Abstract
Purpose
Few studies have examined the co-morbidity between insomnia and sleep-disordered breathing in the clinical setting. This study evaluated treatment-seeking insomnia patients and their self-report of sleep breathing complaints.
Methods
A retrospective chart review was conducted on 1,035 consecutive treatment-seeking, chronic insomnia patients who reported insomnia as their primary problem upon seeking care at a private, community-based sleep medical center. Measurements included the insomnia severity index, standard subjective sleep measures as well as rankings, attributions, and self-reports about sleep breathing disorders, problems, and symptoms.
Results
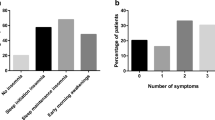
A total of 1,035 adult, treatment-seeking insomnia patients indicated insomnia interfered with daytime functioning, and their average insomnia severity was in the range of a clinically relevant problem: total sleep time (5.50 h, SD = 1.60), sleep efficiency (71.05 %, SD = 18.26), wake time after sleep onset (120.70 min, SD = 92.56), and an insomnia severity index (18.81, SD = 5.09). Of these 1,035 insomnia patients, 42 % also ranked a sleep breathing disorder among their list of reasons for seeking treatment, another 13 % revealed a concern about a sleep breathing problem, and another 26 % reported awareness of sleep breathing symptoms. Only 19 % of this clinical insomnia sample reported no awareness or concerns about sleep breathing disorders, problems, or symptoms. A greater proportion of men than women reported significantly more sleep breathing disorders, problems, or symptoms.
Conclusions
Sleep breathing complaints were extremely common among a large sample of treatment-seeking, self-identified, adult chronic insomnia patients. Prospective prevalence research is needed to corroborate or revise these findings, and polysomnography should be considered in appropriate cohorts to determine the clinical relevance of treatment-seeking chronic insomnia patients' sleep breathing complaints.

Similar content being viewed by others
References
Edinger JD, Hoelscher TJ, Webb MD, Marsh GR, Radtke RA, Erwin CW (1989) Polysomnographic assessment of DIMS: empirical evaluation of its diagnostic value. Sleep 12:315–322
Jacobs EA, Reynolds CF III, Kupfer DJ, Lovin PA, Ehrenpreis AB (1988) The role of polysomnography in the differential diagnosis of chronic insomnia. Am J Psychiatry 145:346–349
Iber C, A-ISCAQS (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. American Academy of Sleep Medicine, Westchester
Cronlein T, Geisler P, Langguth B, Eichhammer P, Jara C, Pieh C, Zulley J, Hajak G (2012) Polysomnography reveals unexpectedly high rates of organic sleep disorders in patients with prediagnosed primary insomnia. Sleep Breath (in press)
Littner M, Hirshkowitz M, Kramer M, Kapen S, Anderson WM, Bailey D, Berry RB, Davila D, Johnson S, Kushida C, Loube DI, Wise M, Woodson BT (2003) Practice parameters for using polysomnography to evaluate insomnia: an update. Sleep 26:754–760
Lichstein KL, Riedel BW, Lester KW, Aquillard RN (1999) Occult sleep apnea in a recruited sample of older adults with insomnia. J Consult Clin Psychol 67:405–410
Krakow B, Melendrez D, Pedersen B, Johnston L, Hollifield M, Germain A, Koss M, Warner TD, Schrader R (2001) Complex insomnia: insomnia and sleep-disordered breathing in a consecutive series of crime victims with nightmares and PTSD. Biol Psychiatry 49:948–953
Guilleminault C, Palombini L, Poyares D, Chowdhuri S (2002) Chronic insomnia, postmenopausal women, and sleep disordered breathing: part 1. Frequency of sleep disordered breathing in a cohort. J Psychosom Res 53:611–615
Krakow B, Ulibarri VA, Romero EA (2010) Patients with treatment-resistant insomnia taking nightly prescription medications for sleep: a retrospective assessment of diagnostic and treatment variables. Prim Care Companion J Clin Psychiatry 12(4)
