Abstract
Frontotemporal dementia (FTD) phenotypes have distinctive and well-established cortical signatures, but their subcortical grey matter profiles are poorly characterised. The comprehensive characterisation of striatal and thalamic pathology along the ALS-FTD spectrum is particularly timely, as dysfunction of frontostriatal and cortico-thalamic networks contribute to phenotype-defining cognitive, behavioral, and motor deficits. Ten patients with behavioral-variant FTD, 11 patients with non-fluent-variant primary progressive aphasia, 5 patients with semantic-variant primary progressive aphasia, 14 ALS-FTD patients with C9orf72 hexanucleotide expansions, 12 ALS-FTD patients without hexanucleotide repeats, 36 ALS patients without cognitive impairment and 50 healthy controls were included in a prospective neuroimaging study. Striatal, thalamic, hippocampal and amygdala pathology was evaluated using volume measurements, density analyses and connectivity-based segmentation. Significant volume reductions were identified in the thalamus and putamen of non-fluent-variant PPA patients. Marked nucleus accumbens and hippocampal atrophy was observed in the behavioral-variant FTD cohort. Semantic-variant PPA patients only exhibited volumetric changes in the left hippocampus. C9-positive ALS-FTD patients showed preferential density reductions in thalamic sub-regions connected to motor and sensory cortical areas. C9-negative ALS-FTD patients exhibited striatal pathology in sub-regions projecting to rostral-motor and executive cortical areas. The bulk of striatal and thalamic pathology in non-fluent-variant PPA patients was identified in foci projecting to motor areas. Subcortical density alterations in svPPA patients were limited to basal ganglia regions with parietal projections. Striatal and thalamic changes in FTD exhibit selective, network-defined vulnerability patterns mirroring cortical pathology. Multi-modal cortico-basal imaging analyses confirm that the subcortical grey matter profiles of FTD phenotypes are just as distinct as their cortical signatures. Our findings support emerging concepts of network-wise degeneration, preferential circuit vulnerability and disease propagation along connectivity patterns.





Similar content being viewed by others
References
Ahmed, R. M., Devenney, E. M., Irish, M., Ittner, A., Naismith, S., Ittner, L. M., et al. (2016). Neuronal network disintegration: common pathways linking neurodegenerative diseases. Journal of Neurology Neurosurgery, and Psychiatry, 87(11), 1234–1241. https://doi.org/10.1136/jnnp-2014-308350.
Bak, T. H., O’Donovan, D. G., Xuereb, J. H., Boniface, S., & Hodges, J. R. (2001). Selective impairment of verb processing associated with pathological changes in Brodmann areas 44 and 45 in the motor neurone disease-dementia-aphasia syndrome. Brain, 124, 103–120.
Balendra, R., Jones, A., Jivraj, N., Knights, C., Ellis, C. M., Burman, R., et al. (2014). Estimating clinical stage of amyotrophic lateral sclerosis from the ALS Functional Rating Scale. Amyotrophic Lateral Sclerosis Frontotemporal Degenerative, 15(3–4), 279–284. https://doi.org/10.3109/21678421.2014.897357.
Bede, P. (2017). Deciphering neurodegeneration: A paradigm shift from focality to connectivity. Neurology. https://doi.org/10.1212/wnl.0000000000004582.
Bede, P., Bokde, A. L., Byrne, S., Elamin, M., McLaughlin, R. L., Kenna, K., et al. (2013a). Multiparametric MRI study of ALS stratified for the C9orf72 genotype. Neurology, 81(4), 361–369. https://doi.org/10.1212/WNL.0b013e31829c5eee.
Bede, P., Elamin, M., Byrne, S., McLaughlin, R. L., Kenna, K., Vajda, A., et al. (2013b). Basal ganglia involvement in amyotrophic lateral sclerosis. Neurology, 81(24), 2107–2115. https://doi.org/10.1212/01.wnl.0000437313.80913.2c.
Bede, P., & Hardiman, O. (2014). Lessons of ALS imaging: Pitfalls and future directions — A critical review. Neuroimage: Clinical, 4(0), 436–443. https://doi.org/10.1016/j.nicl.2014.02.011.
