Abstract
Apoptosis-inducing factor (AIF), a flavoprotein with NADH oxidase activity anchored to the mitochondrial inner membrane, is known to be involved in complex I maintenance. During apoptosis, AIF can be released from mitochondria and translocate to the nucleus, where it participates in chromatin condensation and large-scale DNA fragmentation. The mechanism of AIF release is not fully understood. Here, we show that a prolonged (∼10 min) increase in intracellular Ca2+ level is a prerequisite step for AIF processing and release during cell death. In contrast, a transient ATP-induced Ca2+ increase, followed by rapid normalization of the Ca2+ level, was not sufficient to trigger the proteolysis of AIF. Hence, import of extracellular Ca2+ into staurosporine-treated cells caused the activation of a calpain, located in the intermembrane space of mitochondria. The activated calpain, in turn, cleaved membrane-bound AIF, and the soluble fragment was released from the mitochondria upon outer membrane permeabilization through Bax/Bak-mediated pores or by the induction of Ca2+-dependent mitochondrial permeability transition. Inhibition of calpain, or chelation of Ca2+, but not the suppression of caspase activity, prevented processing and release of AIF. Combined, these results provide novel insights into the mechanism of AIF release during cell death.
Similar content being viewed by others
Main
Apoptosis, a genetically controlled mode of cell death, is of critical importance for embryogenesis and maintenance of tissue homeostasis in the adult organism and is also important for the removal of potentially dangerous cells, for example precursor tumor cells.1 Apoptosis is characterized by various morphological features, such as shrinkage of the cell nucleus and condensation and fragmentation of chromosomal DNA.2 A key event in apoptotic signaling is the release of proapoptotic proteins, for example cytochrome c, apoptosis-inducing factor (AIF), Smac/DIABLO and Omi/HtrA2, from the mitochondrial intermembrane space (IMS). Being released, these proteins can promote apoptosis through the activation of both caspase-dependent and caspase-independent pathways. Cytochrome c, together with Apaf-1, dATP and procaspase-9, forms the apoptosome complex in the cytosol, leading to autocatalytic activation of procaspase-9 and initiation of a downstream caspase cascade. In contrast to cytochrome c, AIF is a caspase-independent death effector; after release, it translocates to the nucleus where it participates in chromatin condensation and large-scale DNA fragmentation.3, 4, 5, 6, 7, 8, 9 Release of AIF from the mitochondria can be induced by various stimuli, including toxic concentrations of glutamate, oxidative stress, hypoxia or ischemia. However, Hsp70 can antagonize AIF translocation to the nucleus by sequestering AIF in the cytosol.10
Deregulation of apoptosis contributes to the development of cancer, as well as to tumor resistance to treatment with anticancer agents. For example, non-small-cell lung carcinomas (NSCLCs) are resistant to both drug- and radiation-induced apoptosis. We have reported earlier that malfunction of AIF release from mitochondria is essential for the chemoresistance of U1810 NSCLC cells, as the activation of caspases alone was not sufficient to kill these cells.11, 12, 13 However, we also found that staurosporine (STS) can reactivate the full apoptotic machinery in U1810 cells. This suggests an important function for the AIF-mediated cell death pathway in NSCLCs.
AIF is a flavoprotein that is anchored to the mitochondrial inner membrane, where it exerts NADH oxidase activity. The flavine adenine nucleotide (FAD) domain is required for the redox activity of AIF, but it does not contribute to its apoptotic activity. Hence, it has been shown that chemical inactivation of the FAD domain, or mutations within the FAD-binding site, did not restrain the apoptotic function of AIF.14, 15, 16, 17 Human AIF is synthesized as a 67 kDa protein with an extension in the N-terminal domain containing a mitochondrial localization signal. Once imported into mitochondria, AIF is processed to the mature 65-kDa form and is N-terminally anchored to the inner mitochondrial membrane. During apoptosis, AIF is further processed and released into the cytosol as a 57 kDa soluble protein.7, 18, 19 Several proteases have been proposed to cleave AIF, including Ca2+-dependent calpains and Ca2+-independent cathepsins B, L and S.20, 21 However, the mechanism by which AIF becomes processed and released from mitochondria during apoptosis is not entirely understood. Here, we report that Ca2+ import from the extracellular store is required for AIF release during cell death. The resultant increase in Ca2+ concentration is sufficient to activate a mitochondrial calpain in the IMS, which can process AIF to generate the releasable fragment.
