Abstract
Several studies argued that cardiovascular evaluation of patients with nonfunctioning adrenal incidentaloma is of particular importance. Therefore, we aimed to evaluate the possibility of stratifying the cardiometabolic risk using metanephrine levels in this setting of patients. A retrospective cross-sectional study was designed, collecting data of metanephrine values in 828 patients with nonfunctioning adrenal incidentaloma, referred to our Division within the University of Turin between 2007 and 2021. The univariate analysis showed associations between urine metanephrines and cardiometabolic variables/parameters, particularly considering the noradrenaline metabolite. At the univariate regression, normetanephrine was associated with metabolic syndrome (OR = 1.13, p = 0.002), hypertensive cardiomyopathy (OR = 1.09, p = 0.026), microalbuminuria (OR = 1.14, p = 0.024), and eGFR < 60 mL/min/1.73 m2 (OR = 1.11, p = 0.013), while metanephrine was associated with microalbuminuria (OR = 1.50, p = 0.008). At multivariate regression, considering all major cardiovascular risk factors as possible confounders, normetanephrine retained a significant association with metabolic syndrome (OR = 1.10, p = 0.037). Moreover, metanephrine retained a significant association with the presence of microalbuminuria (OR = 1.66, p = 0.003). The present study showed a further role for metanephrines in the cardiovascular risk stratification of patients with nonfunctioning adrenal incidentaloma. Individuals with high levels of these indirect markers of sympathetic activity should be carefully monitored and may benefit from an aggressive treatment to reduce their additional cardiometabolic burden.
Similar content being viewed by others
Introduction
An adrenal incidentaloma is an adrenal mass ≥ 1 cm, detected on imaging not performed for suspected adrenal disease1. In this setting, the diagnostic work-up consists in the exclusion of a malignant neoplasm (either primary or a metastatic tumor) and in the assessment of the hormone secretion, which are both potential indications for surgical treatment. An accurate hormone evaluation of gluco- and mineralocorticoid function, in some cases of androgenic secretion and in most cases of the catecholamine (CA) production is thus performed. Dopamine, noradrenaline and adrenaline derive from tyrosine metabolism2 and are adaptive/maladaptive stress hormones. The metanephrines, the urine and plasma metabolites of CA through the activity of Catechol-O-MethylTransferase (COMT), are nowadays the preferred markers for diagnosis and follow-up of pheochromocytoma and paraganglioma (PPGL)3,4,5. Metanephrines derive from non-neuronal sources (extra-neuronal and adrenomedullary pathways), because sympathetic nerves contain monoamine oxidase (MAO), but not COMT2. It has been suggested that metanephrines can be considered indirect markers of the whole sympathetic system activity6; moreover, a recent research of our group showed that, in patients without the evidence of PPGL, the elevation of metanephrines is associated with cardiometabolic complications, and that metanephrines could thus be useful in the stratification of cardiovascular (CV) risk7, highlighting the importance of a strict follow-up and an aggressive treatment of cardiometabolic risk factors in patients with a mild elevation of these metabolites.
In last years, the scientific community showed growing interest in the definition of the CV risk in patients with nonfunctioning adrenal incidentaloma (NFAI), even if a cause-effect relationship is not readily evident. In this setting, a non-detectable small amount of glucocorticoid excess would not completely justify the CV risk and the impairment of cardiometabolic profile seems to occur over a long time, leading to difficulties in studying this issue in a prospective manner.
Therefore, we aimed to determine if higher levels of urine metanephrines can be associated with CV and metabolic risk in patients with NFAI. In order to account for the physiologic variability of the sympathetic activity, we collected a large sample size, and the most commonly used risk scores were adopted as the assessment tool for CV risk.
