Abstract
Aim:
To explore the effects of noradrenaline (NA) on hepatic stellate cells (HSCs) in vitro and to determine the adrenoceptor (AR) subtypes and underlying mechanisms.
Methods:
The distribution and expressions of α1A-, α1B-, and α1D-ARs in HSC-T6 cells were analyzed using immunocytochemistry and RT-PCR. Cell proliferation was evaluated with MTT assay. The expression of HSC activation factors [transforming factor-β1 (TGF-β1) and α-smooth muscle actin (α-SMA)], extracellular matrix (ECM) secretion factors [tissue inhibitor of metalloproteinase-1 (TIMP-1) and collagen-Ι (ColΙ)] and PKC-PI3K-AKT signaling components (PKC, PI3K, and AKT) in the cells were detected by Western blotting and RT-PCR.
Results:
Both α1B- and α1D-AR were expressed in the membrane of HSC-T6 cells, whereas α1A-AR was not detected. Treatment of the cells with NA concentration-dependently increased cell proliferation (EC50=277 nmol/L), which was suppressed by the α1B-AR antagonist CEC or by the α1D-AR antagonist BMY7378. Furthermore, NA (0.001, 0.1, and 10 μmol/L) concentration-dependently increased the expression of TGF-β1, α-SMA, TIMP-1 and ColΙ, PKC and PI3K, and phosphorylation of AKT in HSC-T6 cells, which were suppressed by CEC or BMY7378, or by pertussis toxin (PT), RO-32-0432 (PKC antagonist), LY294002 (PI3K antagonist) or GSK690693 (AKT antagonist).
Conclusion:
NA promotes HSC-T6 cell activation, proliferation and secretion of ECM in vitro via activation of Gα-coupled α1B-AR and α1D-AR and the PKC-PI3K-AKT signaling pathway.
Similar content being viewed by others
Introduction
Liver fibrosis is a chronic liver damage caused by a variety of pathogenic factors1. It is a common pathology and a necessary step on the way to liver dysfunction and cirrhosis2. The mechanisms of pathogenesis are the excessive production and low degradation of extracellular matrix (ECM), which leads to ECM deposits in liver and the formation of liver fibrosis3. The HSC is the most important cell type involved in liver fibrosis4. The activation of hepatic stellate cells (HSCs) is central to liver fibrosis, whereas the apoptosis of HSCs can reverse liver fibrosis5.
The sympathetic nervous system (SNS) is widely distributed in the body and participates in the regulation of body functions6. Liver tissue is rich in autonomic nervous system (ANS) tissue, which is distributed around the Disse cavity7. Stoyanova8 showed that there are many autonomic nerve fibers in the hepatic portal area and hepatic lobule. HSCs express catecholamine biosynthetic enzymes and can synthesize and release noradrenaline (NA), dopamine, 5-hydroxytryptamine (5-HT) and other neurotransmitters9. Studies have shown that liver fibrogenesis requires sympathetic neurotransmitters10 and that SNS blockers significantly reduce liver fibrosis11. Numerous evidence is available showing that excessive activation of the SNS is related to the occurrence and development of liver fibrosis12.
Previous studies have indicated that NA promotes the proliferation of HSCs. The non-selective α-AR and β-AR antagonists inhibit the growth of HSCs13. We investigated the expression of 3 AR subtypes of α1-AR in the hepatic stellate cell-T6 (HSC-T6) cell line. We explored the effects of NA on HSCs, the AR subtypes through which NA plays a role and the possible mechanisms through which NA acts on HSCs.
Materials and methods
Drugs and reagents
NA bitartrate was purchased from Harvest (Shanghai, China). The α1B-AR selective antagonist chloroethylclonidine (CEC), the α1D-AR selective antagonist BMY7378 and the PI3K antagonist LY294002 were purchased from Sigma (St Louis, MO, USA)14. Gα protein antagonist pertussis toxin (PT) was purchased from Calbiochem (Darmstadt, Hesse, Germany). The PKC antagonist RO-32-0432 and α1A-AR, α1B-AR and α1D-AR primary antibodies were purchased from Santa Cruz Biotechnology Inc (Santa Cruz, CA, USA). The AKT antagonist GSK690693 was purchased from Selleckchem (Houston, TX, USA). SABC three-step kit was purchased from Boster (Wuhan, China). Other primary antibodies were purchased from Cell signaling (Boston, MA, USA). Primers were synthesized by Sangon Biotech Co, Ltd (Shanghai, China) (Table 1)15,16,17.