Bede, P., & Hardiman, O. (2017). Longitudinal structural changes in ALS: a three time-point imaging study of white and gray matter degeneration. Amyotrophic Lateral Sclerosis Frontotemporal Degenerative, 1–10, https://doi.org/10.1080/21678421.2017.1407795.
Bede, P., Iyer, P. M., Finegan, E., Omer, T., & Hardiman, O. (2017). Virtual brain biopsies in amyotrophic lateral sclerosis: Diagnostic classification based on in vivo pathological patterns. Neuroimage Clinics, 15, 653–658. https://doi.org/10.1016/j.nicl.2017.06.010.
Bede, P., Iyer, P. M., Schuster, C., Elamin, M., McLaughlin, R. L., Kenna, K., et al. (2016). The selective anatomical vulnerability of ALS: ‘disease-defining’ and ‘disease-defying’ brain regions. Amyotrophic Lateral Sclerosis Frontotemporal Degenerative, 1–10, https://doi.org/10.3109/21678421.2016.1173702.
Behrens, T. E., Johansen-Berg, H., Woolrich, M. W., Smith, S. M., Wheeler-Kingshott, C. A., Boulby, P. A., et al. (2003a). Non-invasive mapping of connections between human thalamus and cortex using diffusion imaging. Nature Neuroscience, 6(7), 750–757. https://doi.org/10.1038/nn1075.
Behrens, T. E., Woolrich, M. W., Jenkinson, M., Johansen-Berg, H., Nunes, R. G., Clare, S., et al. (2003b). Characterization and propagation of uncertainty in diffusion-weighted MR imaging. Magnetic Resonance in Medicine, 50(5), 1077–1088. https://doi.org/10.1002/mrm.10609.
Bisenius, S., Mueller, K., Diehl-Schmid, J., Fassbender, K., Grimmer, T., Jessen, F., et al. (2017). Predicting primary progressive aphasias with support vector machine approaches in structural MRI data. Neuroimage Clinics, 14, 334–343. https://doi.org/10.1016/j.nicl.2017.02.003.
Bonelli, R. M., & Cummings, J. L. (2007). Frontal-subcortical circuitry and behavior. Dialogues Clinical Neuroscience, 9(2), 141–151.
Brettschneider, J., Del Tredici, K., Toledo, J. B., Robinson, J. L., Irwin, D. J., Grossman, M., et al. (2013). Stages of pTDP-43 pathology in amyotrophic lateral sclerosis. Annals Neurology.
Brooks, B. R., Miller, R. G., Swash, M., & Munsat, T. L. & World Federation of Neurology Research Group on Motor Neuron, D. (2000). El Escorial revisited: revised criteria for the diagnosis of amyotrophic lateral sclerosis. Amyotroph Lateral Sclerosis Other Motor Neuron Disorders, 1(5), 293–299.
Byrne, S., Elamin, M., Bede, P., Shatunov, A., Walsh, C., Corr, B., et al. (2012). Cognitive and clinical characteristics of patients with amyotrophic lateral sclerosis carrying a C9orf72 repeat expansion: a population-based cohort study. Lancet Neurology, 11(3), 232–240. https://doi.org/10.1016/S1474-4422(12)70014-5.
Davatzikos, C., Resnick, S. M., Wu, X., Parmpi, P., & Clark, C. M. (2008). Individual patient diagnosis of AD and FTD via high-dimensional pattern classification of MRI. Neuroimage, 41(4), 1220–1227. https://doi.org/10.1016/j.neuroimage.2008.03.050.
de Souza, L. C., Chupin, M., Bertoux, M., Lehericy, S., Dubois, B., Lamari, F., et al. (2013). Is hippocampal volume a good marker to differentiate Alzheimer’s disease from frontotemporal dementia? Journal of Alzheimers Disease, 36(1), 57–66. https://doi.org/10.3233/jad-122293.
Desikan, R. S., Segonne, F., Fischl, B., Quinn, B. T., Dickerson, B. C., Blacker, D., et al. (2006). An automated labeling system for subdividing the human cerebral cortex on MRI scans into gyral based regions of interest. Neuroimage, 31(3), 968–980. https://doi.org/10.1016/j.neuroimage.2006.01.021.
