Abstract
Background
This study aimed to determine the prevalence of clinical depression as defined by ICD-10 criteria in all patients with obstructive sleep apnea (OSA) referred to a sleep center.
Methods
Prospective general and sleep evaluations were conducted in 447 consecutive patients referred to our sleep center during the first quarter of 2008. Inclusion criteria were Apnea Hypopnea Index (AHI) > 9, completion of the Beck Depression Inventory (BDI-II) with a score ≥14 and World Health Organization WHO-5 Well-Being Index (WHO-5) ≤ 13. The subsequent psychiatric examination according to ICD-10 criteria was performed by in-house clinical sleep specialists.
Results
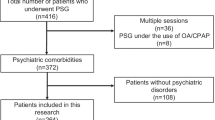
A total of 447 patients were surveyed, of whom 322 had an AHI > 9. Out of these, 85 met the combined screening criterion BDI II ≥ 14 and WHO-5 ≤ 13.
Eighty-one patients underwent a psychiatric examination by psychiatric sleep specialists. In 21.5 % of the sample, clinical depression was diagnosed. Other complaints existed in 12 % (n = 10); 7 % (n = 6) of patients had a different psychiatric diagnosis.
Conclusions
The prevalence of clinical depression according to ICD-10 criteria in a selected clinical sample (referred to the sleep center) was 21.5 %. Mood scales tend to overestimate complaints as compared to psychiatric consultation. Interdisciplinary cooperation is recommended for both OSA patients with symptoms of depression and depressed patients with treatment resistance.

Similar content being viewed by others
References
Young THRFLBSPM (1996) The gender bias in sleep apnea diagnosis: are women missed because they have different symptoms? Arch Intern Med 156(21):2445–2451. doi:10.1001/archinte.1996.00440200055007
Young T, Palta M, Dempsey J et al (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17):1230–1235. doi:10.1056/NEJM199304293281704
Guilleminault C, Eldridge FL, Tilkian A et al (1977) Sleep apnea syndrome due to upper airway obstruction: a review of 25 cases. Arch Intern Med 137(3):296–300
Reynolds CF3, Kupfer DJ, McEachran AB et al (1984) Depressive psychopathology in male sleep apneics. J Clin Psychiatry 45(7):287–290
Reynolds CF3, Coble PA, Spiker DG et al (1982) Prevalence of sleep apnea and nocturnal myoclonus in major affective disorders: clinical and polysomnographic findings. J Nerv Ment Dis 170(9):565–567
Millman RP, Fogel BS, McNamara ME et al (1989) Depression as a manifestation of obstructive sleep apnea: reversal with nasal continuous positive airway pressure. J Clin Psychiatry 50(9):348–351
Barnes M, McEvoy RD, Banks S et al (2004) Efficacy of positive airway pressure and oral appliance in mild to moderate obstructive sleep apnea. Am J Respir Crit Care Med 170(6):656–664. doi:10.1164/rccm.200311-1571OC
Goncalves MA, Guilleminault C, Ramos E et al (2005) Erectile dysfunction, obstructive sleep apnea syndrome and nasal CPAP treatment. Sleep Med 6(4):333–339. doi:10.1016/j.sleep.2005.03.001
Goncalves MA, Paiva T, Ramos E et al (2004) Obstructive sleep apnea syndrome, sleepiness, and quality of life*. Chest 125(6):2091–2096. doi:10.1378/chest.125.6.2091
Ishman SL, Cavey RM, Mettel TL et al (2010) Depression, sleepiness, and disease severity in patients with obstructive sleep apnea. Laryngoscope 120(11):2331–2335. doi:10.1002/lary.21111
McCall WV, Harding D, O’Donovan C (2006) Correlates of depressive symptoms in patients with obstructive sleep apnea. J Clin Sleep Med 2(4):424–426
Schwartz DJ, Kohler WC, Karatinos G (2005) Symptoms of depression in individuals with obstructive sleep apnea may be amenable to treatment with continuous positive airway pressure. Chest 128(3):1304–1309. doi:10.1378/chest.128.3.1304
Munoz A, Mayoralas LR, Barbe F et al (2000) Long-term effects of CPAP on daytime functioning in patients with sleep apnoea syndrome. Eur Respir J 15(4):676–681
Vandeputte M, de WA (2003) Sleep disorders and depressive feelings: a global survey with the Beck depression scale. Sleep Med 4(4):343–345
Means M, Lichstein K, Edinger J et al (2003) Changes in depressive symptoms after continuous positive airway pressure treatment for obstructive sleep apnea. Sleep Breath 7(1):31–42. doi:10.1007/s11325-003-0031-x
Akashiba T, Kawahara S, Akahoshi T et al (2002) Relationship between quality of life and mood or depression in patients with severe obstructive sleep apnea syndrome. Chest 122(3):861–865
Peppard PE, Szklo-Coxe M, Hla KM et al (2006) Longitudinal association of sleep-related breathing disorder and depression. Arch Intern Med 166(16):1709–1715. doi:10.1001/archinte.166.16.1709
