Abstract
Purpose
Delayed plasma concentration profiles of the active irinotecan metabolite SN-38 were observed in cancer patients with severe renal failure (SRF), even though SN-38 is eliminated mainly via the liver. Here, we examined the plasma concentrations of unbound SN-38 in such patients.
Methods
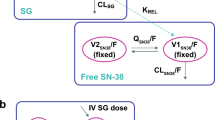
Plasma unbound concentrations were examined by ultrafiltration. Physiologically-based pharmacokinetic (PBPK) models of irinotecan and SN-38 were established to quantitatively assess the principal mechanism for delayed SN-38 elimination.
Results
The area under the plasma unbound concentration-time curve (AUCu) of SN-38 in SRF patients was 4.38-fold higher than that in normal kidney patients. The unbound fraction of SN-38 was also 2.6-fold higher in such patients, partly because SN-38 protein binding was displaced by the uremic toxin 3-carboxy-4-methyl-5-propyl-2-furanpropionate (CMPF). This result was supported by correlation of the unbound fraction of SN-38 with the plasma CMPF concentration, which negatively correlated with renal function. PBPK modeling indicated substantially reduced influx of SN-38 into hepatocytes and approximately one-third irinotecan dose for SRF patients to produce an unbound concentration profile of SN-38 similar to normal kidney patients.
Conclusion
The AUCu of SN-38 in SRF cancer patients is much greater than that of normal kidney patients primarily because of the reduced hepatic uptake of SN-38.








Similar content being viewed by others
Abbreviations
- ABCB1:
-
ATP-binding cassette, sub-family B, member 1
- ABCC2:
-
ATP-binding cassette, sub-family C, member 2
- ABCG2:
-
ATP-binding cassette, sub-family G, member 2
- AUC:
-
Area under the plasma concentration-time curve
- AUCu :
-
Area under the plasma unbound concentration-time curve
- C1,CPT-11 :
-
Plasma concentration of irinotecan
- C1,SN-38 :
-
Plasma concentration of SN-38
- C2,CPT-11 :
-
Concentration of irinotecan in extracellular space
- C2,SN-38 :
-
Concentration of SN-38 in extracellular space
- C3,CPT-11 :
-
Concentration of irinotecan in hepatocyte
- C3,SN-38 :
-
Concentration of SN-38 in hepatocyte
- CES:
-
Carboxylesterase
- CLR,CPT-11 :
-
Renal clearance of irinotecan
- CLR,SN-38 :
-
Renal clearance of SN-38
- CMPF:
-
3-Carboxy-4-methyl-5-propyl-2-furanpropionate
- eGFR:
-
Estimated glomerular filtration rate
- fp,CPT-11 :
-
Unbound fraction of irinotecan in plasma
- fp,SN-38 :
-
Unbound fraction of SN-38 in plasma
- ft,CPT-11 :
-
Unbound fraction of irinotecan in tissue
- ft,SN-38 :
-
Unbound fraction of SN-38 in tissue
- HA:
-
Hippuric acid
- IS:
-
Indoxyl sulfate
- OATPs:
-
Organic anion transporting polypeptides
- PBPK:
-
Physiologically based pharmacokinetic
- PSbile,CPT-11 :
-
Bile excretion clearance of irinotecan
- PSbile,SN-38 :
-
Bile excretion clearance of SN-38
- PSeff,CPT-11 :
-
Efflux clearance of irinotecan from hepatocyte
- PSeff,SN-38 :
-
Efflux clearance of SN-38 from hepatocyte
- PSinf,CPT-11 :
-
Influx clearance of irinotecan into hepatocyte
- PSinf,SN-38 :
-
Influx clearance of SN-38 into hepatocyte
- PSm,CES :
-
CES-mediated metabolic clearance of irinotecan
- PSm,CYP3A :
-
CYP3A-mediated metabolic clearance of irinotecan
- PSm,UGT :
-
UGT-mediated metabolic clearance of SN-38
- PSmBlood,CES :
-
CES-mediated metabolism of irinotecan in blood
- Qh :
-
Hepatatic blood flow rate
- RB,CPT-11 :
-
Blood-to-plasma partition coefficient of irinotecan
- RB,SN-38 :
-
Blood-to-plasma partition coefficient of SN-38
- Rinf :
-
Infusion rate of irinotecan
- SN-38:
-
7-ethyl-10-hydroxycamptothecin
- UGT:
-
UDP-glucuronosyltransferase
- V1,CPT-11,f :
-
Distribution volume of unbound irinotecan
- V1,SN-38,f :
-
Distribution volume of unbound SN-38
- V2 :
-
Volume of extracellular space in the liver
- V3 :
-
Volume of the liver.
