Abstract
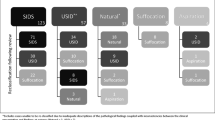
Although the rate of the sudden infant death syndrome (SIDS) has decreased over the last two decades, medical examiners and coroners are increasingly unwilling to use the SIDS diagnosis, particularly when there is an unsafe sleeping environment that might pose a risk for asphyxia. In order to reliably classify the infant deaths studied in a research setting in the mixed ancestory population in Cape Town, South Africa, we tested a classification system devised by us that incorporates the uncertainty of asphyxial risks at an infant death scene. We classified sudden infant deaths as: A) SIDS (where only a trivial potential for an overt asphyxial event existed); B) Unclassified—Possibly Asphyxial-Related (when any potential for an asphyxial death existed); C) Unclassified—Non-Asphyxial-Related (e.g., hyperthermia); D) Unclassified—No autopsy and/or death scene investigation; and E) Known Cause of Death. Ten infant deaths were classified according to the proposed schema as: SIDS, n = 2; Unclassified—Possibly Asphyxial-Related, n = 4; and Known Cause, n = 4. A conventional schema categorized the deaths as 6 cases, SIDS, and 4 cases, Known Cause, indicating that 4/6 (67%) of deaths previously classified as SIDS are considered related importantly to asphyxia and warrant their own subgroup. This new classification schema applies a simpler, more qualitative approach to asphyxial risk in infant deaths. It also allows us to test hypotheses about the role of asphyxia in sudden infant deaths, such as in brainstem defects in a range of asphyxial challenges.




Similar content being viewed by others
References
Krous HF, Beckwith JB, Byard RW, et al. Sudden infant death syndrome and unclassified sudden infant deaths: a definitional and diagnostic approach. Pediatrics. 2004;114(1):234–8.
Hauck FR, Tanabe KO. International trends in sudden infant death syndrome: stablization of rates requires further action. Pediatrics. 2008;122:660–6.
Mitchell EA, Brunt JM, Everard C. Reduction in mortality from sudden infant death syndrome in New Zealand: 1986–92. Arch Dis Child. 1994;70(4):291–4.
Beal SM. Sudden infant death syndrome in South Australia 1968–97. Part I: changes over time. J Pediatr Child Health. 2000;36(6):540–7.
Shapiro-Mendoza CK, Tomashek KM, Anderson RN, Wingo J. Recent national trends in sudden, unexpected infant deaths: more evidence supporting a change in classification or reporting. Am J Epidemiol. 2006;163(8):762–9.
The American Academy of Pediatrics. The changing concept of sudden infant death syndrome: diagnostic coding shifts, controversies regarding the sleeping environment, and new variables to consider in reducing risk. Pediatrics. 2005;116(5):1245–55.
Pasquale-Styles MA, Tackitt PL, Schmidt CJ. Infant death scene investigation and the assessment of potential risk factors for asphyxia: a review of 209 sudden unexpected infant deaths. J Forensic Sci. 2007;52(4):924–9.
Williams SM, Mitchell EA, Stewart AW, Taylor BJ. Temperature and the sudden infant death syndrome. Pediatr Perinat Epidemiol. 1996;10(2):136–49.
Fleming PJ, Levine MR, Azaz Y, Wigfield R, Stewart AJ. Interactions between thermoregulation and the control of respiration in infants: possible relationship to sudden infant death. Acta Pediatr Suppl. 1993;82 Suppl 389:57–9.
Harper RM. Autonomic control during sleep and risk for sudden death in infancy. Arch Ital Biol. 2001;139:185–94.
Molteno CD, Ress E, Kibel MA. Early childhood mortality in Cape Town. S Afr Med J. 1989;75:570–4.
Dempers JJ, Folkerth RD, Kinney HC, Odendaal H, Sens MA, Randall BB, Wadee SA. The institution of a standardized SIDS investigation protocol in South Africa: feasibility study of 11 cases in the Western Cape. International SIDS Meeting, Portsmouth, England, June, 2008 (Getting citation).
CDC for Disease Control and Prevention: Guidelines for death scene investigation of sudden, unexplained infant deaths: Recommendation of the interagency panel on sudden infant death scene investigation. MMWR. 1996;45(RR-10):1–6.
