Abstract
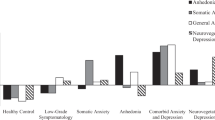
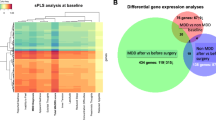
We identified biologically relevant moderators of response to tumor necrosis factor (TNF)-α inhibitor, infliximab, among 60 individuals with bipolar depression. Data were derived from a 12-week, randomized, placebo-controlled clinical trial secondarily evaluating the efficacy of infliximab on a measure of anhedonia (i.e., Snaith–Hamilton Pleasure Scale). Three inflammatory biotypes were derived from peripheral cytokine measurements using an iterative, machine learning-based approach. Infliximab-randomized participants classified as biotype 3 exhibited lower baseline concentrations of pro- and anti-inflammatory cytokines and soluble TNF receptor-1 and reported greater pro-hedonic improvements, relative to those classified as biotype 1 or 2. Pretreatment biotypes also moderated changes in neuroinflammatory substrates relevant to infliximab’s hypothesized mechanism of action. Neuronal origin-enriched extracellular vesicle (NEV) protein concentrations were reduced to two factors using principal axis factoring: phosphorylated nuclear factorκB (p-NFκB), Fas-associated death domain (p-FADD), and IκB kinase (p-IKKα/β) and TNF receptor-1 (TNFR1) comprised factor “NEV1,” whereas phosphorylated insulin receptor substrate-1 (p-IRS1), p38 mitogen-activated protein kinase (p-p38), and c-Jun N-terminal kinase (p-JNK) constituted “NEV2”. Among infliximab-randomized subjects classified as biotype 3, NEV1 scores were decreased at weeks 2 and 6 and increased at week 12, relative to baseline, and NEV2 scores increased over time. Decreases in NEV1 scores and increases in NEV2 scores were associated with greater reductions in anhedonic symptoms in our classification and regression tree model (r2 = 0.22, RMSE = 0.08). Our findings provide preliminary evidence supporting the hypothesis that the pro-hedonic effects of infliximab require modulation of multiple TNF-α signaling pathways, including NF-κB, IRS1, and MAPK.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Rush AJ, Trivedi MH, Wisniewski SR, Nierenberg AA, Stewart JW, Warden D, et al. Acute and longer-term outcomes in depressed outpatients requiring one or several treatment steps: a STAR*D report. Am J Psychiatry. 2006;163:1905–17. https://doi.org/10.1176/ajp.2006.163.11.1905.
Fava M, Rush AJ, Wisniewski SR, Nierenberg AA, Alpert JE, McGrath PJ, et al. A comparison of mirtazapine and nortriptyline following two consecutive failed medication treatments for depressed outpatients: a STAR*D report. Am J Psychiatry. 2006;163:1161–72. https://doi.org/10.1176/appi.ajp.163.7.1161.
Insel TR, Cuthbert BN. Medicine. Brain disorders? Precisely. Sci. 2015;348:499–500. https://doi.org/10.1126/science.aab2358.
Trivedi MH, Morris DW, Wisniewski SR, Lesser I, Nierenberg AA, Daly E, et al. Increase in work productivity of depressed individuals with improvement in depressive symptom severity. Am J Psychiatry. 2013;170:633–41. https://doi.org/10.1176/appi.ajp.2012.12020250.
Webb CA, Trivedi MH, Cohen ZD, Dillon DG, Fournier JC, Goer F, et al. Personalized prediction of antidepressant v. placebo response: evidence from the EMBARC study. Psychol Med. 2019;49:1118–27. https://doi.org/10.1017/S0033291718001708.
Lee Y, Ragguett R-M, Mansur RB, Boutilier JJ, Rosenblat JD, Trevizol A, et al. Applications of machine learning algorithms to predict therapeutic outcomes in depression: a meta-analysis and systematic review. J Affect Disord. 2018;241:519–32. https://doi.org/10.1016/j.jad.2018.08.073.
Strawbridge R, Arnone D, Danese A, Papadopoulos A, Herane Vives A, Cleare AJ. Inflammation and clinical response to treatment in depression: a meta-analysis. Eur Neuropsychopharmacol. 2015;25:1532–43. https://doi.org/10.1016/j.euroneuro.2015.06.007.
Benedetti F, Poletti S, Hoogenboezem TA, Locatelli C, de Wit H, Wijkhuijs AJM, et al. Higher baseline proinflammatory cytokines mark poor antidepressant response in bipolar disorder. J Clin Psychiatry. 2017;78:e986–93. https://doi.org/10.4088/JCP.16m11310.
