Abstract
Purpose
Although obstructive sleep apnea (OSA) syndrome is a common disorder; the connection between OSA and smoking habits is still controversial. In this study, we investigated whether active smoking and pack × years of smoking have an impact on the severity of the disease regarding the patients with OSA.
Methods
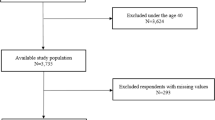
This study included 964 patients referred to the Sleep Disorders Clinic between 01.01.2007 and 01.03.2013 with an overnight polysomnographic diagnosis of OSA. The correlation between smoking habits and polysomnographic parameters has been studied in detail.
Results
There were 684 male (79 %) and 280 female (21 %) patients, 367 (50.6 %) of whom never smoked. Of all, 20.7 % of the smokers were current smokers (n = 150) while 28.2 % were former smokers (n = 208). Active smokers had a mean age of 49.53 (SD 10.17) while former smokers and never smokers had a mean age of 51.37 (SD 10.62), 54.2 (SD 11.56), respectively, which was statistically significant (p < 0.0001). There was a significant male predominance in smoking (p < 0.0001). In addition, male patients displayed more severe OSA than female patients. (p = 0.001). Desaturation time during sleep was found to be significantly longer in the group of former smokers in comparison to never smokers (73.84 SD 97.1–52 SD 85.8) (p = 0.005). Besides, as the apnea hypopnea index increased, the mean pack × years rose significantly (p = 0.01). Severe smokers compared to mild smokers had higher AHI, lower NREM 3, higher NREM1-2 stages (p = 0. 017, p = 0.007, p < 0.001).
Conclusion
In this study, we found that cigarette smoking was associated with early age disease; heavy smokers had more severe OSA.




Similar content being viewed by others
References
Guilleminault C, Eldridge FL, Dement WC (1973) Insomnia with sleep apnea: a new syndrome. Science 31:856–858
Whitney CW, Enright PL, Newman AB, Bonekat W, Foley D, Quan SF (1998) Correlates of daytime sleepiness in 4578 elderly persons: the Cardiovascular Health Study. Sleep 21:27–36
Lindberg E, Gislason T (2000) Epidemiology of sleep-related obstructive breathing. Sleep Med Rev 4:411–433
Greenberg GD, Watson RK, Deptula D (1987) Neuropsychological dysfunction in sleep apnea. Sleep 10:254–262
Parati G, Lombardi C, Narkiewicz K (2007) Sleep apnea: epidemiology, pathophysiology, and relation to cardiovascular risk. Am J Physiol Regul Integr Comp Physiol 293:1671–1683
Peled N, Kassirer M, Shitrit D, Kogan Y, Shlomi D, Berliner AS, Kramer MR (2007) The association of OSA with insulin resistance, inflammation and metabolic syndrome. Respir Med 101:1696–1701
Bearpark H, Elliott L, Grunstein R, Cullen S, Schneider H, Althaus W, Sullivan C (1995) Snoring and sleep apnea. A population study in Australian men. Am J Respir Crit Care Med 151:1459–1465
Franklin KA, Gislason T, Omenaas E et al (2004) The influence of active and passive smoking on habitual snoring. Am J Respir Crit Care Med 170:799–803
Lindberg E, Taube A, Janson C, Gislason T, Svardsudd K, Boman G (1998) A 10-year follow-up of snoring in men. Chest 114:1048–1055
Wetter DW, Young TB, Bidwell TR, Badr MS, Palta M (1994) Smoking as a risk factor for sleep-disordered breathing. Arch Intern Med 154:2219–2224
Krishnan V, Dixon-Williams S, Thornton JD (2014) Where there is smoke there is sleep apnea: exploring the relationship between smoking and sleep apnea. Chest 146:1673–1680
Iber C, Ancoli-Israel S, Chesson AL, Quan SF (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology, and technical specifications. Westchester, Ill, USA
The International Classification of Sleep Disorders: Diagnostic and Coding Manual (2005) 2nd edition. Westchester, Ill, USA
Berg S (2008) Obstructive sleep apnea syndrome: current status. Clin Respir J. doi:10.1111/j.1752-699X.2008.00076.x
Punjabi NM (2008) The epidemiology of adult obstructive sleep apnea. Proc Am Thorac Soc. doi:10.1513/pats.200709-155MG
Johns MW (1994) Sleepiness in different situations measured by the Epworth sleepiness scale. Sleep 17:703–710
Bloom JW, Kaltenborn WT, Quan SF (1988) Risk factors in a general population for snoring Importance of cigarette smoking and obesity. Chest 93:678–683
Ekici M, Ekici A, Keles H, Akin A, Karlidag A, Tunckol M, Kocyigit P (2008) Risk factors and correlates of snoring and observed apnea. Sleep Med 9:290–296
Lavie L, Lavie P (2008) Smoking interacts with sleep apnea to increase cardiovascular risk. Sleep Med 9:247–253
