Abstract
Status of lymph node metastasis has important implications in deciding treatment of oncologic patients. The appropriate choice of imaging modality is crucial to obtain accurate evaluation of lymph node status. Current imaging methods are mainly divided into two categories, conventional structural imaging and more recently emerging functional imaging. In depth understanding of these imaging tools is essential in making the correct choice for individual patients, and eventually for better diagnosis and treatment.
Similar content being viewed by others
Introduction
Lymph node (LN) metastasis is an important prognostic factor for most malignancies. The site and the number of metastatic LNs directly influence the staging of the tumors, and consequently affect selection of a treatment plan and patient’s survival rate. Over-staging often leads to unnecessary extended surgical interventions, and added morbidity; under-staging, on the other hand, may lead to increase in recurrence rate and may shorten the survival time. Therefore, it is crucial to choose the right imaging approach for LN evaluation.
An ideal imaging method should be able to clearly detect and display the site and structural characteristics of LNs, accurately distinguish the malignant nodes from benign ones, and be widely available, affordable, easy to interpret, non-invasive and non-radiative. Unfortunately, current-imaging modalities mainly rely on anatomical and morphological assessment, and provide little information into the functional aspect of LNs. Our decision-making is still based on the structural criteria shortcomings that have been extensively studied and published [1, 2, 3••, 4•]. The purpose of the following review is to focus on the conventional methods such as ultrasound (US), computed tomography (CT), magnetic resonance imaging (MRI), and some novel methods like diffusion weighted imaging of MRI, positron emission tomography (PET) or PET/CT and MRI and novel MR contrasts with reference to characterization of LNs. Merits and demerits of each modality are discussed, along with recent advances.
Sonography
Gray Scale US
Gray scale US is the most common method for evaluating superficial LNs. It is economically affordable, widely available, easy to use and has a good safety profile [5]. High frequency linear array US transducers are typically used for evaluating superficial LNs, such as those located in the neck, inguinal region or the axillary fossa. With high spatial resolution, high frequency US can evaluate the nodes for shape, size, echotexture and anatomical demarcation of the cortex and medulla in LNs (Table 1). The absence of a fatty hilum caused by cortical thickening in a LN is regarded as the most specific predictive factor for metastasis [6, 7]. Sonography has much higher sensitivity than high-resolution CT (29 %) [8] in detecting LN hilum (Fig. 1). Moghaddam et al. [7] reported an echogenic hilum of cervical LN in 81 % of benign LNs and 55 % of malignant ones, thus pointing the absence of hilum as a marker for LN involvement on US. The sensitivity and specificity were 45 % and 81 %, respectively. On this basis, Song et al. promoted the significance of the cortex-hilum (CH) area ratio on gray-scale US imaging in diagnosing axillary LN. They recommend that the CH area ratio (> 2) of an axillary LN on US be used as a quantitative indicator for the diagnosis of LN metastasis due to its superior sensitivity of 94.1 % [9]. But it is important to note that the invisibility of LN hilum can also occur in chronically inflamed LNs and small benign LNs [10]. Besides hilum, some other specific signs within LNs can be displayed by US, such as necrosis and microcalcifications (Fig. 2). Necrosis is often caused by tumor metastasis, inflammation and treatments. Microcalcifications are considered as a better predictor of malignant thyroid carcinoma, with a high specificity of 96.5 % [11–13]. However, due to the limited penetration, high frequency US cannot be used for evaluating deeper LNs, such as deeper LNs in the neck, abdominal, deep pelvic or retroperitoneal areas, which could only be evaluated by low frequency US with less detail of the intranodal architectural changes [14]. Moreover, different etiologies of lymphadenopathy can show identical appearances on sonogram. For example, inflammatory LNs and metastatic LNs may present as enlarged, elliptical LNs with necrosis, which makes the differential diagnosis difficult.
Hilum of lymph node can be demonstrated by multiple imaging methods. a Gray-scale ultrasound shows hyperechoic hilar structure (arrow) in a benign enlarged cervical lymph node. b Gray-scale ultrasound demonstrated a metastatic cervical lymph node with absence of hyperechoic hilar structure in a woman with thyroid cancer. c On axial CT scan, hilar structures are often visualized as fat density (arrow), as shown in this right sided enlarged inguinal lymph node. d The coronal T1 weighted fat saturated image showing the hilar structures (arrow) on MRI
Sonography can identify the changes of the internal structure and the vascularity in lymph nodes. a Gray-scale ultrasound displays a cluster of microcalcifications (arrow) in a lymph node that was pathologically confirmed as metastasis from thyroid cancer. b Gray-scale ultrasound can clearly show necrosis (arrow) in a cervical lymph node. c Color Doppler demonstrated a increasing vascularity in a metastatic lymph node in this patient with thyroid cancer. d An inflammatory lymph node showed slightly increased vascularity on color Doppler. e Ultrasound provides a useful tool to guide biopsy of superficially located LNs
Color Doppler
Color Doppler is useful in distinguishing non-metastatic nodes from metastatic nodes based on the vascularity of LNs (Table 1). Abundant vascularity in LN is often linked with reactive proliferation, lymphoma and metastasis (Fig. 2), especially if the vessels are derived from outside the hilum. Imani et al. [7] reported peripheral and mixed vascular patterns had 100 % specificity in detecting metastatic cervical LNs. Dangore-Khasbage et al. [15] explained these signs may be due to new revascularization from peripheral vessels inducted by the destruction of hilar vascularity. Additionally, Color Doppler flow imaging provides quantitative parameters of vascularity in LN, such as pulsatility index (PI) and arterial resistive index (RI). In their assessment of cervical LNs by triplex sonography (gray scale, color mapping and spectral Doppler), Mazaher et al. stated the mean RI (> 0.8) and PI were significantly higher in malignant LNs (> 1.5) than in benign LNs, possibly owing to the compression of intranodal vessels by the tumor cells.