Cell culture
The HSC-T6 cell line was obtained from the Institute of Clinical Pharmacology, Anhui Medical University. The cells were cultured at 37 °C in 5% CO2 in Dulbecco's modified Eagle's medium (DMEM) from Gibco BRL Life Technologies Inc (Grand Island, NY, USA) supplemented with 10% fetal bovine serum (FBS) (Sigma, St Louis, MO, USA).
Experimental groups and drug delivery
Cultured HSC-T6 cells were divided into 13 groups: Control group; NA (10−4, 10−5, 10−6, 10−7, 10−8, and 10−9 mol/L) groups; α1B-AR antagonist (CEC) group; α1D-AR antagonist (BMY7378) group; Gα protein inhibitor (PT) group; PKC inhibitor (RO-32-0432) group; PI3K inhibitor (LY294002) group and AKT inhibitor (GSK690693) group. HSC-T6 cells in an exponential growth phase were cultured at a density of 5×104 cells/well in a 96-well plate for 3-(4,5-dimethyl-2-thiazolyl)-2,5-diphenyl-2-H-tetrazolium bromide (MTT) or 1×105 cells/well in a 6-well plate for immunocytochemistry, Western blot and reverse transcription-polymerase chain reaction (RT-PCR). The cells were incubated overnight in DMEM containing 10% FBS then starved for serum 24 h before being treated with the compounds. HSC-T6 cells were incubated with α1B-AR and α1D-AR antagonists and with Gα protein, protein kinase C (PKC), phosphatidylinositol 3-kinase (PI3K) and AKT inhibitors (1×10−5 mol/L) for 12 h. NA at different concentrations was then added to cells for 24 h at 37 °C.
Immunocytochemistry
The cells were cultured in 6-well plates containing cover slips. The cover slips were washed twice with phosphate buffered saline (PBS) and fixed in 4% paraformaldehyde for 20 min. Immunohistochemical staining for α1A-AR, α1B-AR, and α1D-AR were performed according to the standard SABC protocol described in the SABC Reagents Kit (Boster, Wuhan, China). Positive expression was detected as brown or yellow staining. PBS was used as a negative control to replace the primary antibodies.
Cell proliferation assay
Plated HSC-T6 cells were cultured in the presence or absence of α1B-AR antagonist CEC (10−5 mol/L) or α1D-AR antagonist BMY7378 (10−5 mol/L) for 12 h. Various concentrations of NA were then added18,19. Proliferation was measured with MTT assay (Sigma, St Louis, MO, USA) to determine the effects of NA with or without α1B-AR and α1D-AR antagonists on cell proliferation. After treatment, MTT solution (5.0 mg/mL in PBS) was added (20.0 μL/well), and the plates were incubated for another 4 h at 37 °C. The purple formazan crystals were dissolved in 150.0 μL of dimethyl sulfoxide (DMSO) per well. After 10 min, the plates were read on a microplate reader (Biotech Instruments, NY, USA) at an absorbance of 490 nm. Untreated cells were used as a control. The assays were performed in three independent experiments. The cell proliferation was calculated using the following formula: cell proliferation (%)=[(OD of the experimental samples/OD of the control)–1] ×100% (n=3, mean±SD).
Western blot analysis
Proteins were extracted from cells treated with NA in the presence or absence of α1B-AR or α1D-AR antagonists and signaling pathway molecule inhibitors using RIPA lysis buffer (Beyotime, Haimen, China) and phenylmethylsulfonyl fluoride (PMSF) (99:1). Each protein sample was mixed with 5× sample buffer (4:1) (Bio-Rad, Hercules, CA, USA) and heated in boiling water for 10 min. The proteins were separated by 12.5% sodium dodecylsulfate-polyacrylamide gel electrophoresis (SDS-PAGE), transferred to polyvinylidene fluoride (PVDF) membranes (Millipore, Bedford, MA, USA), and incubated overnight at 4 °C with various primary antibodies at a 1:500 dilution. The secondary antibody [peroxidase (HRP)-labeled goat anti-mouse or goat anti-rabbit] was added and incubated at 1:30 000 dilution. Immunodetection was performed with an enhanced chemiluminescence system (ECL, Pierce, Rockford, IL, USA) using hydrogen peroxide and luminol as a substrate.
