Abstract
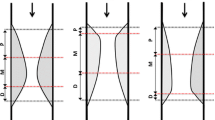
Inflammation has been recognized as a critical process in the progression of coronary atherosclerosis. Virtual Histology-intravascular ultrasound (VH-IVUS) has been reported to be a useful tool for tissue characterization of coronary atherosclerotic plaque. We investigated relationships between plaque composition and inflammation-related factors possibly contributing to atheromatous plaque formation and progression, since these are largely unknown. Using VH-IVUS, we measured plaque volume and composition at the culprit lesions in patients with stable angina undergoing elective percutaneous coronary intervention (n = 33, 39 de novo lesions), and then analyzed correlations between plaque components and serum levels of inflammatory factors in both aorta and culprit coronary artery obtained by aspiration using a distal protection device. Linear regression analysis revealed that both aortic and coronary LDL cholesterol levels correlated with %plaque burden along the culprit lesions (r = 0.535 and 0.539, respectively), but with none of the plaque components. Of %plaque components, fibro-fatty (FF) correlated positively with both aortic and coronary T cell/B cell ratios (r = 0.335 and 0.359, respectively) whereas necrotic core (NC) correlated negatively with both aortic and coronary T cell/B cell ratios (r = −0.373 and −0.483, respectively). These results suggest that LDL cholesterol may be a good marker for total coronary plaque volume whereas the lymphocyte subset of T cell/B cell ratios may be a good marker for plaque composition, especially FF and NC components volume.





Similar content being viewed by others
References
Libby P. Inflammation in atherosclerosis. Nature. 2002;420:868–74.
Berk BC, Weintraub WS, Alexander RW. Elevation of C-reactive protein in “active” coronary artery disease. Am J Cardiol. 1990;65:168–72.
Lagrand WK, Visser CA, Hermens WT, Niessen HWM, Verheugt FWA, Wolbink G-J, et al. C-reactive protein as a cardiovascular risk factor. More than an epiphenomenon? Circulation. 1999;100:96–102.
Aukrust P, Müller F, Ueland T, Berget T, Aaser E, Brunsvig A, et al. Enhanced levels of soluble and membrane-bound CD40 ligand in patients with unstable angina. Possible reflection of T lymphocytes and platelet involvement in the pathogenesis of acute coronary syndromes. Circulation. 1999;100:614–20.
Heeschen C, Dimmeler S, Hamm CW, van den Brand MJ, Boersma E, Zeiher AM, et al. Soluble CD40 ligand in acute coronary syndromes. N Eng J Med. 2003;348:1104–11.
Mach F, Schönbeck U, Sukhova GK, Bourcier T, Bonnefoy J-Y, Pober JS, et al. Functional CD40 ligand is expressed on human vascular endothelial cells, smooth muscle cells, and macrophages: Implications for CD40-CD40 ligand signaling in atherosclerosis. Proc Natl Acad Sci USA. 1997;94:1931–6.
Bruemmer D, Riggers U, Holzmeister J, Grill M, Lippek F, Settmacher U, et al. Expression of CD40 in vascular smooth muscle cells and macrophages is associated with early development of human atherosclerotic lesions. Am J Cardiol. 2001;87:21–7.
Schönbeck U, Libby P. CD40 signaling and plaque instability. Circ Res. 2001;89:1092–103.
Szmitko PE, Wang C-H, Weisel RD, de Almeida JR, Anderson TJ, Verma S. New markers of inflammation and endothelial cell activation. Circulation. 2003;108:1917–23.
Liuzzo G, Biasucci LM, Gallimore JR, Grillo RL, Rebuzzi AG, Pepys MB, et al. The prognostic value of C-reactive protein and serum amyloid A protein in severe unstable angina. N Eng J Med. 1994;331:417–24.
Maier W, Altwegg LA, Corti R, Gay S, Hersberger M, Maly FE, et al. Inflammatory markers at the site of ruptured plaque in acute myocardial infarction. Locally increased interleukin-6 and serum amyloid A but decreased C-reactive protein. Circulation. 2005;111:1355–61.
Inoue T, Kato T, Uchida T, Sakuma M, Nakajima S, Shibazaki M, et al. Local release of C-reactive protein from vulnerable plaque or coronary arterial wall injured by stenting. J Am Coll Cardiol. 2005;46:239–45.
Satoh S, Mori E, Yokoyama S, Kimura Y, Sagara Y, Mori T, et al. Characterization of differences in inflammatory markers and lymphocyte subsets at culprit lesions in patients with stable angina and acute myocardial infarction. Jpn J Interv Cardiol. 2009;23:422–9.
Nair A, Kuban BD, Tuzcu EM, Schoenhagen P, Nissen P, Vince DG. Coronary plaque classification with intravascular ultrasound radiofrequency data analysis. Circulation. 2002;106:2200–6.