Advances in Sonography
Contrast enhanced US is emerging as a new technique for nodal characterization. It is more sensitive than grey scale imaging in displaying subtle intra-nodular necrosis, which manifests as rim enhancement [16]. Enhanced US offers additional advantages in guiding US fine needle aspiration (USFNA) by avoiding the sampling of nodal necrotic areas. Endoscopic ultrasonogrphy (EUS) is another method in predicting deep-seated nodes like mediastinal LNs metastasis even smaller than 5 mm with an accuracy of 84 %, while the accuracy of CT is only 49 % [17]. It’s also provides an opportunity for simultaneous US guided FNA.
Computed Tomography
Since the rapid development both in hardware and software in the last decade, the temporal and spatial resolution of CT has seen remarkable improvement. CT has now become the most important and commonly used method for pretreatment evaluation of cancer patients. As a structural imaging method, the CT diagnostic criteria for metastatic LNs mainly depends on location and the structural features, such as size, shape, margin, density and enhancement patterns (Table 1). Among them, size is still the most common criterion, though with a wide variable range from 5 to 15 mm. A short axis diameter beyond 1 cm is generally accepted as a threshold for malignancy in most studies [18–20] (Fig. 3). However, the diagnostic sensitivity of this standard is obviously weakened by a high false negative ratio, according to 21–74 % metastatic LNs with normal size [21–23] (Fig. 4). For example, Tiguert et al. found the proportion of metastatic LNs with an axial size less than 1 cm and 5 mm could reach 74 and 26 %, respectively, in patients with prostate cancer [23]. Fukuya et al. [22] also detected 28 % metastatic LNs smaller than 9 mm in gastric cancer. A submillimeter spatial resolution of CT has significantly improved the capability of detecting these normal or small size LNs. The reconstructed three-dimensional (3D) images help in distinguishing nodes from small vessels (Fig. 3) and describing the structural details of LNs. According to Yang et al., an accuracy for determination of LN metastasis was 90 and 71 % in early and advanced gastric cancer, respectively, with an overall accuracy of 80 % by using 64-multidetector CT (MDCT) and multi-plane reformation technique [24]. Even more recently, nodular volumetry based on three-dimensional (3D) reconstructive technique showed promising results in malignant lymphoma. Puesken et al. found that accuracies for volumetry in the cervical/inguinal region were significantly higher compared with long-axis diameter (LAD) and 3D diameter in malignant lymphoma. Therefore, adding LN volumetry to single LAD assessment was recommended for accurate structural categorization of LNs in malignant lymphoma [25]. Besides the high spatial resolution, the prominent temporal resolution of MDCT provides help to detect perigastric and peribowel LNs for avoiding motion artifacts from respiratory and bowel peristalsis to a great extent. Although these advanced techniques have improved the diagnostic ability of MDCT in LN evaluation to some degree, it is difficult to have high sensitivity, especially if we rely only on the nonspecific structural criteria. The diagnostic accuracy of size is influenced by reactive hyperplasia of LNs (Fig. 5) and micrometastasis. The former may increase the number of benign nodes with abnormal diameter or false-positive results; conversely, the latter may increase the number of metastatic nodes with normal diameter or false-negative results, as mentioned above. Consequently, it is difficult to choose an appropriate cutoff to balance the sensitivity and specificity at the same time. If taking ≥ 10 mm as a positive criterion for axillary LN metastasis, the sensitivity and specificity are 50 and 75 %, respectively [26]. Peters et al. adopted a smaller criterion of ≥ 5 mm to evaluate the presence of paratracheal LN metastasis, showing change in sensitivity and specificity of CT to 70 and 36 %, respectively. For the variable diagnostic accuracy, CT is more often used as an anatomical location tool to biopsy (Fig. 3) and PET in LNs evaluation, rather than a differential diagnostic tool. In addition, relying on subcutaneous injection of some special contrast, iohexol or iopamidol, CT can provide locating information for sentinel lymph nodes (SLNs) and display lymphatic pathways of some tumors [27, 28]. Last but not least, though the lower interobserver variation and high reproducibility enable MDCT for follow-up examinations, ionizing radiation risk should be considered in vulnerable populations such as children and young adults [29 •, 30].
A 60-year-old man with a history of prostate carcinoma. a Venous phase CT image showing multiple enlarged aortocaval lymph nodes (arrow) with ill-defined border, and heterogeneous enhancement were seen measuring up to 2.2 × 1.3 cm. b Coronal reconstructed CT image clearly displayed the adjacent relationship between nodes (arrow) and main vessels. c CT-guided biopsy was performed and the largest node was positive for malignant cells on pathology
A 44-year-old woman with a history of breast cancer and axillary node metastasis. a The axial T1 weighted image showed multiple enlarged left axillary lymph nodes, with the largest node measuring 2.0 × 1.5 cm. b On the axial T2 weighted imaging, the largest node displayed heterogeneous internal texture. c On enhanced MRI scan, the nodes showed significant enhancement with a small necrosis in the largest one (arrow head). d Axial CT scan also demonstrated the necrosis (arrow head). e On axial T1 weighted image, another small metastatic node with a short diameter of 4 mm and well-defined border was noted on the anterior chest wall adjacent axillary. f On axial T2 weighted image, the small node showed similar high signal intensity with the largest node. g Enhanced T1 weighted image also demonstrated a significant enhancement of the small node. h On enhanced CT scan, the small one showed a moderate enhancement
A 53-year-old man with severe peripheral vascular disease. a On axial non-enhanced CT scan, a cluster of enlarged lymph nodes (arrow heads) with homogeneous moderate density was identified in the pelvis along the left external iliac and inguinal regions. b PET image showed an extensive increased fluorodeoxyglucose (FDG) uptake in these nodes (arrows heads). c On color Doppler image, a diffusely increased vascularity was observed in the nodes. d Ultrasound-guided fine needle biopsy demonstrated reactive nodal hyperplasia
Magnetic Resonance Imaging
Conventional MRI