References
Fujita K, Sugiura T, Okumura H, Umeda S, Nakamichi N, Watanabe Y, et al. Direct inhibition and down-regulation by uremic plasma components of hepatic uptake transporter for SN-38, an active metabolite of irinotecan, in humans. Pharm Res. 2014;31(1):204–15.
Chu XY, Kato Y, Sugiyama Y. Multiplicity of biliary excretion mechanisms for irinotecan, CPT-11, and its metabolites in rats. Cancer Res. 1997;57(10):1934–8.
Chu XY, Kato Y, Ueda K, Suzuki H, Niinuma K, Tyson CA, et al. Biliary excretion mechanism of CPT-11 and its metabolites in humans: involvement of primary active transporters. Cancer Res. 1998;58(22):5137–43.
Nakatomi K, Yoshikawa M, Oka M, Ikegami Y, Hayasaka S, Sano K, et al. Transport of 7-ethyl-10-hydroxycamptothecin (SN-38) by breast cancer resistance protein ABCG2 in human lung cancer cells. Biochem Biophys Res Commun. 2001;288(4):827–32.
Fujita K, Sunakawa Y, Miwa K, Akiyama Y, Sugiyama M, Kawara K, et al. Delayed elimination of SN-38 in cancer patients with severe renal failure. Drug Metab Dispos. 2011;39(2):161–4.
Vanholder R, De Smet R, Glorieux G, Argiles A, Baurmeister U, Brunet P, et al. European Uremic Toxin Work G. Review on uremic toxins: classification, concentration, and interindividual variability. Kidney Int. 2003;63(5):1934–43.
De Smet R, Dhondt A, Eloot S, Galli F, Waterloos MA, Vanholder R. Effect of the super-flux cellulose triacetate dialyser membrane on the removal of non-protein-bound and protein-bound uraemic solutes. Nephrol Dial Transplant. 2007;22(7):2006–12.
Niwa T. Removal of protein-bound uraemic toxins by haemodialysis. Blood Purification. 2013;35 Suppl 2:20–5.
Mathijssen RH, van Alphen RJ, Verweij J, Loos WJ, Nooter K, Stoter G, et al. Clinical pharmacokinetics and metabolism of irinotecan (CPT-11). Clin Cancer Res. 2001;7(8):2182–94.
Combes O, Barre J, Duche JC, Vernillet L, Archimbaud Y, Marietta MP, et al. In vitro binding and partitioning of irinotecan (CPT-11) and its metabolite, SN-38, in human blood. Invest New Drugs. 2000;18(1):1–5.
de Jong FA, Kitzen JJ, de Bruijn P, Verweij J, Loos WJ. Hepatic transport, metabolism and biliary excretion of irinotecan in a cancer patient with an external bile drain. Cancer Biol Ther. 2006;5(9):1105–10.
Slatter JG, Schaaf LJ, Sams JP, Feenstra KL, Johnson MG, Bombardt PA, et al. Pharmacokinetics, metabolism, and excretion of irinotecan (CPT-11) following I.V. infusion of [(14)C]CPT-11 in cancer patients. Drug Metab Dispos. 2000;28(4):423–33.
Sparreboom A, de Jonge MJ, de Bruijn P, Brouwer E, Nooter K, Loos WJ, et al. Irinotecan (CPT-11) metabolism and disposition in cancer patients. Clin Cancer Res. 1998;4(11):2747–54.
Guemei AA, Cottrell J, Band R, Hehman H, Prudhomme M, Pavlov MV, et al. Human plasma carboxylesterase and butyrylcholinesterase enzyme activity: correlations with SN-38 pharmacokinetics during a prolonged infusion of irinotecan. Cancer Chemother Pharmacol. 2001;47(4):283–90.
Davies B, Morris T. Physiological parameters in laboratory animals and humans. Pharm Res. 1993;10(7):1093–5.
Nishi K, Kobayashi M, Nishii R, Shikano N, Takamura N, Kuga N, et al. Pharmacokinetic alteration of (99m)Tc-MAG3 using serum protein binding displacement method. Nucl Med Biol. 2013;40(3):366–70.
Takamura N, Haruta A, Kodama H, Tsuruoka M, Yamasaki K, Suenaga A, et al. Mode of interaction of loop diuretics with human serum albumin and characterization of binding site. Pharm Res. 1996;13(7):1015–9.
Sakai T, Takadate A, Otagiri M. Characterization of binding site of uremic toxins on human serum albumin. Biol Pharm Bull. 1995;18(12):1755–61.