Thach BT. Tragic and sudden death. Potential and proven mechanisms causing sudden infant death syndrome. EMBO Rep. 2008;9(2):114–8.
McKenna JJ, Ball HL, Gettier LT. Mother-infant cosleeping, breastfeeding and sudden infant death syndrome: what biological anthropology has discovered about normal infant sleep and pediatric sleep medicine. Am J Phys Anthropol. 2007; Suppl 45:133–61.
Brenner RA, Simons-Morton BG, Bhaskar B, Ravenus M, Das A, Clemens JD. Infant parent bed sharing in an inner-city population. Arch Pediatr Adolesc Med. 2003;157:33–9.
Kemp JS, Kowalski RM, Burch PM, Graham MA, Thach BT. Unintentional suffocation by rebreathing: a death scene and physiologic investigation of a possible cause of sudden infant death. J Pediatr. 1993;122(6):874–80.
Patel AL, Harris K, Thach BT. Inspired CO(2) and O(2) in sleeping infants rebreathing from bedding: relevance for sudden infant death syndrome. J Appl Physiol. 2001;91(6):2537–45. incidence of SIDS with bed sharing.
Kemp JS, Unger B, Wilkins D, et al. Unsafe sleep practices and an analysis of bedsharing among infants dying suddenly and unexpectedly: results of a four-year, population-based, death-scene investigation study of sudden infant death syndrome and related deaths. Pediatrics. 2000;106(3):E41. bed sharing and hypercapnia.
Thach BT, Lijowska A. Arousals in infants. [Review] [11 refs]. Sleep. 1996;19(10 Suppl):S271–3.
Sridhar R, Thach BT, Kelly DH, Henslee JA. Characterization of successful and failed autoresuscitation in human infants, including those dying of SIDS. Pediatr Pulmonol. 2003;36(2):113–22.
Meny RG, Carroll JL, Carbone MT, Kelly DH. Cardiorespiratory recordings from infants dying suddenly and unexpectedly at home. Pediatrics. 1994;93(1):44.
Poets CF. Apparent life-threatening events and sudden infant death on a monitor. Paediatr Respir Rev. 2004;5 Suppl A:S383–6.
Kinney HC, Richerson GB, Dymecki SB, Darnall RA, Nattie EE. The brainstem, serotonin, and sudden infant death syndrome: a review. Annu Rev Pathol Mech Dis. 2009;4:517–49.
Cutz E, Perrin DG, Pan J, Haas EA, Krous HF. Pulmonary neuroendocrine cells and neuroepithelial bodies in sudden infant death syndrome: potential markers of airway chemoreceptor dysfunction. Pediatr Dev Pathol. 2007;10:106–16.
Vege A, Chen Y, Opdal SH, Saugstad OD, Rognum TO. Vitreous humor hypoxanthine levels in SIDS and infectious death. Acta Paediatr. 1994;83(6):634–9.
Jones KL, Krous HF, Nadeau J, Blackbourne B, Zielke HR, Gozal D. Vascular endothelial growth factor in the cerebrospinal fluid of infants who died of sudden infant death syndrome: evidence for antecedent hypoxia. Pediatrics. 2003;111:358–63.
Kinney HC, Burger PC, Harrell FE Jr, Hudson RP Jr. ‘Reactive gliosis’ in the medulla oblongata of victims of the sudden infant death syndrome. Pediatrics. 1983;72(2):181–7.
Takashima S, Armstrong D, Becker L, Bryan C. Cerebral hypoperfusion in the sudden infant death syndrome? Brainstem gliosis and vasculature. Ann Neurol. 1978;4(3):257–62.
Paterson DS, Trachtenberg FL, Thompson EG, et al. Multiple serotonergic brainstem abnormalities in sudden infant death syndrome. JAMA. 2006;296(17):2124–32.
Acknowledgments
We appreciate the help of Mr. Richard A. Belliveau in manuscript preparation. Drs. Eugene E. Nattie and Henry F. Krous provided critical reviews.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Randall, B.B., Wadee, S.A., Sens, M.A. et al. A practical classification schema incorporating consideration of possible asphyxia in cases of sudden unexpected infant death. Forensic Sci Med Pathol 5, 254–260 (2009). https://doi.org/10.1007/s12024-009-9083-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12024-009-9083-y