Abstract
Background
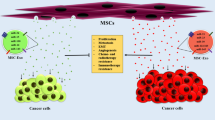
Mesenchymal stromal cell derived extracellular vesicles (MSC-EVs) have been implicated in the regulation of tumor growth. Studies remain preclinical with effects ranging from inhibition of tumor growth to cancer progression. A systematic review and meta-analysis is needed to clarify the effect of MSC-EVs on tumor growth to facilitate potential translation to clinical trials.
Methods
A systematic search of the literature (MEDLINE, Embase, and BIOSIS databases to June 1, 2019) identified all pre-clinical controlled studies investigating the effect of MSC-EVs on tumor growth. Study selection and data extraction were performed in duplicate. Potential risk of bias was assessed using the SYRCLE tool. A random effects meta-analysis of reduction in tumor weight/volume (primary outcome) was performed.
Results
We identified 29 articles and 22 reported data on tumor responses that were included for meta-analysis. Studies were associated with unclear risk of bias in a large proportion of domains in accordance with the SYRCLE tool for determining risk of bias in preclinical studies. A high risk of bias was not identified in any study. MSC-EVs had a mixed response on tumor progression with some studies reporting inhibition of tumor growth and others reporting tumor progression. Overall, MSC-EVs exerted a non-significant reduction in tumor growth compared to controls (standardized mean difference (SMD) -0.80, 95 % CI -1.64 to 0.03, p = 0.06, I2 = 87 %). Some studies reported increased tumor growth which aligned with their stated hypothesis and some interrogated mechanisms in cancer biology. EVs isolated from MSCs that overexpressed anti-tumor RNAs were associated with significant tumor reduction in meta-analysis (SMD − 2.40, 95 % CI -3.36 to -1.44, p < 0.001). Heterogeneity between studies was observed and included aspects of study design such as enrichment of MSC-EVs with specific anti-tumor molecules, tissue source of MSCs, method of EV isolation, characterization of MSCs and EVs, dosage and administration schedules, and tissue type and source of tumor cells studied.
Conclusions
MSC-EVs are associated with mixed effects on tumor growth in animal models of cancer. In studies where anti-tumor RNAs are packaged in EVs, a significant reduction in tumor growth was observed. Reducing heterogeneity in study design may accelerate our understanding of the potential effects of MSC-EVs on cancer. [274 words]
Graphical Abstract
Forest plot of MSC-EV effect on tumor growth accordinggenetic modification of EVs in animal studies identified from a systematicreview of the literature. All cohorts from studies with multiple interventiongroups are presented separately with control groups divided equally among thegroups. M, modified; H, hypoxia





Similar content being viewed by others
Data Availability
Not applicable.
Code Availability
Not applicable.
References
Tieu, A., Lalu, M. M., Slobodian, M., et al. (2020). An analysis of mesenchymal stem cell-derived extracellular vesicles for preclinical use. ACS Nano, 14(8), 9728–9743. https://doi.org/10.1021/acsnano.0c01363.
Ding, D.-C., Shyu, W.-C., & Lin, S.-Z. (2011). Mesenchymal stem cells. Cell Transplant, 20(1), 5–14. https://doi.org/10.3727/096368910X.
Allan, D., Tieu, A., Lalu, M., & Burger, D. (2020). Mesenchymal stromal cell-derived extracellular vesicles for regenerative therapy and immune modulation: Progress and challenges toward clinical application. Stem Cells Translational Medicine, 9(1), 39–46. https://doi.org/10.1002/sctm.19-0114.
Tieu, A., Slobodian, M., Fergusson, D. A., et al. (2019). Methods and efficacy of extracellular vesicles derived from mesenchymal stromal cells in animal models of disease: A preclinical systematic review protocol. Systematic Reviews, 8(1), 322. https://doi.org/10.1186/s13643-019-1242-y.