Kawahara S, Akashiba T, Akahoshi T et al (2005) Nasal CPAP improves the quality of life and lessens the depressive symptoms in patients with obstructive sleep apnea syndrome. Intern Med 44(5):422–427
Lewis KE, Seale L, Bartle IE et al (2004) Early predictors of CPAP use for the treatment of obstructive sleep apnea. Sleep 27(1):134–138
Kjelsberg FN, Ruud EA, Stavem K (2005) Predictors of symptoms of anxiety and depression in obstructive sleep apnea. Sleep Med 6(4):341–346. doi:10.1016/j.sleep.2005.02.004
Doherty LS, Kiely JL, Lawless G et al (2003) Impact of nasal continuous positive airway pressure therapy on the quality of life of bed partners of patients with obstructive sleep apnea syndrome. Chest 124(6):2209–2214
Shepertycky MR, Banno K, Kryger MH (2005) Differences between men and women in the clinical presentation of patients diagnosed with obstructive sleep apnea syndrome. Sleep 28(3):309–314
Yamamoto H, Akashiba T, Kosaka N et al (2000) Long-term effects nasal continuous positive airway pressure on daytime sleepiness, mood and traffic accidents in patients with obstructive sleep apnoea. Respir Med 94(1):87–90. doi:10.1053/rmed.1999.0698
Mosko S, Zetin M, Glen S et al (1989) Self-reported depressive symptomatology, mood ratings, and treatment outcome in sleep disorders patients. J Clin Psychol 45(1):51–60
Sharafkhaneh A, Giray N, Richardson P et al (2005) Association of psychiatric disorders and sleep apnea in a large cohort. Sleep 28(11):1405–1411
El-Sherbini AM, Bediwy AS, El-Mitwalli A (2011) Association between obstructive sleep apnea (OSA) and depression and the effect of continuous positive airway pressure (CPAP) treatment. Neuropsychiatr Dis Treat 7:715–721. doi:10.2147/NDT.S26341
Dahlöf P, Ejnell H, Hällström T et al (2000) Surgical treatment of the sleep apnea syndrome reduces associated major depression. International Journal of Behavioral Medicine 7(1):73–88
Mackinger HF, Svaldi JJ (2004) Autobiographical memory predicts cognitive but not somatic change in sleep apnea patients vulnerable for affective disorder. J Affect Disord 81(1):17–22. doi:10.1016/S0165-0327(03)00170-8
Sforza E, de Saint Hilaire Z, Pelissolo A et al (2002) Personality, anxiety and mood traits in patients with sleep-related breathing disorders: effect of reduced daytime alertness. Sleep Med 3(2):139–145
Ohayon MM (2003) The effects of breathing-related sleep disorders on mood disturbances in the general population. J Clin Psychiatry 64(10):1195
Sanchez AI, Buela-Casal G, Bermudez MP et al (2001) The effects of continuous positive air pressure treatment on anxiety and depression levels in apnea patients. Psychiatry Clin Neurosci 55(6):641–646
Saunamaki T, Jehkonen M (2007) Depression and anxiety in obstructive sleep apnea syndrome: a review. Acta Neurol Scand 116(5):277–288. doi:10.1111/j.1600-0404.2007.00901.x
Aikens JE, Caruana-Montaldo B, Vanable PA et al (1999) MMPI correlates of sleep and respiratory disturbance in obstructive sleep apnea. Sleep 22(3):362–369
Aikens JE, Mendelson WB (1999) A matched comparison of MMPI responses in patients with primary snoring or obstructive sleep apnea. Sleep 22(3):355–359
Aikens JE, Vanable PA, Tadimeti L et al (1999) Differential rates of psychopathology symptoms in periodic limb movement disorder, obstructive sleep apnea, psychophysiological insomnia, and insomnia with psychiatric disorder. Sleep 22(6):775–780
Aikens JE, Mendelson WB, Baehr EK (2000) Replicability of psychometric differences between obstructive sleep apnea, primary snoring, and periodic limb movement disorder. J Sleep Hypnosis 4:211–215
Choi J-A, Yoon I-Y, Han E-G et al (2011) Subjective and objective CPAP compliance in patients with obstructive sleep apnea syndrome. Sleep Medicine Research 2(2):63–68
Borak J, Cieslicki JK, Koziej M et al (1996) Effects of CPAP treatment on psychological status in patients with severe obstructive sleep apnoea. J Sleep Res 5(2):123–127
Henkel V, Mergl R, Coyne JC et al (2004) Screening for depression in primary care: will one or two items suffice? Eur Arch Psychiatry Clin Neurosci 254(4):215–223. doi:10.1007/s00406-004-0476-3
Henkel V, Mergl R, Kohnen R et al (2003) Identifying depression in primary care: a comparison of different methods in a prospective cohort study. BMJ 326(7382):200–201
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Bardwell WA, Moore P, Ancoli-Israel S et al (2003) Fatigue in obstructive sleep apnea: driven by depressive symptoms instead of apnea severity? Am J Psychiatry 160(2):350–355
Bixler EO, Vgontzas AN, Lin H-M et al (2005) Excessive daytime sleepiness in a general population sample: the role of sleep apnea, age, obesity, diabetes, and depression. J Clin Endocrinol Metab 90(8):4510–4515. doi:10.1210/jc.2005-0035