Results
AIF is processed and released from mitochondria in the presence of Ca2+
Release of proapoptotic proteins from mitochondria requires permeabilization of the outer mitochondrial membrane (OMM). It is known that AIF has to be processed before its release into the cytosol; therefore, one might expect that its release should be delayed in time as compared with the release of a free pool of cytochrome c. Thus, we decided to monitor the release of AIF and cytochrome c upon permeabilization of the OMM. To this end, U1810 cells with digitonin-permeabilized plasma membrane were incubated with 0.5 mM Ca2+ in the presence of succinate, a substrate for mitochondrial respiration, and the induction of mitochondrial permeability transition (MPT) was monitored using a Ca2+-sensitive electrode (Figure 1a). Addition of Ca2+ to U1810 cells resulted in the accumulation of this ion in the mitochondria followed by its release upon induction of MPT. Western blot analysis of samples collected at different time points after MPT induction showed that AIF was processed and released from mitochondria in the presence of Ca2+. The release of the soluble fragment of AIF into the cytosol occurred in a time-dependent manner, whereas the amount of cytochrome c present in the cytosol reached a plateau as soon as 15 min after addition of Ca2+ (Figure 1b). A quantification of these data is presented in Figure 1c. This shows that AIF is cleaved in a Ca2+-dependent manner before being released from mitochondria. It is of interest to note that similar results were obtained using HEK293 hepatoma cells and SH-SY5Y neuroblastoma cells (data not shown).
The release of AIF and cytochrome c from mitochondria upon Ca2+-stimulated MPT induction. (a) Cells were permeabilized with digitonin, 0.5 mM CaCl2 was added and the induction of MPT was monitored with a Ca2+-sensitive electrode. (b) Permeabilized U1810 cells were incubated for different time periods after MPT was induced. The control sample was taken before Ca2+ addition. Immunoblots show the distribution of AIF and cytochrome c in mitochondria (pellet) and cytosol (supernatant). (c) Quantification of the amount of released proteins from (b)
AIF is processed by mitochondrial calpain
It has been reported that both calpain and cathepsins can cleave AIF.20, 21, 22 In the case of calpain, the subcellular localization of the enzyme responsible for AIF cleavage is not known. Although both m- and μ-calpains are generally considered to be cytosolic, mitochondria were also shown to contain Ca2+-dependent calpain 1.23 To investigate whether AIF can be processed by a mitochondrial protease, we used several independent approaches. First, a sucrose gradient purification of mitochondria from U1810 cells was performed to exclude the presence of non-mitochondrial proteases. The purity of the mitochondrial fraction was confirmed by the absence of nuclear and cytosolic contaminants using antibodies against lamin B and actin, respectively. The addition of Ca2+ stimulated AIF proteolysis, indicating that an intramitochondrial Ca2+-activated protease is involved (Figure 2a). Further analysis identified this protease as calpain I (Figure 2b). Importantly, the endogenous inhibitor of calpains, calpastatin, was not detected in the mitochondrial fraction (Figure 2b).
AIF is cleaved by mitochondrial calpain. (a) Purified mitochondria from U1810 cells were incubated in the presence or absence of 0.5 mM CaCl2 in SHKCl buffer. Mitochondrial lysates were analyzed by western blotting. The lack of nuclear and cytosolic contamination was confirmed by reprobing the membrane with antibodies against lamin B (nucleus) and actin (cytosol). (b) Total and mitochondrial lysates were analyzed for the presence of calpain I and calpastatin. (c) Permeabilized U1810 cells were incubated at 37 °C in SHKCl buffer supplemented with 5 mM succinate, in the presence or absence of 0.5 mM CaCl2 and 2 μg/ml ruthenium red (RR). After incubation, samples were analyzed by western blotting and probed for AIF. OMM intactness was confirmed by mitochondrial localization of cytochrome c in the sample where ruthenium red (RR) was added. (d) MEFs were treated with 0.2 μM STS for 24 h and analyzed for AIF processing and release. (e) U1810 cells were incubated as described in (c) and analyzed for AIF cleavage upon tBid-induced permeabilization of OMM. Analysis of cytochrome c release was used to confirm permeabilization of OMM. (f) Permeabilized U1810 cells were incubated at 37 °C in the presence of 0.5 mM CaCl2 and the following inhibitors; PMSF (5 mM), z-VAD-fmk (10 μM), Complete protease inhibitor cocktail (1 × ), calpain inhibitor I (100 μM), BAPTA/AM (10 μM) and PD150606 (200 μM). As positive control, 10 μg/ml (1.4 U/ml) of recombinant calpain I was used. Immunoblots were probed for AIF and subsequently reprobed for actin to confirm equal loading of the samples
Next, digitonin-permeabilized U1810 cells were incubated in the presence or absence of Ca2+. Ruthenium red, an inhibitor of mitochondrial Ca2+ uptake, was added to selected samples to prevent possible permeabilization of the OMM through Ca2+-dependent MPT. As shown in Figure 2c, Ca2+-triggered AIF processing was not inhibited by ruthenium red. As a control of OMM intactness, release of cytochrome c into the cytosol was analyzed and found to be absent (Figure 2c). Further, the comparison of wild-type (wt) and Bax−/−Bak−/− mouse embryonic fibroblasts (MEFs) revealed that AIF was processed in both cell lines in response to STS, although it was only released from the mitochondria in wt MEFs (Figure 2d).