Arteaga-Henríquez G, Simon MS, Burger B, Weidinger E, Wijkhuijs A, Arolt V, et al. Low-grade inflammation as a predictor of antidepressant and anti-inflammatory therapy response in MDD patients: a systematic review of the literature in combination with an analysis of experimental data collected in the EU-MOODINFLAME Consortium. Front Psychiatry. 2019;10:458. https://doi.org/10.3389/fpsyt.2019.00458.
Miller AH, Raison CL. The role of inflammation in depression: from evolutionary imperative to modern treatment target. Nat Rev Immunol. 2016;16:22–34. https://doi.org/10.1038/nri.2015.5.
Rosenblat JD, Kakar R, Berk M, Kessing LV, Vinberg M, Baune BT, et al. Anti-inflammatory agents in the treatment of bipolar depression: a systematic review and meta-analysis. Bipolar Disord. 2016;18:89–101. https://doi.org/10.1111/bdi.12373.
Kappelmann N, Lewis G, Dantzer R, Jones PB, Khandaker GM. Antidepressant activity of anti-cytokine treatment: a systematic review and meta-analysis of clinical trials of chronic inflammatory conditions. Mol Psychiatry. 2018;23:335–43. https://doi.org/10.1038/mp.2016.167.
McIntyre RS, Subramaniapillai M, Lee Y, Pan Z, Carmona NE, Shekotikhina M, et al. Efficacy of adjunctive infliximab vs placebo in the treatment of adults with bipolar I/II depression: a randomized clinical trial. JAMA Psychiatry. 2019;76:783–90. https://doi.org/10.1001/jamapsychiatry.2019.0779.
Lee Y, Mansur RB, Brietzke E, Carmona NE, Subramaniapillai M, Pan Z, et al. Efficacy of adjunctive infliximab vs. placebo in the treatment of anhedonia in bipolar I/II depression. Brain Behav Immun. 2020. https://doi.org/10.1016/j.bbi.2020.04.063.
Raison CL, Rutherford RE, Woolwine BJ, Shuo C, Schettler P, Drake DF, et al. A randomized controlled trial of the tumor necrosis factor antagonist infliximab for treatment-resistant depression: the role of baseline inflammatory biomarkers. JAMA Psychiatry. 2013;70:31–41. https://doi.org/10.1001/2013.jamapsychiatry.4.
Andersson KME, Wasén C, Juzokaite L, Leifsdottir L, Erlandsson MC, Silfverswärd ST, et al. Inflammation in the hippocampus affects IGF1 receptor signaling and contributes to neurological sequelae in rheumatoid arthritis. Proc Natl Acad Sci USA. 2018;115:E12063–72. https://doi.org/10.1073/pnas.1810553115.
Kleinridders A, Cai W, Cappellucci L, Ghazarian A, Collins WR, Vienberg SG, et al. Insulin resistance in brain alters dopamine turnover and causes behavioral disorders. Proc Natl Acad Sci USA. 2015;112:3463–8. https://doi.org/10.1073/pnas.1500877112.
Nasca C, Dobbin J, Bigio B, Watson K, de Angelis P, Kautz M, et al. Insulin receptor substrate in brain-enriched exosomes in subjects with major depression: on the path of creation of biosignatures of central insulin resistance. Mol Psychiatry. 2020. https://doi.org/10.1038/s41380-020-0804-7.
Millett CE, Harder J, Locascio JJ, Shanahan M, Santone G, Fichorova RN, et al. TNF-α and its soluble receptors mediate the relationship between prior severe mood episodes and cognitive dysfunction in euthymic bipolar disorder. Brain Behav Immun. 2020. https://doi.org/10.1016/j.bbi.2020.04.003.
Haroon E, Welle JR, Woolwine BJ, Goldsmith DR, Baer W, Patel T, et al. Associations among peripheral and central kynurenine pathway metabolites and inflammation in depression. Neuropsychopharmacology. 2020;45:998–1007. https://doi.org/10.1038/s41386-020-0607-1.
Osimo EF, Pillinger T, Rodriguez IM, Khandaker GM, Pariante CM, Howes OD. Inflammatory markers in depression: a meta-analysis of mean differences and variability in 5,166 patients and 5,083 controls. Brain Behav Immun. 2020;87:901–9. https://doi.org/10.1016/j.bbi.2020.02.010.
Husain M, Roiser JP. Neuroscience of apathy and anhedonia: a transdiagnostic approach. Nat Rev Neurosci. 2018;19:470–84. https://doi.org/10.1038/s41583-018-0029-9.