Conventional MRI has high repeatability and reliability in evaluating LNs status; however, it is not better than US and MDCT in diagnostic accuracy based only on structural size criteria [31]. In a meta-analysis of pelvic LNs in patients with prostate cancer, Hovels et al. reported the pooled sensitivity and specificity of CT and MRI were 42 and 82 %, and 39 and 82 %, respectively. The differences in performance of CT and MRI were not statistically significant [32]. Comparing pelvic MRI and endorectal ultrasonography (ERUS) in 34 patients with rectal tumor, Halefoglu et al. concluded that MRI gave an accuracy of 74.50 % with a sensitivity of 61.6 % and a specificity of 80.88 %, similar to those in ERUS, 76.47, 52.94 and 84.31 %, respectively [33 •]. In another meta-analysis study of cervical LNs in patients with head and neck squamous cell carcinoma, Wu et al. found the sensitivity, specificity and positive likelihood ratios of MRI were 76, 86 % and 5.47, respectively, and stated that the comparison of MRI performance with that of other diagnostic tools (PET, CT, and US) suggested no major differences between any of these methods [34]. With high spatial and soft tissue resolution based on multiple sequences and parameters, MRI provides additional structural diagnostic information to demonstrate nodal relationship with adjacent structures and intranodal textures, which may benefit the characterization of the small LNs and differential diagnosis. In uterine cervical cancer patients, Kim et al. demonstrated the accuracy, sensitivity and specificity of MRI with a short axis diameter of 1.0 cm had 93.0, 62.2 and 97.9 %, respectively [35]. In a study about LN detection of pelvic malignancies, Saokar et al. reported that MRI detected more LNs compared to CT in all nodal regions, including the external iliac, obturator, and internal iliac chains. Based on size, the numbers of nodes detected by CT and MRI were equal when nodal size above 10 mm; however, when size is 1–5 mm, MRI is capable to detect more nodes [36]. In a MRI study of pelvic LNs in cervical carcinoma, Yang et al. obtained a higher sensitivity and specificity of 70.6 and 89.8 %, respectively, using a size threshold of 1 cm in long axis diameter or the presence of central necrosis [37]. Moreover, without ionizing radiation, repeated MR scans can routinely be used for observation of postoperative LN metastasis and therapeutic effects.
In contrast, a relatively long scanning time makes MRI more susceptible to motion artifacts from breath or gastrointestinal peristalsis [38]. That may limit its use in evaluating regional LNs of chest and abdominal malignancies. Fortunately, some new emerging techniques have shown capabilities to improve the quality of MR images in these regions, through increasing temporal resolution and reducing the influence of motion artifacts; for instance, radial gradient echo sequence with K-space weighted image contrast (KWIC) and periodically rotated overlapping parallel lines with enhanced reconstruction (PROPELLER) sequences [39 •, 40, 41].
Diffusion Weighted Imaging
Different from conventional MRI, functional magnetic resonance imaging (fMRI) may allow a more accurate evaluation of malignant involvement based on metabolic or physiological changes in the LNs, aside from the structural signs mentioned above. As a simple, fast, non-invasive and non-contrast tool, diffusion weighted imaging (DWI) has been the most potential representative of fMRI in LNs mapping in recent years [34, 42, 43]. Some authors observed that both benign and malignant LNs demonstrated high signal intensity in pelvic cancers [44, 45], which formed a strong contrast against the dark background signal from fat deposited around LNs. Depending on the high contrast, DWI can provide a greater capacity to detect LNs and a more simple interpretation for both radiologists and clinicians [44, 46] (Fig. 6). Moreover, fused with high-resolution, T2 weighted images can make up for the weakness of DWI on anatomic details and result in its increased performance [47]. DWI can reflect the random (Brownian) motion of water molecules in the microstructure of LNs, and with the apparent diffusion coefficient (ADC), it further provides a quantitative evaluation to different physiological status of LNs. In theory, when comparing with normal or benign tissue, malignant tissue has a larger cell size, higher cellularity and nucleus to cytoplasm ratio, which may limit diffusion movement of water molecules and hence cause a higher signal on DWI with a lower ADC value [48, 49]. The correlation between cell density and normalized ADC (r = −0.58; p = 0.023) was studied by Ginat et al. [50•] for malignant skull lesions. Multiple studies on nodal DWI demonstrated there is a difference between benign and malignant nodes on diffusion weighted images and ADC maps. Lee et al. reported ADC value can help to differentiate malignant from benign LNs in predicting of nodal metastasis in head and neck cancer. Using a threshold value of 0.851 × 10−3 mm2 s−1, the accuracy, sensitivity and specificity of ADC value for differential diagnosis are 91.0, 91.3 and 91.1 %, respectively [51•]. In a retrospective study of pelvic LNs in patients with prostate cancer, Eiber et al. found there was a significant difference between the mean ADC value (×10−3 mm2 s−1) of malignant (1.07 ± 0.23) versus benign (1.54 ± 0.25) LNs, even in subgroup for LNs smaller versus larger than 10 mm. At a cutoff 1.30 × 10−3 mm2 s−1, a good accuracy of 85.6 % with a sensitivity of 86.0 % and specificity of 85.3 % was obtained, which was superior to a size-based analysis at a cutoff of 8 mm (accuracy, sensitivity and specificity in their study was 66.1, 82.0 and 54.4 %, respectively) [52]. The reasons for a more powerful diagnostic ability of DWI than other size-dependent imaging methods may be due to two aspects. One is that more normal size LNs with micrometastasis are evaluated correctly, and another is hyperplastic benign nodes are appropriately excluded. Not all the researchers admitted the advantage of DWI and ADC value in differential diagnosis of LNs. Roy et al. reported there were no significant differences in ADC values in metastatic nodes and control nodes (p > 0.05), and the mean ADC (×10−3 mm3 s−1 ± SD) of involved nodes, control iliac nodes, control inguinal nodes and control iliac plus inguinal were 924 ± 217, 968 ± 182 and 1,036 ± 181, respectively [44]. In addition, a new technique named as diffusion-weighted whole-body imaging with background body signal suppression (DWIBS) provides data which can be post-processed to create a whole body LN map as similar to PET, so it is also called as “PET-like” imaging [53]. This technique acquires images during free breathing, and obtains more outstanding contrast LNs maps than conventional DWI by means of multiple signal averaging, fat suppression pre-pulse and heavy diffusion weighting. But DWIBS needs to be interpreted with T1 or T2 weighted images for better anatomical correlation. Although DWI has been widely accepted in the diagnosis of intracranial diseases, it has not become a clinical standard in body imaging. In spite of this, the most common sequence of single-shot echo-planar imaging (EPI) is easily affected by magnetic susceptibility artifacts and produces image distortion in the body. These drawbacks may be more obvious when small LNs in mediastinal and perigastrointestinal areas are evaluated. In summary, DWI is a powerful tool to detect the number and site of LNs, but with a indefinite accuracy in differential diagnosis and a relative unstable imaging quality.