RT-PCR
Total RNA was extracted from HSC-T6 cells using TRIzol reagent (Invitrogen, CA, USA) according to the manufacturer's protocol. The integrity and concentration of RNA were determined by measuring absorbance at 260 nm and total RNA was stored at −80 °C. RNA was separated for RT-PCR by agarose gel electrophoresis (Thermo, MA, USA). Total RNA from each sample (2 μg) was re-suspended in a final volume of 25 μL of reaction buffer. PCR for GAPDH was performed on each individual sample as an internal control. The PCR conditions were 95 °C for 5 min, followed by 35 cycles of 95 °C for 5 s, 40–60 °C for 30 s and 72 °C for 30 s. After the last cycle of amplification, samples were incubated for 10 min at 72 °C. The amplified RT-PCR products were subjected to electrophoresis at 85 V on 2% agarose gels (Sigma, St Louis, MO, USA) for 30 min. A DNA ladder was used as a molecular marker. Agarose gels were stained with 0.5 mg/mL ethidium bromide (Sigma, St Louis, MO, USA) in TAE buffer. The gel bands were examined using the gel image system (Tanon, Shanghai, China).
Statistical analysis
Statistical analyses were performed using the SPSS 11.0 software program (SPSS Software Products, Chicago, IL, USA). All data are presented as number or mean±SD. Statistical analysis among groups was performed by one-way analysis of variance (ANOVA). Statistical analysis between two groups was performed using Dunnett′s method. The Bliss20 method was used to determine the linear regression equation to calculate EC50. The threshold for statistical significance of differences was P<0.05.
Results
The expression of α1A-AR, α1B-AR, and α1D-AR in HSC-T6 cells
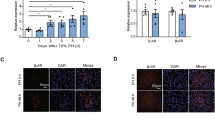
The SABC method was used to determine the expression of α1A-AR, α1B-AR, and α1D-AR. α1B-AR and α1D-AR were expressed in the membrane, but α1A-AR was almost undetectable (Figure 1A and 1B). We then measured the expression of α1A-AR, α1B-AR, and α1D-AR mRNA. α1B-AR was expressed at a higher level than α1D-AR (P<0.05), and α1A-AR was not expressed (Figure 1C and 1D).
The expression of α1A-AR, α1B-AR, and α1D-AR in HSC-T6 cells. (A) The expression of α1-AR subtypes in HSC-T6 was analyzed using the SABC method. (B) Bar graphs showed semi-quantitative analysis of their expression. (C) α1-AR subtype mRNA was analyzed by RT-PCR. GAPDH was used as internal control. (D) Bar graphs showed semi-quantitative analysis of α1-ARs expression. Data are presented as the mean±SD (n=3). bP<0.05 α1B-AR group compared with the α1D-AR group.
NA promotes HSC-T6 cell proliferation and adrenoceptor antagonists reduce HSC-T6 cell proliferation
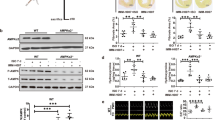
We plated HSC-T6 cells in the presence and absence of α1B-AR antagonist CEC (10 μmol/L) or α1D-AR antagonist BMY7378 (10 μmol/L) for 12 h and then added various concentrations of NA. Using the MTT assay to measure the proliferation of HSC-T6 cells, we found that NA significantly induced HSC-T6 cell proliferation in a concentration-dependent manner compared with the control group (P<0.05) (Figure 2A). The EC50 was 277 nmol/L (Figure 2B). The α1B-AR antagonist CEC and the α1D-AR antagonist BMY7378 both reduced HSC-T6 cell proliferation compared with the equivalent concentration of NA only (P<0.01) (Figure 2A). The α1B-AR antagonist may be a competitive antagonist and the α1D-AR antagonist may be a noncompetitive antagonist, because the HSC proliferation curve moved to the right when the cells were cultured with the α1B-AR antagonist. With an increased concentration of NA, the curve did not reach the original Emax. However, the HSC cell proliferation curve moved in parallel to the right when the cells were cultured with the α1D-AR antagonist. With an increased concentration of NA, the curve reached the original Emax (Figure 2C).