Materials and methods
Design and study population
This retrospective cross-sectional study followed the STROBE statement for reporting observational studies8 and analysed all consecutive patients with adrenal incidentaloma, referred to the Division of Endocrinology, Diabetes and Metabolism of the City of Health and Science University Hospital of Turin, between September 2007 and September 2021. Patients < 18 years old, with chronic heart failure, arrhythmias, secondary hypertension (primary aldosteronism, pheochromocytoma/paraganglioma, autonomous cortisol secretion, overt hypercortisolism, obstructive sleep apnoea, renal artery stenosis, primary hyperparathyroidism and other causes), renal insufficiency with estimated glomerular filtration rate (eGFR) < 30 mL/min, psychiatric illness, liver cirrhosis, chronic diseases with major organ involvement, excessive alcohol ingestion, current assumption of sympathomimetics, cocaine and drugs commonly affecting the measurement of metanephrines (Acetaminophen, Labetalol, Sotalol, tricyclic antidepressants, Buspirone, Phenoxybenzamine, MAO inhibitors, Sulphasalazine and Levodopa) were excluded from the study.
Regarding the hormone evaluation of incidentaloma, patients with cortisol over 1.8 μg/dL after 1 mg dexamethasone suppression test (DST) and with aldosterone-to-renin ratio (ARR) > 300 [(pg/mL)/(ng/mL/h)] or with ARR > 200 [(pg/mL)/(ng/mL/h)] with signs and symptoms of mineralocorticoid hypertension were excluded. The basal aldosterone cut-off for considering the suspicion of primary aldosterone was 150 pg/mL.
An accurate endocrinological evaluation (repeating the dosages of metanephrine, adding Chromogranin A and Neuron Specific Enolase, and even performing functional imaging techniques, where appropriate) and follow-up (every 6–12 months, if necessary) were performed for patients with metanephrine values over the upper cut-off limits. Patients diagnosed with PPGL were excluded, checking data from the registry of the Piedmont Oncological Network to avoid the risk of including small PPGL with mild/non-secretive phenotype.
Data were collected within prospective registries and analysed retrospectively. The study was performed in accordance with the guidelines in the Declaration of Helsinki and approved by the Ethics Committee of City of Health and Science University Hospital of Turin (no. 0035241). Written informed consent was obtained from all enrolled patients (ClinicalTrials.gov no. 04495231).
Clinical and biochemical investigations
Personal and clinical data, familial history of arterial hypertension, diabetes mellitus (DM) and early cardiovascular event, office blood pressure (BP) values9, serum levels of glucose, lipid profile, sodium, potassium, creatinine, values of 24-h urinary metanephrines, aldosterone, plasma renin activity (PRA) and cortisol after 1 mg dexamethasone suppression test (DST) were collected. Measurement of CA metabolites was performed on single or double 24-h urine collection. In the case of two or more dosages, we considered the value of the first collection. Cardiovascular risk was estimated using risk calculator (Framingham risk score10, Progetto CUORE11 and SCORE12).
Evaluation of metabolic syndrome and organ damage
Metabolic syndrome was defined according to the ATP III criteria13. Organ damage was defined according to the 2018 ESC/ESH guidelines. eGFR was estimated using CKD-EPI formula and microalbuminuria was defined between 30 and 300 mg/24 h or by an albumin to creatinine ratio of 30–300 mg/g. Left ventricular mass index, assessed by echocardiography, was calculated with the formula: 0.8 * 1.04 * [(interventricular septum + left ventricular internal diameter + inferolateral wall thickness)3 − left ventricular internal diameter3] + 0.6 gr; in normal weight subjects, this value was indexed for body surface area, and left ventricular hypertrophy was defined by a left ventricular mass index > 115 g/m2 for men and > 95 g/m2 for women; in overweight and obese subjects, it was indexed for height, and left ventricular hypertrophy was defined by a left ventricular mass index > 50 g/m2.7 for men and > 47 g/m2.7 for women9.