Oloyo, A. K., Ambele, M. A., & Pepper, M. S. (2018). Contrasting views on the role of mesenchymal stromal/stem cells in tumour growth: a systematic review of experimental design. Advances in Experimental Medicine and Biology, 1083, 103–124. https://doi.org/10.1007/5584_2017_118.
Lang, F. M., Hossain, A., Gumin, J., et al. (2018). Mesenchymal stem cells as natural biofactories for exosomes carrying miR-124a in the treatment of gliomas. Neuro-Oncology. https://doi.org/10.1093/neuonc/nox152.
(2019) P. G. Concise review: Adipose-derived stem cells (ASCs) and adipocyte-secreted exosomal microrna (A-SE-miR) modulate cancer growth and promote wound repair. Journal of Clinical Medicine. 8(6), 855. https://doi.org/10.3390/jcm8060855
Kordelas, L., Rebmann, V., Ludwig, A. K., et al. (2014). MSC-derived exosomes: A novel tool to treat therapy-refractory graft-versus-host disease. Leukemia, 28(4), 970–973. https://doi.org/10.1038/leu.2014.41.
Chen, W., Huang, Y., Han, J., et al. (2016). Immunomodulatory effects of mesenchymal stromal cells-derived exosome. The Journal of Immunology. https://doi.org/10.1007/s12026-016-8798-6.
van Niel, G., D’Angelo, G., & Raposo, G. (2018). Shedding light on the cell biology of extracellular vesicles. Nature Reviews Molecular Cell Biology, 19(4), 213–228. https://doi.org/10.1038/nrm.2017.125.
Yáñez-Mó, M., Siljander, P. R. M., Andreu, Z., et al. (2015). Biological properties of extracellular vesicles and their physiological functions. Journal of Extracellular Vesicles, 4, 27066. https://doi.org/10.3402/jev.v4.27066.
Kalluri, H., Kolli, C. S., & Banga, A. K. (2011). Characterization of microchannels created by metal microneedles: Formation and closure. American Association of Pharmaceutical Scientists Journal. https://doi.org/10.1208/s12248-011-9288-3.
Batrakova, E. V., & Kim, M. S. (2015). Using exosomes, naturally-equipped nanocarriers, for drug delivery. Journal of Controlled Release. https://doi.org/10.1016/j.jconrel.2015.07.030.
Z, Z. G. (2019). Exosomes - beyond stem cells for restorative therapy in stroke and neurological injury. Nature Reviews Neurology, 15(4), 193–203. https://doi.org/10.1038/s41582-018-0126-4.
L, P. G. B., A-M, S., et al. (2018). Mesenchymal stem cells-derived exosomes for wound regeneration. Advances in Experimental Medicine and Biology, 1119, 119–131. https://doi.org/10.1007/5584_2018_251.
Yaghoubi, Y., Movassaghpour, A., Zamani, M., Talebi, M., Mehdizadeh, A., & Yousefi, M. (2019). Human umbilical cord mesenchymal stem cells derived-exosomes in diseases treatment. Life Sciences, 233, 116733. https://doi.org/10.1016/j.lfs.2019.116733
Lopatina, T., Grange, C., Fonsato, V., et al. (2019). Extracellular vesicles from human liver stem cells inhibit tumor angiogenesis. International Journal of Cancer. https://doi.org/10.1002/ijc.31796.
Dong, L., Pu, Y., Zhang, L., et al. (2018). Human umbilical cord mesenchymal stem cell-derived extracellular vesicles promote lung adenocarcinoma growth by transferring miR-410 article. Cell Death and Disease. https://doi.org/10.1038/s41419-018-0323-5.
Rosenberger, L., Ezquer, M., Lillo-Vera, F., et al. (2019). Stem cell exosomes inhibit angiogenesis and tumor growth of oral squamous cell carcinoma. Scientific Reports. https://doi.org/10.1038/s41598-018-36855-6.