The selective α-AR agonist NA promoted HSC-T6 cell proliferation and the α1B-AR antagonist CEC and the α1D-AR antagonist BMY7378 inhibited the growth of HSC-T6 cells. (A) NA promoted HSC-T6 cell proliferation and adrenoceptor antagonists inhibited the growth of HSC-T6 cells. Data are presented as the mean±SD (n=3). bP<0.05, cP<0.01 compared with the control group. fP<0.01 compared with the corresponding concentration of NA. (B) Using logarithmic NA concentration as the X-axis and cell proliferation rate as the Y-axis to perform linear regression, the regression equation is y=0.1933x+1.7675, R2=0.9722. There was an obvious linear relationship. The EC50 of NA was 277 nmol/L. (C) The concentration-effect curve of NA and α1-AR antagonists on HSC-T6 cell proliferation.
NA promotes the expression of TGF-β1, α-SMA, TIMP-1, PKC, and PI3K protein and the phosphorylation of AKT but α1-AR antagonists inhibit their expressions in HSC-T6 cells
To explore the effects and possible mechanisms of action of NA and α1-AR antagonists on HSC-T6 cells, and to explore the function of the PKC-PI3K-AKT signaling pathway, we measured the expression of HSC activation factors (TGF-β1 and α-SMA), ECM secretion factors (TIMP-1) and PKC-PI3K-AKT signaling pathway molecules (PKC, PI3K, and AKT) in HSC-T6 cells after treatment with NA with or without α1-AR antagonists. The results showed that NA significantly promoted the expression of TGF-β1, α-SMA, TIMP-1, PKC, PI3K protein and the phosphorylation of AKT in HSC-T6 cells (P<0.05). The α1B-AR and α1D-AR antagonists significantly inhibited their expression (P<0.05) (Figure 3 and 4).
α1-AR antagonists down-regulated the protein expression of TGF-β1, α-SMA, TIMP-1, PKC, and PI3K in NA treated HSC-T6 cells. (A) Western blot results showed the expression of these proteins in HSC-T6 cells. β-Actin was used as a loading control. (B) Bar graphs showed semi-quantitative evaluation of their expression by densitometry from triplicate independent experiments. Mean±SD. bP<0.05, cP<0.01 compared with the control group. eP<0.05, fP<0.01 compared with the 0.1 μmol/L NA group.
α1-AR antagonists down-regulated the phosphorylation of AKT in NA treated HSC-T6 cells. (A) Western blot results showed the expression of AKT and p-AKT in HSC-T6 cells. β-Actin was used as a loading control. (B) Bar graphs showed semi-quantitative analysis of their expression by densitometry from triplicate independent experiments. (C) Bar graph shows p-AKT/AKT ratio. Mean±SD. cP<0.01 compared with the control group. eP<0.05, fP<0.01 compared with the 0.1 μmol/L NA group.
NA promotes TGF-β1, TIMP-1, ColΙ, and PI3K mRNA expression and α1-AR antagonists inhibits their expressions in HSC-T6 cells
The results of RT-PCR showed that NA significantly promoted the mRNA expression of HSC activation factor TGF-β1, ECM secretion factor TIMP-1 and ColI and PKC-PI3K-AKT signaling pathway molecule PI3K in HSC-T6 cells. These results indicate that NA significantly increased their expression (P<0.01). The α1B-AR and α1D-AR antagonists significantly inhibited their expression (P<0.05) (Figure 5).