Lee Y, Subramaniapillai M, Brietzke E, Mansur RB, Ho RC, Yim SJ, et al. Anti-cytokine agents for anhedonia: targeting inflammation and the immune system to treat dimensional disturbances in depression. Ther Adv Psychopharmacol. 2018;8:337–48. https://doi.org/10.1177/2045125318791944.
Snaith RP, Hamilton M, Morley S, Humayan A, Hargreaves D, Trigwell P. A scale for the assessment of hedonic tone the Snaith-Hamilton Pleasure Scale. Br J Psychiatry. 1995;167:99–103. https://doi.org/10.1192/bjp.167.1.99.
Leventhal AM, Chasson GS, Tapia E, Miller EK, Pettit JW. Measuring hedonic capacity in depression: a psychometric analysis of three anhedonia scales. J Clin Psychol. 2006;62:1545–58. https://doi.org/10.1002/jclp.20327.
Kramer NE, Cosgrove VE, Dunlap K, Subramaniapillai M, McIntyre RS, Suppes T. A clinical model for identifying an inflammatory phenotype in mood disorders. J Psychiatr Res. 2019;113:148–58. https://doi.org/10.1016/j.jpsychires.2019.02.005.
Mustapic M, Eitan E, Werner JK Jr, Berkowitz ST, Lazaropoulos MP, Tran J, et al. Plasma extracellular vesicles enriched for neuronal origin: a potential window into brain pathologic processes. Front Neurosci. 2017;11:278. https://doi.org/10.3389/fnins.2017.00278.
Mullins RJ, Mustapic M, Goetzl EJ, Kapogiannis D. Exosomal biomarkers of brain insulin resistance associated with regional atrophy in Alzheimer’s disease. Hum Brain Mapp. 2017;38:1933–40. https://doi.org/10.1002/hbm.23494.
Athauda D, Gulyani S, Karnati HK, Li Y, Tweedie D, Mustapic M, et al. Utility of neuronal-derived exosomes to examine molecular mechanisms that affect motor function in patients with parkinson disease: a secondary analysis of the exenatide-PD trial. JAMA Neurol. 2019;76:420–9. https://doi.org/10.1001/jamaneurol.2018.4304.
Sáenz-Cuesta M, Arbelaiz A, Oregi A, Irizar H, Osorio-Querejeta I, Muñoz-Culla M, et al. Methods for extracellular vesicles isolation in a hospital setting. Front Immunol. 2015;6:50. https://doi.org/10.3389/fimmu.2015.00050.
Mansur RB, Delgado-Peraza F, Subramaniapillai M, Lee Y, Iacobucci M, Rodrigues N, et al. Extracellular vesicle biomarkers reveal inhibition of neuroinflammation by infliximab in association with antidepressant response in adults with bipolar depression. Cells. 2020;9. https://doi.org/10.3390/cells9040895.
Breiman L. Classification and regression trees. Boca Raton: Routledge; 2017.
Bergstra J, Bengio Y. Random search for hyper-parameter optimization. J Mach Learn Res. 2012;13:281–305. http://www.jmlr.org/papers/v13/bergstra12a.html.
Shmueli G. To explain or to predict? Stat Sci. 2010;25:289–310. https://projecteuclid.org/euclid.ss/1294167961.
R Core Team. R: A Language and Environment for Statistical Computing. Vienna, Austria: R Foundation for Statistical Computing; 2020. https://www.R-project.org/.
Revelle W. psych: procedures for psychological, psychometric, and personality research. Evanston, Illinois: Northwestern University; 2019. https://CRAN.R-project.org/package=psych.
Hennig C. fpc: flexible procedures for clustering. 2019. https://CRAN.R-project.org/package=fpc.
Hennig C. Cluster-wise assessment of cluster stability. Comput Stat Data Anal. 2007;52:258–71. http://www.sciencedirect.com/science/article/pii/S0167947306004622.
Pedregosa F, Varoquaux G, Gramfort A, Michel V, Thirion B, Grisel O, et al. Scikit-learn: machine learning in python. J Mach Learn Res. 2011;12:2825–30.
Chen G, Bhojani MS, Heaford AC, Chang DC, Laxman B, Thomas DG, et al. Phosphorylated FADD induces NF-kappaB, perturbs cell cycle, and is associated with poor outcome in lung adenocarcinomas. Proc Natl Acad Sci USA. 2005;102:12507–12. https://doi.org/10.1073/pnas.0500397102.
Lawrence T, Bebien M, Liu GY, Nizet V, Karin M. IKKalpha limits macrophage NF-kappaB activation and contributes to the resolution of inflammation. Nature. 2005;434:1138–43. https://doi.org/10.1038/nature03491.