Bruno, S., Collino, F., Deregibus, M. C., Grange, C., Tetta, C., & Camussi, G. (2013). Microvesicles derived from human bone marrow mesenchymal stem cells inhibit tumor growth. Stem Cells and Development. https://doi.org/10.1089/scd.2012.0304.
Kalimuthu, S., Gangadaran, P., Li, X. J., et al. (2016). In Vivo therapeutic potential of mesenchymal stem cell-derived extracellular vesicles with optical imaging reporter in tumor mice model. Scientific Reports. https://doi.org/10.1038/srep30418.
Alzahrani, F. A., El-Magd, M. A., Abdelfattah-Hassan, A., et al. (2018). Potential effect of exosomes derived from cancer stem cells and MSCs on progression of DEN-Induced HCC in Rats. Stem Cells International. https://doi.org/10.1155/2018/8058979.
Raposo, G., & Stoorvogel, W. (2013). Extracellular vesicles: Exosomes, microvesicles, and friends. Journal of Cell Biology. https://doi.org/10.1083/jcb.201211138.
Moher, D., Liberati, A., Tetzlaff, J., et al. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Medicine, 6(7), e1000097. https://doi.org/10.1371/journal.pmed.1000097.
McGowan, J., Sampson, M., Salzwedel, D. M., Cogo, E., Foerster, V., & Lefebvre, C. (2016). PRESS peer review of electronic search strategies: 2015 guideline statement. Journal of Clinical Epidemiology, 75, 40–46. https://doi.org/10.1016/j.jclinepi.2016.01.021.
Viswanathan, S., Shi, Y., Galipeau, J., et al. (2019). Mesenchymal stem versus stromal cells: International Society for Cell & Gene Therapy (ISCT®) Mesenchymal Stromal Cell committee position statement on nomenclature. Cytotherapy, 21(10), 1019–1024. https://doi.org/10.1016/j.jcyt.2019.08.002.
Théry, C., Witwer, K. W., Aikawa, E., et al. (2018). Minimal information for studies of extracellular vesicles 2018 (MISEV2018): a position statement of the International Society for Extracellular Vesicles and update of the MISEV2014 guidelines. Journal of Extracellular Vesicles, 7(1), 1535750. https://doi.org/10.1080/20013078.2018.1535750.
Hooijmans, C. R., Rovers, M. M., De Vries, R. B. M., Leenaars, M., Ritskes-Hoitinga, M., & Langendam, M. W. (2014). SYRCLE’s risk of bias tool for animal studies. BMC Medical Research Methodology, 14, 43. https://doi.org/10.1186/1471-2288-14-43.
DerSimonian, R., & Laird, N. (1986). Meta-analysis in clinical trials. Controlled Clinical Trials. https://doi.org/10.1016/0197-2456(86)90046-2.
(2019) Cochrane Handbook for Systematic Reviews of Interventions. https://doi.org/10.1002/9781119536604.
Higgins, J. P. T., Thomas, J., Chandler, J., Cumpston, M., Li, T., & Page, M. J. W. V. (2019). Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane database Syst Rev. ;10:ED000142. https://doi.org/10.1002/14651858.ED000142.
Iranpour, S., Hosseinzadeh, A., & Alipour, A. (2019). Efficacy of miltefosine compared with glucantime for the treatment of cutaneous leishmaniasis: a systematic review and meta-analysis. Epidemiology and Health, 41, e2019011. https://doi.org/10.4178/epih.e2019011.
Ji, R., Zhang, B., Zhang, X., et al. (2015). Exosomes derived from human mesenchymal stem cells confer drug resistance in gastric cancer. Cell Cycle. https://doi.org/10.1080/15384101.2015.1005530.
Du, T., Ju, G., Wu, S., et al. (2014). Microvesicles derived from human Wharton’s jelly mesenchymal stem cells promote human renal cancer cell growth and aggressiveness through induction of hepatocyte growth factor. PLoS One. https://doi.org/10.1371/journal.pone.0096836.
