Abstract
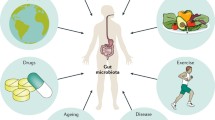
Intestinal microbiota is essential for gut homeostasis. Specifically, the microorganisms inhabiting the gut lumen interact with the intestinal immune system, supply key nutrients for the major components of the gut wall, and modulate energy metabolism. Host–microbiome interactions can be either beneficial or deleterious, driving gastrointestinal lymphoid tissue activities and shaping gut wall structures. This overview briefly focuses on the potential role played by abnormalities in gut microbiota and relative responses of the gastrointestinal tract in the determination of important pathological conditions such as the irritable bowel syndrome, inflammatory bowel diseases and colorectal cancer.
Similar content being viewed by others
References
Barbara G, Stanghellini V, Brandi G, Cremon C, Di Nardo G, De Giorgio R, Corinaldesi R (2005) Interactions between commensal bacteria and gut sensorimotor function in health and disease. Am J Gastroenterol 100(11):2560–2568
Longstreth GF, Thompson WG, Chey WD, Houghton LA, Mearin F, Spiller RC (2006) Functional bowel disorders. Gastroenterology 130(5):1480–1491
Malinen E, Rinttilä T, Kajander K, Mättö J, Kassinen A, Krogius L, Saarela M, Korpela R, Palva A (2005) Analysis of the fecal microbiota of irritable bowel syndrome patients and healthy controls with real-time PCR. Am J Gastroenterol 100(2):373–382
Kassinen A, Krogius-Kurikka L, Mäkivuokko H, Rinttilä T, Paulin L, Corander J, Malinen E, Apajalahti J, Palva A (2007) The fecal microbiota of irritable bowel syndrome patients differs significantly from that of healthy subjects. Gastroenterology 133(1):24–33
Lyra A, Rinttilä T, Nikkilä J, Krogius-Kurikka L, Kajander K, Malinen E, Mättö J, Mäkelä L, Palva A (2009) Diarrhoea-predominant irritable bowel syndrome distinguishable by 16S rRNA gene phylotype quantification. World J Gastroenterol 15(47):5936–5945
Spiller R, Garsed K (2009) Postinfectious irritable bowel syndrome. Gastroenterology 136(6):1979–1988
Schoepfer AM, Schaffer T, Seibold-Schmid B, Müller S, Seibold F (2008) Antibodies to flagellin indicate reactivity to bacterial antigens in IBS patients. Neurogastroenterol Motil 20(10):1110–1118
Preidis GA, Versalovic J (2009) Targeting the human microbiome with antibiotics, probiotics, and prebiotics: gastroenterology enters the metagenomics era. Gastroenterology 136(6):2015–2031
Moayyedi P, Ford AC, Talley NJ, Cremonini F, Foxx-Orenstein AE, Brandt LJ, Quigley EM (2010) The efficacy of probiotics in the treatment of irritable bowel syndrome: a systematic review. Gut 59(3):325–332
Pimentel M, Park S, Mirocha J, Kane SV, Kong Y (2006) The effect of a nonabsorbed oral antibiotic (rifaximin) on the symptoms of the irritable bowel syndrome: a randomized trial. Ann Intern Med 145(8):557–563
Balsari A, Ceccarelli A, Dubini F, Fesce E, Poli G (1982) The fecal microbial population in the irritable bowel syndrome. Microbiologica 5(3):185–194
Wyatt GM, Bayliss CE, Lakey AF, Bradley HK, Hunter JO, Jones VA (1988) The faecal flora of two patients with food-related irritable bowel syndrome during challenge with symptom-provoking foods. J Med Microbiol 26(4):295–299
Madden JAJ, Plummer S, Sen S, Dear K, Tarry S, Hunter JO (2001) Comparison of the caecal and faecal microflora of healthy subjects and patients with irritable bowel syndrome (IBS). Gut 48(Suppl 1):A58
Pimentel M, Chow EJ, Lin HC (2000) Eradication of small intestinal bacterial overgrowth reduces symptoms of irritable bowel syndrome. Am J Gastroenterol 95(12):3503–3506
Pimentel M, Chow EJ, Lin HC (2003) Normalization of lactulose breath testing correlates with symptom improvement in irritable bowel syndrome a double-blind, randomized, placebo-controlled study. Am J Gastroenterol 98(2):412–419
Pimentel M, Wallace D, Hallegua D, Chow E, Kong Y, Park S, Lin HC (2004) A link between irritable bowel syndrome and fibromyalgia may be related to findings on lactulose breath testing. Ann Rheum Dis 63(4):450–452
McCallum R, Schultz C, Sostarich S (2005) Evaluating the role of small intestinal bacterial overgrowth (SIBO) in diarrhea predominant IBS (IBS-D) patients utilizing the glucose breath test. Gastroenterology 128:T1118