α1-AR antagonists down-regulated the mRNA expression of TGF-β1, ColI, TIMP-1 and PI3K in NA treated HSC-T6 cells. (A) RT-PCR results showed the expression levels of them in HSC-T6 cells. GAPDH was used as an internal control. (B) Bar graphs showed semi-quantitative analysis of their expression by densitometry from triplicate independent experiments. Mean±SD. cP<0.01 compared with the control group. eP<0.05, fP<0.01 compared with the 0.1 μmol/L NA group.
Gα, PKC, PI3K, and AKT inhibitors down-regulate the protein expression of TGF-β1, α-SMA, and TIMP-1 in NA treated HSC-T6 cells
To explore the mechanisms of the effect of NA on HSC-T6 cells, we plated HSC-T6 cells in the presence and absence of various inhibitors for 12 h. NA was then added, and the expression of TGF-β1, α-SMA, and TIMP-1 was measured. The results showed that NA significantly increased TGF-β1, α-SMA, and TIMP-1 protein expressions in HSC-T6 cells (P<0.01). Various inhibitors significantly inhibited their expression (P<0.01) (Figure 6).
Gα, PKC, PI3K and AKT inhibitors down-regulated the protein expression of TGF-β1, α-SMA, and TIMP-1 in NA treated HSC-T6 cells. (A) Western blot results showed their expression in HSC-T6 cells. β-Actin was used as a loading control. (B) Bar graphs showed semi-quantitative analysis of their expression by densitometry from triplicate independent experiments. Mean±SD. cP<0.01 compared with the control group; fP<0.01 compared with the 0.1 μmol/L NA group.
Gα, PKC, PI3K, and AKT inhibitors down-regulate the mRNA expression of TGF-β1, TIMP-1, and ColΙ in NA treated HSC-T6 cells
The RT-PCR results showed that NA significantly increased TGF-β1, α-SMA, and TIMP-1 mRNA expression in HSC-T6 cells (P<0.05). Various inhibitors significantly inhibited their expression (P<0.05) (Figure 7).
Gα, PKC, PI3K, and AKT inhibitors down-regulated the mRNA expression of TGF-β1, ColΙ, and TIMP-1 in NA treated HSC-T6 cells. (A) RT-PCR results showed their expression in HSC-T6 cells. GAPDH was used as an internal control. (B) Bar graphs showed semi-quantitative analysis of their expression by densitometry from triplicate independent experiments. Mean±SD. bP<0.05, cP<0.01 compared with the control group. eP<0.05, fP<0.01 compared with the 0.1 μmol/L NA group.
Discussion
Studies have shown that the SNS is involved in regulation in the liver and plays an important role in the development of liver fibrosis. The HSC could be the target of SNS regulation21. Oben et al11 suggested that leptin deficient ob/ob mice have the characteristic of fibrosis resistance in chronic liver injury, because the expression of NA is low and the activation of the SNS is suppressed in these mice. Drugs that have effects on the SNS may provide new strategies for the clinical treatment of liver fibrosis. We are interested in understanding the effects and mechanisms of SNS action on HSC cells and determining the AR subtypes that play a role in this process. We are interested in finding alternative therapeutic targets to increase drug effectiveness and reduce adverse reactions.
Studies have suggested that sympathetic nerve neurotransmitters promote the repair of liver injuries. They also promote the activation of HSCs by coupling with ARs22. Sancho-Bru et al23 confirmed that liver tissue expressed α1A-AR, α1B-AR, α2A-AR, α2B-AR, β1-AR, and β2-AR. HSCs also express a variety of adrenoceptor subtypes such as α1A-AR, α2B-AR and β2-AR. However, Oben et al18 showed that HSCs express α1B-AR, α1D-AR, β1-AR, and β2-AR. Currently, the distribution and function of adrenoceptor subtypes in liver tissue and HSCs are controversial and need further research. Our study examined this issue further, and we observed the expression of three α1-AR subtypes (α1A-AR, α1B-AR, and α1D-AR) in HSCs. We found that α1B-AR and α1D-AR are expressed in cell membranes but α1A-AR not. Previous studies have shown that NA promotes HSC proliferation and inhibits apoptosis in vitro, mainly through α-AR and β2-AR13. Other results suggested that α1-AR and β2-AR expression increased in the liver tissue of rats with liver fibrosis24. Duan et al25 also suggested that NA, α1-AR, and β2-AR were more highly expressed in rat liver tissue with liver fibrosis. α1-AR plays important roles in many physiological processes26. We studied the various subtypes of α1-AR to further define the mechanism of action of the SNS in the development of liver fibrosis. The results showed that blocking either α1B-AR or α1D-AR down-regulated the activation, proliferation and secretion of NA treated HSC cells.
