Abstract
Since the discovery of T helper type 1 and type 2 effector T cell subsets 20 years ago, inducible regulatory T cells and interleukin 17 (IL-17)-producing T helper cells have been added to the 'portfolio' of helper T cells. It is unclear how many more effector T cell subsets there may be and to what degree their characteristics are fixed or flexible. Here we show that transforming growth factor-β, a cytokine at the center of the differentiation of IL-17-producing T helper cells and inducible regulatory T cells, 'reprograms' T helper type 2 cells to lose their characteristic profile and switch to IL-9 secretion or, in combination with IL-4, drives the differentiation of 'TH-9' cells directly. Thus, transforming growth factor-β constitutes a regulatory 'switch' that in combination with other cytokines can 'reprogram' effector T cell differentiation along different pathways.
Similar content being viewed by others
Main
CD4+ helper T cells differentiate into functionally distinct subsets after encountering antigen. For a considerable length of time, T helper 1 (TH1) and TH2 represented the sole paradigm of this functional diversification1. Subsequently, the identification of the interleukin 17 (IL-17)-producing T helper (TH-17) subset as well as transforming growth factor (TGF-β; A002271)-induced regulatory 7 cells (iTreg cells) has added complexity to the CD4+ effector T cell program. T cell antigen receptor–mediated signals together with cytokine signals have been shown to direct the differentiation of CD4+ T cells and to initiate reciprocal activation and silencing of the genes encoding the cytokines IL-4 and interferon-γ2. This process was thought to be irreversible after a certain number of divisions3,4, thereby fixing the polarization state of a particular T cell subset. Nevertheless, rigid polarization into one particular subset is not usually seen in vivo, and the idea that memory cells might have to be flexible to provide protection against a pathogen re-encountered in a different setting or different route of entry in particular suggests that there might be more functional plasticity in helper T cells than originally thought. Thus, the functional heterogeneity of T cells may incorporate a fair amount of flexibility and is shaped by many components, such as the strength of the initial T cell antigen receptor signal, cytokines, epigenetic factors and interactions with other cell types in the microenvironment encountered in vivo5.
TH2 effector differentiation depends on the presence of the transcription factor STAT6 (A002236) and IL-4 (A001262) and is determined by expression of the GATA-3 transcription factor6. TH2 cells provide helper signals that facilitate the development of antibody responses of the immunoglobulin G1 and E class, are essential in the protective immune response against helminth infection and are causally involved in the development of airway inflammation and asthma. The cytokines attributed to TH2 cells are IL-4, IL-5 and IL-13. Like many T cell subsets, TH2 cells can also produce IL-10 (ref. 7). In addition, IL-9 (ref. 8), which is involved in immune responses to helminths as well as allergy6,7, is generally attributed to TH2 cells, although a study has suggested that regulatory T cells (Treg cells) produce more IL-9 than TH2 cells do8. We have made a comparative gene microarray analysis of highly polarized CD4+ effector cells subsets and unexpectedly found that IL-9 seemed to be associated with the TH-17 subset. Subsequent careful delineation of the conditions in which IL-9 production was promoted showed that IL-9-producing T cells were distinct from TH1, TH2, Treg and TH-17 cells and we therefore have provisionally called them 'TH-9' cells. Furthermore, we found that TGF-β, a cytokine that influences fate 'decisions' in the development of TH-17 and iTreg cells, was crucial in 'reprogramming' committed TH2 cells toward a 'TH-9' phenotype.
Results
IL-9 expression distinct from other CD4 T cell subsets
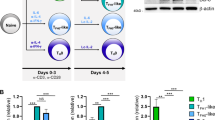
Quantitative PCR analysis of highly polarized effector T cell subsets showed that T cells producing IL-9 emerged 'preferentially' in response to TGF-β1 in the absence of IL-6 but required the presence of IL-4 and did therefore not follow the main pathway for TH-17 differentiation. The expression of IL-9 mRNA and protein was concordant (Fig. 1a) and the expression of IL-9 mRNA was further upregulated in the presence of recombinant IL-9 (Fig. 1a), which indicated an autocrine positive feedback. In contrast, no IL-9 signal was detectable in thymus-derived Treg cells sorted by flow cytometry on the basis of CD25 expression, whether they were tested immediately after isolation or were cultured in IL-2 with or without TGF-β (Fig. 1c). Furthermore, iTreg cells induced in vitro by activation in the presence of TGF-β did not express IL-9 (Fig. 1c), nor did Treg cells from mice expressing green fluorescent protein (GFP) from the locus encoding the transcription factor Foxp3 (Foxp3 reporter mice) sorted on the basis of GFP expression (Fig. 1c).
