ABSTRACT
BACKGROUND
There has been considerable focus on the burden of mental illness (including post-traumatic stress disorder, PTSD) in returning Operation Enduring Freedom/Operation Iraqi Freedom (OEF/OIF) veterans, but little attention to the burden of medical illness in those with PTSD.
OBJECTIVES
(1) Determine whether the burden of medical illness is higher in women and men OEF/OIF veterans with PTSD than in those with No Mental Health Conditions (MHC). (2) Identify conditions common in those with PTSD.
DESIGN
Cross-sectional study using existing databases (Fiscal Year 2006–2007).
SETTING
Veterans Health Administration (VHA) patients nationally.
PATIENTS
All 90,558 OEF/OIF veterans using VHA outpatient care nationally, categorized into strata: PTSD, Stress-Related Disorders, Other MHCs, and No MHC.
MEASUREMENTS
(1) Count of medical conditions; (2) specific medical conditions (from ICD9 codes, using Agency for Health Research and Quality’s Clinical Classifications software framework).
MAIN RESULTS
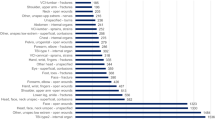
The median number of medical conditions for women was 7.0 versus 4.5 for those with PTSD versus No MHC (p < 0.001), and for men was 5.0 versus 4.0 (p < 0.001). For PTSD patients, the most frequent conditions among women were lumbosacral spine disorders, headache, and lower extremity joint disorders, and among men were lumbosacral spine disorders, lower extremity joint disorders, and hearing problems. These high frequency conditions were more common in those with PTSD than in those with No MHC.
CONCLUSIONS
Burden of medical illness is greater in women and men OEF/OIF veteran VHA users with PTSD than in those with No MHC. Health delivery systems serving them should align clinical program development with their medical care needs.

Similar content being viewed by others
REFERENCES
Seal KH, Bertenthal D, Miner CR, Sen S, Marmar C. Bringing the war back home: mental health disorders among 103,788 US veterans returning from Iraq and Afghanistan seen at Department of Veterans Affairs facilities. Arch Intern Med. 2007;167(5):476–482.
Hoge CW, Auchterlonie JL, Milliken CS. Mental health problems, use of mental health services, and attrition from military service after returning from deployment to Iraq or Afghanistan. JAMA. 2006;295(9):1023–1032.
Kang HK, Hyams KC. Mental health care needs among recent war veterans. N Engl J Med. 2005;352(13):1289.
Schnurr PP, Green BL. Trauma and Health, Physical Health Consequences of Exposure to Extreme Stress. Washington, DC: American Psychological Association; 2004.
Lang AJ, Rodgers CS, Laffaye C, Satz LE, Dresselhaus TR, Stein MB. Sexual trauma, posttraumatic stress disorder, and health behavior. Behav Med. Winter. 2003;28(4):150–158.
Geuze E, Westenberg HG, Jochims A, et al. Altered pain processing in veterans with posttraumatic stress disorder. Arch Gen Psychiatry. 2007;64(1):76–85.
Kimerling R, Ouimette P, Wolfe J, eds. Gender and PTSD. New York: The Guilford Press; 2002.
Friedman MJ, Schnurr PP, McDonagh-Coyle A. Post-traumatic stress disorder in the military veteran. Psychiatr Clin North Am. 1994;17(2):265–277.
Yano EM, Bastian LA, Frayne SM, et al. Toward a VA women’s health research agenda: Setting evidence-based priorities to improve the health and health care of women veterans. J Gen Intern Med. 2006;21(s3):S93–S101.
VIREC, VIREC Research User Guide: FY2006 VHA Medical SAS Outpatient Datasets. Hines, IL: Edward J. Hines, Jr. VA Hospital (151 V); September 2007 2007.
Elixhauser A, Steiner C, Palmer L. Clinical Classifications Software (CCS), 2008. (accessed August 13, 2010); http://www.hcup-us.ahrq.gov/toolssoftware/ccs/ccs.jsp.
Kimerling R, Ouimette P, Prins A, et al. Brief report: Utility of a short screening scale for DSM-IV PTSD in primary care. J Gen Intern Med. 2005;21(1):65–67.
Schnurr PP, Ford JD, Friedman MJ, Green BL, Dain BJ, Sengupta A. Predictors and outcomes of posttraumatic stress disorder in World War II veterans exposed to mustard gas. J Consult Clin Psychol. 2000;68(2):258–268.
Stephens M. EDF statistics for goodness of fit and some comparisons. Journal of the American Statistical Association. 1974;69:730–737.
Beckham JC, Moore SD, Feldman ME, Hertzberg MA, Kirby AC, Fairbank JA. Health status, somatization, and severity of posttraumatic stress disorder in Vietnam combat veterans with posttraumatic stress disorder. Am J Psychiatry. 1998;155(11):1565–1569.
Frayne SM, Seaver MR, Loveland S, et al. Burden of medical illness in women with depression and posttraumatic stress disorder. Arch Intern Med. 2004;164(12):1306–1312.
Hoge CW, Terhakopian A, Castro CA, Messer SC, Engel CC. Association of posttraumatic stress disorder with somatic symptoms, health care visits, and absenteeism among Iraq war veterans. Am J Psychiatry. 2007;164(1):150–153.
Wagner AW, Wolfe J, Rotnitsky A, Proctor SP, Erickson DJ. An investigation of the impact of posttraumatic stress disorder on physical health. J Trauma Stress. 2000;13(1):41–55.
Wolfe J, Proctor SP, Erickson DJ, et al. Relationship of psychiatric status to Gulf War veterans’ health problems. Psychosom Med. 1999;61(4):532–540.
