Abstract
Purpose
This study investigated gender differences in the effect of comorbid insomnia symptom on depression, anxiety, fatigue, daytime sleepiness, and quality of life in patients with obstructive sleep apnea. There are gender differences in the presentation of obstructive sleep apnea. However, the influence of gender on the presentation of comorbid insomnia symptom and obstructive sleep apnea is not known.
Methods
Allparticipantsperformed overnightpolysomnography and completed a battery of questionnaires including Beck Depression Inventory, State-Trait Anxiety Inventory, Multidimensional Fatigue Inventory, Epworth Sleepiness Scale, and Short Form-36 Health Survey. Insomnia symptom was defined as present if a patient had any insomnia complaints longer than 1 month and at least one time per week.
Results
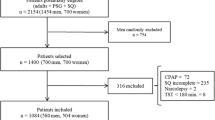
Six hundred fifty-five adult patients with obstructive sleep apnea were enrolled; 233 (35.5 %) reported comorbid insomnia symptom with obstructive sleep apnea. The severity of obstructive sleep apnea was not related to comorbid insomnia symptom. Based on linear regression, women had higher depression, fatigue, and daytime sleepiness and lower health-related quality of life than men (all, p < 0.05). The presence of insomnia symptom had negative effects on fatigue (p = 0.005) and quality of life only (p = 0.015) in men but not in women when taking gender-by-insomnia interaction into consideration. There were significant differences in polysomnography-based sleep architecture between the obstructive sleep apnea-only and obstructive sleep apnea–insomnia groups, but only in the subgroup of men.
Conclusions
Men are more prone to the negative impact of comorbid insomnia symptom and obstructive sleep apnea on their level of fatigue and quality of life than women.
Similar content being viewed by others
References
Cho YW, Shin WC, Yun CH, Hong SB, Kim J, Earley CJ (2009) Epidemiology of insomnia in Korean adults: prevalence and associated factors. J Clin Neurol 5:20–23
Punjabi NM (2008) The epidemiology of adult obstructive sleep apnea. Proc Am Thorac Soc 5:136–143
Chung KF (2005) Insomnia subtypes and their relationships to daytime sleepiness in patients with obstructive sleep apnea. Respiration 72:460–465
Krakow B, Melendrez D, Ferreira E, Clark J, Warner TD, Sisley B, Sklar D (2001) Prevalence of insomnia symptoms in patients with sleep-disordered breathing. Chest 120:1923–1929
Smith S, Sullivan K, Hopkins W, Douglas J (2004) Frequency of insomnia report in patients with obstructive sleep apnoea hypopnea syndrome (OSAHS). Sleep Med 5:449–456
Buckley TM, Schatzberg AF (2005) On the interactions of the hypothalamic-pituitary-adrenal (HPA) axis and sleep: normal HPA axis activity and circadian rhythm, exemplary sleep disorders. J Clin Endocrinol Metab 90:3106–3114
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342:1378–1384
Yun CH, Jung KH, Chu K, Kim SH, Ji KH, Park HK, Kim HC, Lee ST, Lee SK, Roh JK (2010) Increased circulating endothelial microparticles and carotid atherosclerosis in obstructive sleep apnea. J Clin Neurol 6:89–98
Baldwin CM, Griffith KA, Nieto FJ, O'Connor GT, Walsleben JA, Redline S (2001) The association of sleep-disordered breathing and sleep symptoms with quality of life in the Sleep Heart Health Study. Sleep 24:96–105
Noh HJ, Joo EY, Kim ST, Yoon SM, Koo DL, Kim D, Lee GH, Hong SB (2012) The relationship between hippocampal volume and cognition in patients with chronic primary insomnia. J Clin Neurol 8:130–138
Luyster FS, Buysse DJ, Strollo PJ (2010) Comorbid insomnia and obstructive sleep apnea: challenges for clinical practice and research. J Clin Sleep Med 6:196–204
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328:1230–1235