Nucera G, Gabrielli M, Lupascu A, Lauritano EC, Santoliquido A, Cremonini F, Cammarota G, Tondi P, Pola P, Gasbarrini G, Gasbarrini A (2005) Abnormal breath tests to lactose, fructose and sorbitol in irritable bowel syndrome may be explained by small intestinal bacterial overgrowth. Aliment Pharmacol Ther 21(11):1391–1395
Pimentel M, Lembo A, Chey WD, Ringel Y, Zakko S, Mareya SM, Shaw AL, Yu J, Bortey E, Forbes WP (2010) Rifaximin treatment for 2 weeks provides acute and sustained relief over 12 weeks of IBS symptoms in non-constipated irritable bowel syndrome: results from 2 North American phase 3 trials (Target 1 and Target 2). Gastroenterology 138(5, Suppl 1):S64–S65
Gasbarrini A, Corazza GR, Gasbarrini G, Montalto M, Di Stefano M, Basilisco G, Parodi A, Usai-Satta P, Vernia P, Anania C, Astegiano M, Barbara G, Benini L, Bonazzi P, Capurso G, Certo M, Colecchia A, Cuoco L, Di Sario A, Festi D, Lauritano C, Miceli E, Nardone G, Perri F, Portincasa P, Risicato R, Sorge M, Tursi A, 1st Rome H2-Breath Testing Consensus Conference Working Group (2009) Methodology and indications of H2-breath testing in gastrointestinal diseases: the Rome Consensus Conference. Aliment Pharmacol Ther 29(Suppl 1):1–49
Posserud I, Stotzer PO, Björnsson ES, Abrahamsson H, Simrén M (2007) Small intestinal bacterial overgrowth in patients with irritable bowel syndrome. Gut 56(6):802–808
Maukonen J, Satokari R, Mättö J, Söderlund H, Mattila-Sandholm T, Saarela M (2006) Prevalence and temporal stability of selected clostridial groups in irritable bowel syndrome in relation to predominant faecal bacteria. J Med Microbiol 55(Pt 5):625–633
Turner JR (2009) Intestinal mucosal barrier function in health and disease. Nat Rev Immunol 9(11):799–809
Nusrat A, Turner JR, Madara JL (2000) Molecular physiology and pathophysiology of tight junctions. IV. Regulation of tight junctions by extracellular stimuli: nutrients, cytokines, and immune cells. Am J Physiol Gastrointest Liver Physiol 279(5):G851–G857
Sartor RB (2008) Microbial influences in inflammatory bowel diseases. Gastroenterology 134(2):577–594
Takeda K, Akira S (2005) Toll-like receptors in innate immunity. Int Immunol 17(1):1–14
Dlugosz A, Lindberg G (2010) The expression of toll-like receptor 4 in colon mucosa is as up-regulated in irritable bowel syndrome as it is in inflammatory bowel disease. Gastroenterology 138 (5, Suppl 1):S626
McKernan DP, Gaszner G, Quigley EM, Cryan JF, Dinan TG (2010) Enhanced release of specific TLR-agonist mediated pro-inflammatory cytokines in irritable bowel syndrome (IBS). Gastroenterology 138 (5, Suppl 1):S628
Swidsinski A, Ladhoff A, Pernthaler A, Swidsinski S, Loening-Baucke V, Ortner M, Weber J, Hoffmann U, Schreiber S, Dietel M, Lochs H (2002) Mucosal flora in inflammatory bowel disease. Gastroenterology 122(1):44–54
Swidsinski A, Weber J, Loening-Baucke V, Hale LP, Lochs H (2005) Spatial organization and composition of the mucosal flora in patients with inflammatory bowel disease. J Clin Microbiol 43(7):3380–3389
Piche T, Barbara G, Aubert P, Bruley des Varannes S, Dainese R, Nano JL, Cremon C, Stanghellini V, De Giorgio R, Galmiche JP, Neunlist M (2009) Impaired intestinal barrier integrity in the colon of patients with irritable bowel syndrome: involvement of soluble mediators. Gut 58(2):196–201
Barbara G, Stanghellini V, De Giorgio R, Cremon C, Cottrell GS, Santini D, Pasquinelli G, Morselli-Labate AM, Grady EF, Bunnett NW, Collins SM, Corinaldesi R (2004) Activated mast cells in proximity to colonic nerves correlate with abdominal pain in irritable bowel syndrome. Gastroenterology 126(3):693–702
Barbara G, Wang B, Stanghellini V, de Giorgio R, Cremon C, Di Nardo G, Trevisani M, Campi B, Geppetti P, Tonini M, Bunnett NW, Grundy D, Corinaldesi R (2007) Mast cell-dependent excitation of visceral-nociceptive sensory neurons in irritable bowel syndrome. Gastroenterology 132(1):26–37
Cenac N, Andrews CN, Holzhausen M, Chapman K, Cottrell G, Andrade-Gordon P, Steinhoff M, Barbara G, Beck P, Bunnett NW, Sharkey KA, Ferraz JG, Shaffer E, Vergnolle N (2007) Role for protease activity in visceral pain in irritable bowel syndrome. J Clin Invest 117(3):636–647
Vernier G, Sendid B, Poulain D, Colombel JF (2004) Relevance of serologic studies in inflammatory bowel disease. Curr Gastroenterol Rep 6(6):482–487
Gewirtz AT (2006) Flag in the crossroads: flagellin modulates innate and adaptive immunity. Curr Opin Gastroenterol 22(1):8–12