Lee, J. K., Park, S. R., Jung, B. K., et al. (2013). Exosomes derived from mesenchymal stem cells suppress angiogenesis by down-regulating VEGF expression in breast cancer cells. PLoS One. https://doi.org/10.1371/journal.pone.0084256.
Wu, S., Ju, G. Q., Du, T., Zhu, Y. J., & Liu, G. H. (2013). Microvesicles derived from human umbilical cord wharton’s jelly mesenchymal stem cells attenuate bladder tumor cell growth in vitro and in vivo. PLoS One. https://doi.org/10.1371/journal.pone.0061366.
Katakowski, M., Buller, B., Zheng, X., et al. (2013). Exosomes from marrow stromal cells expressing miR-146b inhibit glioma growth. Cancer Letters. https://doi.org/10.1016/j.canlet.2013.02.019.
Zhu, W., Huang, L., Li, Y., et al. (2012). Exosomes derived from human bone marrow mesenchymal stem cells promote tumor growth in vivo. Cancer Letters. https://doi.org/10.1016/j.canlet.2011.10.002.
O’Brien, K. P., Khan, S., Gilligan, K. E., et al. (2018). Employing mesenchymal stem cells to support tumor-targeted delivery of extracellular vesicle (EV)-encapsulated microRNA-379. Oncogene. https://doi.org/10.1038/s41388-017-0116-9.
Grigorian-Shamagian, L., Fereydooni, S., Liu, W., Echavez, A., & Marbán, E. (2017). Harnessing the heart’s resistance to malignant tumors: Cardiacderived extracellular vesicles decrease fibrosarcoma growth and leukemia-related mortality in rodents. Oncotarget. https://doi.org/10.18632/oncotarget.20454.
Shi, S., Zhang, Q., Xia, Y., et al. (2016). Mesenchymal stem cell-derived exosomes facilitate nasopharyngeal carcinoma progression. Am J Cancer Res. 6(2):459-72.
Ko, S. F., Yip, H. K., Zhen, Y. Y., et al. (2015). Adipose-derived mesenchymal stem cell exosomes suppress hepatocellular carcinoma growth in a rat model: apparent diffusion coefficient, natural killer T-cell responses, and histopathological features. Stem Cells International. https://doi.org/10.1155/2015/853506.
Roccaro, A. M., Sacco, A., Maiso, P., et al. (2013). BM mesenchymal stromal cell-derived exosomes facilitate multiple myeloma progression. Journal of Clinical Investigation. https://doi.org/10.1172/JCI66517.
Ren, W., Hou, J., Yang, C., et al. (2019). Extracellular vesicles secreted by hypoxia pre-challenged mesenchymal stem cells promote non-small cell lung cancer cell growth and mobility as well as macrophage M2 polarization via miR-21-5p delivery. Journal of Experimental & Clinical Cancer Research. https://doi.org/10.1186/s13046-019-1027-0.
Lin, S., Zhu, B., Huang, G., Zeng, Q., & Wang, C. (2019). Microvesicles derived from human bone marrow mesenchymal stem cells promote U2OS cell growth under hypoxia: the role of PI3K/AKT and HIF-1α. Human Cell. https://doi.org/10.1007/s13577-018-0224-z.
Ding, Y., Cao, F., Sun, H., et al. (2019). Exosomes derived from human umbilical cord mesenchymal stromal cells deliver exogenous miR-145-5p to inhibit pancreatic ductal adenocarcinoma progression. Cancer Letters. https://doi.org/10.1016/j.canlet.2018.10.039.
Shamili, F. H., Bayegi, H. R., Salmasi, Z., et al. (2018). Exosomes derived from TRAIL-engineered mesenchymal stem cells with effective anti-tumor activity in a mouse melanoma model. International Journal of Pharmaceutics. https://doi.org/10.1016/j.ijpharm.2018.07.067.