(a, b) RT-PCR of Il9 mRNA expression (a) and ELISA of IL-9 protein expression (b) by naive CD4+ T cells from B6 mice sorted by flow cytometry, cultured on plates coated with anti-CD3 and anti-CD28 in the presence of various cytokines and collected on day 5 for analysis. (a) Il9 mRNA expression presented relative to Hprt1 expression. (b) IL-9 protein in cell supernatants. ND, not done in wells containing recombinant IL-9. (c) IL-9 mRNA expression by natural Treg cells sorted by flow cytometry on the basis of CD25 expression immediately after isolation or after 48 h of culture in cytokines (CD4+CD25+); by naive CD4+ T cells sorted by flow cytometry and cultured in vitro in iTreg-inducing conditions with TGF-β (iTreg); and by ex vivo Foxp3-expressing (GFP+) Treg cells from Foxp3 reporter mice (Foxp3+). Data are representative of three independent experiments (mean ± s.d.).
Culture of naive T cells in TH1, TH2, iTreg or TH-17 conditions did not lead to IL-9 production, which confirmed the quantitative PCR results reported above (Fig. 2a). Conversely, culture of cells in 'TH-9' conditions (that is, in the presence of TGF-β and IL-4) gave rise to cells producing IL-9. Although a small proportion of cells expressing Foxp3, IL-4 or IL-17 developed in 'TH-9' conditions, none of these markers costained with IL-9 (Fig. 2a), which emphasized that the T cells producing IL-9 were distinct from the other T cell subsets. In agreement with that finding, CD4+ T cells producing IL-9 did not express any of the known transcription factors T-bet, GATA-3, Foxp3 or RORγt that define the other subsets (Fig. 2b). The dependence of IL-9-secreting T cells on TGF-β and IL-4 for their development was further demonstrated by the finding that naive CD4+ T cells isolated from mice with defective TGF-β signaling due to expression of a dominant negative TGF-β receptor II ('CD4dnTGFβRII' mice) and cultured with IL-4 and TGF-β failed to develop into 'TH-9' cells, as did CD4+ T cells isolated from Stat6−/− mice (Fig. 2c). The failure to respond to TGF-β or IL-4 respectively was demonstrated by the finding the CD4+ T cells from CD4dnTGFβRII mice also did not develop into iTreg or TH-17 cells and CD4+ T cells from Stat6−/− mice did not develop into TH2 cells (Fig. 2c and Supplementary Fig. 1a, b online). Although these data may indicate the existence of a 'TH-9' subset, we have not been able to identify a unique transcription factor that might promote the differentiation of such a subset from naive CD4+ precursors, so this idea remains speculative at present.
(a) Intracellular staining of cytokines in naive CD4+ T cells from B6 mice sorted by flow cytometry and cultured for 5 d in TH1, TH2, iTreg or TH-17 conditions (top row) or 'TH-9' conditions (bottom row). (b) RT-PCR of transcription factors in CD4+ subsets of the cells in a, presented relative to Hprt1 expression. (c) Intracellular staining of cytokines in cells from CD4dnTGFβRII mice or Stat6−/− mice cultured in TH2 conditions (left) or 'TH-9' conditions (right). Numbers in quadrants (a, c) indicate percent cells in each. Data are representative of three independent experiments.