A 65-year-old woman with a history of bladder cancer. a On diffusion weighted image, multiple left-sided retroperitoneal lymph nodes were identified adjacent to the left renal vein with high signal intensity. The largest one with a size of 3.0 × 1.5 cm was significantly enlarged as per the size criteria. b On ADC map, the largest one showed low signal intensity due to restricted diffusion. c On T2 weighted image, the nodes showed high signal intensity. d Post-contrast scan demonstrated significant homogeneous enhancement in the nodes. e The CT-guilded biopsy of the node demonstrated reactive hyperplasia. f On the follow-up scan after 14 months, the node remained stable in size on DWI
Novel MRI Contrast Agents
Compared to DWI and other structural imaging methods, some novel lymphotropic contrasts such as ferumoxtran-10, ferumoxytol and gadofluorine M showed a significantly higher sensitivity and specificity in discriminating metastatic LNs from non-metastatic ones in recent years [54–57, 58•, 59]. Ferumoxtran-10 and ferumoxytol are reticuloendothelial system–targeted MR imaging contrast agents consisting of ultrasmall superparamagnetic iron oxide particles. These nanoparticles can get into the reticuloendothelial system through capillary walls and be carried to LNs by macrophages [54]. A normal LN contains a large amount of macrophages which show a low signal intensity with ferumoxtran-10 because of the T2 shortening effect of the nanoparticles. In contrast, metastatic LNs retain high signal intensity for absence of macrophages with nanoparticles caused by tumor involvement [55, 60] (Fig. 7). An excellent high diagnostic sensitivity and specificity of ferumoxtran-10 was demonstrated in evaluation of various regional LNs. In a prostate cancer LNs MRI study with lymphotropic superparamagnetic nanoparticles, Harisinghani et al. correctly identified all 33 patients with metastases, and obtained a perfect sensitivity of 100 % on a patient-by-patient analysis, as well as a significantly higher sensitivity and specificity than conventional MRI (90.5 vs. 35.4 %, 90.4 vs. 97.8 %, respectively) or nomograms on node-by-node analysis. This differential diagnostic advantage is more obvious when detecting small LNs (a short diameter of 5–10 mm), in which the sensitivity of MRI with ferumoxtran-10 can reach 96.4 %. The improved detecting ability of normal size LNs with micrometastasis may be a reasonable explanation for that [55]. Unfortunately, ferumoxtran-10, with its significantly high accuracy, is not accepted as a routine tool for LN evaluation, because of its commercial unavailability, time consuming scan (at least 24–48 h) [61] and long interpretation time (median reading time: 80 min) [56]. Thoeny et al. combined ferumoxtran-10 with DWI (USPIO–DW–MRI) and utilized a larger signal difference between malignant and benign nodes caused by signal overlay from diffusion and T2/T2* after ferumoxtran-10 to effectively reduce the median reading time from 80 to 13 min [56]. Gadofluorine M (Schering, Berlin, Germany) is another emerging LN-selective MRI contrast agent used in T1 weighted sequence. It is a macrocyclic gadolinium chelate with a perfluorinated side chain and results in formation of micelles in aqueous solutions [57, 58•]. This agent has potential for showing a high signal intensity contrast between functional and metastatic LNs on T1 weighted sequence 15–120 min after injection, which is much faster than ferumoxtran-10 [57]. The superior contrast not only promises a significantly higher accuracy (sensitivity of 100 % and specificity of 89.5 %) for metastatic node depiction, but also enables the detective ability on metastatic LNs with small metastases (long-axis diameter of 3 mm or less) located at the subcapsular portion of LNs [59]. However, with the drawbacks of reader dependency and relative high false-negative rate of 43 % in small LNs without necrosis, it is as of yet far from becoming a routine in clinical practice [58•].