Young T, Hutton R, Finn L, Badr S, Palta M (1996) The gender bias in sleep apnea diagnosis. Are women missed because they have different symptoms? Arch Intern Med 156:2445–2451
Shepertycky MR, Banno K, Kryger MH (2005) Differences between men and women in the clinical presentation of patients diagnosed with obstructive sleep apnea syndrome. Sleep 28:309–314
Brostrom A, Johansson P, Stromberg A, Albers J, Martensson J, Svanborg E (2007) Obstructive sleep apnoea syndrome—patients’ perceptions of their sleep and its effects on their life situation. J Adv Nurs 57:318–327
American Academy of Sleep Medicine (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. American Academy of Sleep Medicine, Westchester. http://www.nswo.nl/userfiles/files/AASM%20-%20Manual%20for%20the%20Scoring%20ofSleep%20and%20Associted%20Events%20-%2005-2007_2.pdf. Accessed 15 Dec 2012
Lee YH, Song JY (1991) A study of the reliability and the validity of the BDI, SDS, and MMPI-D scales. J Korean Neuropsychiatr Assoc 10:93–113
Kim JT, Shin DK (1978) A study based on the standardization of the STAI for Korea. Recent Medicine 2:69–75
Smets EM, Garssen B, Bonke B, De Haes JC (1995) The Multidimensional Fatigue Inventory (MFI) psychometric qualities of an instrument to assess fatigue. J Psychosom Res 39:315–325
Cho YW, Lee JH, Son HK, Lee SH, Shin C, Johns MW (2011) The reliability and validity of the Korean version of the Epworth sleepiness scale. Sleep Breath 15:377–384
Han CW, Lee EJ, Iwaya T, Kataoka H, Kohzuki M (2004) Development of the Korean version of Short-Form 36-Item Health Survey: health related QOL of healthy elderly people and elderly patients in Korea. Tohoku J Exp Med 203:189–194
Krell SB, Kapur VK (2005) Insomnia complaints in patients evaluated for obstructive sleep apnea. Sleep Breath 9:104–110
Kessler RC, McGonagle KA, Swartz M, Blazer DG, Nelson CB (1993) Sex and depression in the National Comorbidity Survey. I: lifetime prevalence, chronicity and recurrence. J Affect Disord 29:85–96
Shochat T, Umphress J, Israel AG, Ancoli-Israel S (1999) Insomnia in primary care patients. Sleep 22(Suppl 2):S359–365
Mohsenin V (2001) Gender differences in the expression of sleep-disordered breathing: role of upper airway dimensions. Chest 120:1442–1447
O'Connor C, Thornley KS, Hanly PJ (2000) Gender differences in the polysomnographic features of obstructive sleep apnea. Am J Respir Crit Care Med 161:1465–1472
Beneto A, Gomez-Siurana E, Rubio-Sanchez P (2009) Comorbidity between sleep apnea and insomnia. Sleep Med Rev 13:287–293
Bixler EO, Vgontzas AN, Lin HM, Vela-Bueno A, Kales A (2002) Insomnia in central Pennsylvania. J Psychosom Res 53:589–592
Bjornsdottir E, Janson C, Gislason T, Sigurdsson JF, Pack AI, Gehrman P, Benediktsdottir B (2012) Insomnia in untreated sleep apnea patients compared to controls. J Sleep Res 21:131–138
Gooneratne NS, Gehrman PR, Nkwuo JE, Bellamy SL, Schutte-Rodin S, Dinges DF, Pack AI (2006) Consequences of comorbid insomnia symptoms and sleep-related breathing disorder in elderly subjects. Arch Intern Med 166:1732–1738
Krakow B, Melendrez D, Lee SA, Warner TD, Clark JO, Sklar D (2004) Refractory insomnia and sleep-disordered breathing: a pilot study. Sleep Breath 8:15–29
Krakow B, Melendrez D, Sisley B, Warner TD, Krakow J, Leahigh L, Lee S (2006) Nasal dilator strip therapy for chronic sleep-maintenance insomnia and symptoms of sleep-disordered breathing: a randomized controlled trial. Sleep Breath 10:16–28
Conflict of interest
All the authors have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, Mh., Lee, SA., Lee, Gh. et al. Gender differences in the effect of comorbid insomnia symptom on depression, anxiety, fatigue, and daytime sleepiness in patients with obstructive sleep apnea. Sleep Breath 18, 111–117 (2014). https://doi.org/10.1007/s11325-013-0856-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-013-0856-x