Analytical methods
As previously described14, 24-h urinary metanephrines (normal ranges: normetanephrine 105–354 μg/day, metanephrine 74–298 μg/day) were measured by chromatographic determination on isocratic high-performance liquid chromatography (HPLC) system with electrochemical detector fixed with a potential of 740 mV (Chromsystems Instruments & Chemicals GmbH, Gräfelfing, Germany). Briefly, 1 mL of 24 h urine samples were mixed with 100 µl Internal Standard and poured in sealable hydrolysis tubes that were incubated for 30 min at 90°–100° in a water bath. Then a neutralization buffer was added to samples, and the entire neutralized urines were applied to sample clean up columns for a solid-phase extraction, that were successively mixed, centrifuged, and washed. Amount (20–50 μl) of eluates were injected into the HPLC system, and the retention times of normetanephrine and metanephrine and Internal Standard were respectively 5.5, 7.0 and 8.4 min. Furthermore, limits of quantification, intra-assay and inter-assay coefficients of variation were respectively: 5 mg/L, 1.4% and 2.7% for normetanephrine and 11 mg/L, 1.8% and 2.8% for metanephrine.
Statistical analysis
Statistical analysis of this study was similar to another research published by our group7, but the studied population was completely different from the previous paper, as it clear from the above sections. Baseline characteristics of all patients with NFAI included in the analysis were summarized using mean and standard deviation (SD), after the analysis of each variable/parameter through the quantile–quantile (Q-Q) plot, considering the large sample size. Binary and categorical data were reported using percent values. In the descriptive statistics, the sample was divided according to the tertiles of normetanephrine and metanephrine. The division into tertiles was decided because it allowed to have an adequate number of patients in each tertile, thus reinforcing the power of the statistical analysis. Between groups differences in personal and clinical features were evaluated by one-way ANOVA for continuous variables and chi-square test or Fisher’s exact test for categorical variables, as appropriate.
Associations between the levels of normetanephrine/metanephrine and the presence of cardiometabolic/renal complications (hypertensive cardiomyopathy, metabolic syndrome, eGFR < 60 ml/min/1.73 m2 and albuminuria) were assessed through univariate and multivariate logistic regressions, considering all the risk factors known to be possibly related with adverse cardiovascular or renal outcomes as possible confounders.
In this analysis, metanephrines were considered as continuous variables, and the coefficients of the models (with correspondent odds ratios) were computed by considering 100 μg/day as their unitary increase. A p-value < 0.05 was considered statistically significant. Statistical analysis was performed using R 3.5.3 (R Core Team, R Foundation for Statistical Computing, Vienna, Austria, 2019).
Results
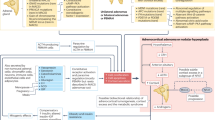
After the application of the inclusion/exclusion criteria, as shown in Fig. 1, 828 patients with NFAI were enrolled in the study (324 males—39.1% and 505 females—60.9%). The sample was divided into tertiles of normetanephrine (I tertile: 20.0–248.0 μg/day; II tertile: 249.0–388.0 μg/day; III tertile: 390.0–2158.0 μg/day) and metanephrine (I tertile: 10.0–69.0 μg/day; II tertile: 69.2–119.0 μg/day; III tertile: 119.6–510.0 μg/day).
When comparing patient characteristics among tertiles, patients with higher levels of urine normetanephrine proved to be older (p = 0.002), had higher proportion of male sex (p < 0.001), smoking habit (p = 0.037), obesity (p = 0.014), history of hypertensive crisis (p = 0.007), metabolic syndrome (p = 0.002), hypertensive cardiomyopathy (p = 0.027), higher values of BMI (p < 0.001), weight (p < 0.001), waist circumference (p = 0.003), office systolic BP (SBP, p = 0.019), office diastolic BP (DBP, p = 0.021), Framingham risk score (p < 0.001), and lower proportion of familial history of arterial hypertension (p = 0.014), compared to patients with normetanephrine into the I-II tertiles.
Regarding the drug therapy, patients with high levels of normetanephrine were taking higher number of antihypertensive drugs (p = 0.003) and had higher proportion of treatment with beta-blockers (p = 0.028), α-blockers (p = 0.005), and angiotensin II receptor blockers (ARB, p = 0.024), if compared to patients with normetanephrine into the I-II tertiles.
