Abstract
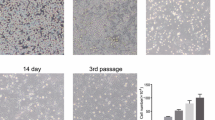
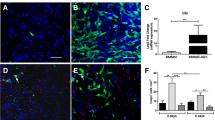
To explore the effect of bone marrow mesenchymal stem cell (BMSC) transplantation on the levels of toll-like receptor 4 (TLR4), interleukin-1β (IL-1β), and tumor necrosis factor (TNF-α) in spinal cord tissue of rat model of spinal cord injury (SCI). BMSCs from 4-week-old male SD rats were isolated, cultured, and characterized after three generations using specific surface markers CD34 and CD44. Fifty four SD male rats were divided into sham group, model group, and cell transplantation group (18 rats each group). SCI model was generated using an improved Allen’s method. Rats in cell transplantation group were treated with BMSCs in caudal vein. Rats were sacrificed at 24 h, 72 h, and 7 d post-injury, and spinal cord tissues were taken out for detection of IL-1β and TNF-α tissue content by enzyme-linked immunosorbent assay. IL-1β and TNF-α mRNA expression was evaluated by qPCR and TLR4 protein expression was analyzed by Western blotting. IL-1β and TNF-α protein levels, as well as IL-1β, TNF-α mRNA, and TLR4 expression were significantly increased in rats with established SCI, and reached its peak in spinal cord tissues at 72 h after the initial injury (p < 0.01 comparing to sham group). BMSC transplantation resulted in significant decrease in IL-1β and TNF-α tissue content, as well as IL-1β, TNF-α mRNA, and TLR4 expression as compared with model group (p < 0.01). BMSCs may alleviate the damaging effect of spinal cord inflammation by weakening TLR4-mediated signaling pathways and reducing tissue content of IL-1β and TNF-α.



Similar content being viewed by others
References
Devivo, M. J. (2012). Epidemiology of traumatic spinal cord injury: Trends and future implications. Spinal Cord, 50, 365–372.
Beattie, M. S., & Bresnahan, I. C. (2000). Cell death, repair, and recovery of function after spinal cord contusion injuries in rats. In R. C. Kalb & S. M. Strittmatter (Eds.), Neurobiology of spinal cord injury (pp. 1–21). Totowa, NJ: Humana Press.
Tator, C. H. (1995). Update on the pathophysiology and pathology of acute spinal cord injury. Brain Pathology, 5, 407–413.
McDonald, J. W., & Sadowsky, C. (2002). Spinal-cord injury. Lancet, 359, 417–425.
Rhoney, D. H., Luer, M. S., Hughes, M., & Hatt, J. (1996). New pharmacologic approaches to acute spinal cord injury. Pharmacotherapy., 16, 382–392.
Young, W. (1987). Recovery mechanisms in spinal cord injury: Implications for regenerative therapy. In F. Seil (Ed.), Frontiers of clinical Neuroscience: Neural regeneration and transplantation (pp. 156–159). New York: Alan R Liss.
Yip, P. K., & Malaspina, A. (2012). Spinal cord trauma and the molecular point of no return. Molecular Neurodegeneration, 7, 6.
Anderson, D. K. (1993). Pathophysiology of spinal cord trauma. Annals of Emergency Medicine, 22, 987–992.
Geisler, F. H., Dorsey, F. C., & Coleman, W. P. (1991). Recovery of motor function after spinal-cord injury—a randomized, placebo-controlled trial with GM-1 ganglioside. New England Journal of Medicine, 324, 1829–1838.
Lapchak, P. A., Araujo, D. M., Song, D., et al. (2001). Neuroprotection by the selective cyclooxygenase-2 inhibitor SC-236 results in improvements in behavioral deficits induced by reversible spinal cord ischemia. Stroke, 32, 1220–1225.
Hausmann, O. N. (2003). Post-traumatic inflammation following spinal cord injury. Spinal Cord, 41, 369–378.
Oyinbo, C. A. (2011). Secondary injury mechanisms in traumatic spinal cord injury: A nugget of this multiply cascade. Acta Neurobiologiae Experimentalis (Wars), 71, 281–299.
Breslin, K., & Agrawal, D. (2012). The use of methylprednisolone in acute spinal cord injury: A review of the evidence, controversies, and recommendations. Pediatric Emergency Care, 28, 12388.
Hawryluk, G. W., Rowland, J., Kwon, B. K., et al. (2008). Protection and repair of the injured spinal cord: A review of completed, ongoing, and planned clinical trials for acute spinal cord injury Neurosurg. Focus, 25, E14.
Cadotte, D. W., & Fehlings, M. G. (2011). Spinal cord injury: A systematic review of current treatment options. Clinical Orthopaedics and Related Research, 469, 7322–7327.
Kwon, B. K., Okon, E., Hillyer, J., et al. (2011). A systematic review of non-invasive pharmacologic neuroprotective treatments for acute spinal cord injury. Journal of Neurotrauma, 28, 1545.
Tator, C. H., Hashimoto, R., Raich, A., et al. (2012). Translational potential of preclinical trials of neuroprotection through pharmacotherapy for spinal cord injury. Journal of Neurosurgery: Spine, 17, 157–229.
Lalu, M. M., McIntyre, L., Pugliese, C., et al. (2012). Safety of cell therapy with mesenchymal stromal cells (SafeCell): A systematic review and meta-analysis of clinical trials. PLoS One, 7, e47559.