TGF-β deviates TH2 cells to a 'TH-9' fate
Instead of the idea presented above, our subsequent experiments showed that T cells committed toward a TH2 pathway were 'reprogrammed' toward a 'TH-9' phenotype by TGF-β1. To confirm the TGF-β1-mediated deviation from the TH2 pathway, we cultured CD4+ T cells from IL-4 reporter mice, engineered to express IL-4 linked by an internal ribosomal entry site with GFP (4get mice)9 in TH2-inducing conditions and sorted cells that had differentiated toward a TH2 program on the basis of their expression of IL-4, as 'reported' by GFP. Intracellular staining for IL-4 confirmed that GFP expression correlated with IL-4 expression. IL-4 protein (Supplementary Fig. 2 online). The polarized population had high expression of GATA-3 (before sorting of GFP+ cells by flow cytometry), and expression of T-bet was not detectable. Furthermore, these cells also expressed IL-5, IL-13 and IL-10 but not IL-9 (Fig. 3a). We also assessed expression of these markers by cells cultured in TH1 or 'TH-9' conditions (Supplementary Fig. 2). Unfortunately, only one antibody to IL-9 labeled with Alexa Fluor 488 or fluorescein isothiocyanate from a collection of ten polyclonal and monoclonal antibodies was able to stain cells intracellularly, so it was not possible to assess IL-9 staining in the GFP+ population (antibody specificity, Supplementary Fig. 3 online). We therefore used quantitative PCR analysis for the following experiments. As shown above (Fig. 1), expression of IL-9 mRNA reliably correlated with expression of IL-9 protein.
(a) RT-PCR analysis (above) of transcription factors and cytokines in the TH2 population of naive CD4+ T cells from 4get mice sorted by flow cytometry and cultured for 5 d in TH2 conditions (other conditions, Supplementary Fig. 2). Below, flow cytometry of cell sorting. Empty, no fluorochrome. Numbers in quadrants indicate percent GFP− cells (left) and GFP+ cells used for subsequent experiments (right; outlined). (b) RT-PCR analysis of transcription factors and cytokines in GFP+ IL-4-expressing cells sorted as described in a and then restimulated for 5 d in TH1, TH2 or 'TH-9' conditions. (c) RT-PCR analysis of transcription factors and cytokines in the TH2 population from a, twice polarized in TH2, restimulated again in TH1, TH2 or 'TH-9' conditions. (d) Quantitative PCR analysis of IL-4, IL-9 and GATA-3 in naive CD4 T cells stimulated for 5 d in TH2 conditions, 'TH-9' conditions or 'TH-9' conditions plus anti-10 receptor (α-IL-10R; 10 μg/ml of monoclonal antibody 3F9; left) or in polarized TH2 cells restimulated for 5 d in those same conditions (right). Expression (a–d) is presented relative to Hprt1. Data are representative of four (a–c) or two (d) independent experiments.
We sorted TH2 cells by flow cytometry from 4get mice, restimulated the cells in TH1 conditions (IL-12), TH2 conditions (IL-4 plus antibody to TGFβ (anti-TGFβ)) or 'TH-9' conditions (TGF-β1) and then analyzed their profiles 5 d later by quantitative PCR. Although the original TH2-committed cells derived from the flow cytometry–sorted GFP+ cells reinforced their TH2 profile in TH2 conditions (Fig. 3b), they did not switch to a typical TH1 profile after culture in TH1 conditions but instead still expressed GATA-3 and IL-4 and almost no T-bet, although small amounts of interferon-γ were detectable (Fig. 3b). This result indicates that plasticity for this pathway was already limited after the first round of TH2 commitment. However, stimulation of the TH2 population in the presence of TGF-β caused a profound loss of expression of TH2 cytokines and transcription factors and instead resulted in expression of IL-9 (Fig. 3b). The only TH2-associated cytokine that continued to be expressed was IL-10, but this cytokine is not specific for TH2 cells, as in certain conditions it is can also be expressed by TH1 or TH-17 cells10. A third round of restimulation of twice-polarized TH2 cells in TH1 or 'TH-9' conditions produced a similar result: no diversion to TH1 profile after culture in TH1 conditions but loss of TH2 markers in favor of expression of IL-9 and IL-10 after culture with TGF-β (Fig. 3c). Thus, TGF-β was able to 'reprogram' TH2 cells that seemed firmly committed, at least in terms of plasticity, to a TH1 profile. IL-10 has been suggested to promote IL-9 production in human11 and mouse12 T cells, but blockade of the IL-10 receptor did not have a negative influence on IL-9 expression in either primary 'TH-9' conditions or in the deviation of TH2 cells to a 'TH-9' profile (Fig. 3d).