Garcia-Garcia HM, Goedhart D, Serruys PW. Relation of plaque size to necrotic core in the three major coronary arteries in patients with acute coronary syndrome as determined by intravascular ultrasonic imaging radiofrequency. Am J Cardiol. 2007;99:790–2.
Higashikuni Y, Tanabe K, Yamamoto H, Aoki J, Nakazawa G, Onuma Y, et al. Relationship between coronary artery remodeling and plaque composition in culprit lesions. An intravascular ultrasound radiofrequency analysis. Circ J. 2007;71:654–60.
Philipp S, Böse D, Wijns W, Marso SP, Schwartz RS, Konig A, et al. Do systemic risk factors impact invasive findings from virtual histology? Insights from the international virtual histology registry. Eur Heart J. 2010;31:196–202.
Nicholls SJ, Hsu A, Wolski K, Hu B, Bayturan O, Lavoie A, et al. Intravascular ultrasound-derived measures of coronary atherosclerotic plaque burden and clinical outcome. J Am Coll Cardiol. 2010;55:2399–407.
Witzum JL, Steinberg D. Role of oxidized low density lipoprotein in atherogenesis. J Clin Invest. 1991;88:1785–92.
Satoh S, Oyama J, Suematsu N, Kadokami T, Shimoyama N, Okutsu M, et al. Increased productivity of tumor necrosis factor-alpha in helper T cells in patients with systolic heart failure. Int J Cardiol. 2006;111:405–12.
Ogasawara D, Shite J, Shinke T, Watanabe S, Otake H, Tanino Y, et al. Pioglitazone reduces the necrotic-core component in coronary plaque in association with enhanced plasma adiponectin in patients with type 2 diabetes mellitus. Circ J. 2009;2009:343–51.
Schönbeck U, Gerdes N, Varo N, Reynolds RS, Horton DB, Bavendiek U, et al. Oxidized low-density lipoprotein augments and 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibitors limit CD40 and CD40L expression in human vascular cells. Circulation. 2002;106:2888–93.
De Palma R, Del Galdo F, Abbate G, Chiariello M, Calabró R, Forte L, et al. Patients with acute coronary syndrome show oligoclonal T-cell recruitment within unstable plaque. Evidence for a local, intracoronary immunologic mechanism. Circulation. 2006;113:640–6.
Matsuzaki M, Kita T, Mabuchi H, Matsuzawa Y, Nakaya N, Oikawa S, et al. Large scale cohort study of the relationship between serum cholesterol concentration and coronary events with low-dose simvastatin therapy in Japanese patients with hypercholesterolemia. Circ J. 2002;66:1087–95.
Hatanaka K, Li XA, Masuda K, Yutani C, Yamamoto A. Immunohistochemical localization of C-reactive protein-binding sites in human atherosclerotic aortic lesions by a modified streptavidin-biotin-staining method. Pathol Int. 1995;45:635–41.
Ishikawa T, Hatakeyama K, Imamura T, Date H, Shibata Y, Hikichi Y, et al. Involvement of C-reactive protein obtained by directional coronary atherectomy in plaque instability and developing restenosis in patients with stable or unstable angina pectoris. Am J Cardiol. 2003;91:287–92.
Lagrand WK, Niessen HWM, Wolbink G-J, Jaspars LH, Visser CA, Verheugt FWA, et al. C-reactive protein colocalizes with complement in human hearts during acute myocardial infarction. Circulation. 1997;95:97–103.
Gauldie J, Richards C, Northemann W, Fey G, Baumann H. IFNb2/BSF2/LI-6 is the monocyte-derived HSF that regulates receptor specific acute phase gene regulation in hepatocytes. Ann N Y Acad Sci. 1989;557:46–59.
Smith JW, McDonald TL. Production of serum amyloid A and C-reactive protein by HepG2 cells stimulated with combination of cytokines or monocyte conditioned media: the effects of prednisolone. Clin Exp Immunol. 1992;90:293–9.
Calabró P, Willerson JT, Yeh ETH. Inflammatory cytokines stimulated C-reactive protein production by human coronary artery smooth muscle cells. Circulation. 2003;108:1930–2.
Acknowledgments
The authors are very grateful to the co-medical staffs in the Departments of Clinical Laboratory, and Radiology, National Hospital Organization Kyushu Medical Center for their expert technical assistance. We have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Satoh, S., Mori, E., Takenaka, K. et al. Relationships between inflammatory mediators and coronary plaque composition in patients with stable angina investigated by ultrasound radiofrequency data analysis. Cardiovasc Interv and Ther 26, 193–201 (2011). https://doi.org/10.1007/s12928-011-0058-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12928-011-0058-z