A similar analysis showed also that individuals with higher values of urine metanephrine had higher proportion of male sex (p < 0.001), smoking habit (p = 0.004), hypertensive crisis (p = 0.003), and treatment with MRA or amiloride (p < 0.001), but lower proportion of obesity (p = 0.036), and therapy with thiazide (-like) diuretics (p = 0.002), compared to patients with metanephrines into the I-II tertiles. No differences were found in the remaining variables/parameters (Tables 1, 2, 3 and S1).
Univariate and multivariate logistic regressions
In the present study, urine metanephrines were analysed as possible independent variables associated to cardiometabolic and renal complications, considering all other common risk factors as potential confounders of these associations.
At univariate regression, normetanephrine proved to be associated to metabolic syndrome (OR = 1.13, 95% CI 1.05–1.22; p = 0.002), hypertensive cardiomyopathy (OR = 1.09, 95% CI 1.01–1.18; p = 0.026), microalbuminuria (OR = 1.14, 95% CI 1.02–1.25; p = 0.024), and with eGFR < 60 mL/min/1.73 m2 (OR = 1.11, 95% CI 1.02–1.19; p = 0.013) (Table 4).
At multivariate analysis, normetanephrine retained a statistically significant association with metabolic syndrome (OR = 1.10, 95% CI 1.01–1.19; p = 0.037), after correction for sex, age, smoking habit (OR = 1.63, 95% CI 1.12–2.39; p = 0.011), familial history of CVD, number of antihypertensive drugs (OR = 1.49, 95% CI 1.27–1.76; p < 0.001) and eGFR (Table 5).
Urine normetanephrine was not significantly associated with presence of potentially hypertension-mediated organ damage, such as hypertensive cardiomyopathy (Table 6), microalbuminuria (Table 7) and impaired renal function (Table 8).
Regarding the adrenaline metabolite, at univariate logistic regression, metanephrine proved to be associated with microalbuminuria (OR = 1.50, 95% CI 1.13–1.87; p = 0.008); conversely, no significant associations with hypertensive cardiomyopathy, metabolic syndrome or eGFR < 60 mL/min/1.73 m2 were found (Table 4).
At multivariate analysis, metanephrine retained a statistically significant association with microalbuminuria (OR = 1.66, 95% CI 1.21–2.98; p = 0.003), considering sex, age, smoking habit, familial history of CVD, BMI, office SBP and DBP, DM (OR = 6.82, 95% CI 2.63–18.03; p < 0.001), eGFR (OR = 0.97, 95% CI 0.95–0.99; p = 0.004) and treatment with ACEi/ARB (OR = 3.65, 95% CI 1.09–12.92; p = 0.039), as covariates (Table 7).
Urine metanephrine was not associated with metabolic syndrome (Table 5), hypertensive cardiomyopathy (Table 6) or eGFR < 60 mL/min/1.73 m2 (Table 8).
To exclude interferences and potential sources of bias, the series was analyzed with the same statistics after excluding all patients treated with drugs affecting the sympathetic system. The results (data not shown) were not different from those previously reported.
Discussion
In the present study, we found that high levels of 24-h urinary metanephrine levels are associated with CV risk and cardiometabolic complications in a large cohort of patients with NFAI. Particularly, high levels of normetanephrine proved to be independently associated with metabolic syndrome, while high metanephrine levels showed an independent association with microalbuminuria. Our study provided evidence on the possibility to stratify cardiovascular risk in patients with NFAI through metanephrine levels, because of their capability in the indirect assessment of the sympathetic activity and not only in the diagnosis of PPGL.