Elamin, M., Bede, P., Byrne, S., Jordan, N., Gallagher, L., Wynne, B., et al. (2013). Cognitive changes predict functional decline in ALS: a population-based longitudinal study. Neurology, 80(17), 1590–1597. https://doi.org/10.1212/WNL.0b013e31828f18ac.
Elamin, M., Phukan, J., Bede, P., Jordan, N., Byrne, S., Pender, N., et al. (2011). Executive dysfunction is a negative prognostic indicator in patients with ALS without dementia. Neurology, 76(14), 1263–1269.
Filippi, M., Agosta, F., Scola, E., Canu, E., Magnani, G., Marcone, A., et al. (2013). Functional network connectivity in the behavioral variant of frontotemporal dementia. Cortex, 49(9), 2389–2401. https://doi.org/10.1016/j.cortex.2012.09.017.
Filippi, M., Basaia, S., Canu, E., Imperiale, F., Meani, A., Caso, F., et al. (2017). Brain network connectivity differs in early-onset neurodegenerative dementia. Neurology, 89(17), 1764–1772. https://doi.org/10.1212/wnl.0000000000004577.
Fischl, B. (2012). FreeSurfer. Neuroimage, 62(2), 774–781. https://doi.org/10.1016/j.neuroimage.2012.01.021.
Fischl, B., & Dale, A. M. (2000). Measuring the thickness of the human cerebral cortex from magnetic resonance images. Proceedings of the National Academy of Sciences, 97(20), 11050–11055, https://doi.org/10.1073/pnas.200033797.
Frazier, J. A., Chiu, S., Breeze, J. L., Makris, N., Lange, N., Kennedy, D. N., et al. (2005). Structural brain magnetic resonance imaging of limbic and thalamic volumes in pediatric bipolar disorder. The American Journal of Psychiatry, 162(7), 1256–1265. https://doi.org/10.1176/appi.ajp.162.7.1256.
Grossman, M., Anderson, C., Khan, A., Avants, B., Elman, L., & McCluskey, L. (2008). Impaired action knowledge in amyotrophic lateral sclerosis. Neurology, 71(18), 1396–1401. https://doi.org/10.1212/01.wnl.0000319701.50168.8c.
Guo, C. C., Tan, R., Hodges, J. R., Hu, X., Sami, S., & Hornberger, M. (2016). Network-selective vulnerability of the human cerebellum to Alzheimer’s disease and frontotemporal dementia. Brain, 139(Pt 5), 1527–1538. https://doi.org/10.1093/brain/aww003.
Halabi, C., Halabi, A., Dean, D. L., Wang, P. N., Boxer, A. L., Trojanowski, J. Q., et al. (2013). Patterns of striatal degeneration in frontotemporal dementia. Alzheimer Disease and Associated Disorders, 27(1), 74–83. https://doi.org/10.1097/WAD.0b013e31824a7df4.
Hodges, J. R., Mitchell, J., Dawson, K., Spillantini, M. G., Xuereb, J. H., McMonagle, P., et al. (2010). Semantic dementia: demography, familial factors and survival in a consecutive series of 100 cases. Brain, 133, 300–306. doi:https://doi.org/10.1093/Brain/Awp248.
Jiskoot, L. C., Dopper, E. G., Heijer, T., Timman, R., van Minkelen, R., van Swieten, J. C., et al. (2016). Presymptomatic cognitive decline in familial frontotemporal dementia: A longitudinal study. Neurology, 87(4), 384–391. https://doi.org/10.1212/wnl.0000000000002895.
Johansen-Berg, H., Behrens, T. E., Sillery, E., Ciccarelli, O., Thompson, A. J., Smith, S. M., et al. (2005). Functional-anatomical validation and individual variation of diffusion tractography-based segmentation of the human thalamus. Cerebral Cortex, 15(1), 31–39. https://doi.org/10.1093/cercor/bhh105.
Jucker, M., & Walker, L. C. (2013). Self-propagation of pathogenic protein aggregates in neurodegenerative diseases. Nature, 501(7465), 45–51. https://doi.org/10.1038/nature12481.
Lagarde, J., Valabregue, R., Corvol, J. C., Garcin, B., Volle, E., Le Ber, I., et al. (2015). Why do patients with neurodegenerative frontal syndrome fail to answer: ‘In what way are an orange and a banana alike?’ Brain, 138(Pt 2), 456–471. https://doi.org/10.1093/brain/awu359.
