Abstract
Objective
Acromegaly is associated with increased cardiovascular morbidity and mortality. The data about the evaluation of coagulation and fibrinolysis in acromegalic patients are very limited and to our knowledge, platelet function analysis has never been investigated. So, we aimed to investigate the levels of protein C, protein S, fibrinogen, antithrombin 3 and platelet function analysis in patients with acromegaly.
Methods
Thirty-nine patients with active acromegaly and 35 healthy subjects were included in the study. Plasma glucose and lipid profile, fibrinogen levels, GH and IGF-1 levels and protein C, protein S and antithrombin III activities were measured in all study subjects. Also, platelet function analysis was evaluated with collagen/ADP and collagen–epinephrine-closure times.
Results
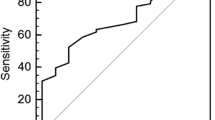
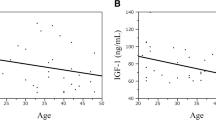
Demographic characteristics of the patient and the control were similar. As expected, fasting blood glucose levels and serum GH and IGF-1 levels were significantly higher in the patient group compared with the control group (pglc: 0.002, pGH: 0.006, pIGF-1: 0.001, respectively). But lipid parameters were similar between the two groups. While serum fibrinogen and antithrombin III levels were found to be significantly higher in acromegaly group (p fibrinogen: 0.005 and pantithrombin III: 0.001), protein S and protein C activity values were significantly lower in the patient group (p protein S: 0.001, p protein C: 0.001). Also significantly enhanced platelet function (measured by collagen/ADP- and collagen/epinephrine-closure times) was demonstrated in acromegaly (p col-ADP: 0.002, p col-epinephrine: 0.002). The results did not change, when we excluded six patients with type 2 diabetes in the acromegaly group. There was a negative correlation between serum GH levels and protein S (r: –0.25, p: 0.04)) and protein C (r: –0.26, p: 0.04) values. Likewise, there was a negative correlation between IGF-1 levels and protein C values (r: –0.39, p: 0.002), protein S values (r: –0.39, p: 0.001), collagen/ADP-closure times (r: –0.28, p: 0.02) and collagen/epinephrine-closure times (r:-0.26, p: 0.04). Also, we observed a positive correlation between IGF-1 levels and fibrinogen levels (r: 0.31, p: 0.01).
Conclusion
Acromegaly was found to be associated with increased tendency to coagulation and enhanced platelet activity. This hypercoagulable state might increase the risk for cardiovascular and cerebrovascular events in acromegaly.
Similar content being viewed by others
References
Vilar L, Naves LA, Costa SS, Abdalla LF, Coelho CE, Casulari LA (2007) Increase of classic and nonclassic cardiovascular risk factors in patients with acromegaly. Endocr Pract 13(4):363–372
Rajasoorya C, Holdaway IM, Wrightson P, Scott DJ, Ibbertson HK (1994) Determinants of clinical outcome and survival in acromegaly. Clin Endocrinol (Oxf) 41(1):95–102
Jurcut R, Găloiu S, Florian A, Vlădaia A, Ioniţă OR, Amzulescu MS, et al (2014) Quantifying subtle changes in cardiovascular mechanics in acromegaly: a Doppler myocardial imaging study. J Endocrinol Invest 37:1081–1090
Wildbrett J, Hanefeld M, Fücker K, Pinzer T, Bergmann S, Siegert G, Breidert M (1997) Anomalies of lipoprotein pattern and fibrinolysis in acromegalic patients: relation to growth hormone levels and insulin-like growth factor I. Exp Clin Endocrinol Diabetes 105(6):331–335
Colao A, Marzullo P, Di Somma C, Lombardi G (2001) Growth hormone and the heart. Clin Endocrinol (Oxf). 54(2):137–154