Mathijssen RH, Verweij J, Loos WJ, de Bruijn P, Nooter K, Sparreboom A. Irinotecan pharmacokinetics-pharmacodynamics: the clinical relevance of prolonged exposure to SN-38. Br J Cancer. 2002;87(2):144–50.
Benet LZ, Hoener BA. Changes in plasma protein binding have little clinical relevance. Clin Pharmacol Ther. 2002;71(3):115–21.
Niemi M, Backman JT, Kajosaari LI, Leathart JB, Neuvonen M, Daly AK, et al. Polymorphic organic anion transporting polypeptide 1B1 is a major determinant of repaglinide pharmacokinetics. Clin Pharmacol Ther. 2005;77(6):468–78.
Kalliokoski A, Neuvonen M, Neuvonen PJ, Niemi M. The effect of SLCO1B1 polymorphism on repaglinide pharmacokinetics persists over a wide dose range. Br J Clin Pharmacol. 2008;66(6):818–25.
Marbury TC, Ruckle JL, Hatorp V, Andersen MP, Nielsen KK, Huang WC, et al. Pharmacokinetics of repaglinide in subjects with renal impairment. Clin Pharmacol Ther. 2000;67(1):7–15.
Zhao P, Vieira Mde L, Grillo JA, Song P, Wu TC, Zheng JH, et al. Evaluation of exposure change of nonrenally eliminated drugs in patients with chronic kidney disease using physiologically based pharmacokinetic modeling and simulation. J Clin Pharmacol. 2012;52(1 Suppl):91S–108S.
Plum A, Muller LK, Jansen JA. The effects of selected drugs on the in vitro protein binding of repaglinide in human plasma. Methods Find Exp Clin Pharmacol. 2000;22(3):139–43.
Zimmerman EI, Hu S, Roberts JL, Gibson AA, Orwick SJ, Li L, et al. Contribution of OATP1B1 and OATP1B3 to the disposition of sorafenib and sorafenib-glucuronide. Clin Cancer Res. 2013;19(6):1458–66.
Meert N, Schepers E, De Smet R, Argiles A, Cohen G, Deppisch R, et al. Inconsistency of reported uremic toxin concentrations. Artif Organs. 2007;31(8):600–11.
Watanabe H, Noguchi T, Miyamoto Y, Kadowaki D, Kotani S, Nakajima M, et al. Interaction between two sulfate-conjugated uremic toxins, p-cresyl sulfate and indoxyl sulfate, during binding with human serum albumin. Drug Metab Dispos: Biol Fate Chem. 2012;40(7):1423–8.
Sakai T, Yamasaki K, Sako T, Kragh-Hansen U, Suenaga A, Otagiri M. Interaction mechanism between indoxyl sulfate, a typical uremic toxin bound to site II, and ligands bound to site I of human serum albumin. Pharm Res. 2001;18(4):520–4.
Pavone B, Sirolli V, Giardinelli A, Bucci S, Forli F, Di Cesare M, et al. Plasma protein carbonylation in chronic uremia. J Nephrol. 2011;24(4):453–64.
Perna AF, Satta E, Acanfora F, Lombardi C, Ingrosso D, De Santo NG. Increased plasma protein homocysteinylation in hemodialysis patients. Kidney Int. 2006;69(5):869–76.
ACKNOWLEDGMENTS AND DISCLOSURES
This study was supported in part by a Grant-in-Aid for Scientific Research (C) [23590198 to K.F.] from the Japan Society for the Promotion of Science (JSPS), in part by a Grant-in-Aid for Scientific Research (C) [26460205 to K.F.] and Grant-in-Aid for Young Scientists (B) [26860099 to Y.M.] from the same society, and in part by a Japanese Association of Dialysis Physicians Grant [JADP Grant 2014–1 to K.F.].
We have no conflict of interest to be disclosed.
Author contributions
Y.M., H.O., Y.W., H.S., Yu.S., K.S., K.K., Y.A., Ya.S., Ma. K., and Mu. K. performed the research. K.F., Y.M., H.O., and Y.A. analyzed the data. K.F., Y.M., and Y.K. wrote the manuscript. K.F. and Y.K. designed the research.
Author information
Authors and Affiliations
Corresponding authors
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 67 kb)
Rights and permissions
About this article
Cite this article
Fujita, Ki., Masuo, Y., Okumura, H. et al. Increased Plasma Concentrations of Unbound SN-38, the Active Metabolite of Irinotecan, in Cancer Patients with Severe Renal Failure. Pharm Res 33, 269–282 (2016). https://doi.org/10.1007/s11095-015-1785-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-015-1785-0