Defective response to TGF-β compromises helminth immunity
IL-9 is involved in immunity to intestinal responses to helminths13. Although it is still a matter of debate what mechanism is directly responsible for the expulsion of the worms, a TH2 immune response accompanied by mucosal mast cell accumulation is linked to successful worm expulsion6. To assess whether mice with defective TGF-β signaling have a defect in IL-9-producing T cells, we infected CD4dnTGFβRII mice with Trichuris muris and compared their response to this infection with that of wild-type C57BL/6 (B6) mice. Although wild-type B6 mice were able to mount a protective immune response and successfully expel T. muris, the worm burden in CD4dnTGFβRII mice remained very high (Fig. 4a). B6 mice had many mast cells in the cecum, whereas CD4dnTGFβRII mice had defective recruitment and/or survival of mast cells (Fig. 4b), in line with their low expression of IL-9 (Fig. 4c). TH2 cytokines such as IL-4 and IL-13 were differentially affected, with much less IL-4 expression but similar IL-13 expression in infected CD4dnTGFβRII mice relative to that in B6 mice (Fig. 4c). The lower IL-4 expression in helmith-infected CD4dnTGFβRII mice was unexpected, given that when crossed to 4get mice, these mice showed spontaneous ex vivo overexpression of the IL-4 reporter in CD4+ T cells from peripheral lymph nodes (Fig. 4d). Although this is indicative that additional defects beyond the lack of IL-9 might contribute to the phenotype of these mice, IL-13 rather than IL-4 is reported to be important in trichuris infection, as IL-13 confers resistance to trichuris in IL-4-deficient mice.
Worm burden (a) and mast cells in cecal crypts (b) of wild-type B6 mice (WT) and CD4dnTGFβRII mice (TG) infected for 25 d with trichuris. (c) Expression of IL-9, IL-4 and IL-13 mRNA (relative to Hprt1 mRNA) in mesenteric lymph node cells from wild-type B6 mice and CD4dnTGFβRII mice infected for 25 d with trichuris (n = 5 mice each) and uninfected B6 control mice (Ctrl; n = 5 mice). (d) Expression of GFP ('reporting' IL-4) by peripheral lymph node cells (PLN) or mesenteric lymph node cells (MLN) from B6 IL-4 reporter mice (B6 4get; left) or B6 IL-4 reporter mice crossed with CD4dnTGFβRII mice (right). Numbers in quadrants indicate percent cells in each. Data are representative of three (a, b, d) or two (c) independent experiments (mean ± s.d., a–c).
Discussion
The commitment of T helper cell subsets to a particular lineage and the molecular control mechanisms that support commitment have been studied extensively and serve as examples of gene regulation and epigenetic influences. The demonstrations of helper cell commitment in vitro have shaped the perception of T cell effector fates for a considerable time, but doubts have remained as to whether the 'decisions' are really so rigidly fixed in vivo14; such doubts are supported by the finding that human TH1 and TH2 cells seem to be more flexible15. Subsequently, the observation of reciprocal development of iTreg cells and TH-17 cells in response to cytokine combinations16 has emphasized that fate 'decisions' taken by helper T cells might be more flexible than anticipated5. Here we have shown that a cytokine long assigned to the TH2 effector subset was in fact secreted by a distinct T cell population that either deviated from a previous TH2 fate or directly developed from naive CD4+ precursors as a new subset that, in keeping with the present tradition, might be called 'TH-9'. We have avoided too much emphasis on the claim that we might be dealing with yet another T cell subset because we have so far failed to identify a unique transcription factor that might be driving the lineage differentiation of such 'TH-9' cells. We did note a signal for the vitamin D3 receptor that seemed to be selectively higher in 'TH-9' polarized cells in our microarray analysis, but we could not verify this result by quantitative PCR. Notably, the assignation of 'TH-17' as a new lineage was suggested in two publications despite the fact that neither had identified the lineage transcription factor for these cells but demonstrated the absence of transcription factors known to drive the development of the other effector subsets2,17.
