Abstract
Purpose
The apnea–hypopnea index (AHI) is used to grade obstructive sleep apnea (OSA) into mild, moderate, and severe forms. Obstructive events are most common in the supine position. The amount of supine sleep thus influences total AHI. Our aim was to determine the prevalence of position-dependent OSA (POSA) and its relation to OSA severity classification as recommended by the American Academy of Sleep Medicine (AASM).
Methods
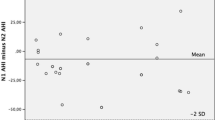
Two hundred sixty-five subjects were recruited from primary care hypertension clinics. Whole-night respiratory recordings were performed to determine the AHI in the supine and non-supine positions, respectively. POSA was defined as supine AHI twice the non-supine AHI with supine AHI ≥5.
Results
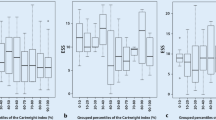
Fifty-three percent had POSA, 22% had non-position-dependent OSA, and 25% had normal respiration. By AASM classification, 81 subjects did not have OSA, but 42% of them had some degree of obstruction when supine, and 5 subjects would have been classified as moderate–severe if they had only slept supine. Conversely, of the 53 classified as mild OSA, 30% would have changed to a more severe classification if they had exclusively slept supine.
Conclusions
POSA was common both in subjects that by AASM classification had OSA as well as those without. The severity of OSA, as defined by AASM, could be dependent on supine time in a substantial amount of subjects.


Similar content being viewed by others
References
Epstein LJ, Kristo D, Strollo PJ Jr, Friedman N, Malhotra A, Patil SP, Ramar K, Rogers R, Schwab RJ, Weaver EM, Weinstein MD (2009) Adult obstructive sleep apnea task force of the American Academy of Sleep Medicine. Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. J Clin Sleep Med 5:263–276
Cartwright RD (1984) Effect of sleep position on sleep apnea severity. Sleep 7:110–114
Oksenberg A, Silverberg DS, Arons E, Radwan H (1997) Positional vs nonpositional obstructive sleep apnea patients: anthropomorphic, nocturnal polysomnographic, and multiple sleep latency test data. Chest 112:629–639
Aarab G, Lobbezoo F, Hamburger HL, Naeije M (2009) Variability in the apnea-hypopnea index and its consequences for diagnosis and therapy evaluation. Respiration 77:32–37
Ahmadi N, Shapiro GK, Chung SA, Shapiro CM (2009) Clinical diagnosis of sleep apnea based on single night of polysomnography vs. two nights of polysomnography. Sleep Breath 13:221–226
Bittencourt LR, Suchecki D, Tufik S, Peres C, Togeiro SM, Bagnato MC, Nery LE (2001) The variability of the apnoea-hypopnoea index. J Sleep Res 10:245–251
Gouveris H, Selivanova O, Bausmer U, Goepel B, Mann W (2010) First-night-effect on polysomnographic respiratory sleep parameters in patients with sleep-disordered breathing and upper airway pathology. Eur Arch Otorhinolaryngol 267:1449–1453
Le Bon O, Hoffmann G, Tecco J, Staner L, Noseda A, Pelc I, Linkowski P (2000) Mild to moderate sleep respiratory events: one negative night may not be enough. Chest 118:353–359
Chung JW, Enciso R, Levendowski DJ, Morgan TD, Westbrook PR, Clark GT (2010) Treatment outcomes of mandibular advancement devices in positional and nonpositional OSA patients. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 109:724–731
Hoffstein V (2007) Review of oral appliances for treatment of sleep-disordered breathing. Sleep Breath 11:1–22
Marklund M, Persson M, Franklin KA (1998) Treatment success with a mandibular advancement device is related to supine-dependent sleep apnea. Chest 114:1630–1635
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14:540–545
Faul F, Erdfelder E, Buchner A, Lang A-G (2009) Statistical power analyses using G*Power 3.1: tests for correlation and regression analyses. Behav Res Methods 41:1149–1160
Pevernagie DA, Shepard JW Jr (1992) Relations between sleep stage, posture and effective nasal CPAP levels in OSA. Sleep 15:162–167
Sahlin C, Franklin KA, Stenlund H, Lindberg E (2009) Sleep in women: normal values for sleep stages and position and the effect of age, obesity, sleep apnea, smoking, alcohol and hypertension. Sleep Med 10:1025–1030
Ng SS, Chan TO, To KW, Ngai J, Tung A, Ko FW, Hui DS (2010) Validation of Embletta portable diagnostic system for identifying patients with suspected obstructive sleep apnoea syndrome (OSAS). Respirology 15:336–342
Franklin KA, Svanborg E (2000) The accuracy of subjective sleep time in sleep apnoea recordings. Respir Med 94:569–573
Svanborg E, Larsson H, Carlsson-Nordlander B, Pirskanen R (1990) A limited diagnostic investigation for obstructive sleep apnea syndrome. Oximetry and static charge sensitive bed. Chest 98:1341–1345
Metersky ML, Castriotta RJ (1996) The effect of polysomnography on sleep position: possible implications on the diagnosis of positional obstructive sleep apnea. Respiration 63:283–287
Svanborg E (2005) Impact of obstructive apnea syndrome on upper airway respiratory muscles. Respir Physiol Neurobiol 147:263–272
Larsson H, Carlsson-Nordlander B, Lindblad LE, Norbeck O, Svanborg E (1992) Temperature thresholds in the oropharynx of patients with obstructive sleep apnea syndrome. Am Rev Respir Dis 146:1246–1249
Sunnergren O, Broström A, Svanborg E (2011) Soft palate sensory neuropathy in the pathogenesis of obstructive sleep apnea. Laryngoscope 121:451–456
Acknowledgments
This work was supported by the Swedish Heart and Lung Foundation, Stockholm, Sweden; Futurum—the Academy for Healthcare, County Council, Jönköping, Sweden; and Acta Oto—Laryngologica, Stockholm, Sweden.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sunnergren, O., Broström, A. & Svanborg, E. Positional sensitivity as a confounder in diagnosis of severity of obstructive sleep apnea. Sleep Breath 17, 173–179 (2013). https://doi.org/10.1007/s11325-012-0666-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-012-0666-6