Interestingly, truncated Bid (tBid)-induced permeabilization of the OMM did not enhance the processing of AIF (Figure 2e), supporting the assumption that a mitochondrial calpain was responsible for AIF cleavage. Finally, to further substantiate our findings, U1810 cells were incubated in the presence of Ca2+ together with a panel of protease inhibitors. AIF processing was abolished by treating the cells with a Ca2+ chelator, BAPTA/AM, or a nonspecific calpain inhibitor I, or a selective calpain inhibitor, PD150606, but not by the caspase inhibitor, zVAD-fmk (Figure 2f). Combined, these findings clearly show that AIF was cleaved in a Ca2+-dependent manner by a calpain, located in the IMS of mitochondria.
Staurosporine-induced Ca2+ influx activates calpain during apoptosis
Elevation of the intracellular Ca2+ concentration has been implicated as an important event in apoptosis.24, 25, 26 Hence, we investigated whether STS treatment of U1810 cells could evoke a Ca2+ signal sufficient to promote calpain-mediated AIF processing. The intracellular Ca2+ level was monitored in cells loaded with the Ca2+-sensitive dye Fluo-3.
Cells were first exposed to ATP, a G protein-coupled receptor agonist known to trigger inositol 1,4,5-trisphosphate (IP3)-mediated Ca2+ release. As expected, ATP treatment resulted in a transient intracellular Ca2+ increase (Figure 3a). In contrast, treatment with 0.2–2 μM STS caused a prolonged increase in the intracellular Ca2+ concentration (Figure 3b) that lasted for several minutes (indicated with bar) and was sufficient to trigger the proteolysis of AIF, which did not occur after the ATP-induced transient Ca2+ increase (Figure 3g). The STS-evoked Ca2+ increase was not observed in cells kept in a Ca2+-free buffer (Figure 3c) or in cells preloaded with BAPTA/AM (Figure 3d), suggesting that the source of the Ca2+ signal was extracellular. The importance of the extracellular Ca2+ store was further investigated by treating the cells with thapsigargin, a sarcoendoplasmic reticulum Ca2+-ATPase inhibitor known to deplete the endoplasmic reticular Ca2+ store. As shown in Figure 3e, an STS-induced Ca2+ increase could still be observed in thapsigargin-treated cells.
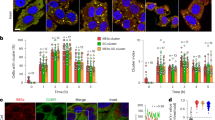
Staurosporine treatment triggers a prolonged increase in the intracellular Ca2+ level that activates calpain. Representative single-cell Ca2+ recordings of Fluo-3/AM-loaded U1810 cells treated with (a) 10 μM ATP or mock (DMSO) and (b) 0.2 μM STS, (c) cells kept in Ca2+-free medium before STS treatment, (d) cells loaded with BAPTA/AM 2 h before STS treatment, (e) cells treated with 10 μM thapsigargin before exposure to STS and (f) cells treated with FCCP before addition of STS. Ratio F/F0 represents fluorescence intensity over baseline. (g) Cells were either treated with 10 μM ATP or 0.2 μM STS for 24 h and analyzed for AIF processing. (h) Cells were treated with 0.2 μM STS for different time points, and samples were analyzed for the cleaved form of Atg5 by western blot. Membranes were reprobed for actin to confirm equal loading of samples. (i) Quantification of results obtained in (g); results are presented as mean±S.D. (n=3)
The initial increase in the cytosolic Ca2+ level upon STS exposure was followed by a time-dependent normalization of intracellular Ca2+ homeostasis. To examine the contribution of mitochondria to the restoration of Ca2+ homeostasis, a mitochondrial uncoupler, FCCP, was used to disrupt the mitochondrial membrane potential and thereby prevent mitochondrial Ca2+ import. Exposing the cells to STS after uncoupling of mitochondria resulted in a cytosolic Ca2+ elevation followed by an incomplete recovery of the basal cytosolic Ca2+ level (Figure 3f, indicated with bar), demonstrating that the mitochondria participate in the restoration of Ca2+ homeostasis following STS treatment of U1810 cells.