In patients with adrenal incidentaloma, the role of mild cortisol excess has been described as a possible cause of metabolic disorders, such as diabetes15, cardiovascular events16 and mortality17, even if the mechanisms that account for the link between cortisol and cardiovascular diseases need to be clarified. But in NFAI, the risk of developing autonomous cortisol secretion is debate and heterogenous in the literature15,16,18. Therefore, a low degree of cortisol excess would not completely justify the additional cardiovascular risk, that was recently described in this group of patients. Even if it seems difficult to prove an association between cardiometabolic complications and NFAI, several studies argued that the cardiovascular evaluation of patients with incidental adrenal findings is of particular importance. In fact, it has been reported that patients with NFAI had high prevalence of arterial hypertension, even resistant19,20, dyslipidemia20, insulin resistance19,20,21,22, type 2 diabetes mellitus20,23 and metabolic syndrome21,24,25,26. It is possible that increased risk for cardiometabolic diseases reported in NFAI patients is at least partially dependent on adipose tissue activity27, as showed by increased leptin and resistin levels19, although data on adiponectin regulation are contradictory19,28. Moreover, some authors demonstrated increased arterial stiffness29,30,31, epicardial fat thickness32, left ventricular mass31,32,33, carotid intima-media thickness21,22,28,30,32,34,35 and other markers of atherosclerosis36 in patients with NFAI, compared to healthy subjects.
It has been suggested that NFAI can manifest a slight excess of cortisol that cannot be detected by current diagnostic tests or intermittent hormonal secretion29,37,38. Some authors hypothesized also that these adrenal tumors can secrete a small amount of non-routinely or non-currently detectable steroids with a detrimental cardiovascular effect. In fact, patients with adrenal incidentalomas showed different steroid profiles, depending on functional activity and adrenal morphology, with potential implications for their cardiovascular status39. It has also to be noted that adrenal cortex and medulla are morphologically and functionally interwoven, through a strong endocrine and paracrine interaction40. Cellular interactions of chromaffin and cortical cells are critical in physiology and disease41. Glucocorticoids play a role in the development of norepinephrine-secreting cells into epinephrine-secreting cells by upregulating the expression of Phenylethanolamine N-MethylTransferase42. Oppositely, CA and/or neuropeptides secreted by the adrenal medulla have been suggested to stimulate the release of steroids and the cellular function of the adrenal cortex40. Moreover, it was shown that if the adrenal cortex is absent or impaired, there could be also consequences for the adjacent medullary tissue43. So, it is also possible that the elevation of metanephrines in patients with NFAI can be related to the presence of the adrenal tumor, revealing a direct link between NFAI and cardiometabolic complications.
This study has several strengths. First of all, the large cohort of patients enrolled, which allows to derive several interesting data; second, the importance of having collected data from a single center prospective registry and third, the excellence of the laboratory that performed the analysis of metanephrines.
Nevertheless, we should describe some study limitations. The retrospective cross-sectional design does not allow to evaluate postsurgical alterations in metabolic parameters and cardiovascular risk factors in NFAI patients. Moreover, metanephrines are not direct markers for the evaluation of sympathetic activity, because they derive from the non-neuronal metabolism of CA, which are the metabolically active hormones; in the last years more direct methods have been developed, but these techniques are not widely adopted in routine practice. It should be noted that small or non-secretive PPGL, which may bias the cardiovascular stratification, could be included in the analysis. However, the careful diagnostic work-up, the at least five years of follow-up, and the data checking through the Piedmont Oncological Network, reduced the risk of misdiagnoses. Moreover, the consistency of the obtained data suggests that these limitations were not critical for the results of the present study.
The present study showed, for the first time, a further role of a simple diagnostic tool, routinely adopted for the hormone assessment of adrenal tumors, for the cardiovascular risk stratification of patients with NFAI. Endocrine Society guidelines3 recommend that all patients with mildly elevated metanephrines should be followed up, because in situations of borderline positive test results and low probability of a tumor, a wait-and-retest approach can illuminate increased likelihood of an enlarging small tumor. This study went further, because our results proved that metanephrines have the capability to stratify cardiovascular risk, through their informative role about the sympathetic activity, with the intent to identify those patients who could benefit from a more aggressive or specific treatment of the known CV risk factors. Nowadays, data in literature have demonstrated that several behavioral (weight loss and sodium restriction)44 and therapeutic strategies (antihypertensive drugs, baroreflex activation, statins and some classes of antidiabetic agents)45,46,47,48,49,50 are active on sympathoinhibition. Using these strategies for patients with NFAI and high metanephrine levels, it may be possible to medically manage this additional cardiometabolic burden, though this needs to be demonstrated in interventional studies.
