pilot evaluation of pulse itraconazole vs. terbinafine for treatment of Candida toenail onychomycosis. Int J Dermatol. 2005;44:785–8. doi:10.1111/j.1365-4632.2004.02117.x.
Acknowledgments
Authors thank the staff of the microbiology and pathology laboratories at the Faculty of Dental Sciences, University of Peradeniya, Sri Lanka for their excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jayatilake, J.A.M.S., Tilakaratne, W.M. & Panagoda, G.J. Candidal onychomycosis: A Mini-Review. Mycopathologia 168, 165–173 (2009). https://doi.org/10.1007/s11046-009-9212-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-009-9212-x