The SNS acts through neurotransmitters interacting with different adrenoceptor subtypes, and then activating downstream signaling pathways. α-AR can activate multiple signaling pathways including the phosphoinositide-calcium signaling system, and the PKC signaling system. β-AR can activate the G protein-cAMP-PKA signaling system. Various receptor subtypes also have different characteristics in coupling with G protein. α1-AR couples with Gαq protein and α2-AR couples with Gαi protein. β1-AR only couples with Gαs protein but β2-AR couples with Gαs and Gαi proteins27.
Studies of heart failure have found that SNS regulates the apoptosis of myocardial cells through β-AR coupling with G protein28. β1-AR promoted apoptosis through the mitogen activated protein kinase (MAPK) signaling pathway and β2-AR inhibited apoptosis through the PI3K signaling pathway29. The PI3K signaling pathway is important in cell proliferation30. Studies of this pathway are important for elucidating the mechanisms of action of the SNS in the development of liver fibrosis. We would like to identify new methods for the effective treatment of liver fibrosis.
The PKC-PI3K-AKT signaling pathway regulates platelet derivation growth factor (PDGF) to promote HSC proliferation and secretion31. Blocking this pathway can inhibit HSC proliferation and ECM expression, leading to an improvement in patients with liver fibrosis32. Marra et al33 showed that the activation of the PKC-PI3K-AKT signaling pathways promoted the mitosis and chemotaxis of HSC cells. Our experiments studied the PKC-PI3K-AKT signaling pathway in depth. We measured the expression of signaling molecules as well as HSC activation and secretion in the presence of a variety of signaling molecules inhibitors. This research illuminated the function of the PKC-PI3K-AKT signaling pathway in liver fibrosis. Blocking this pathway can down-regulate the activity of NA on HSCs.
Previous experiments have shown that NA promotes HSC proliferation34. We demonstrated this action by MTT and performed further experiments. We found that NA promoted the proliferation of HSCs in a concentration-dependence manner. The EC50 was 277 nmol/L. Understanding the EC50 of drugs is important in guiding clinical use of the drug. And 277 nmol/L is approximately 10−7 mol/L. In our experiments, we used 10−7 mol/L of NA in co-culture with antagonists or inhibitors to study the effect of NA on HSCs after blocking receptors or signaling pathways. Based on the concentration-effect curves, we demonstrated that the α1D-AR antagonist is competitive and the α1B-AR antagonist is noncompetitive in HSCs. In addition to HSC proliferation, our experiments studied the activation and secretion of HSC-T6 cells. The results showed that NA promoted the activation and secretion of HSC-T6 cells and that the selective α1B-AR and α1D-AR antagonists and the inhibitors of PKC-PI3K-AKT signaling pathways down-regulated the effect of NA.
In conclusion, our study demonstrated that, through α1B-AR and α1D-AR, NA activates Gα protein coupling with the PKC-PI3K-AKT signaling pathway, which might be one of the mechanisms to promote HSC-T6 activation, proliferation and secretion of ECM.
Author contribution
Yong MA and Wei WEI designed the experiments; Ti-long DING guided the research; and Ting-ting LIU performed experiments, analyzed data and wrote the paper.
References
Yi ET, Liu RX, Wen Y, Yin CH . Telmisartan attenuates hepatic fibrosis in bile duct-ligated rats. Acta Pharmacol Sin 2012; 33: 1518–24.
Moreno M, Gonzalo T, Kok RJ, Sancho-Bru P, van Beuge M, Swart J, et al. Reduction of advanced liver fibrosis by short-term targeted delivery of an angiotensin receptor blocker to hepatic stellate cells in rats. Hepatology 2010; 51: 942–52.