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
References
Fassnacht, M. et al. Management of adrenal incidentalomas: European Society of Endocrinology Clinical Practice Guideline in collaboration with the European Network for the Study of Adrenal Tumors. Eur. J. Endocrinol. 175, G1–G34 (2016).
Eisenhofer, G., Kopin, I. J. & Goldstein, D. S. Catecholamine metabolism: A contemporary view with implications for physiology and medicine. Pharmacol. Rev. 56, 331–349 (2004).
Lenders, J. W. M. et al. Pheochromocytoma and paraganglioma: An endocrine society clinical practice guideline. J. Clin. Endocrinol. Metab. 99, 1915–1942 (2014).
Plouin, P. F. et al. European Society of Endocrinology Clinical Practice Guideline for long-term follow-up of patients operated on for a phaeochromocytoma or a paraganglioma. Eur. J. Endocrinol. 174, G1–G10 (2016).
Parasiliti-Caprino, M. et al. Predictors of recurrence of pheochromocytoma and paraganglioma: A multicenter study in Piedmont, Italy. Hypertens. Res. 43, 500–510 (2020).
Eisenhofer, G. et al. Plasma metadrenalines: Do they provide useful information about sympatho-adrenal function and catecholamine metabolism?. Clin. Sci. 88, 533–542 (1995).
Parasiliti-Caprino, M. et al. Association of urine metanephrine levels with cardiometabolic risk: An observational retrospective study. J. Clin. Med. 10, 1967 (2021).
von Elm, E. et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: Guidelines for reporting observational studies. J. Clin. Epidemiol. 61, 344–349 (2008).
Williams, B. et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur. Heart J. 39, 3021–3104 (2018).
Wilson, P. W. F. et al. Prediction of coronary heart disease using risk factor categories. Circulation 97, 1837–1847 (1998).
Palmieri, L. et al. La valutazione del rischio cardiovascolare globale assoluto: Il punteggio individuale del Progetto CUORE. Annali dell’Istituto Superiore di Sanità 40, 393–399 (2004).
Conroy, R. M. et al. Estimation of ten-year risk of fatal cardiovascular disease in Europe: The SCORE project. Eur. Heart J. 24, 987–1003 (2003).
Cleeman, J. I. Executive summary of the third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (adult treatment panel III). J. Am. Med. Assoc. 285, 2486–2497 (2001).
Parasiliti-Caprino, M. et al. Prevalence of primary aldosteronism and association with cardiovascular complications in patients with resistant and refractory hypertension. J. Hypertens. 38, 1841–1848 (2020).
Araujo-Castro, M. et al. Cardiometabolic profile of non-functioning and autonomous cortisol-secreting adrenal incidentalomas. Is the cardiometabolic risk similar or are there differences?. Endocrine 66, 650–659 (2019).
Morelli, V. et al. Long-term follow-up in adrenal incidentalomas: An Italian multicenter study. J. Clin. Endocrinol. Metab. 99, 827–834 (2014).
Di Dalmazi, G. et al. Cardiovascular events and mortality in patients with adrenal incidentalomas that are either non-secreting or associated with intermediate phenotype or subclinical Cushing’s syndrome: A 15-year retrospective study. Lancet Diabetes Endocrinol. 2, 396–405 (2014).
Elhassan, Y. S. et al. Natural history of adrenal incidentalomas with and without mild autonomous cortisol excess: A systematic review and meta-analysis. Ann. Intern. Med. 171, 107–116 (2019).