Christian F, Smith EL, Carmody RJ. The regulation of NF-κB subunits by phosphorylation. Cells. 2016;5. https://doi.org/10.3390/cells5010012.
Block ML, Zecca L, Hong J-S. Microglia-mediated neurotoxicity: uncovering the molecular mechanisms. Nat Rev Neurosci. 2007;8:57–69. https://doi.org/10.1038/nrn2038.
Barger SW, Hörster D, Furukawa K, Goodman Y, Krieglstein J, Mattson MP. Tumor necrosis factors alpha and beta protect neurons against amyloid beta-peptide toxicity: evidence for involvement of a kappa B-binding factor and attenuation of peroxide and Ca2+ accumulation. Proc Natl Acad Sci USA. 1995;92:9328–32. https://doi.org/10.1073/pnas.92.20.9328.
Fenn AM, Henry CJ, Huang Y, Dugan A, Godbout JP. Lipopolysaccharide-induced interleukin (IL)-4 receptor-α expression and corresponding sensitivity to the M2 promoting effects of IL-4 are impaired in microglia of aged mice. Brain Behav Immun. 2012;26:766–77. https://doi.org/10.1016/j.bbi.2011.10.003.
Mehta D, Raison CL, Woolwine BJ, Haroon E, Binder EB, Miller AH, et al. Transcriptional signatures related to glucose and lipid metabolism predict treatment response to the tumor necrosis factor antagonist infliximab in patients with treatment-resistant depression. Brain Behav Immun. 2013;31:205–15. https://doi.org/10.1016/j.bbi.2013.04.004.
Lügering A, Schmidt M, Lügering N, Pauels HG, Domschke W, Kucharzik T. Infliximab induces apoptosis in monocytes from patients with chronic active Crohn’s disease by using a caspase-dependent pathway. Gastroenterology. 2001;121:1145–57. https://doi.org/10.1053/gast.2001.28702.
Chaudhari U, Romano P, Mulcahy LD, Dooley LT, Baker DG, Gottlieb AB. Efficacy and safety of infliximab monotherapy for plaque-type psoriasis: a randomised trial. Lancet. 2001;357:1842–7. https://doi.org/10.1016/s0140-6736(00)04954-0.
Horiuchi T, Mitoma H, Harashima S-I, Tsukamoto H, Shimoda T. Transmembrane TNF-alpha: structure, function and interaction with anti-TNF agents. Rheumatology. 2010;49:1215–28. https://doi.org/10.1093/rheumatology/keq031.
Mitoma H, Horiuchi T, Hatta N, Tsukamoto H, Harashima S-I, Kikuchi Y, et al. Infliximab induces potent anti-inflammatory responses by outside-to-inside signals through transmembrane TNF-alpha. Gastroenterology. 2005;128:376–92. https://doi.org/10.1053/j.gastro.2004.11.060.
Genovese T, Mazzon E, Crisafulli C, Di Paola R, Muià C, Esposito E, et al. TNF-alpha blockage in a mouse model of SCI: evidence for improved outcome. Shock. 2008;29:32–41. https://doi.org/10.1097/shk.0b013e318059053a.
Hoffmann A, Natoli G, Ghosh G. Transcriptional regulation via the NF-kappaB signaling module. Oncogene. 2006;25:6706–16. https://doi.org/10.1038/sj.onc.1209933.
Lügering A, Lebiedz P, Koch S, Kucharzik T. Apoptosis as a therapeutic tool in IBD? Ann NY Acad Sci. 2006;1072:62–77. https://doi.org/10.1196/annals.1326.013.
Nikolaus S, Raedler A, Kühbacker T, Sfikas N, Fölsch UR, Schreiber S. Mechanisms in failure of infliximab for Crohn’s disease. Lancet. 2000;356:1475–9. https://doi.org/10.1016/s0140-6736(00)02871-3.
Hotamisligil GS, Peraldi P, Budavari A, Ellis R, White MF, Spiegelman BM. IRS-1-mediated inhibition of insulin receptor tyrosine kinase activity in TNF-alpha- and obesity-induced insulin resistance. Science. 1996;271:665–8. https://doi.org/10.1126/science.271.5249.665.
Greene MW, Sakaue H, Wang L, Alessi DR, Roth RA. Modulation of insulin-stimulated degradation of human insulin receptor substrate-1 by Serine 312 phosphorylation. J Biol Chem. 2003;278:8199–211. https://doi.org/10.1074/jbc.M209153200.