Edinger JD, Carwile S, Miller P et al (1994) Psychological status, syndromatic measures, and compliance with nasal CPAP therapy for sleep apnea. Percept Mot Skills 78(3 Pt 2):1116–1118
Dominici M, Gomes M (2009) Obstructive sleep apnea (OSA) and depressive symptoms. Arq Neuropsiquiatr 67(1):35–39
Wheaton AG, Perry GS, Chapman DP et al (2012) Sleep disordered breathing and depression among U.S. adults: national health and nutrition examination survey, 2005-2008. Sleep 35(4):461–467. doi:10.5665/sleep.1724
Aloia MS, Arnedt JT, Smith L et al (2005) Examining the construct of depression in obstructive sleep apnea syndrome. Sleep Med 6(2):115–121. doi:10.1016/j.sleep.2004.09.003
Yang CK, Yang KS, Clerk A (2011) Perceived stress, depression, and coping strategies in patients with sleep-related breathing disorder. Sleep Medicine Research 2(2):54–62
Hattori M, Kitajima T, Mekata T et al (2009) Risk factors for obstructive sleep apnea syndrome screening in mood disorder patients. Psychiatry Clin Neurosci 63(3):385–391. doi:10.1111/j.1440-1819.2009.01956.x
Lang FU, Hösch H, Seibert H et al (2011) Obstruktives Schlaf-Apnoe-Syndrom als Ursache einer atypischen depression (obstructive sleep apnoea syndrome as the cause of atypical depression). Fortschr Neurol Psychiatr 79(9):531–534. doi:10.1055/s-0031-1281625
Farney R, Lugo A, Jensen R et al (2004) Simultaneous use of antidepressant and antihypertensive medications increases likelihood of diagnosis of obstructive sleep apnea syndrome. Chest 125(4):1279–1285
Smith R, Ronald J, Delaive K et al (2002) What are obstructive sleep apnea patients being treated for prior to this diagnosis? Chest 121(1):164–172
Smith S, Sullivan K, Hopkins W et al (2004) Frequency of insomnia report in patients with obstructive sleep apnoea hypopnea syndrome (OSAHS). Sleep Med 5(5):449–456. doi:10.1016/j.sleep.2004.03.005
Teodorescu MC, Avidan AY, Teodorescu M et al (2007) Sleep medicine content of major medical textbooks continues to be underrepresented. Sleep Med 8(3):271–276
Ejaz SM, Khawaja IS, Bhatia S et al (2011) Obstructive sleep apnea and depression: a review. Innov Clin Neurosci 8(8):17–25
Edwards C, Mukherjee S, Simpson L et al (2015) Depressive symptoms before and after treatment of obstructive sleep apnea in men and women. J Clin Sleep Med 11(9):1029–1038. doi:10.5664/jcsm.5020
Habukawa M, Uchimura N, Kakuma T et al (2010) Effect of CPAP treatment on residual depressive symptoms in patients with major depression and coexisting sleep apnea: contribution of daytime sleepiness to residual depressive symptoms. Sleep Med 11(6):552–557. doi:10.1016/j.sleep.2010.02.007
Wells RD, Freedland KE, Carney RM et al (2007) Adherence, reports of benefits, and depression among patients treated with continuous positive airway pressure. Psychosom Med 69(5):449–454. doi:10.1097/psy.0b013e318068b2f7
Schröder CM, O’Hara R (2005) Depression and obstructive sleep apnea (OSA). Ann Gen Psychiatry 4:13. doi:10.1186/1744-859X-4-13
Quintana-Gallego E, Carmona-Bernal C, Capote F et al (2004) Gender differences in obstructive sleep apnea syndrome: a clinical study of 1166 patients. Respir Med 98(10):984–989
Pillar G, Lavie P (1998) Psychiatric symptoms in sleep apnea syndrome: effects of gender and respiratory disturbance index. Chest 114(3):697–703
Ferrari AJ, Charlson FJ, Norman RE et al (2013) The epidemiological modelling of major depressive disorder: application for the global burden of disease study 2010. PLoS One 8(7):e69637. doi:10.1371/journal.pone.0069637
Wharton W, Gleason CE, Olson SRMS et al (2012) Neurobiological underpinnings of the estrogen—mood relationship. Curr Psychiatry Rev 8(3):247–256. doi:10.2174/157340012800792957
Ong JC, Gress JL, San Pedro-Salcedo MG et al (2009) Frequency and predictors of obstructive sleep apnea among individuals with major depressive disorder and insomnia. J Psychosom Res 67(2):135–141. doi:10.1016/j.jpsychores.2009.03.011
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Heinen und Löwenstein (manufacturer of CPAC devices) provided financial support in the form of third-party funding. The sponsor had no role in the design or conduct of this research.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Richter K contributed equally to this work.
Rights and permissions
About this article
Cite this article
Acker, J., Richter, K., Piehl, A. et al. Obstructive sleep apnea (OSA) and clinical depression—prevalence in a sleep center. Sleep Breath 21, 311–318 (2017). https://doi.org/10.1007/s11325-016-1411-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-016-1411-3