Gong Y . Identifying the targets for treatment of liver fibrosis and hepatocellular carcinoma from both Western medicine and Chinese medicine. Chin J Integr Med 2012; 18: 245–9.
Liu Q, Wang X, Zhang Y, Li CJ, Hu LH, Shen X . Leukamenin F suppresses liver fibrogenesis by inhibiting both hepatic stellate cell proliferation and extracellular matrix production. Acta Pharmacol Sin 2010; 31: 839–48.
Xu C, Chen X, Chang C, Wang G, Wang W, Zhang L, et al. Analysis of gene expression profiles of liver stellate cells during liver regeneration in rats. Mol Cells 2011; 31: 17–23.
Mancia G, Bousquet P, Elghozi JL, Esler M, Grassi G, Julius S, et al. The sympathetic nervous system and the metabolic syndrome. J Hypertens 2007; 25: 909–20.
Fukuda Y, Imoto M, Koyama Y, Miyazawa Y, Hayakawa T . Demonstration of noradrenaline-immunoreactive nerve fibres in the liver. J Int Med Res 1996; 24: 466–72.
Stoyanova II . Relevance of mast cells and hepatic lobule innervation to liver injury. Rom J Gastroenterol 2004; 13: 203–9.
Tian XP, Zhang XL . Sympathetic nervous system in pathogenesis of hepatic fibrosis. Int J Dig Dis 2008; 28: 323–5.
Dubuisson L, Desmoulière A, Decourt B, Evadé L, Bedin C, Boussarie L, et al. Inhibition of rat liver fibrogenesis through noradrenergic antagonism. Hepatology 2002; 35: 325–31.
Oben JA, Roskams T, Yang S, Lin H, Sinelli N, Li Z, et al. Norepinephrine induces hepatic fibrogenesis in leptin deficient ob/ob mice. Biochem Biophys Res Commun 2003; 308: 284–92.
Timmermans JP, Geerts A . Nerves in liver: superfluous structures? A special issue of The Anatomical Record updating our views on hepatic innervation. Anat Rec B New Anat 2005; 282: 4.
Liu N, Zhang XL, Liang CD, Yao DM, Liu L, Zhao DQ, et al. Dynamic changes of α-AR, β1-AR, and β2-AR expression during hepatic fibrogenesis. Chin J Hepatol 2009; 17: 653–6.
Koshimizu TA, Tanoue A, Hirasawa A, Yamauchi J, Tsujimoto G . Recent advances in α1-adrenoceptor pharmacology. Pharmacol Ther 2003; 98: 235–44.
Knittel T, Aurisch S, Neubauer K, Eichhorst S, Ramadori G . Cell-type-specific expression of neural cell adhesion molecule (N-CAM) in Ito cells of rat. Am J Pathol 1996; 149: 449–62.
Sun DX, Liu Z, Tan XD, Cui DX, Wang BS, Dai XW . Nanoparticle-mediated local delivery of an antisense TGF-β1 construct inhibits intimal hyperplasia in autogenous vein grafts in rats. PLoS One 2012; 7: e 41857.
Dun ZN, Zhang XL, An JY, Zheng LB, Barrett R, Xie SR . Specific shRNA targeting of FAK influenced collagen metabolism in rat hepatic stellate cells. World J Gastroenterol 2010; 16: 4100–6.
Oben JA, Roskams T, Yang S, Lin H, Sinelli N, Torbenson M . Hepatic fibrogenesis requires sympathetic neurotransmitters. Gut 2004; 53: 438–45.
Hansel DE, Eipper BA, Ronnett GV . Neuropeptide Y functions as a neuroproliferative factor. Nature 2001; 410: 940–4.
Liu CX, Sun RY . Drug evaluation experiment design and statistical basis. Beijing: Military Medical Science Press, 1999. p 84–6.
Püschel GP . Control of hepatocyte metabolism by sympathetic and parasympathetic hepatic nerves. Anat Rec A Discov Mol Cell Evol Biol 2004; 280: 854–67.
Van Heeswijk JC, Vianen GJ, van den Thillart GE . The adrenergic control of hepatic glucose and FFA metabolism in rainbow trout (Oncorhynchus mykiss): increased sensitivity to adrenergic stimulation with fasting. Gen Comp Endocrinol 2006; 145: 51–61.