Lee, S. E., Sias, A. C., Mandelli, M. L., Brown, J. A., Brown, A. B., Khazenzon, A. M., et al. (2017). Network degeneration and dysfunction in presymptomatic C9ORF72 expansion carriers. Neuroimage Clinics, 14, 286–297. https://doi.org/10.1016/j.nicl.2016.12.006.
Lu, P. H., Lee, G. J., Shapira, J., Jimenez, E., Mather, M. J., Thompson, P. M., et al. (2014). Regional differences in white matter breakdown between frontotemporal dementia and early-onset Alzheimer’s disease. Journal of Alzheimers Disease, 39(2), 261–269. https://doi.org/10.3233/jad-131481.
Ludolph, A., Drory, V., Hardiman, O., Nakano, I., Ravits, J., Robberecht, W., et al. (2015). A revision of the El Escorial criteria – 2015. Amyotrophic Lateral Sclerosis Frontotemporal Degenerative, 16(5–6), 291–292. https://doi.org/10.3109/21678421.2015.1049183.
Luis, E., Ortiz, A., Eudave, L., Ortega-Cubero, S., Borroni, B., van der Zee, J., et al. (2016). Neuroimaging Correlates of Frontotemporal Dementia Associated with SQSTM1 Mutations. Journal of Alzheimers Disease, 53(1), 303–313. https://doi.org/10.3233/jad-160006.
Macfarlane, M. D., Jakabek, D., Walterfang, M., Vestberg, S., Velakoulis, D., Wilkes, F. A., et al. (2015). Striatal Atrophy in the Behavioural Variant of Frontotemporal Dementia: Correlation with Diagnosis, Negative Symptoms and Disease Severity. PLoS One, 10(6), e0129692. https://doi.org/10.1371/journal.pone.0129692.
Machts, J., Loewe, K., Kaufmann, J., Jakubiczka, S., Abdulla, S., Petri, S., et al. (2015). Basal ganglia pathology in ALS is associated with neuropsychological deficits. Neurology, 85(15), 1301–1309. https://doi.org/10.1212/wnl.0000000000002017.
McMillan, C. T., Avants, B. B., Cook, P., Ungar, L., Trojanowski, J. Q., & Grossman, M. (2014). The power of neuroimaging biomarkers for screening frontotemporal dementia. Human Brain Mapping, 35(9), 4827–4840. https://doi.org/10.1002/hbm.22515.
Meyer, S., Mueller, K., Stuke, K., Bisenius, S., Diehl-Schmid, J., Jessen, F., et al. (2017). Predicting behavioral variant frontotemporal dementia with pattern classification in multi-center structural MRI data. Neuroimage Clinics, 14, 656–662. https://doi.org/10.1016/j.nicl.2017.02.001.
Moller, C., Dieleman, N., van der Flier, W. M., Versteeg, A., Pijnenburg, Y., Scheltens, P., et al. (2015). More atrophy of deep gray matter structures in frontotemporal dementia compared to Alzheimer’s disease. Journal of Alzheimers Disease, 44(2), 635–647. https://doi.org/10.3233/jad-141230.
Nichols, T. E., & Holmes, A. P. (2002). Nonparametric permutation tests for functional neuroimaging: a primer with examples. Human Brain Mapping, 15(1), 1–25.
O’Callaghan, C., Bertoux, M., & Hornberger, M. (2013). Beyond and below the cortex: the contribution of striatal dysfunction to cognition and behaviour in neurodegeneration. Journal of Neurology, Neurosurgery, and Psychiatry. https://doi.org/10.1136/jnnp-2012-304558.
Omer, T., Finegan, E., Hutchinson, S., Doherty, M., Vajda, A., McLaughlin, R. L., et al. (2017). Neuroimaging patterns along the ALS-FTD spectrum: a multiparametric imaging study. Amyotrophic Lateral Sclerosis Frontotemporal Degenerative, 1–13, https://doi.org/10.1080/21678421.2017.1332077.