A 66-year-old man with a history of prostate cancer. a Coronal T1 weighted image showed a 12 mm short axis right perirectal lymph node (arrow) with a well-defined border and low signal intensity. b On coronal T2 weighted image, multiple small bilateral inguinal lymph nodes under size criterion were noted. c On axial Ferumoxytol enhanced T2* weighted image, the small inguinal lymph nodes (arrow) showed low signal intensity, suggesting benign nature of these nodes. d On axial Ferumoxytol enhanced T2* weighted image, the right perirectal lymph node showed the high signal intensity suggesting metastasis, which was also confirmed by biopsy
Positron Emission Tomography
Positron Emission Tomography (PET) is a powerful functional imaging technique for tumor evaluation based on metabolic markers labeled with the positron-emitting radionuclides such as fluorine-18, carbon-11, and oxygen-15. With these agents, PET discriminates the differences in metabolism between benign and malignant cells [62] (Fig. 8). The radiopharmaceutical most commonly used with PET for oncologic imaging is fluorine 18 fluorodeoxyglucose (18F-FDG), which allows the detection of abnormal high glucose uptake of tumors [3••]. Most studies demonstrated that 18F-FDG PET improved the accuracy for identifying LN involvement compared to other structural imaging examinations. Gould et al. compared the diagnostic accuracy of CT and 18F-FDG PET for mediastinal staging in patients with non–small-cell lung cancer by meta-analysis, and found that both median sensitivity and specificity of CT were lower than FDG-PET (61 and 79 %, 85 and 90 %, respectively). Meanwhile, 18F-FDG PET was more sensitive but less specific when CT showed enlarged LNs (median sensitivity and specificity: 100 vs. 82 % and 78 vs. 93 %, respectively) [63]. Part of the reason for the lower sensitivity of PET in detecting normal size LNs may lie in its inaccurate anatomical localization, which can be complemented by fusing PET images with other high spatial resolution anatomical images from CT and MRI. In detection of cervical metastatic LNs in head and neck tumors by 18F-FDG PET/CT, the sensitivity, specificity, accuracy reached 100, 98.2, and 95 %, respectively [14, 64]. In an intention-to-treat analysis of non-small cell lung cancer, Fischer et al. obtained a significantly improved sensitivity (from 59 to 75 %) and similar high specificity (from 98 to 100 %) of mediastinal staging after adding prior PET/CT to invasive diagnostic procedures [65••]. PET/CT or/and PET/MRI studies in pelvic malignancies, for example penile cancer and cervical cancer, also showed a considerably high sensitivity of 80–80.6 % and a specificity of 92.4–100 % for diagnosing inguinal LN involvement [66•, 67]. However, not all researchers obtained such optimistic results in LN assessment by fusing PET technique [68, 69•]. Heusch et al. reported relatively low sensitivity for the detection of cervical LN metastases of head and neck squamous cell carcinoma (HNSCC) in a series of fusing PET images including 18F-FDG-PET/CT (30 %), 18F-FDG-PET-MRI (52 %) and 18F-FDG-PET-MRI plus DWI (53 %). This might be due to the fact that a stringent histological reference standard with detection of a higher frequency of micrometastases was used in this study [69•]. The FDG uptake in nodes tends to vary. Low uptake of FDG in some tumors and metastatic nodes may result in false negative cases (Fig. 9). In patients with prostate cancer, slow-growing tumor results in a low, undifferentiating, uptake of FDG [70], and a large amount of excretion from 18F-FDG PET via the urinary tract and bowel may limit its accurate evaluation of pelvic nodes [3••]. Replacing 18F-FDG with 11C-Choline validly covers this drawback. In a meta-analysis of prostate cancer, Evangelista et al. [71] reported a pooled sensitivity of 100 % and a pooled specificity of 81.8 % for LN metastases. The false positive cases due to uptake of benign inflammatory LNs, necrosis and small node volume decrease the diagnostic accuracy of PET. Onal et al. [72] obtained a false-positive rate of 75 % in evaluating isolated mediastinal LNs for patients with cervical cancer by FDG-PET/CT alone caused by intranodal granulomatous changes. Besides, partial volume effects may induce PET/CT or PET/MRI with an unreliable explanation in nodes <0.8 cm [73]. Lastly, the expensive cost and limited coverage of fusing PET examination also decreases its utilization rate in LN assessment.
A 57-year-old woman with a history of B cell lymphoma. a On axial enhanced neck CT scan, a mass (arrow) of 4.2 × 3.1 cm with a ill-defined border and heterogeneous enhancement was noted in the upper left internal jugular region. A 1-cm left parapharyngeal lymph node (arrow head) was seen medial to the left internal carotid artery. b On PET scan, both mass and node showed increasing FDG uptake
A 56-year-old woman with a history of colon cancer and retroperitoneal node metastasis. a The axial T1 weighted image uncovered a 2.2 × 1.8 cm lymph node with slight low signal intensity adjacent to the celiac axis. b On fat-suppression T2 weighted image, the node showed a slightly increased signal intensity. c Enhanced MRI scan demonstrated a marked contrast enhancement of the node. d On the non-enhanced CT image after 4 months, the node showed a slightly enlargement and ill-defined border. e On PET scan, this metastatic node didn’t show a high level FDG uptake
Conclusion
An accurate imaging assessment of LN status has high directive value in making therapy plans for patients with tumors. Structural imaging methods, including US, CT and conventional MRI, show the strong abilities to depict the location, size, shape, and texture of LNs, but do not reliably distinguish benign LNs from malignant ones. Conversely, functional imaging methods, including DWI, lymphotropic contrasts and PET, demonstrate relatively high sensitivities and specificities in differential diagnosis of LNs, while all evaluation abilities are limited by relatively low spatial resolution or time-consuming processes. The emerging fusing imaging techniques, such as DWI-T2WI, USPIO-DW-MRI, and PET/CT or MRI, bypass these shortcomings. As the clinical paradigm shifts from structural to functional imaging, these techniques will be of prime importance in detecting and characterizing the LNs in cancer patients.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance, •• Of major importance
Mack MG, Rieger J, Baghi M, Bisdas S, Vogl TJ. Cervical lymph nodes. Eur J Radiol. 2008;66:493–500.
Bille A, Pelosi E, Skanjeti A, Arena V, Errico L, Borasio P, et al. Preoperative intrathoracic lymph node staging in patients with non-small-cell lung cancer: accuracy of integrated positron emission tomography and computed tomography. Eur J Cardiothorac Surg. 2009;36:440–5.
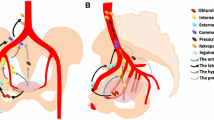
•• Pano B, Sebastia C, Bunesch L, Mestres J, Salvador R, Macias NG, et al. Pathways of lymphatic spread in male urogenital pelvic malignancies. Radiographics. 2011;31:135–160. This article had a good summary of the pathways of nodal metastasis and current imaging techniques for staging of nodal metastases in pelvic tumors.
• Hedgire SS, Pargaonkar VK, Elmi A, Harisinghani AM, Harisinghani MG. Pelvic nodal imaging. Radiol Clin North Am. 2012;50:1111–1125. This is a comprehensive review of nodal drainage pathways and imaging modalities in genitourinary cancers.
Vassallo P, Wernecke K, Roos N, Peters PE. Differentiation of benign from malignant superficial lymphadenopathy: the role of high-resolution US. Radiology. 1992;183:215–20.