Akkus, G., Evran, M., Sert, M. & Tetiker, T. Adipocytokines in non-functional adrenal incidentalomas and relation with insulin resistance parameters. Endocr. Metab. Immune Disord. Drug Targets 19, 326–332 (2019).
RibeiroCavalari, E. M. et al. Nonfunctioning adrenal incidentaloma: A novel predictive factor for metabolic syndrome. Clin. Endocrinol. 89, 586–595 (2018).
Emral, R., Aydoğan, B. İ, Köse, A. D., Demir, Ö. & Çorapçıoğlu, D. Could a nonfunctional adrenal incidentaloma be a risk factor for increased carotid intima-media thickness and metabolic syndrome. Endocrinologia, diabetes y nutricion 66, 402–409 (2019).
Delibasi, T. et al. Circulating E-selectin levels and insulin resistance are associated with early stages of atherosclerosis in nonfunctional adrenal incidentaloma. Arch. Endocrinol. Metab. 59, 310–317 (2015).
Lopez, D. et al. “Nonfunctional” adrenal tumors and the risk for incident diabetes and cardiovascular outcomes: A cohort study. Ann. Intern. Med. 165, 533–542 (2016).
Moraes, A. B. et al. Evaluation of body composition using dual-energy X-ray absorptiometry in patients with non-functioning adrenal incidentalomas and an intermediate phenotype: Is there an association with metabolic syndrome?. J. Endocrinol. Investig. 42, 797–807 (2019).
Erbil, Y. et al. Cardiovascular risk in patients with nonfunctional adrenal incidentaloma: Myth or reality?. World J. Surg. 33, 2099–2105 (2009).
Araujo-Castro, M. Cardiometabolic profile and urinary metabolomic alterations in non-functioning adrenal incidentalomas: A review. Clin. Endocrinol. https://doi.org/10.1111/CEN.14745 (2022).
Babinska, A., Kaszubowski, M. & Sworczak, K. Adipokine and cytokine levels in non-functioning adrenal incidentalomas (NFAI). Endocr. J. 65, 849–858 (2018).
Tuna, M. M. et al. Non-functioning adrenal incidentalomas are associated with higher hypertension prevalence and higher risk of atherosclerosis. J. Endocrinol. Investig. 37, 765–768 (2014).
Akkan, T., Altay, M., Ünsal, Y., Dağdeviren, M. & Beyan, E. Nonfunctioning adrenal incidentaloma affecting central blood pressure and arterial stiffness parameters. Endocrine 58, 513–520 (2017).
Cansu, G. B., Sari, R., Yilmaz, N., Özdem, S. & Çubuk, M. Markers of subclinical cardiovascular disease in nonfunctional adrenal incidentaloma patients without traditional cardiovascular risk factors. Exp. Clin. Endocrinol. Diabetes 125, 57–63 (2017).
Imga, N. N. et al. Comparison of echocardiographic findings in patients with nonfunctioning adrenal incidentalomas. Kaohsiung J. Med. Sci. 33, 295–301 (2017).
Imga, N. N. et al. The relationship between increased epicardial fat thickness and left ventricular hypertrophy and carotid intima-media thickness in patients with nonfunctional adrenal incidentaloma. Int. J. Endocrinol. Metab. 14, e37635 (2016).
Sokmen, G. et al. Assessment of subclinical cardiac alterations and atrial electromechanical delay by tissue doppler echocardiography in patients with nonfunctioning adrenal incidentaloma. Arq. Bras. Cardiol. 111, 656–663 (2018).
Yener, S. et al. Carotid intima media thickness is increased and associated with morning cortisol in subjects with non-functioning adrenal incidentaloma. Endocrine 35, 365–370 (2009).
Evran, M. et al. Carotid intima-media thickness as the cardiometabolic risk indicator in patients with nonfunctional adrenal mass and metabolic syndrome screening. Med. Sci. Monit. 22, 991–997 (2016).
Akkus, O. et al. Increased rates of coronary artery calcium score in patients with non-functioning adrenal incidentaloma. Endocr. Metab. Immune Disord. Drug Targets 21, 1319–1325 (2021).