Patenaude, B., Smith, S. M., Kennedy, D. N., & Jenkinson, M. (2011). A Bayesian model of shape and appearance for subcortical brain segmentation. Neuroimage, 56(3), 907–922.
Perry, D. C., Brown, J. A., Possin, K. L., Datta, S., Trujillo, A., Radke, A., et al. (2017). Clinicopathological correlations in behavioural variant frontotemporal dementia. Brain, 140(12), 3329–3345. https://doi.org/10.1093/brain/awx254.
Phukan, J., Elamin, M., Bede, P., Jordan, N., Gallagher, L., Byrne, S., et al. (2012). The syndrome of cognitive impairment in amyotrophic lateral sclerosis: a population-based study. Journal of Neurology, Neurosurgery, and Psychiatry, 83(1), 102–108.
Piguet, O., Hornberger, M., Mioshi, E., & Hodges, J. R. (2011). Behavioural-variant frontotemporal dementia: diagnosis, clinical staging, and management. Lancet Neurology, 10(2), 162–172. https://doi.org/10.1016/S1474-4422(10)70299-4.
Premi, E., Garibotto, V., Gazzina, S., Formenti, A., Archetti, S., Gasparotti, R., et al. (2014). Subcortical and Deep Cortical Atrophy in Frontotemporal Dementia due to Granulin Mutations. Dementia and Geriatric Cognitive Disorders Extra, 4(1), 95–102. https://doi.org/10.1159/000355428.
Rascovsky, K., Hodges, J. R., Knopman, D., Mendez, M. F., Kramer, J. H., Neuhaus, J., et al. (2011). Sensitivity of revised diagnostic criteria for the behavioural variant of frontotemporal dementia. Brain, 134, 2456–2477. https://doi.org/10.1093/Brain/Awr179.
Rohrer, J. D., Nicholas, J. M., Cash, D. M., van Swieten, J., Dopper, E., Jiskoot, L., et al. (2015). Presymptomatic cognitive and neuroanatomical changes in genetic frontotemporal dementia in the Genetic Frontotemporal dementia Initiative (GENFI) study: a cross-sectional analysis. Lancet Neurology, 14(3), 253–262. https://doi.org/10.1016/s1474-4422(14)70324-2.
Schuster, C., Elamin, M., Hardiman, O., & Bede, P. (2015). Presymptomatic and longitudinal neuroimaging in neurodegeneration–from snapshots to motion picture: a systematic review. Journal of Neurology, Neurosurgery, and Psychiatry, 86(10), 1089–1096. https://doi.org/10.1136/jnnp-2014-309888.
Schuster, C., Hardiman, O., & Bede, P. (2017). Survival prediction in Amyotrophic lateral sclerosis based on MRI measures and clinical characteristics. BMC Neurology, 17(1), 73. https://doi.org/10.1186/s12883-017-0854-x.
Snowden, J., Neary, D., & Mann, D. (2007). Frontotemporal lobar degeneration: clinical and pathological relationships. Acta Neuropathologica, 114(1), 31–38. https://doi.org/10.1007/s00401-007-0236-3.
Steinacker, P., Semler, E., Anderl-Straub, S., Diehl-Schmid, J., Schroeter, M. L., Uttner, I., et al. (2017). Neurofilament as a blood marker for diagnosis and monitoring of primary progressive aphasias. Neurology, 88(10), 961–969. https://doi.org/10.1212/wnl.0000000000003688.
Tziortzi, A. C., Haber, S. N., Searle, G. E., Tsoumpas, C., Long, C. J., Shotbolt, P., et al. (2014). Connectivity-based functional analysis of dopamine release in the striatum using diffusion-weighted MRI and positron emission tomography. Cerebral Cortex, 24(5), 1165–1177. https://doi.org/10.1093/cercor/bhs397.
Verstraete, E., Turner, M. R., Grosskreutz, J., Filippi, M., & Benatar, M. (2015). Mind the gap: The mismatch between clinical and imaging metrics in ALS. Amyotrophic Lateral Sclerosis Frontotemporal Degenerative, 16(7–8), 524–529. https://doi.org/10.3109/21678421.2015.1051989.
Verstraete, E., Veldink, J. H., van den Berg, L. H., & van den Heuvel, M. P. (2013). Structural brain network imaging shows expanding disconnection of the motor system in amyotrophic lateral sclerosis. Human Brain Mapping. https://doi.org/10.1002/hbm.22258.