Imani MM, Davachi B, Mostaan LV, Langaroodi AJ, Memar B, Azimi SA, et al. Evaluation of the sonographic features of metastatic cervical lymph nodes in patients with head and neck malignancy. J Craniofac Surg. 2011;22:2179–84.
Uematsu T, Sano M, Homma K. In vitro high-resolution helical CT of small axillary lymph nodes in patients with breast cancer: correlation of CT and histology. AJR Am J Roentgenol. 2001;176:1069–74.
Song SE, Seo BK, Lee SH, Yie A, Lee KY, Cho KR, et al. Classification of metastatic versus non-metastatic axillary nodes in breast cancer patients: value of cortex-hilum area ratio with ultrasound. J Breast Cancer. 2012;15:65–70.
Ying M, Ahuja A, Brook F, Metreweli C. Vascularity and grey-scale sonographic features of normal cervical lymph nodes: variations with nodal size. Clin Radiol. 2001;56:416–9.
Shi C, Li S, Shi T, Liu B, Ding C, Qin H. Correlation between thyroid nodule calcification morphology on ultrasound and thyroid carcinoma. J Int Med Res. 2012;40:350–7.
Shin LK, Olcott EW, Jeffrey RB, Desser TS. Sonographic evaluation of cervical lymph nodes in papillary thyroid cancer. Ultrasound Q. 2013;29:25–32.
Kim DW, Choo HJ, Lee YJ, Jung SJ, Eom JW, Ha TK. Sonographic features of cervical lymph nodes after thyroidectomy for papillary thyroid carcinoma. J Ultrasound Med. 2013;32:1173–80.
Yoon DY, Hwang HS, Chang SK, Rho YS, Ahn HY, Kim JH, et al. CT, MR, US,18F-FDG PET/CT, and their combined use for the assessment of cervical lymph node metastases in squamous cell carcinoma of the head and neck. Eur Radiol. 2009;19:634–42.
Dangore-Khasbage S, Degwekar SS, Bhowate RR, Banode PJ, Bhake A, Choudhary MS, et al. Utility of color Doppler ultrasound in evaluating the status of cervical lymph nodes in oral cancer. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;108:255–63.
King AD, Tse GM, Ahuja AT, Yuen EH, Vlantis AC, To EW, et al. Necrosis in metastatic neck nodes: diagnostic accuracy of CT, MR imaging, and US. Radiology. 2004;230:720–6.
Gress FG, Savides TJ, Sandler A, Kesler K, Conces D, Cummings O, et al. Endoscopic ultrasonography, fine-needle aspiration biopsy guided by endoscopic ultrasonography, and computed tomography in the preoperative staging of non-small-cell lung cancer: a comparison study. Ann Int Med. 1997;127:604–12.
van den Brekel MW, Stel HV, Castelijns JA, Nauta JJ, van der Waal I, Valk J, et al. Cervical lymph node metastasis: assessment of radiologic criteria. Radiology. 1990;177:379–84.
Kramer H, Groen HJ. Current concepts in the mediastinal lymph node staging of nonsmall cell lung cancer. Ann Surg. 2003;238:180–8.
Jager GJ, Barentsz JO, Oosterhof GO, Witjes JA, Ruijs SJ. Pelvic adenopathy in prostatic and urinary bladder carcinoma: MR imaging with a three-dimensional TI-weighted magnetization-prepared-rapid gradient-echo sequence. AJR Am J Roentgenol. 1996;167:1503–7.
Monig SP, Zirbes TK, Schroder W, Baldus SE, Lindemann DG, Dienes HP, et al. Staging of gastric cancer: correlation of lymph node size and metastatic infiltration. AJR Am J Roentgenol. 1999;173:365–7.
Fukuya T, Honda H, Hayashi T, Kaneko K, Tateshi Y, Ro T, et al. Lymph-node metastases: efficacy for detection with helical CT in patients with gastric cancer. Radiology. 1995;197:705–11.
Tiguert R, Gheiler EL, Tefilli MV, Oskanian P, Banerjee M, Grignon DJ, et al. Lymph node size does not correlate with the presence of prostate cancer metastasis. Urology. 1999;53:367–71.
Yang DM, Kim HC, Jin W, Ryu CW, Kang JH, Park CH, et al. 64 multidetector-row computed tomography for preoperative evaluation of gastric cancer: histological correlation. J Comput Assist Tomogr. 2007;31:98–103.
Puesken M, Buerke B, Gerss J, Frisch B, Beyer F, Weckesser M, et al. Prediction of lymph node manifestations in malignant lymphoma: significant role of volumetric compared with established metric lymph node analysis in multislice computed tomography. J Comput Assist Tomogr. 2010;34:564–9.
March DE, Wechsler RJ, Kurtz AB, Rosenberg AL, Needleman L. CT-pathologic correlation of axillary lymph nodes in breast carcinoma. J Comput Assist Tomogr. 1991;15:440–4.
Suga K, Ogasawara N, Yuan Y, Okada M, Matsunaga N, Tangoku A. Visualization of breast lymphatic pathways with an indirect computed tomography lymphography using a nonionic monometric contrast medium iopamidol: preliminary results. Invest Radiol. 2003;38:73–84.
Sugi K, Kitada K, Yoshino M, Hirazawa K, Matsuda E, Azuma T, et al. New method of visualizing lymphatics in lung cancer patients by multidetector computed tomography. J Comput Assist Tomogr. 2005;29:210–4.
• Lee YJ, Chung YE, Lim JS, Kim JH, Kim YJ, Lee HJ, et al. Cumulative radiation exposure during follow-up after curative surgery for gastric cancer. Korean J Radiol. 2012;13:144–151. This article reminded us that we should pay more attention to the radiation risk from CT scans.
Pearce MS, Salotti JA, Little MP, McHugh K, Lee C, Kim KP, et al. Radiation exposure from CT scans in childhood and subsequent risk of leukaemia and brain tumours: a retrospective cohort study. Lancet. 2012;380:499–505.