Prockop, D. J., Brenner, M., Fibbe, W. E., et al. (2010). Defining the risks of mesenchymal stromal cell therapy. Cytotherapy, 12, 576–578.
Caplan, A. I. (2009). Why are MSCs therapeutic? New data: New insight. The Journal of Pathology, 217, 318–324.
Vawda, R., & Fehlings, M. G. (2013). Mesenchymal cells in the treatment of spinal cord injury: Current & future perspectives. Current Stem Cell Research & Therapy, 8, 25–38.
Li, J., & Lepski, G. (2013). Cell transplantation for spinal cord injury: A systematic review. BioMed Research International, 2013, 786475.
Fleming, J. C., Norenberg, M. D., Ramsay, D. A., et al. (2006). The cellular inflammatory response in human spinal cords after injury. Brain, 129, 3249.
Nguyen, H. X., O’Barr, T. J., & Anderson, A. J. (2007). Polymorphonuclear leukocytes promote neurotoxicity through release of matrix metalloproteinases, reactive oxygen species, and TNF-alpha. Journal of Neurochemistry, 102, 900.
Uccelli, A., Benvenuto, F., Laroni, A., et al. (2011). Neuroprotective features of mesenchymal stem cells. Best Practice & Research Clinical Haematology, 24, 59–64.
Neuhuber, B., Timothy Himes, B., Shumsky, J. S., et al. (2005). Axon growth and recovery of function supported by human bone marrow stromal cells in the injured spinal cord exhibit donor variations. Brain Research, 1035, 73–85.
Abrams, M. B., Dominguez, C., Pernold, K., et al. (2009). Multipotent mesenchymal stromal cells attenuate chronic inflammation and injury-induced sensitivity to mechanical stimuli in experimental spinal cord injury. Restorative Neurology and Neuroscience, 27, 307–321.
Ohta, M., Suzuki, Y., Noda, T., et al. (2004). Bone marrow stromal cells infused into the cerebrospinal fluid promote functional recovery of the injured rat spinal cord with reduced cavity formation. Experimental Neurology, 187, 266–278.
Tran, C. T., Gargiulo, C., Thao, H. D., et al. (2011). Culture and differentiation of osteoblasts on coral scaffold from human bone marrow mesenchymal stem cells. Cell and Tissue Banking, 12(4), 247–261.
Sakata, N., Goto, M., Yoshimatsu, G., et al. (2011). Utility of co-transplanting mesenchymal stem cells in islet transplantation. World Journal of Gastroenterology, 17(47), 5150–5155.
Allen, A. R. (1911). Surgery of experimental lesion of spinal cord equivalent to crush injury of fracture dislocation of spinal column a preliminary report. JAMA, 57, 878–880.
David, S., & Kroner, A. (2011). Repertoire of microglial and macrophage responses after spinal cord injury. Nature Reviews Neuroscience, 12(7), 388–399.
van den Brand, R., Heutschi, J., Barraud, Q., et al. (2012). Restoring voluntary control of locomotion after paralyzing spinal cord injury. Science, 336(6085), 1182–1185.
Zhang, N., Yin, Y., Xu, S. J., et al. (2012). Inflammation & apoptosis in spinal cord injury. Indian Journal of Medical Research, 35, 287–296.
David, S., & Kroner, A. (2011). Repertoire of microglial and macrophage responses after spinal cord injury. Nature Reviews Neuroscience, 12, 388–399.
Jaerve, A., & Muller, H. W. (2012). Chemokines in CNS injury and repair. Cell and Tissue Research, 349, 229–248.
Erşahin, M., Çevik, Ö., Akakın, D., et al. (2012). Montelukast inhibits caspase-3 activity and ameliorates oxidative damage in the spinal cord and urinary bladder of rats with spinal cord injury. Prostaglandins & Other Lipid Mediators, 99(3–4), 131–139.
Bastien, D., & Lacroix, S. (2014). Cytokine pathways regulating glial and leukocyte function after spinal cord and peripheral nerve injury. Experimental Neurology, 258, 62–77.
Shi, Y., Zhang, D., Huff, T. B., et al. (2011). Longitudinal in vivo coherent anti-Stokes Raman scattering imaging of demyelination and remyelination in injured spinal cord. Journal of Biomedical Optics, 16(10), 106012-1–106012-4.
Liu, H., Peng, H., Wu, Y., et al. (2013). The promotion of bone regeneration by nanofibrous hydroxyapatite/chitosan scaffolds by effects on integrin-BMP/Smad signaling pathway in BMSCs. Biomaterials, 34(18), 4404–4417.
Blight, A. R., & Young, W. (1989). Central axons in injured cat spinal cord recover electrophysiological function following remyelination by Schwann cells. Journal of the Neurological Sciences, 91, 15–34.
Kayagaki, N., Wong, M. T., Stowe, I. B., et al. (2013). Noncanonical inflammasome activation by intracellular LPS independent of TLR4. Science, 341(6151), 1246–1249.
Caicco, M. J., Zahir, T., Mothe, A. J., et al. (2013). Characterization of hyaluronan-methylcellulose hydrogels for cell delivery to the injured spinal cord. Journal of Biomedical Materials Research Part A, 101A(5), 1472–1477.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Han, D., Wu, C., Xiong, Q. et al. Anti-inflammatory Mechanism of Bone Marrow Mesenchymal Stem Cell Transplantation in Rat Model of Spinal Cord Injury. Cell Biochem Biophys 71, 1341–1347 (2015). https://doi.org/10.1007/s12013-014-0354-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-014-0354-1