Recently, it has been demonstrated that autophagy-related gene 5 (Atg5) is cleaved specifically by calpains during apoptosis to generate a 24 kDa product.27 To confirm that calpains are indeed activated upon STS treatment, Atg5 cleavage was used as a marker of calpain activity. Hence, STS-evoked Atg5 cleavage was analyzed at different time points. As shown in Figure 3h and i, the amount of the 24 kDa Atg5 product was significantly increased 2 h after STS addition. Taken together, these results indicate that STS treatment causes a rapid influx of extracellular Ca2+, resulting in an elevation of the intracellular Ca2+ level sufficient to activate calpain, which can cleave AIF.
AIF, but not cytochrome c, release is prevented by calpain inhibition
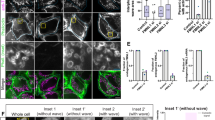
The significance of calpain activation for AIF release was further confirmed in situ by confocal imaging. Treatment of U1810 cells with different proapoptotic agents, such as kinase inhibitors (STS, protein kinase C inhibitor (PKC 412)) or a DNA-damaging agent (cisplatin), stimulated the release of both cytochrome c and AIF from mitochondria (Figure 4a, middle panel). However, pretreatment of cells with a selective calpain inhibitor, PD150606 or BAPTA/AM (not shown), efficiently blocked the release of AIF, but not cytochrome c, from the mitochondria (Figure 4a, lower panel). A quantification of these observations is presented in Figure 4b. This demonstrates that suppression of AIF release was indeed a result of calpain inhibition and not due to the prevention of OMM permeabilization. Similar results were obtained when cells were treated with PKC 412 or cisplatin (data not shown). In contrast, zVAD-fmk was unable to block AIF processing and release, indicating that this is a caspase-independent process (Figure 4c and d). The finding that AIF processing is mediated by calpain activation was further confirmed by immunoblotting. In agreement with the observations reported above, cleavage of AIF was blocked by a selective calpain inhibitor, or a Ca2+ chelator, whereas caspase inhibition did not affect this process (Figure 4d). These findings emphasize the importance of a mitochondrial calpain for AIF processing, independently of cell type or apoptotic stimuli, as the treatment of cells with either a DNA-damaging agent or kinase inhibitors produced similar effects.
AIF, but not cytochrome c, release is prevented by calpain inhibitor, PD150606. (a) Representative single-cell confocal images of untreated (upper panel), STS-treated (middle panel) and PD150606 or BAPTA/AM exposed cells before STS treatment (lower panel). The profile of the costaining with AIF and cytochrome c is shown in the panel to the right. White line indicates the area from which the profile of fluorescence was made. (b) Quantification of results obtained in (a). At least 50 cells from three independent experiments were counted per sample 24 h postexposure to 0.2 μM STS. Results are presented as mean±S.D. (n=3). (c) Representative single-cell confocal images of cells exposed for 2 h to 10 μM zVAD-fmk before 0.2 μM STS treatment. (d) Cells were exposed to zVAD-fmk (10 μM), BAPTA/AM (10 μM) or PD150606 (200 μM) for 2 h before 0.2 μM STS treatment for 24 h. Cells were collected and proteolysis of AIF was analyzed by immunoblotting. Membranes were reprobed for actin to confirm equal loading of the samples
Discussion
Malfunction of AIF release from mitochondria has been shown to be an important step in the development of resistance to conventional anticancer treatment of NSCLCs.11, 12, 13 However, the mechanisms by which AIF release is regulated have not yet been established conclusively. Therefore, in this study, we focused on the molecular mechanisms of AIF processing and release. We report that a prolonged increase in intracellular Ca2+ level is a prerequisite step for AIF processing and release from mitochondria during cell death signaling. As illustrated schematically in Figure 5, the elevated Ca2+ appears to activate a mitochondrial calpain located in the IMS, which in turn cleaves AIF before its release.