Stagakis I, Bertsias G, Karvounaris S, Kavousanaki M, Virla D, Raptopoulou A, et al. Anti-tumor necrosis factor therapy improves insulin resistance, beta cell function and insulin signaling in active rheumatoid arthritis patients with high insulin resistance. Arthritis Res Ther. 2012;14:R141 https://doi.org/10.1186/ar3874.
Hançer NJ, Qiu W, Cherella C, Li Y, Copps KD, White MF. Insulin and metabolic stress stimulate multisite serine/threonine phosphorylation of insulin receptor substrate 1 and inhibit tyrosine phosphorylation. J Biol Chem. 2014;289:12467–84. https://doi.org/10.1074/jbc.M114.554162.
Ho RCM, Chua AC, Tran BX, Choo CC, Husain SF, Vu GT, et al. Factors associated with the risk of developing coronary artery disease in medicated patients with major depressive disorder. Int J Environ Res Public Health. 2018;15. https://doi.org/10.3390/ijerph15102073.
Goldstein BI, Carnethon MR, Matthews KA, McIntyre RS, Miller GE, Raghuveer G, et al. Major depressive disorder and bipolar disorder predispose youth to accelerated atherosclerosis and early cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 2015;132:965–86. https://doi.org/10.1161/CIR.0000000000000229.
Rosenstiel P, Agnholt J, Kelsen J, Medici V, Waetzig GH, Seegert D, et al. Differential modulation of p38 mitogen activated protein kinase and STAT3 signalling pathways by infliximab and etanercept in intestinal T cells from patients with Crohn’s disease. Gut. 2005;54:314–5. https://www.ncbi.nlm.nih.gov/pubmed/15647208.
Waetzig GH, Seegert D, Rosenstiel P, Nikolaus S, Schreiber S. p38 mitogen-activated protein kinase is activated and linked to TNF-alpha signaling in inflammatory bowel disease. J Immunol. 2002;168:5342–51. https://doi.org/10.4049/jimmunol.168.10.5342.
Waetzig GH, Rosenstiel P, Nikolaus S, Seegert D, Schreiber S. Differential p38 mitogen-activated protein kinase target phosphorylation in responders and nonresponders to infliximab. Gastroenterology. 2003;125:633–4. https://doi.org/10.1016/s0016-5085(03)00979-x.
Acknowledgements
This study was funded by the Stanley Medical Research Institute (Grant 13T-012 to RSM and TS). This research was supported in part by the Intramural Research Program of the National Institute on Aging, NIH (authors DK, FDP, SC, CNO).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
RSM has received research grant support from the Stanley Medical Research Institute and the Canadian Institutes of Health Research/Global Alliance for Chronic Diseases/National Natural Science Foundation of China and speaker/consultation fees from Lundbeck, Janssen, Shire, Purdue, Pfizer, Otsuka, Allergan, Takeda, Neurocrine, Sunovion, and Minerva within the past 36 months. EB has been supported by Faculty of Health Sciences, Queen’s University and received honoraria as speaker/member of advisory board from Daiichi-Sankyo not related to the content of this study. JDR has received research grant support from the University of Toronto, Canadian Cancer Society, Canadian Psychiatric Association, American Psychiatric Association, American Society of Psychopharmacology (New Investigator Award), University Health Network Centre for Mental Health, Joseph M. West Family Memorial Fund and Timeposters Fellowship and industry funding for speaker/consultation/research fees from Allergan, Lundbeck and COMPASS; and is the medical director of a private clinic providing off-label ketamine infusions for depression. BIG receives grant or research support from the Brain and Behavior Research Foundation (NARSAD), Brain Canada, the Canadian Institutes of Health Research, the Heart and Stroke Foundation, National Institute of Mental Health, the Ontario Ministry of Research and Innovation, and the Departments of Psychiatry of Sunnybrook Health Sciences Centre and the University of Toronto. MV has received consultancy fees from Lundbeck, Sunovion, and Janssen/Cilag within the last 3 years. All other authors declare no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Lee, Y., Mansur, R.B., Brietzke, E. et al. Peripheral inflammatory biomarkers define biotypes of bipolar depression. Mol Psychiatry 26, 3395–3406 (2021). https://doi.org/10.1038/s41380-021-01051-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41380-021-01051-y
This article is cited by
-
Putative Risk Biomarkers of Bipolar Disorder in At-risk Youth
Neuroscience Bulletin (2024)
-
Neuron-derived extracellular vesicles in blood reveal effects of exercise in Alzheimer’s disease
Alzheimer's Research & Therapy (2023)