Krakow B, Melendrez D, Ferreira E, Clark J, Warner TD, Sisley B, Sklar D (2001) Prevalence of insomnia symptoms in patients with sleep-disordered breathing. Chest 120:1923–1929
Krakow B, Melendrez D, Lee SA, Warner TD, Clark JO, Sklar D (2004) Refractory insomnia and sleep-disordered breathing: a pilot study. Sleep Breath 8:15–29
Krakow B (2004) An emerging interdisciplinary sleep medicine perspective on the high prevalence of co-morbid sleep-disordered breathing and insomnia. Sleep Med 5:431–433
Krakow B, Melendrez D, Sisley B, Warner TD, Krakow J, Leahigh L, Lee S (2006) Nasal dilator strip therapy for chronic sleep-maintenance insomnia and symptoms of sleep-disordered breathing: a randomized controlled trial. Sleep Breath 10:16–28
Krakow B, Ulibarri VA, Romero E (2010) Persistent insomnia in chronic hypnotic users presenting to a sleep medical center: a retrospective chart review of 137 consecutive patients. J Nerv Ment Dis 198:734–741
American Academy of Sleep Medicine (2005) International classification of sleep disorders: diagnostic and coding manual, 2nd edn. American Academy of Sleep Medicine, Westchester, pp 51–55
Bastien CH, Vallieres A, Morin CM (2001) Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med 2:297–307
Larsson LG, Lindberg A, Franklin KA, Lundback B (2003) Gender differences in symptoms related to sleep apnea in a general population and in relation to referral to sleep clinic. Chest 124:204–211
Luyster FS, Buysse DJ, Strollo PJ Jr (2010) Comorbid insomnia and obstructive sleep apnea: challenges for clinical practice and research. J Clin Sleep Med 6:196–204
Wickwire EM, Collop NA (2010) Insomnia and sleep-related breathing disorders. Chest 137:1449–1463
Beneto A, Gomez-Siurana E, Rubio-Sanchez P (2009) Comorbidity between sleep apnea and insomnia. Sleep Med Rev 13:287–293
Al Jawder SE, Bahammam AS (2011) Comorbid insomnia in sleep-related breathing disorders: an under-recognized association. Sleep Breath 16:295–304
Subramanian S, Guntupalli B, Murugan T, Bopparaju S, Chanamolu S, Casturi L, Surani S (2011) Gender and ethnic differences in prevalence of self-reported insomnia among patients with obstructive sleep apnea. Sleep Breath 15:711–715
Krell SB, Kapur VK (2005) Insomnia complaints in patients evaluated for obstructive sleep apnea. Sleep Breath 9:104–110
Lavie P (2007) Insomnia and sleep-disordered breathing. Sleep Med 8(Suppl 4):S21–S25
Krakow B, Melendrez D, Warner TD, Dorin R, Harper R, Hollifield M (2002) To breathe, perchance to sleep: sleep-disordered breathing and chronic insomnia among trauma survivors. Sleep Breath 6:189–202
Series F (2009) Can improving sleep influence sleep-disordered breathing? Drugs 69(Suppl 2):77–91
Ohayon MM (1997) Prevalence of DSM-IV diagnostic criteria of insomnia: distinguishing insomnia related to mental disorders from sleep disorders. J Psychiatr Res 31:333–346
Acknowledgments
This is not an industry-supported study. Dr. Krakow operates six websites providing education and offering products and services for sleep disorder patients, markets and sells three books for sleep disorder patients, owns and operates a commercial sleep center, and is the president of a non-profit sleep research center which has received support from ConAlma, Respironics, GlaxoSmithKlein, and Covidien. He has participated in speaking engagements supported by ResMed and Respironics. Mr. Ulibarri has indicated no financial conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Krakow, B., Ulibarri, V.A. Prevalence of sleep breathing complaints reported by treatment-seeking chronic insomnia disorder patients on presentation to a sleep medical center: a preliminary report. Sleep Breath 17, 317–322 (2013). https://doi.org/10.1007/s11325-012-0694-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-012-0694-2