However, regardless of whether there might be an effector T cell subset dedicated to the production of IL-9, our data have shown that TGF-β, a cytokine with a wide range of functions in the immune system18,19,20, could alter TH2 cells to the extent that they lost their previous characteristics, including expression of GATA-3 (refs. 20, 21) and the 'signature' cytokines IL-4, IL-5 and IL-13, and 'switch on' IL-9 instead. Loss of GATA-3 by conditional gene deletion in an established TH2 population has been shown to abolish the production of IL-5 and IL-13 but not IL-4 production22, which makes it unlikely that the effect of TGF-β simply mimics the loss of GATA-3. The only trace of 'TH2-ness' remaining after treatment of TH2 cells with TGF-β was abundant production of IL-10, and this cytokine was also produced by naive CD4+ precursors in 'TH-9-polarizing' conditions. However, IL-10 is not restricted to the TH-2 lineage but is also induced in all other CD4+ T cell subsets10,23,24. GATA-3 is involved in remodeling of the Il10 locus in TH2 and IL-10-producing Treg cells25. Although GATA-3 was below the limit of detection in 'TH-9' cells here, whether differentiated from naive T cells or diverted from TH2 cells, it is not clear whether progression to this effector profile requires GATA-3 expression at some stage in their development. An absence of STAT6 precluded the differentiation of 'TH-9' cells, which is in line with the requirement for IL-4 and emphasizes their relationship with the TH2 program, although TH2 development can also proceed in a STAT6- and IL-4-independent way26,27.
IL-10 has been suggested to promote IL-9 production in human11 and mouse12 T cells, but in our system, blockade of the IL-10 receptor did not have a negative influence on IL-9 expression in either primary 'TH-9' conditions or in deviation of TH2 cells to a 'TH-9' profile. Our observations seem in contradiction with the reported absence of IL-9 after immunization of IL-10-deficient mice with keyhole limpet hemocyanin12 and with its partial inhibition by anti-IL-10 after human T cell activation11. However, the absence of IL-9 in mice lacking IL-10 could be an indirect consequence of the exacerbated TH1 cytokine expression of these mice, and the function of IL-10 in human T cells could be limited to the response of memory cells, as the IL-9 produced in those experiments11 was restricted to CD45 RO+ cells.
The link of IL-9 production to TGF-β has been described before28. That report also indicated an important function for IL-2, which suggests that basal IL-9 production in cells from IL-4-deficient mice can be induced by TGF-β and IL-2 independently of IL-4. Similarly, another report has described an IL-4-independent route for IL-9 production12. Those studies measured IL-9 production by enzyme-linked immunosorbent assay (ELISA), which did not allow it to be linked directly to a particular T cell population. Similarly, another study describing IL-9 production by Treg cells did not directly ascertain this by intracellular staining or rigorous purification of the cells by sorting by flow cytometry8. Here we carefully analyzed Treg cells isolated by sorting by flow cytometry either on the basis of CD25 expression or from Foxp3 reporter mice, relying on GFP expression, and found no IL-9 expression in these cells whether analyzed immediately after isolation or activated in vitro in the presence or absence of IL-2 and/or TGF-β. A very small signal appeared in sorted CD25+ Treg cells cultured with IL-2 and TGF-β in vitro, but as there was no coexpression of Foxp3 and IL-9, this result suggests that in these culture conditions, a few IL-9-producing T cells were generated but were distinct from Treg cells. Intracellular staining also verified that IL-9 expression did not coincide with that of interferon-γ, IL-4, IL-13 and IL-17. The last finding was particularly notable, as we had initially found IL-9 to be differentially expressed in TH-17 conditions by microarray analysis (data not shown). However, our subsequent analysis established that there was only a minor signal for IL-9 in response to IL-6 and TGF-β, the standard conditions for TH-17 differentiation.
The physiological function of IL-9 seems to be in some way connected with a TH2 response, as IL-9 is important in the immune defense against helminth infection but also appears during allergic reactions in the lung, both scenarios that depend on TH2 responses. Our data have shown that defective responsiveness to TGF-β in CD4+ T cells compromises an IL-9-dependent function such as the recruitment and/or survival of mast cells. Although expression of IL-4 was considerably compromised in infected CD4dnTGFβRII mice, these mice do not have an overall defect in TH2 responses but instead have greater responses because of the lack of TGF-β inhibition29. Another TH2 cytokine, IL-13, shown to confer resistance to trichuris in IL-4-deficient mice30, was expressed in amounts similar to those in wild-type mice.
