Abstract
Background
Bariatric surgery is a valuable therapeutic option in the treatment of obesity but the outcomes show a large subject-to-subject variability yet to be explained. Thyroid function may represent an involved factor and we have only few controversial data about its influence.
Subjects/methods
We retrospectively assessed using a longitudinal approach the relation between baseline TSH levels and short-term (6 and 12 months) weight loss in 387 euthyroid patients who underwent laparoscopic gastric banding (LAGB; n = 187) or sleeve gastrectomy (SG; n = 200).
Results
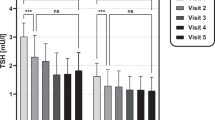
After LAGB, patients with low-normal TSH levels (0.40–1.40 mUI/L) had higher percent total weight loss, ∆BMI and percent excess weight loss when compared to patients with normal (1.41–2.48 mUI/L) and high-normal (2.49–4.00 mUI/L) TSH (p < 0.05). Conversely, no association was detected after SG (p = 0.17). The multivariable regression analysis showed that also baseline BMI (6–12 months) and HOMA2-IR (only at 6 months) were independently associated with the outcomes.
Conclusions
TSH levels may influence the short-term weight loss response after LAGB. The lack of association after SG suggests that the influence of baseline endocrine and metabolic factors may not be relevant for procedures with greater and more immediate calorie intake restriction.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Swinburn BA, Sacks G, Hall KD, McPherson K, Finegood DT, Moodie ML, et al. The global obesity pandemic: shaped by global drivers and local environments. Lancet. 2011;378:804–14.
Peeters A, Barendregt JJ, Willekens F, Mackenbach JP, Mamun AA, Bonneux L, et al. Obesity in adulthood and its consequences for life expectancy: a life-table analysis. Ann Intern Med. 2003;138:24–32.
Jakobsen GS, Småstuen MC, Sandbu R, Nordstrand N, Hofsø D, Lindberg M, et al. Association of bariatric surgery vs medical obesity treatment with long-term medical complications and obesity-related comorbidities. JAMA. 2018;319:291–301.
Eldar S, Heneghan H, Brethauer S, Schauer P. Bariatric surgery for treatment of obesity. Int J Obes. 2011;35:S16–S21.
Fox CS, Pencina MJ, D’Agostino RB, Murabito JM, Seely EW, Pearce EN, et al. Relations of thyroid function to body weight: cross-sectional and longitudinal observations in a community-based sample. Arch Int Med. 2008;168:587–92.
Mullur R, Liu Y-Y, Brent GA. Thyroid hormone regulation of metabolism. Physiol Rev. 2014;94:355–82.
Liu G, Liang L, Bray GA, Qi L, Hu FB, Rood J, et al. Thyroid hormones and changes in body weight and metabolic parameters in response to weight loss diets: the POUNDS LOST trial. Int J Obes. 2017;41:878–86.
Marzullo P, Minocci A, Mele C, Fessehatsion R, Tagliaferri M, Pagano L, et al. The relationship between resting energy expenditure and thyroid hormones in response to short-term weight loss in severe obesity. PLoS ONE. 2018;13:e0205293.
Hashimoto K, Tagami T, Yamakage H, Muranaka K, Tanaka M, Odori S, et al. Serum free thyroxine levels is associated with the efficacy of weight reduction therapy in obese female patients. Endocr J. 2016;63:221–9.
Wolters B, Lass N, Reinehr T. TSH and free triiodothyronine concentrations are associated with weight loss in a lifestyle intervention and weight regain afterwards in obese children. Eur J Endocrinol. 2013;168:323–9.
Brethauer SA, Kim J, El Chaar M, Papasavas P, Eisenberg D, Rogers A, et al. Standardized outcomes reporting in metabolic and bariatric surgery. Obes Surg. 2015;25:587–606.
Janssen IM, Homan J, Schijns W, Betzel B, Aarts EO, Berends FJ, et al. Subclinical hypothyroidism and its relation to obesity in patients before and after Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2015;11:1257–63.
De Moraes CMM, Mancini MC, de Melo ME, Figueiredo DA, Villares SMF, Rascovski A, et al. Prevalence of subclinical hypothyroidism in a morbidly obese population and improvement after weight loss induced by Roux-en-Y gastric bypass. Obes Surg. 2005;15:1287–91.
Neves JS, Souteiro P, Oliveira SC, Pedro J, Magalhães D, Guerreiro V, et al. Preoperative thyroid function and weight loss after bariatric surgery. Int J Obes. 2019;43:432–6.
Muraca E, Ciardullo S, Oltolini A, Zerbini F, Bianconi E, Perra S, et al. Resting energy expenditure in obese women with primary hypothyroidism and appropriate levothyroxine replacement therapy. J Clin Endocrinol Metab. 2020;105:dgaa097.
Sesti G, Folli F, Perego L, Hribal ML, Pontiroli AE. Effects of weight loss in metabolically healthy obese subjects after laparoscopic adjustable gastric banding and hypocaloric diet. PLoS ONE. 2011;6:e17737.
Bradley D, Magkos F, Klein S. Effects of bariatric surgery on glucose homeostasis and type 2 diabetes. Gastroenterology. 2012;143:897–912.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics
The protocol (TIREOBARIATRIC) was approved by the ethics committee della Provincia di Monza e Brianza.
Informed consent
Informed consent has been obtained from each patient or subject after full explanation of the purpose and nature of all procedures used.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Muraca, E., Oltolini, A., Pizzi, M. et al. Baseline TSH levels and short-term weight loss after different procedures of bariatric surgery. Int J Obes 45, 326–330 (2021). https://doi.org/10.1038/s41366-020-00665-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-020-00665-6
This article is cited by
-
Free T4 is associated with exenatide-related weight loss in patients with type 2 diabetes mellitus and obesity
International Journal of Diabetes in Developing Countries (2024)