How to improve the ability to detect pelvic lymph node metastases of urologic malignancies USPIO-DWI IS BETTER.
Hovels AM, Heesakkers RA, Adang EM, Jager GJ, Strum S, Hoogeveen YL, et al. The diagnostic accuracy of CT and MRI in the staging of pelvic lymph nodes in patients with prostate cancer: a meta-analysis. Clin Radiol. 2008;63:387–95.
• Wu LM, Xu JR, Liu MJ, Zhang XF, Hua J, Zheng J, et al. Value of magnetic resonance imaging for nodal staging in patients with head and neck squamous cell carcinoma: a meta-analysis. Acad Radiol. 2012;19:331–340. This article analyzed and confirmed a good diagnostic performance of MRI in the overall pretreatment evaluation of node staging with HNSCC.
Wu LM, Xu JR, Liu MJ, Zhang XF, Hua J, Zheng J, et al. Value of magnetic resonance imaging for nodal staging in patients with head and neck squamous cell carcinoma: a meta-analysis. Acad Radiol. 2012;19:331–40.
Kim SH, Kim SC, Choi BI, Han MC. Uterine cervical carcinoma: evaluation of pelvic lymph node metastasis with MR imaging. Radiology. 1994;190:807–11.
Saokar A, Islam T, Jantsch M, Saksena MA, Hahn PF, Harisinghani MG. Detection of lymph nodes in pelvic malignancies with Computed Tomography and Magnetic Resonance Imaging. Clin Imaging. 2010;34:361–6.
Yang WT, Lam WW, Yu MY, Cheung TH, Metreweli C. Comparison of dynamic helical CT and dynamic MR imaging in the evaluation of pelvic lymph nodes in cervical carcinoma. AJR Am J Roentgenol. 2000;175:759–66.
Yang RK, Roth CG, Ward RJ, DeJesus JO, Mitchell DG. Optimizing abdominal MR imaging: approaches to common problems. Radiographics. 2010;30:185–99.
• Darge K, Anupindi SA, Jaramillo D. MR imaging of the abdomen and pelvis in infants, children, and adolescents. Radiology. 2011;261:12–29. This article reviewed recent developments of MRI in the investigation of abdominal and pelvic disease in pediatrics.
Tamhane AA, Arfanakis K, Anastasio M, Guo X, Vannier M, Gao JH. Rapid PROPELLER-MRI: a combination of iterative reconstruction and under-sampling. J Magn Reson Imaging. 2012;36:1241–7.
Kim KW, Lee JM, Jeon YS, Kang SE, Baek JH, Han JK, et al. Free-breathing dynamic contrast-enhanced MRI of the abdomen and chest using a radial gradient echo sequence with K-space weighted image contrast (KWIC). Eur Radiol. 2013;23:1352–60.
Holzapfel K, Duetsch S, Fauser C, Eiber M, Rummeny EJ, Gaa J. Value of diffusion-weighted MR imaging in the differentiation between benign and malignant cervical lymph nodes. Eur J Radiol. 2009;72:381–7.
Kim JK, Kim KA, Park BW, Kim N, Cho KS. Feasibility of diffusion-weighted imaging in the differentiation of metastatic from nonmetastatic lymph nodes: early experience. J Magn Reson Imaging. 2008;28:714–9.
Roy C, Bierry G, Matau A, Bazille G, Pasquali R. Value of diffusion-weighted imaging to detect small malignant pelvic lymph nodes at 3 T. Eur Radiol. 2010;20:1803–11.
Whittaker CS, Coady A, Culver L, Rustin G, Padwick M, Padhani AR. Diffusion-weighted MR imaging of female pelvic tumors: a pictorial review. Radiographics. 2009;29(759–74):774–8.
Sumi M, van Cauteren M, Nakamura T. MR microimaging of benign and malignant nodes in the neck. AJR Am J Roentgenol. 2006;186:749–57.
Mir N, Sohaib SA, Collins D, Koh DM. Fusion of high b-value diffusion-weighted and T2-weighted MR images improves identification of lymph nodes in the pelvis. J Med Imaging Radiat Oncol. 2010;54:358–64.
Sumi M, Van Cauteren M, Nakamura T. MR micro imaging of benign and malignant nodes in the neck. AJR Am J Roentgenol. 2006;186(3):749–57.
Abdel RA, Soliman NY, Elkhamary S, Alsharaway MK, Tawfik A. Role of diffusion-weighted MR imaging in cervical lymphadenopathy. Eur Radiol. 2006;16:1468–77.
• Ginat DT, Mangla R, Yeaney G, Johnson M, Ekholm S. Diffusion-weighted imaging for differentiating benign from malignant skull lesions and correlation with cell density. AJR Am J Roentgenol. 2012;198:W597–W601. This study demonstrated ADC values correlate with cell density and help us to refine interpretation of DWI in differential diagnosis of benign and malignant lesions.
• Lee MC, Tsai HY, Chuang KS, Liu CK, Chen MK. Prediction of nodal metastasis in head and neck cancer using a 3T MRI ADC map. AJNR Am J Neuroradiol. 2013;34:864–869. This study assessed the ability of ADC values at 3T to distinguish malignant from benign cervical lymph nodes.
Eiber M, Beer AJ, Holzapfel K, Tauber R, Ganter C, Weirich G, et al. Preliminary results for characterization of pelvic lymph nodes in patients with prostate cancer by diffusion-weighted MR-imaging. Invest Radiol. 2010;45:15–23.
Kwee TC, Takahara T, Ochiai R, Nievelstein RA, Luijten PR. Diffusion-weighted whole-body imaging with background body signal suppression (DWIBS): features and potential applications in oncology. Eur Radiol. 2008;18:1937–52.
Anzai Y, McLachlan S, Morris M, Saxton R, Lufkin RB. Dextran-coated superparamagnetic iron oxide, an MR contrast agent for assessing lymph nodes in the head and neck. AJNR Am J Neuroradiol. 1994;15:87–94.