Further investigation of the functions of IL-9 in the immune system would benefit from an IL-9 reporter mouse. At present, the reagents available to detect IL-9 responses, such as antibodies suitable for intracellular staining, are limited and not sensitive enough to monitor the kinetic development of IL-9 production during immune responses in vivo. Such a model system would be essential to ascertain whether there is indeed a direct 'TH-9' pathway from naive CD4+ precursors in response to certain stimuli.
However, regardless of whether a CD4+ T cell subset dedicated to production of IL-9 exists, the IL-9 system provides an example of flexibility in the CD4+ effector cell differentiation program. Although there seems to be little plasticity between TH1 and TH2 differentiation, with relatively early fixation of the program as documented before, TH2 cells allowed 'reprogramming' by TGF-β at least through two rounds of polarization in vitro. It is conceivable that the reverse may be true as well, but without the technical means to highly purify IL-9-producing CD4+ T cells, the possibility that 'TH-9' cells may revert to TH2 cannot be accurately assessed, as polarized 'TH-9' cell populations still include uncommitted cells that would complicate interpretation of the data. Given that irreversible commitment may be even less common during exposure of cells to various environmental stimuli in vivo, it is conceivable that plasticity for different effector profiles is the norm. It is furthermore possible that such plasticity is more prevalent between effector programs that are functionally more closely related, such as TH2 and 'TH-9', to allow 'fine-tuning' of responses in the course of immune responses.
Methods
Mice.
Transgenic CD4dnTGFβRII mice29 and 4get mice9 on a B6 background, as well as wild-type B6 mice, were kept in specific pathogen–free conditions, and all animal experiments were done according to institutional guidelines (National Institute for Medical Research Ethical Review Panel) and UK Home Office regulations. Spleens from Stat6−/− mice on a BALB/c background were provided by C. Watson.
In vitro T cell differentiation and cytokine analysis.
Naive T cells (CD4+CD25−CD44lo) sorted by flow cytometry were cultured in Iscove's modified Dulbecco's medium (Sigma) supplemented with 5% (vol/vol) FCS, L-glutamine (2 μM), penicillin (100 U/ml), streptomycin (100 μg/ml) and mercaptoethanol (50 nM; all from Sigma) in the presence of anti-CD3 (1 μg/ml; 2C11) and anti-CD28 (10 μg/ml; 37.51; both plate bound). Cytokines for effector cell differentiation were as follows (all from Invitrogen): TH1, IL-12 (3 ng/ml); TH2, IL-4 (10 ng/ml) and anti-TGF-β (5 μg/ml; 1D11); iTreg, TGF-β (5 ng/ml) and anti-IL-4 (5 μg/ml; 11B11); TH-17, TGF-β (1 ng/ml), IL-6 (20 ng/ml) and anti-IL-4 (5 μg/ml); and 'TH-9', IL-4 (10 ng/ml) and TGF-β (1 ng/ml). Cells were cultured for 5 d and then restimulated for 4 h with phorbol dibutyrate and ionomycin (both at 500 ng/ml) in the presence of brefeldin A (1 μg/ml) before intracellular staining of cytokines. For intracellular staining of IL-9, goat anti–mouse IL-9 was affinity-purified (0.5 mg) and was labeled with Alexa Fluor 488 (Invitrogen) or fluorescein isothiocyanate according to the manufacturer's instructions. For ELISA of mouse IL-9, the mouse IL-9–specific monoclonal antibody MM9C1 (ref. 12) was used as the capture antibody and goat anti-IL-9 was used for development.
Quantitative analysis of mRNA for cytokines and transcription factors.
RNA was extracted with TRIzol and 1-bromo-3-chloro-propane (Sigma) and was reverse-transcribed with oligo(dT)16 (Applied Biosystems) according to the manufacturer's protocol. The cDNA served as template for amplification of target genes, as well as of the 'housekeeping' gene Hprt1 (encoding hypoxanthine guanine phosphoribosyl transferase), by real-time PCR with TaqMan Gene Expression sssays (Applied Biosystems), universal PCR Master Mix (Applied Biosystems) and the ABI-PRISM 7900 sequence-detection system (Applied Biosystems). Expression of target genes was calculated with by comparative method for relative quantification after normalization to Hprt1 expression.
Infection with T muris.