Westeneng, H. J., Verstraete, E., Walhout, R., Schmidt, R., Hendrikse, J., Veldink, J. H., et al. (2015). Subcortical structures in amyotrophic lateral sclerosis. Neurobiology Aging, 36(2), 1075–1082. https://doi.org/10.1016/j.neurobiolaging.2014.09.002.
Whitwell, J. L., Jack, C. R. Jr., Boeve, B. F., Senjem, M. L., Baker, M., Rademakers, R., et al. (2009). Voxel-based morphometry patterns of atrophy in FTLD with mutations in MAPT or PGRN. Neurology, 72(9), 813–820. https://doi.org/10.1212/01.wnl.0000343851.46573.67.
Whitwell, J. L., Weigand, S. D., Boeve, B. F., Senjem, M. L., Gunter, J. L., DeJesus-Hernandez, M., et al. (2012). Neuroimaging signatures of frontotemporal dementia genetics: C9ORF72, tau, progranulin and sporadics. Brain, 135(Pt 3), 794–806. https://doi.org/10.1093/brain/aws001.
Winkler, A. M., Ridgway, G. R., Webster, M. A., Smith, S. M., & Nichols, T. E. (2014). Permutation inference for the general linear model. Neuroimage, 92, 381–397. https://doi.org/10.1016/j.neuroimage.2014.01.060.
Zhou, J., Greicius, M. D., Gennatas, E. D., Growdon, M. E., Jang, J. Y., Rabinovici, G. D., et al. (2010). Divergent network connectivity changes in behavioural variant frontotemporal dementia and Alzheimer’s disease. Brain, 133(Pt 5), 1352–1367. https://doi.org/10.1093/brain/awq075.
Acknowledgements
We gratefully acknowledge the kindness and generosity of our patients and their caregivers. This work was supported by the Health Research Board (HRB – Ireland; HRB EIA-2017-019), the Irish Institute of Clinical Neuroscience IICN − Novartis Ireland Research Grant, the Iris O’Brien Foundation, the Perrigo Clinician-Scientist Research Fellowship, and the Research Motor Neuron (RMN-Ireland) Foundation.
Funding
This study was funded by the Health Research Board (HRB – Ireland; HRB EIA-2017-019), the Irish Institute of Clinical Neuroscience IICN − Novartis Ireland Research (IICN – 2016), the Iris O’Brien Foundation, the Perrigo Clinician-Scientist Research Fellowship, and the Research Motor Neuron (RMN-Ireland) Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Peter Bede declares that he has no conflict of interest. Taha Omer declares that he has no conflict of interest. Eoin Finegan declares that he has no conflict of interest. Rangariroyashe H. Chipika declares that she has no conflict of interest. Parameswaran M. Iyer declares that he has no conflict of interest. Mark A. Doherty declares that he has no conflict of interest. Alice Vajda declares that she has no conflict of interest. Niall Pender declares that he has no conflict of interest. Russell L. McLaughlin declares that he has no conflict of interest. Siobhan Hutchinson declares that she has no conflict of interest. Orla Hardiman has received speaking honoraria from Janssen Cilag, Biogen Idec, Sanofi Aventis and Merck-Serono, she has been a member of advisory panels for Biogen Idec, Allergen, Cytokinetics, Ono Pharmaceuticals and Sanofi Aventis.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional (Ethics (Medical Research) Committee - Beaumont Hospital, Dublin, Ireland) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.


11682_2018_9837_MOESM3_ESM.jpg
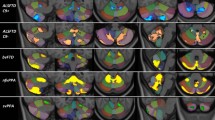
The grey matter density profile of individual FTD phenotypes in connectivity-based striatal and thalamic sub-regions (JPG 440 KB)
Rights and permissions
About this article
Cite this article
Bede, P., Omer, T., Finegan, E. et al. Connectivity-based characterisation of subcortical grey matter pathology in frontotemporal dementia and ALS: a multimodal neuroimaging study. Brain Imaging and Behavior 12, 1696–1707 (2018). https://doi.org/10.1007/s11682-018-9837-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-018-9837-9