Hypothetical model of AIF processing. An apoptotic stimulus leads to (1) the influx of Ca2+ into the cell. The prolonged increase of the intracellular Ca2+ level results in (2) the activation of calpain in the IMS of mitochondria leading to (3) AIF processing. The AIF cleavage fragment is then (4) released into the cytosol through Bax/Bak-mediated pores (or as a result of the induction of Ca2+-dependent mitochondrial permeability transition) and translocates to the nucleus, where it can participate in chromatin condensation and large-scale DNA fragmentation. BAPTA/AM was able to completely abolish the elevation of intracellular Ca2+ and thereby to prevent calpain activation. PD150606, which specifically binds the Ca2+-binding site of calpains, prevents calpain activation and the downstream effects on AIF
As mentioned above, both m- and μ-calpains are generally considered to be located in the cytosol; however, these proteases have also been associated with the ER, Golgi and mitochondria. This association is hydrophobic; therefore, calpains reside mainly on the cytosolic side of the organelle membranes.28, 29, 30, 31 However, recent findings indicate that calpain 1 is also present within the mitochondria.23
It has been suggested that OMM permeabilization should precede AIF processing during apoptosis, as the overexpression of Bcl-2 and Bcl-XL prevented both AIF cleavage and release.18 In addition, based on the results obtained using recombinant proteins and permeabilized, isolated mitochondria, it has been reported that cytosolic calpain I can cleave AIF.20 The authors proposed that permeabilization of OMM was a prerequisite step granting calpain I access to its substrate. In contrast, using permeabilized cells we found that AIF was processed by calpain, even when the OMM was intact (cf. Figure 2a, c and d). Moreover, tBid-induced permeabilization of the OMM did not enhance the processing of AIF (cf. Figure 2e). This shows that the calpain responsible for AIF processing is present within the mitochondria and is thereby protected from the endogenous inhibitor calpastatin, which was detected only in the total lysate (cf. Figure 2b). Recently, it was reported that an increase in the Ca2+ level activates calpain 10 in the matrix of the mitochondria.32 However, as treatment of the cells with ruthenium red failed to prevent the cleavage of AIF in our experiments, the responsible calpain appears to be localized in the IMS rather than in the mitochondrial matrix (cf. Figure 2c). It has recently been shown that calpain I contains a mitochondrial localization signal and that the small subunit of calpain I can be coimported into the IMS together with the calpain I large subunit.23 In addition, the mitochondrial localization of calpain I was also demonstrated by live imaging of cells transfected with a GFP construct containing the N terminal of calpain I. The authors suggested that the mitochondrial outer membrane represents a barrier separating calpain I from its endogenous inhibitor calpastatin.23 If so, the only trigger needed for the activation of mitochondrial calpain I would be a Ca2+ signal. Our findings support this hypothesis, as we could detect calpain I in purified mitochondria and the addition of Ca2+ led to the generation of the soluble 57 kDa AIF fragment (cf. Figure 2a and c). However, exposing the cells to a level of ATP that triggers a transient IP3-mediated Ca2+ release into the cytosol did not result in cleavage of AIF (cf. Figure 3g). Therefore, it seems that a prolonged increase in intracellular Ca2+ level is required for AIF processing. This might explain why AIF is processed solely under pathological conditions (i.e. STS treatment) and not during physiological IP3-mediated Ca2+ signaling.
Churbanova and Sevrioukova33 recently reported that the AIF cleavage site is not exposed in untreated cells and suggested that AIF undergoes redox-dependent structural changes that could finally lead to the exposure of the cleavage site. Similarly, we have recently observed that stimulation of mitochondrial ROS production promotes Ca2+-mediated AIF processing (data not shown). Hence, the results obtained in earlier studies,23, 33 along with our current observations, suggest a scenario in which the processing of AIF might be regulated by a three-step mechanism. First, a prolonged increase in Ca2+ level activates mitochondrial calpain in the IMS. The second step might involve conformational changes of AIF leading to the exposure of the calpain cleavage site, which would then lead to the third step – AIF processing (Figure 5).