Peppa, M., Koliaki, C. & Raptis, S. A. Adrenal incidentalomas and cardiometabolic morbidity: An emerging association with serious clinical implications. J. Intern. Med. 268, 555–566 (2010).
Androulakis, I. I. et al. Patients with apparently nonfunctioning adrenal incidentalomas may be at increased cardiovascular risk due to excessive cortisol secretion. J. Clin. Endocrinol. Metab. 99, 2754–2762 (2014).
Di Dalmazi, G. et al. The steroid profile of adrenal incidentalomas: Subtyping subjects with high cardiovascular risk. J. Clin. Endocrinol. Metab. 104, 5519–5528 (2019).
Ehrhart-Bornstein, M., Hinson, J. P., Bornstein, S. R., Scherbaum, W. A. & Vinson, G. P. Intraadrenal interactions in the regulation of adrenocortical steroidogenesis. Endocr. Rev. 19, 101–143 (1998).
Bornstein, S. R., Berger, I., Scriba, L., Santambrogio, A. & Steenblock, C. Adrenal cortex–medulla interactions in adaptation to stress and disease. Curr. Opin. Endocr. Metab. Res. 8, 9–14 (2019).
Unsicker, K., Huber, K., Schober, A. & Kalcheim, C. Resolved and open issues in chromaffin cell development. Mech. Dev. 130, 324–329 (2013).
Haase, M., Willenberg, H. S. & Bornstein, S. R. Update on the corticomedullary interaction in the adrenal gland. Endocr. Dev. 20, 28–37 (2011).
Straznicky, N. E. et al. The effects of dietary weight loss on indices of norepinephrine turnover: Modulatory influence of hyperinsulinemia. Obesity 22, 652–662 (2014).
Lambert, E. A. et al. Effects of moxonidine and low-calorie diet: Cardiometabolic benefits from combination of both therapies. Obesity 25, 1894–1902 (2017).
Lohmeier, T. E. et al. Systemic and renal-specific sympathoinhibition in obesity hypertension. Hypertension 59, 331–338 (2012).
Katsurada, K. et al. Central glucagon-like peptide-1 receptor signaling via brainstem catecholamine neurons counteracts hypertension in spontaneously hypertensive rats. Sci. Rep. 9, 1–13 (2019).
Kobayashi, D. et al. Effect of pioglitazone on muscle sympathetic nerve activity in type 2 diabetes mellitus with alpha-glucosidase inhibitor. Autonomic Neurosci. Basic Clin. 158, 86–91 (2010).
Yokoe, H. et al. Effect of pioglitazone on arterial baroreflex sensitivity and sympathetic nerve activity in patients with acute myocardial infarction and type 2 diabetes mellitus. J. Cardiovasc. Pharmacol. 59, 563–569 (2012).
Lambert, E. A. et al. Obesity-associated organ damage and sympathetic nervous activity. Hypertension 73, 1150–1159 (2019).
Acknowledgements
We wish to acknowledge the European Reference Network for rare endocrine conditions (Endo-ERN), of which several authors of this publication are members (Project ID No. 739543).
Funding
This study did not receive any specific grant from any funding agency in the public, commercial or not-for-profit sector.
Author information
Authors and Affiliations
Contributions
Conceptualization: M.P.C., M.M. and R.G.; methodology: M.P.C., F.B. and F.P.; validation: I.G. and F.S.; resources: M.B., C.S. and M.C.D.C.; data curation: M.P.C., C.L. and C.S.; writing—original draft preparation: M.P.C. and C.S.; writing—review and editing: I.G. and F.S.; supervision: G.M. and E.G.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Parasiliti-Caprino, M., Lopez, C., Bollati, M. et al. A retrospective study on the association between urine metanephrines and cardiometabolic risk in patients with nonfunctioning adrenal incidentaloma. Sci Rep 12, 14913 (2022). https://doi.org/10.1038/s41598-022-19321-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-022-19321-2
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.