Engel CC Jr, Liu X, McCarthy BD, Miller RF, Ursano R. Relationship of physical symptoms to posttraumatic stress disorder among veterans seeking care for Gulf War-related health concerns. Psychosom Med. 2000;62(6):739–745.
Barrett DH, Doebbeling CC, Schwartz DA, et al. Posttraumatic stress disorder and self-reported physical health status among US Military personnel serving during the Gulf War period: a population-based study. Psychosomatics. May-Jun. 2002;43(3):195–205.
Hoge CW, McGurk D, Thomas JL, Cox AL, Engel CC, Castro CA. Mild traumatic brain injury in US Soldiers returning from Iraq. N Engl J Med. 2008;358(5):453–463.
Cohen BE, Gima K, Bertenthal D, Kim S, Marmar CR, Seal KH. Mental health diagnoses and utilization of VA non-mental health medical services among returning Iraq and Afghanistan veterans. J Gen Intern Med. 2010;25(1):18–24.
Helmer DA, Chandler HK, Quigley KS, Blatt M, Teichman R, Lange G. Chronic widespread pain, mental health, and physical role function in OEF/OIF veterans. Pain Med. 2009;10(7):1174–1182.
Wolfe J, Schnurr PP, Brown PJ, Furey J. Posttraumatic stress disorder and war-zone exposure as correlates of perceived health in female Vietnam War veterans. J Consult Clin Psychol. 1994;62(6):1235–1240.
Taft CT, Stern AS, King LA, King DW. Modeling physical health and functional health status: the role of combat exposure, posttraumatic stress disorder, and personal resource attributes. J Trauma Stress. 1999;12(1):3–23.
Dobie DJ, Kivlahan DR, Maynard C, Bush KR, Davis TM, Bradley KA. Posttraumatic stress disorder in female veterans: association with self-reported health problems and functional impairment. Arch Intern Med. 2004;164(4):394–400.
Kazis LE, Miller DR, Clark J, et al. Health-related quality of life in patients served by the Department of Veterans Affairs: results from the Veterans Health Study. Arch Intern Med. 1998;158(6):626–632.
Redelmeier DA, Tan SH, Booth GL. The treatment of unrelated disorders in patients with chronic medical diseases. N Engl J Med. 1998;338(21):1516–1520.
Schnurr PP, Friedman MJ, Sengupta A, Jankowski MK, Holmes T. PTSD and utilization of medical treatment services among male Vietnam veterans. J Nerv Ment Dis. 2000;188(8):496–504.
Sheehan B, Lall R, Bass C. Does somatization influence quality of life among older primary care patients? Int J Geriatr Psychiatry. 2005;20(10):967–972.
Acknowledgements
The authors are very grateful to Kristian Gima, BA (National Center for PTSD, VA Palo Alto Health Care System), for his technical contributions, to Ann Thrailkill, RNP, MSN, CNS (Women’s Health Center of Excellence, VA Palo Alto Health Care System), Mark W. Smith PhD (Health Economics Resource Center, VA Palo Alto Health Care System), Jenny Hyun MPH, PhD (National Center for PTSD, VA Palo Alto Health Care System), and Amy Street, PhD (National Center for PTSD, VA Boston Healthcare System) for their contributions to study development, and to Rudolf Moos, PhD (Center for Health Care Evaluation, VA Palo Alto Health Care System, and Department of Psychiatry, Stanford University) for his helpful comments on an earlier version of the manuscript. None of the individuals listed in the Acknowledgements section received compensation from this study.
Conflicts of Interest
None disclosed.
Disclaimer
The views expressed in this article are those of the authors and do not necessarily represent the views of the Department of Veterans Affairs.
Prior Presentation
One aspect of the data (information regarding the relationship between PTSD and obesity) was presented in poster format at a national meeting: Phibbs CS, Frayne S, Kimerling R, Pavao J, Berg E, Laungani K, Gima K. "Obesity and PTSD in OIF-OEF Veterans." Poster presentation at AcademyHealth National Meeting, Washington DC, June 2008.
Financial Support
This material is based upon work supported by Department of Veterans Affairs Health Services Research and Development grants SDR 07-331, SHP 08-161, and IAE 05-291. The views expressed in this article are those of the authors and do not necessarily represent the views of the Department of Veterans Affairs.
Role of the Funding Sources
The funding sources had no role in any of the following: design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript.
Access to Data
Dr. Frayne and Mr. Berg had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix 1
Mental Health Condition Specifications (PDF 54.4 KB)
Appendix 2
Gender-stratified Frequency of all 222 Medical Conditions, by PTSD Status, in OEF/OIF Veterans Health Administration Patients; Frequency Rank for Women and Men with PTSD (with 1 indicating most frequent); and Age-Adjusted Odds Ratio (PTSD vs No MHC)* (PDF 484 KB)
Appendix 3
Cumulative Medical Condition Count by PTSD Status by Gender, Sensitivity Analysis 1-4, truncated at 25 conditions. (PDF 295 KB)
Appendix 4
Definition of VA Outpatient Face-to-Face Visits (Technical specifications: clinic “stop” codes used to define face-to-face visits.) (PDF 118 KB)
Appendix 5
Definition of Primary Care Clinic Stops. (Technical specifications: Clinic stop codes used to define primary care encounters.) (PDF 13.2 KB)
Rights and permissions
About this article
Cite this article
Frayne, S.M., Chiu, V.Y., Iqbal, S. et al. Medical Care Needs of Returning Veterans with PTSD: Their Other Burden. J GEN INTERN MED 26, 33–39 (2011). https://doi.org/10.1007/s11606-010-1497-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-010-1497-4