In some experimental systems, elevation of the intracellular Ca2+ level is regarded as an important mediator of apoptosis.26 For instance, it has been reported that STS treatment of PC12 cells resulted in both a rapid (min) and prolonged (h) elevation of intracellular Ca2+. The authors proposed that the prolonged, but not the rapid, Ca2+ increase was associated with apoptosis signaling.34 However, we found that the STS-induced increase in intracellular Ca2+ concentration was followed by its normalization within 15–20 min. Thus, it appears that a Ca2+ rise of this duration was sufficient to activate the cell death pathway in U1810 cells, whereas an ATP-triggered transient (1–3 min) Ca2+ signal was insufficient. It cannot be excluded that the STS-mediated Ca2+ increase might also contribute to OMM permeabilization during apoptosis. Indeed, as reported above, normalization of the cytosolic Ca2+ level after STS exposure involved mitochondrial Ca2+ sequestration, which might eventually stimulate MPT-dependent permeabilization of the OMM and the release of AIF. This scenario would also explain the previously observed protective effect of Bcl-2 and Bcl-XL,18 as overexpression of these antiapoptotic proteins is known to stabilize mitochondria toward MPT induction.35
Altogether, we report that a prolonged increase in intracellular Ca2+ concentration is required for AIF processing and release during cell death. The elevated Ca2+ level is required for the activation of a mitochondrial calpain in the IMS. The activated calpain can then process AIF to generate the 57 kDa protein that is subsequently released into the cytosol (Figure 5). The activation of calpain and its function in AIF processing appear not to be restricted to a particular cell type or apoptotic stimulus.
Materials and Methods
Cell culture
The human NSCLC cell line, U1810, used in this study has been previously investigated with regard to apoptosis susceptibility and resistance.11, 13 U1810 cells were grown in RPMI-1640 complete medium supplemented with 10% (v/v) heat-inactivated fetal bovine serum, 2% (w/v) glutamine, 100 U/ml penicillin and 100 U/ml streptomycin in a humidified 5% CO2 atmosphere at 37 °C and were maintained at a cell density allowing exponential growth. Hepatoma HEK293 cells and neuroblastoma SH-SY5Y cells were grown in DMEM and MEM medium, respectively. Wild-type and Bax−/− Bak−/− MEFs were both grown in DMEM medium. Cells were treated with either 0.2–2.0 μM STS (Sigma-Aldrich), 30 μM cisplatin or 10 μM PKC 412. The calpain inhibitor PD150606 (200 μM) (Alexis Biochemicals), BAPTA/AM (10 μM) (Biomol Research Laboratories Inc.), the pan-caspase inhibitor z-VAD-fmk (10 μM) (Enzyme Systems Products) were added to selected samples 2 h before treatment.
Immunofluorescence
Cells were seeded on coverslips, fixed for 20 min in 4% formaldehyde at 4 °C and washed with PBS. Incubations with primary antibodies, diluted (1 : 400) in PBS containing 0.3% Triton X-100 and 0.5% bovine serum albumin (BSA), and secondary antibodies (1 : 200) were performed at 4 °C overnight in a humid chamber and at room temperature for 60 min, respectively. Nuclei were counterstained with Hoechst 33342 (10 μg/ml in PBS solution) by 5 min incubation at room temperature. Between all steps, cells were washed for 3 × 10 min with PBS. The following primary antibodies were used: goat anti-AIF (Santa Cruz Biotechnology) and mouse anti-cytochrome c (BD Biosciences). Secondary FITC-conjugated antibodies directed to mouse (Alexa 488) or rabbit (Alexa 594) were purchased from Molecular Probes. Stained slides were mounted using Vectashield H-1000 (Vector Laboratories Inc.) and examined under a Zeiss LSM 510 META confocal laser scanner microscope (Zeiss).