T. muris was maintained as described31. Mice were infected with 150 embryonated eggs by oral gavage on day 0, and the number of adult worms in the cecum was assessed 30 d later. Cecal tissue was fixed in Carnoy's fluid and was histologically processed by standard methods; sections 5 μm in thickness were stained for mucosal mast cells (0.5% (vol/vol) toluidine blue). Mucosal mast cells per 20 randomly selected cecal crypt units were counted by light microscopy from at least two sections per mouse.
Statistical analysis.
P values were calculated by the two-tailed Student t-test.
Accession codes.
UCSD-Nature Signaling Gateway (http://www.signaling-gateway.org): A002271, A002236 and A001262.
Note: Supplementary information is available on the Nature Immunology website.
References
Mosmann, T.R. et al. Two types of murine helper T cell clone. I. Definition according to profiles of lymphokine activities and secreted proteins. J. Immunol. 136, 2348–2357 (1986).
Ansel, K.M., Lee, D.U. & Rao, A. An epigenetic view of helper T cell differentiation. Nat. Immunol. 4, 616–623 (2003).
Grogan, J.L. et al. Early transcription and silencing of cytokine genes underlie polarization of T helper cell subsets. Immunity 14, 205–215 (2001).
Murphy, E. et al. Reversibility of T helper 1 and 2 populations is lost after long-term stimulation. J. Exp. Med. 183, 901–913 (1996).
O'Shea, J.J., Hunter, C.A. & Germain, R.N. T cell heterogeneity: firmly fixed, predominantly plastic or merely malleable? Nat. Immunol. 9, 450–453 (2008).
Faulkner, H., Renauld, J.C., Van Snick, J. & Grencis, R.K. Interleukin-9 enhances resistance to the intestinal nematode Trichuris muris. Infect. Immun. 66, 3832–3840 (1998).
Soussi-Gounni, A., Kontolemos, M. & Hamid, Q. Role of IL-9 in the pathophysiology of allergic diseases. J. Allergy Clin. Immunol. 107, 575–582 (2001).
Lu, L.F. et al. Mast cells are essential intermediaries in regulatory T-cell tolerance. Nature 442, 997–1002 (2006).
Stetson, D.B. et al. Constitutive cytokine mRNAs mark natural killer (NK) and NK T cells poised for rapid effector function. J. Exp. Med. 198, 1069–1076 (2003).
O'Garra, A. & Vieira, P. TH1 cells control themselves by producing interleukin-10. Nat. Rev. Immunol. 7, 425–428 (2007).
Houssiau, F.A. et al. A cascade of cytokines is responsible for IL-9 expression in human T cells. Involvement of IL-2, IL-4, and IL-10. J. Immunol. 154, 2624–2630 (1995).
Monteyne, P. et al. IL-4-independent regulation of in vivo IL-9 expression. J. Immunol. 159, 2616–2623 (1997).
Khan, W.I. et al. Modulation of intestinal muscle contraction by interleukin-9 (IL-9) or IL-9 neutralization: correlation with worm expulsion in murine nematode infections. Infect. Immun. 71, 2430–2438 (2003).
Krawczyk, C.M., Shen, H. & Pearce, E.J. Functional plasticity in memory T helper cell responses. J. Immunol. 178, 4080–4088 (2007).
Messi, M. et al. Memory and flexibility of cytokine gene expression as separable properties of human TH1 and TH2 lymphocytes. Nat. Immunol. 4, 78–86 (2003).
Bettelli, E. et al. Reciprocal developmental pathways for the generation of pathogenic effector TH17 and regulatory T cells. Nature 441, 235–238 (2006).
Harrington, L.E. et al. Interleukin 17–producing CD4+ effector T cells develop via a lineage distinct from the T helper type 1 and 2 lineages. Nat. Immunol. 6, 1123–1132 (2005).
Letterio, J.J. TGF-β signaling in T cells: roles in lymphoid and epithelial neoplasia. Oncogene 24, 5701–5712 (2005).
Veldhoen, M. & Stockinger, B. TGFβ1, a “Jack of all trades”: the link with pro-inflammatory IL-17-producing T cells. Trends Immunol. 27, 358–361 (2006).
Li, M.O., Sanjabi, S. & Flavell, R.A. Transforming growth factor-β controls development, homeostasis, and tolerance of T cells by regulatory T cell-dependent and -independent mechanisms. Immunity 25, 455–471 (2006).