Sancho-Bru P, Bataller R, Colmenero J, Gasull X, Moreno M, Arroyo V, et al. Norepinephrine induces calcium spikes and proinflammatory actions in human hepatic stellate cells. Am J Physiol Gastrointest Liver Physiol 2006; 291: G877–84.
Zapater P, Gómez-Hurtado I, Peiró G, González-Navajas JM, García I, Giménez P, et al. Beta-adrenergic receptor 1 selective antagonism inhibits norepinephrine-mediated TNF-alpha downregulation in experimental liver cirrhosis. PLoS One 2012; 7: e 43371.
Duan RX, Tang WX, Wu CH, Liu HY, Gao X, Guo Y, et al. The effects of sympathetic neurotransmitters and adrenergic receptors on liver fibrosis in murine schistosomiasis. Zhonghua Gan Zang Bing Za Zhi 2008; 16: 352–4.
Docherty JR . Subtypes of functional alpha1-adrenoceptor. Cell Mol Life Sci 2010; 67: 405–17.
Xiao RP, Avdonin P, Zhou YY, Cheng H, Akhter SA, Eschenhagen T, et al. Coupling of β2-adrenoceptor to Gi proteins and its physiological relevance in murine cardiac myocytes. Circ Res 1999; 84: 43–52.
Remondino A, Kwon SH, Communal C, Pimentel DR, Sawyer DB, Singh K, et al. β-Adrenergic receptor-stimulated apoptosis in cardiac myocytes is mediated by reactive oxygen species/c-Jun NH2-terminal kinase-dependent activation of the mitochondrial pathway. Circ Res 2003; 92: 136–8.
Hakuno D, Fukuda K, Makino S, Konishi F, Tomita Y, Manabe T, et al. Bone marrew-derived regenerated cardiomyocytes (CMG cells) express functional adrenergic and musearinic receptors. Circulation 2002; 105: 380–6.
Zhai YP, Lu Q, Liu YW, Cheng Q, Wei YQ, Zhang F, et al. Over-production of nitric oxide by oxidative stress-induced activation of the TGF-β1/PI3K/Akt pathway in mesangial cells cultured in high glucose. Acta Pharmacol Sin 2013; 34: 507–14.
Jones SM, Kazlauskas A . Growth-factor-dependent mitogenesis requires two distinct phases of signaling. Nat Cell Biol 2001; 3: 165–72.
Parsons CJ, Takashima M, Rippe RA . Molecular mechanisms of hepatic fibrogenesis. J Gastroenterol Hepatol 2007; 22: S79–84.
Marra F, Romanelli RG, Giannini C, Failli P, Pastacaldi S, Arrighi MC, et al. Monocyte chemotactic protein-1 as a chemoattractant for human hepatic stellate cells. Hepatology 1999; 29: 140–8.
Oben JA, Yang S, Lin H, Ono M, Diehl AM . Norepinephrine and neuropeptide Y promote proliferation and collagen gene expression of hepatic myofibroblastic stellate cells. Biochem Biophys Res Commun 2003; 302: 685–90.
Acknowledgements
This study was supported by the National Natural Science Foundation of China (No 81173075) and the Nanjing Military Medical Science and Technology Innovation Foundation of China (No 10MA037).
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Liu, Tt., Ding, Tl., Ma, Y. et al. Selective α1B- and α1D-adrenoceptor antagonists suppress noradrenaline-induced activation, proliferation and ECM secretion of rat hepatic stellate cells in vitro. Acta Pharmacol Sin 35, 1385–1392 (2014). https://doi.org/10.1038/aps.2014.84
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/aps.2014.84
Keywords
This article is cited by
-
Norepinephrine-stimulated HSCs secrete sFRP1 to promote HCC progression following chronic stress via augmentation of a Wnt16B/β-catenin positive feedback loop
Journal of Experimental & Clinical Cancer Research (2020)
-
Interaction of dendritic cells and T lymphocytes for the therapeutic effect of Dangguiliuhuang decoction to autoimmune diabetes
Scientific Reports (2015)