Harisinghani MG, Barentsz J, Hahn PF, Deserno WM, Tabatabaei S, van de Kaa CH, et al. Noninvasive detection of clinically occult lymph-node metastases in prostate cancer. N Engl J Med. 2003;348:2491–9.
Thoeny HC, Triantafyllou M, Birkhaeuser FD, Froehlich JM, Tshering DW, Binser T, et al. Combined ultrasmall superparamagnetic particles of iron oxide-enhanced and diffusion-weighted magnetic resonance imaging reliably detect pelvic lymph node metastases in normal-sized nodes of bladder and prostate cancer patients. Eur Urol. 2009;55:761–9.
Misselwitz B, Platzek J, Weinmann HJ. Early MR lymphography with gadofluorine M in rabbits. Radiology. 2004;231:682–8.
• Lee JY, Choi BI, Son KR, Lee JM, Kim SJ, Park HS, et al. Lymph node metastases from gastric cancer: gadofluorine M and gadopentetate dimeglumine MR imaging in a rabbit model. Radiology. 2012;263:391–400. This is pioneering animal research in evaluating the accuracy of Gadofluorine M in the diagnosis of deep metastatic nodes.
Choi SH, Han MH, Moon WK, Son KR, Won JK, Kim JH, et al. Cervical lymph node metastases: MR imaging of gadofluorine M and monocrystalline iron oxide nanoparticle-47 in a rabbit model of head and neck cancer. Radiology. 2006;241:753–62.
Guimaraes R, Clement O, Bittoun J, Carnot F, Frija G. MR lymphography with superparamagnetic iron nanoparticles in rats: pathologic basis for contrast enhancement. AJR Am J Roentgenol. 1994;162:201–7.
Harisinghani MG, Saini S, Hahn PF, Weissleder R, Mueller PR. MR imaging of lymph nodes in patients with primary abdominal and pelvic malignancies using ultrasmall superparamagnetic iron oxide (Combidex). Acad Radiol. 1998;5(1):S167–83.
Patz EJ, Goodman PC. Positron emission tomography imaging of the thorax. Radiol Clin North Am. 1994;32:811–23.
Gould MK, Kuschner WG, Rydzak CE, Maclean CC, Demas AN, Shigemitsu H, et al. Test performance of positron emission tomography and computed tomography for mediastinal staging in patients with non-small-cell lung cancer: a meta-analysis. Ann Int Med. 2003;139:879–92.
Kunawudhi A, Pak-art R, Keelawat S, Tepmongkol S. Detection of subcentimeter metastatic cervical lymph node by 18F-FDG PET/CT in patients with well-differentiated thyroid carcinoma and high serum thyroglobulin but negative 131I whole-body scan. Clin Nucl Med. 2012;37:561–7.
•• Fischer BM, Mortensen J, Hansen H, Vilmann P, Larsen SS, Loft A, et al. Multimodality approach to mediastinal staging in non-small cell lung cancer. Faults and benefits of PET-CT: a randomised trial. Thorax. 2011;66:294–300. This article suggested answers to and discussed several unresolved problems and controversies on PET-CT for mediastinal staging in non-small cell lung cancer.
• Sadeghi R, Gholami H, Zakavi SR, Kakhki VR, Horenblas S. Accuracy of 18F-FDG PET/CT for diagnosing inguinal lymph node involvement in penile squamous cell carcinoma: systematic review and meta-analysis of the literature. Clin Nucl Med. 2012;37:436–441. This analysis demonstrated a low sensitivity of 18 F-FDG PET/CT in cN0 penile cancer patients for detection of inguinal lymph node.
Mueller-Lisse UG, Scher B, Scherr MK, Seitz M. Functional imaging in penile cancer: PET/computed tomography, MRI, and sentinel lymph node biopsy. Curr Opin Urol. 2008;18:105–10.
Jeong HS, Baek CH, Son YI, Choi JY, Kim HJ, Ko YH, et al. Integrated 18F-FDG PET/CT for the initial evaluation of cervical node level of patients with papillary thyroid carcinoma: comparison with ultrasound and contrast-enhanced CT. Clin Endocrinol (Oxf). 2006;65:402–7.
• Heusch P, Sproll C, Buchbender C, Rieser E, Terjung J, Antke C, et al. Diagnostic accuracy of ultrasound, F-FDG-PET/CT, and fused F-FDG-PET-MR images with DWI for the detection of cervical lymph node metastases of HNSCC. Clin Oral Investig. 2013. This study discussed the diagnostic value of multiple PET fused imagings.
Effert PJ, Bares R, Handt S, Wolff JM, Bull U, Jakse G. Metabolic imaging of untreated prostate cancer by positron emission tomography with 18fluorine-labeled deoxyglucose. J Urol. 1996;155:994–8.
Evangelista L, Zattoni F, Guttilla A, Saladini G, Zattoni F, Colletti PM, et al. Choline PET or PET/CT and biochemical relapse of prostate cancer: a systematic review and meta-analysis. Clin Nucl Med. 2013;38:305–14.
Onal C, Oymak E, Findikcioglu A, Reyhan M. Isolated mediastinal lymph node false positivity of [18F]-fluorodeoxyglucose-positron emission tomography/computed tomography in patients with cervical cancer. Int J Gynecol Cancer. 2013;23:337–42.
Lin E, Alavi A. PET and PET/CT, a clinical guide. New York: Thieme; 2009.
Acknowledgments
The authors would like to acknowledge Aiza Zia and Rachel Borczuk for their contribution to the manuscript.
Compliance with Ethics Guidelines
Conflict of Interest
Yun Mao, Sandeep Hedgire and Mukesh Harisinghani declare that they have no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Essentials in Oncologic Imaging.
Rights and permissions
About this article
Cite this article
Mao, Y., Hedgire, S. & Harisinghani, M. Radiologic Assessment of Lymph Nodes in Oncologic Patients. Curr Radiol Rep 2, 36 (2014). https://doi.org/10.1007/s40134-013-0036-6
Published:
DOI: https://doi.org/10.1007/s40134-013-0036-6