Elson C, Cong Y, McCracken VJ, Dimmitt RA, Lorenz RG, Weaver CT (2005) Experimental models of inflammatory bowel disease reveal innate, adaptive, and regulatory mechanisms of host dialogue with the microbiota. Immunol Rev 206:260–276
Barnich N, Carvalho FA, Glasser AL et al (2007) CEACAM6 acts as a receptor for adherent-invasive E. coli, supporting ileal mucosa colonization in Crohn disease. J Clin Invest 117:1566–1574
Frank DN, St Amand AL, Feldman RA, Boedeker EC, Harpaz N, Pace NR (2007) Molecular-phylogenetic characterization of microbial community imbalances in human inflammatory bowel diseases. Proc Natl Acad Sci USA 104:13780–13785
Turner JR (2006) Molecular basis of epithelial barrier regulation: from basic mechanisms to clinical application. Am J Pathol 169:1901–1909
Lee J, Mo JH, Katakura K et al (2006) Maintenance of colonic homeostasis by distinctive apical TLR9 signalling in intestinal epithelial cells. Nat Cell Biol 8:1327–1336
Barrett JC, Hansoul S, Nicolae DL et al (2008) Genome-wide association defines more than 30 distinct susceptibility loci for Crohn’s disease. Nat Genet 40:955–962
Lesage S, Zouali H, Cézard JP et al (2002) CARD15/NOD2 mutational analysis and genotype–phenotype correlation in 612 patients with inflammatory bowel disease. Am J Hum Genet 70:845–857
Economou M, Trikalinos TA, Loizou KT, Tsianos EV, Ioannidis JP (2004) Differential effects of NOD2 variants on Crohn’s disease risk and phenotype in diverse populations: a metaanalysis. Am J Gastroenterol 99:2393–2404
Smythies LE, Sellers M, Clements RH et al (2005) Human intestinal macrophages display profound inflammatory anergy despite avid phagocytic and bacteriocidal activity. J Clin Invest 115:66–75
Kamada N, Hisamatsu T, Okamoto S et al (2008) Unique CD14 intestinal macrophages contribute to the pathogenesis of Crohn disease via IL-23/IFN-gamma axis. J Clin Invest 118:2269–2280
Hedl M, Li J, Cho JH, Abraham C (2007) Chronic stimulation of Nod2 mediates tolerance to bacterial products. Proc Natl Acad Sci USA 104:19440–19445
Burkitt DP (1971) Epidemiology of cancer of the colon and the rectum. Cancer 28:3220
Gibson GR, Cummings JH, Macfarlane GT et al (1990) Alternative pathways for hydrogen disposal during fermentation in the human colon. Gut 31:679–683
Roedinger WEW, Moore J, Babidge W (1997) Colonic sulfide in pathogenesis and treatment of ulcerative colitis. Dig Dis Sci 42:1571–1579
Reddy BS, Weinsenburger JH, Wynder EL (1975) Effect of high-risk and low-risk diets for colon carcinogenesis of fecal microflora and steroids in man. J Nutr 105:878–884
De Giorgio R, Blandizzi C (2010) Targeting enteric neuroplasticity: diet and bugs as new key factors. Gasroenterology 138:1663–1666
Barbara G, Stanghellini V, Cremon C, De Giorgio R, Fronzoni L, Serra M, Corinaldesi R (2009) Aminosalicylates and other anti-inflammatory compounds for irritable bowel syndrome. Dig Dis 27(Suppl 1):115–121
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
The article has been retracted upon request of the authors as it contains similarities with paragraphs of previously published articles: Abraham C, Cho H.J. N Engl J Med 2009; 361:2066-2078, SE McGarr, JM Ridlon, PB Hylemon (2005) J Clin Gastroenterol 39(2):98-109, Barbara G (2006) Mucosal Barrier Defects in Irritable Bowel Syndrome. Who Left the Door Open? Am J Gastroenterol 101.1295-1298, Barbara G, Stanghellini V, Cremon C (2008) Probiotics and irritable bowel syndrome: rationale and clinical evidence for their use. J Clin Gastroenterol 42(suppl)S214-S217 without any proper reference to the above-mentioned articles.Authors acknowledge full responsibility for this unfortunate situation which they attribute to an honest mistake due to erroneous submission of a preliminary version of the manuscript and not to an intentional plagiarism. They apologize with Editor in Chief and readers as well as with authors of the original articles and agreed to the retraction.
An erratum to this article can be found at http://dx.doi.org/10.1007/s11739-014-1164-6.
About this article
Cite this article
Stanghellini, V., Barbara, G., Cremon, C. et al. RETRACTED ARTICLE: Gut microbiota and related diseases: clinical features. Intern Emerg Med 5 (Suppl 1), 57–63 (2010). https://doi.org/10.1007/s11739-010-0451-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-010-0451-0