Abstract
Background and aims
Most elderly persons live in developing countries where current geriatric epidemiological data are scarce. We aimed to study major comorbidities, polypharmacy, functional and nutritional status in a Turkish community-dwelling female elderly clinic population.
Methods
Female geriatrics outpatient clinic patients were assessed cross-sectionally. Patients underwent comprehensive geriatric cassessment, including identification of chronic diseases, drugs, functionality, and nutrition. Comorbidities and drugs were defined by the review of patients’ self-reports and current medications. Geriatric depression and cognition were assessed by 30-item geriatric depression scale and Folstein mini-mental-state-examination. Functional status was assessed by the evaluation of activities of daily living (ADL) and instrumental activities of daily living (IADL) scales. Nutritional assessment was performed by mini-nutritional-assessment-short form.
Results
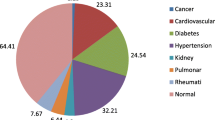
Five-hundred and fifteen patients were included in this study over an 8-year period. Mean age was 73.4 ± 6.9 years. Mean number of chronic diseases was 2.8. 61.1 % had >3 chronic diseases. Most common 3 diagnoses were hypertension (75.3 %), depression (45.5 %) and dementia (39.4 %). Mean number of drugs was 4.8. Polypharmacy was noted as 63.2 and 47.6 % by definitions as >4 or >5 chronic drug use, respectively. Subjects with at least one dependency of ADL and IADL were 23.4 and 64.0 %. Prevalence of poor nutrition was 39.1 %. In patients with at least one ADL or IADL dependency, undernutrition (p < 0.001), dementia (p < 0.001), cerebrovascular accident, Parkinson’s disease, diabetes were more prevalent (p < 0.05) and were taking higher number of drugs (p < 0.01).
Conclusions
Polypharmacy and functional dependency seem to be prevalent among female elders in our country. Nutritional status was worse than the other reported urban area of Turkey and also than among males of same region but better than among Iranian counterparts. This study illustrates geographical differences in and between the individual countries and supports the continued need for comprehensive geriatric assessment worldwide.
Similar content being viewed by others
References
Guralnik JM, Ferrucci L (2009) Demography and Epidemiology. In: Halter JB, Ouslander JG, Tinetti ME, Studenski S, High KP, Asthana S (eds). Hazzards Geriatric Medicine and Gerontology, 6th edn. McGraw Hill, New York, p 45
Lesage J (1991) Polypharmacy in the geriatric patient. Nurs Clin North Am 26:273–290
Nubé M, Van Den Boom GJ (2003) Gender and adult undernutrition in developing countries. Ann Hum Biol 30:520–537
Bernabei R, Gray L, Hirdes J, et al (2009) International Gerontology. In: Halter JB, Ouslander JG, Tinetti ME, Studenski S, High KP, Asthana S (eds). Hazzards Geriatric Medicine and Gerontology, 6th edn. McGraw Hill, New York. p 69–96
Yesavage JA, Brink TL, Rose TL, et al (1982–1983) Development and validation of a geriatric depression screening scale: a preliminary report.J Psychiatr Res 17:37–49
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
Lawton MP, Brody EM (1969) Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist 9:179–186
Rubenstein LZ, Harker JO, Salva A, Guigoz Y, Vellas B (2001) Screening for undernutrition in geriatric practice: developing the short-form Mini-Nutritional Assessment (MNA-SF). J Gerontol A Biol Sci Med Sci 56:M366–M372
Cuervo M, García A, Ansorena D et al (2009) Nutritional assessment interpretation on 22,007 Spanish community-dwelling elders through the Mini Nutritional Assessment test. Public Health Nutr 12:82–90
Rochon PA (2011) Drug prescribing for older adults. Section Editor: Schmader KE, Deputy Editor: Sokol HN. UpToDate. Last updated June 2011
Ferner RE, Aronson JK (2006) Communicating information about drug safety. BMJ 333:143–145
Medicines and older people: implementing medicines-related aspects of the NSF for older people. http://www.gov.uk/nsf/olderpeople/htm
Blyth FM, Rochat S, Cumming RG et al (2008) Pain, frailty and comorbidity on older men: the CHAMP study. Pain 140:224–230
Prescriptions dispensed in community statistics for 1989–1999: England. Statistical Bulletin. (2007). Available from: http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@en/documents/digitalasset/dh_4021990.pdf
Arias-Merino ED, Mendoza-Ruvalcaba NM, Ortiz GG, Velázquez-Brizuela IE, Meda-Lara RM, Cueva-Contreras J (2012) Physical function and associated factors in community-dwelling elderly people in Jalisco, Mexico. Arch GerontolGeriatr 54:e271–e278
Johnson JK, Lui LY, Yaffe KJ (2007) Executive function, more than global cognition, predicts functional decline and mortality in elderly women. Gerontol A BiolSci Med Sci 62:1134–1141
Guigoz Y (2006) The Mini Nutritional Assessment (MNA) review of the literature—what does it tell us? J Nutr Health Aging 10:466–485
Aliabadi M, Kimiagar M, Ghayour-Mobarhan M et al (2008) Prevalence of malnutrition in free living elderly people in Iran: a cross-sectional study. Asia Pac J Clin Nutr 17:285–289
Ülger Z, Halil M, Kalan I et al (2010) Comprehensive assessment of malnutrition risk and related factors in a large group of community-dwelling older adults. Clin Nutr 29:507–511
Conflict of interest
The authors report no conflict of interest. The authors alone are responsible for the content and writing of the article. None of the authors of this manuscript have any financial or personal relationships with other people or organizations that could inappropriately influence (bias) their work. None of the co-authors have direct or indirect conflicts of interest, financial or otherwise, relating to the subject of our report. There is role of no sponsorship.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bahat, G., Tufan, F., Bahat, Z. et al. Comorbidities, polypharmacy, functionality and nutritional status in Turkish community-dwelling female elderly. Aging Clin Exp Res 26, 255–259 (2014). https://doi.org/10.1007/s40520-014-0229-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-014-0229-8