Gorelik, L., Fields, P.E. & Flavell, R.A. Cutting edge: TGF-β inhibits Th type 2 development through inhibition of GATA-3 expression. J. Immunol. 165, 4773–4777 (2000).
Zhu, J. et al. Conditional deletion of Gata3 shows its essential function in TH1-TH2 responses. Nat. Immunol. 5, 1157–1165 (2004).
McGeachy, M.J. et al. TGF-β and IL-6 drive the production of IL-17 and IL-10 by T cells and restrain TH-17 cell–mediated pathology. Nat. Immunol. 8, 1390–1397 (2007).
Stumhofer, J.S. et al. Interleukins 27 and 6 induce STAT3-mediated T cell production of interleukin 10. Nat. Immunol. 8, 1363–1371 (2007).
Shoemaker, J., Saraiva, M. & O'Garra, A. GATA-3 directly remodels the IL-10 locus independently of IL-4 in CD4+ T cells. J. Immunol. 176, 3470–3479 (2006).
Dent, A.L., Hu-Li, J., Paul, W.E. & Staudt, L.M. T helper type 2 inflammatory disease in the absence of interleukin 4 and transcription factor STAT6. Proc. Natl. Acad. Sci. USA 95, 13823–13828 (1998).
Ouyang, W. et al. Stat6-independent GATA-3 autoactivation directs IL-4-independent Th2 development and commitment. Immunity 12, 27–37 (2000).
Schmitt, E. et al. IL-9 production of naive CD4+ T cells depends on IL-2, is synergistically enhanced by a combination of TGF-β and IL-4, and is inhibited by IFN-γ. J. Immunol. 153, 3989–3996 (1994).
Gorelik, L. & Flavell, R.A. Abrogation of TGFβ signaling in T cells leads to spontaneous T cell differentiation and autoimmune disease. Immunity 12, 171–181 (2000).
Bancroft, A.J. et al. Gastrointestinal nematode expulsion in IL-4 knockout mice is IL-13 dependent. Eur. J. Immunol. 30, 2083–2091 (2000).
Helmby, H., Takeda, K., Akira, S. & Grencis, R.K. Interleukin (IL)-18 promotes the development of chronic gastrointestinal helminth infection by downregulating IL-13. J. Exp. Med. 194, 355–364 (2001).
Acknowledgements
We thank A. Rae and G. Preece for cell sorting; I. Baar for testing the specificity of goat anti-IL-9 by ELISA; and C. Watson (University of Cambridge) for spleens from Stat6−/− mice on a BALB/c background. Supported by the Fonds National de la Recherche Scientifique, Belgium (C.U. and J.v.S.).
Author information
Authors and Affiliations
Contributions
M.V. did and designed the experiments; C.U. and J.v.S. generated and labeled IL-9-specific monoclonal and polyclonal antibodies and did ELISA; H.H. did the trichuris experiments; B.M. contributed to experiments on deviation; A.W. and J.B. did the microarray analyses that were the starting basis of these studies; and B.S. designed experiments and wrote the manuscript.
Corresponding author
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–3 (PDF 820 kb)
Rights and permissions
About this article
Cite this article
Veldhoen, M., Uyttenhove, C., van Snick, J. et al. Transforming growth factor-β 'reprograms' the differentiation of T helper 2 cells and promotes an interleukin 9–producing subset. Nat Immunol 9, 1341–1346 (2008). https://doi.org/10.1038/ni.1659
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.1659
This article is cited by
-
Immune modulation in malignant pleural effusion: from microenvironment to therapeutic implications
Cancer Cell International (2024)
-
Role of LINC00240 on T-helper 9 differentiation in allergic rhinitis through influencing DNMT1-dependent methylation of PU.1
Immunologic Research (2024)
-
Haemonchus contortus HcL6 promoted the Th9 immune response in goat PBMCs by activating the STAT6/PU.1/NF-κB pathway
Veterinary Research (2023)
-
The Dysregulation of Inflammatory Pathways Triggered by Copper Exposure
Biological Trace Element Research (2023)
-
MiR-493-5p inhibits Th9 cell differentiation in allergic asthma by targeting FOXO1
Respiratory Research (2022)