Franklin KA, Gislason T, Omenaas E et al (2004) The influence of active and passive smoking on habitual snoring. Am J Respir Crit Care Med 170:799–803
Kim KS, Kim JH, Park SY, Won HR, Lee HJ, Yang HS, Kim HJ (2012) Smoking induces oropharyngeal narrowing and increases the severity of obstructive sleep apnea syndrome. J Clin Sleep Med. doi:10.5664/jcsm.2024
Dessi P, Sambuc R, Moulin G, Ledoray V, Cannoni M (1994) Effect of heavy smoking on nasal resistance. Acta Otolaryngol 114:305–310
Young T, Finn L, Kim H (1997) Nasal obstruction as a risk factor for sleep-disordered breathing. The University Of Wisconsin Sleep and Respiratory Research Group. J Allergy Clin Immunol 99:757–762
Hadar T, Yaniv E, Shvili Y, Koren R, Shvero J (2009) Histopathological changes of the nasal mucosa induced by smoking. Inhal Toxicol 21:1119–1122
Cohen NA, Zhang S, Sharp DB, Tamashiro E, Chen B, Sorscher EJ et al (2009) Cigarette smoke condensate inhibits transepithelial chloride transport and ciliary beat frequency. Laryngoscope 119:2269–2274
Anthonisen NR, Connett JE, Murray RP (2002) Smoking and lung function of Lung Health Study participants after 11 years. Am J Respir Crit Care Med 166:675–679
Arcavi L, Benowitz NL (2004) Cigarette smoking and infection. Arch Intern Med 164:2206–2216
Hızlı Ö, Özcan M, Ünal A (2013) Evaluation of comorbidities in patients with OSAS and simple snoring. Scientific World Journal. doi:10.1155/2013/709292
İtil O (2000) Akciğer kanserlerinin epidemiyolojisi ve etyolojisi. In: Haydaroğlu A (ed) Akciğer kanserleri: Tanı ve tedavi. Ege Üniversitesi Basımevi, İzmir, pp 15–34
Chervin RD, Guilleminault C (1996) Obstructive sleep apnea and related disorders. Neurol Clin 14:583–609
Sahlin C, Franklin KA, Stenlund H, Lindberg E (2009) Sleep in women: normal values for sleep stages and position and the effect of age, obesity, sleep apnea, smoking, alcohol and hypertension. Sleep Med. doi:10.1016/j.sleep.2008.12.008
Hukkanen J, Jacob P, Benowitz NL (2005) Metabolism and disposition kinetics of nicotine. Pharmacol Rev. doi:10.1124/pr.57.1.3
Aksu K, Firat Güven S, Aksu F, Ciftci B, Ulukavak Ciftci T, Aksaray S, Sipit T, Peker Y (2009) Obstructive sleep apnea, cigarette smoking and plasma orexin-A in a sleep clinic cohort. J Int Med Res 37:331–340
Casasola GG, Álvarez-Sala JL, Marqués JA, Sánchez-Alarcos JM, Tashkin DP, Espinos D (2002) Cigarette smoking behavior and respiratory alterations during sleep in a healthy population. Sleep Breath 6:19–24
Conway SG, Roizenblatt SS, Palombini L, Castro LS, Bittencourt LR, Silva RS et al (2008) Effect of smoking habits on sleep. Braz J Med Biol Res 41:722–727
Lewis KW, Bosque EM (1995) Deficient hypoxia awakening response in infants of smoking mothers: possible relationship to sudden infant death syndrome. J Pediatr 127:691–699
Fewell JE, Smith FG (1998) Perinatal nicotine exposure impairs ability of newborn rats to autoresuscitate from apnea during hypoxia. J Appl Physiol 85:2066–2074
Hafström O, Milerad J, Sundell HW (2002) Prenatal nicotine exposure blunts the cardiorespiratory response to hypoxia in lambs. Am J Respir Crit Care Med 166:1544–1549
Wetter DW, Young TB (1994) The relation between cigarette smoking and sleep disturbance. Prev Med 23:328–334
Zhang L, Samet J, Caffo B, Punjabi NM (2006) Cigarette smoking and nocturnal sleep architecture. Am J Epidemiol 164:529–537
Zhang L, Samet J, Caffo B, Bankman I, Punjabi NM (2008) Power spectral analysis of EEG activity during sleep in cigarette smokers. Chest 133:427–432
Conflicts of interest
The authors declared that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Yelda Varol holds a degree in medicine, Dr. Suat Seren Chest Diseases and Chest Surgery Training and Research Hospital.
Ceyda Anar holds a degree in medicine, Dr. Suat Seren Chest Diseases and Chest Surgery Training and Research Hospital.
Ozlem Egemen Tuzel holds a degree in medicine, Dr. Suat Seren Chest Diseases and Chest Surgery Training and Research Hospital.
Salih Zeki Guclu holds a degree in medicine, Dr. Suat Seren Chest Diseases and Chest Surgery Training and Research Hospital.
Zeynep Zeren Ucar holds a degree in medicine, Dr. Suat Seren Chest Diseases and Chest Surgery Training and Research Hospital.
Rights and permissions
About this article
Cite this article
Varol, Y., Anar, C., Tuzel, O.E. et al. The impact of active and former smoking on the severity of obstructive sleep apnea. Sleep Breath 19, 1279–1284 (2015). https://doi.org/10.1007/s11325-015-1159-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-015-1159-1