Erem C, Nuhoglu I, Kocak M, Yilmaz M, Sipahi ST, Ucuncu O, Ersoz HO (2008) Blood coagulation and fibrinolysis in patients with acromegaly: increased plasminogen activator inhibitor-1 (PAI-1), decreased tissue factor pathway inhibitor (TFPI), and an inverse correlation between growth hormone and TFPI. Endocrine 33(3):270–276. doi:10.1007/s12020-008-9088-4
Delaroudis SP, Efstathiadou ZA, Koukoulis GN, Kita MD, Farmakiotis D, Dara OG et al (2008) Amelioration of cardiovascular risk factors with partial biochemical control of acromegaly. Clin Endocrinol (Oxf) 69(2):279–284
Landin-Wilhelmsen K, Tengborn L, Wilhelmsen L, Bengtsson BA (1997) Elevated fibrinogen levels decrease following treatment of acromegaly. Clin Endocrinol (Oxf) 46(1):69–74
Sartorio A, Cattaneo M, Bucciarelli P, Bottasso B, Porretti S, Epaminonda P, Faglia G, Arosio M (2000) Alterations of haemostatic and fibrinolytic markers in adult patients with growth hormone deficiency and with acromegaly. Exp Clin Endocrinol Diabetes 108(7):486–492
Harrison P, Mackie I, Mathur A, Robinson MS, Hong Y, Erusalimsky JD, Machin SJ, Martin JF (2005) Platelet hyper-function in acute coronary syndromes. Blood Coagul Fibrinolysis 16(8):557–562
Frossard M, Fuchs I, Leitner JM, Hsieh K, Vlcek M, Losert H, Domanovits H et al (2004) Platelet function predicts myocardial damage in patients with acute myocardial infarction. Circulation 110(11):1392–1397 Epub 2004 Aug 16
Favaloro EJ (2002) Clinical application of the PFA-100. Curr Opin Hematol 9:407–415
Jilma B (2001) Platelet function analyzer (PFA-100): a tool to quantify congenital or acquired dysfunction. J Lab Clin Med 138:152–163
Renda G, Zurro M, Malatesta G, Ruggieri B, De Caterina R (2010) Inconsistency of different methods for assessing ex vivo platelet function: relevance for the detection of aspirin resistance. Haematol 95(12):2095–2101
Katznelson L, Laws ER Jr, Melmed S, Molitch ME, Murad MH, Utz A, Wass JA (2014) Endocrine Society. Acromegaly: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 99(11):3933–3951
Mestron A, Webb SM, Astorga R, Benito P, Catala M, Gaztambide S et al (2004) Epidemiology, clinical characteristics, outcome, morbidity and mortality in acromegaly based on the Spanish Acromegaly Registry (Registro Espanol de Acromegalia, REA). Eur J Endocrinol 151(4):439–446
Arosio M, Reimondo G, Malchiodi E, Berchialla P, Borraccino A, De Marinis L, Italian Study Group of Acromegaly et al (2012) Predictors of morbidity and mortality in acromegaly: an Italian survey. Eur J Endocrinol 167(2):189–198
Colao A, Ferone D, Marzullo P, Lombardi G (2004) Systemic complications of acromegaly: epidemiology, pathogenesis, and management. Endocr Rev 25(1):102–152
Feinbloom D, Bauer KA (2005) Assessment of hemostatic risk factors in predicting arterial thrombotic events. Arterioscler Thromb Vasc Biol 25(10):2043–2053
Vitale G, Pivonello R, Galderisi M, D’Errico A, Spinelli L, Lupoli G, Lombardi G, Colao A (2001) Cardiovascular complications in acromegaly: methods of assessment. Pituit 4(4):251–257
Dahlbäck B, Villoutreix BO (2005) The anticoagulant protein C pathway. FEBS Lett 579(15):3310–3316
Conflict of interest
None.
Ethical approval
All procedures performed in this study was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Colak, A., Yılmaz, H., Temel, Y. et al. Coagulation parameters and platelet function analysis in patients with acromegaly. J Endocrinol Invest 39, 97–101 (2016). https://doi.org/10.1007/s40618-015-0300-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-015-0300-0