Naseri, Z., Oskuee, R. K., Jaafari, M. R., & Moghadam, M. F. (2018). Exosome-mediated delivery of functionally active miRNA-142-3p inhibitor reduces tumorigenicity of breast cancer in vitro and in vivo. International Journal of Nanomedicine. https://doi.org/10.2147/IJN.S182384.
Mendt, M., Kamerkar, S., Sugimoto, H., et al. (2018). Generation and testing of clinical-grade exosomes for pancreatic cancer. JCI Insight. https://doi.org/10.1172/jci.insight.99263.
Li, H., Yang, C., Shi, Y., & Zhao, L. (2018). Exosomes derived from siRNA against GRP78 modified bone-marrow-derived mesenchymal stem cells suppress Sorafenib resistance in hepatocellular carcinoma. Journal of Nanobiotechnology. https://doi.org/10.1186/s12951-018-0429-z.
Kim, R., Lee, S., Lee, J., et al. (2018). Exosomes derived from microRNA-584 transfected mesenchymal stem cells: Novel alternative therapeutic vehicles for cancer therapy. BMB Reports. https://doi.org/10.5483/BMBREP.2018.51.8.105.
Kamerkar, S., Lebleu, V. S., Sugimoto, H., et al. (2017). Exosomes facilitate therapeutic targeting of oncogenic KRAS in pancreatic cancer. Nature. https://doi.org/10.1038/nature22341.
Vallabhaneni, K. C., Penfornis, P., Dhule, S., et al. (2015). Extracellular vesicles from bone marrow mesenchymal stem/stromal cells transport tumor regulatory microRNA, proteins, and metabolites. Oncotarget. https://doi.org/10.18632/oncotarget.3211.
Lou, G., Song, X., Yang, F., et al. (2015). Exosomes derived from MIR-122-modified adipose tissue-derived MSCs increase chemosensitivity of hepatocellular carcinoma. Journal of Hematology & Oncology. https://doi.org/10.1186/s13045-015-0220-7.
Henderson, V. C., Kimmelman, J., Fergusson, D., Grimshaw, J. M., & Hackam, D. G. (2013). Threats to validity in the design and conduct of preclinical efficacy studies: a systematic review of guidelines for in vivo animal experiments. PLoS Medicine, 10(7), e1001489. https://doi.org/10.1371/journal.pmed.1001489.
Busatto, S., Vilanilam, G., Ticer, T., et al. (2018). Tangential flow filtration for highly efficient concentration of extracellular vesicles from large volumes of fluid. Cells. https://doi.org/10.3390/cells7120273.
Mount, N. M., Ward, S. J., Kefalas, P., & Hyllner, J. (2015). Cell-based therapy technology classifications and translational challenges. Philosophical Transactions of the Royal Society B. https://doi.org/10.1098/rstb.2015.0017.
Funding
AB and was supported by funding from Canadian Blood Services. AT was supported by a Vanier Canada Graduate Scholarship from CIHR and the Canadian Vascular Network Scholar Award. MS was supported by The Ottawa Hospital Foundation. MML is supported by The Ottawa Hospital Anesthesia Alternate Funds Association and holds a University of Ottawa Junior Research Chair in Innovative Translational Research.
Author information
Authors and Affiliations
Contributions
All authors contributed to the design, conduct, analysis and/or writing of the manuscript. All authors approved of the final version of this manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors have no conflicts of interest to declare.
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article belongs to the Topical Collection: Special Issue on Exosomes and Microvesicles: from Stem Cell Biology to Translation in Human Diseases
Guest Editor: Giovanni Camussi
Rights and permissions
About this article
Cite this article
Bailey, A.J., Tieu, A., Gupta, M. et al. Mesenchymal Stromal Cell‐derived Extracellular Vesicles in Preclinical Animal Models of Tumor Growth: Systematic Review and Meta‐analysis. Stem Cell Rev and Rep 18, 993–1006 (2022). https://doi.org/10.1007/s12015-021-10163-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-021-10163-5