Immunoblotting
Cell were trypsinized, washed in PBS and lysed for 5 min at room temperature in Complete Lysis-M buffer (Roche Diagnostics) supplemented with complete protease inhibitors (Roche Diagnostics). Cell extracts were centrifuged at 10 000 × g for 5 min at room temperature to separate insoluble material, followed by determination of protein concentration using the BCA assay (Pierce). Proteins from each sample were mixed with Laemmli's loading buffer, boiled for 5 min and subjected to SDS-PAGE at 40 mA followed by transfer to nitrocellulose membranes for 90 min at 120 V. Membranes were blocked for 30 min with 5% non-fat milk in TBS at room temperature and subsequently probed with the desired primary antibody. Blots were revealed by ECL™ (Amersham Biosciences). The following primary antibodies were used: goat anti-AIF, goat anti-calpain I, rabbit anti-Tom40, mouse anti-calpastatin (all from Santa Cruz Biotechnology), mouse anti-cytochrome c (BD Biosciences), rabbit anti-Atg5 (Abgent), rabbit anti-actin (Sigma) and mouse anti-Lamin B (Novo Castra Laboratories). All primary antibodies were diluted in TBS containing 1% BSA, 0.05% Tween 20 and 0.1% NaN3. Secondary antibodies were diluted in blocking buffer. Horseradish peroxidase-conjugated secondary antibodies were purchased from Pierce.
Isolation of mitochondria from U1810 cells
U1810 cells were harvested and pellets were resuspended in MSH buffer (210 mM mannitol, 70 mM sucrose, 5 mM Hepes (pH 7.5)) supplemented with 1 mM EDTA and 0.005% digitonin to disrupt the plasma membrane. The cell suspension was homogenized with a glass-Teflon homogenizer on ice (20 × ). Homogenates were centrifuged at 1500 × g for 5 min at 4 °C. This procedure was repeated twice and supernatants were pooled and centrifuged at 10 000 × g for 15 min to form a mitochondria-enriched pellet that was washed in MSH buffer and recentrifuged at 10 000 × g for 15 min. The pellet was resuspended in MSH buffer. The latter fraction was further purified by a gradient consisting of 1.5 ml 0.75 M sucrose, 1.5 ml 1 M sucrose, 3 ml 1.3 M sucrose and 1.5 ml 2.2 M sucrose, prepared in 5 mM Hepes (pH 7.5). Samples were centrifuged at 50 000 × g for 3 h at 4 °C in a Beckman L-60 ultracentrifuge with a SW41 swing-out rotor. The mitochondrial fraction was collected with a syringe and diluted five times in 5 mM Hepes (pH 7.5). The mitochondria were pelleted by centrifugation for 15 min at 10 000 × g. Mitochondrial pellet was resuspended in MSH buffer.
In vitro assays with permeabilized U1810 cells
Cells were harvested, washed in PBS and resuspended in SHKCL buffer (600 mM sorbitol, 125 mM KCl, 25 mM Hepes/KOH (pH 7.4)). Cells were permeabilized by the addition of 0.005% digitonin and incubated for different time periods at 37 °C under gentle shaking. In some experiments, permeabilized cells were incubated in SHKCl buffer containing 0.5 mM CaCl2 and 5 mM succinate to energize mitochondria. The following protease inhibitors were used: PMSF (5 mM), z-VAD-fmk (10 μM), Complete protease inhibitor cocktail (1 × ), calpain inhibitor I (100 μM), BAPTA/AM (10 μM) and PD150606 (200 μM). As positive control, 10 μg/ml of recombinant calpain I was used. For AIF processing assays, incubations were stopped by the addition of Laemmli buffer. For protein release assays, samples were fractionated into supernatant and pelleted by centrifugation at 16 000 × g at 4 °C for 15 min before addition of Laemmli buffer.
Ca2+ measurements
Cells were incubated (30 min at 37 °C in 5% CO2) in Hepes medium containing 5 μM Fluo-3/AM (Molecular Probes) together with 0.1% Pluronic F-127 (Molecular Probes). The Hepes medium contained 130 mM NaCl, 4.7 mM KCl, 1.3 mM CaCl2, 1 mM MgSO4, 1.2 mM KH2PO4, 20 mM Hepes (pH 7.4) and 5 mM dextrose. Petri dishes were transferred to a Zeiss LSM 510 META scanning laser confocal microscope equipped with a × 20/1.0 dipping lens (Zeiss). Images were acquired at 0.2 Hz, and all drugs were bath-applied. Thapsigargin was from Molecular Probes.
For measurement of MPT induction, 4 × 106 cells were suspended in 400 μl of buffer (150 mM KCl, 5 mM KH2PO4, 5 mM succinate, 1 mM MgSO4, 5 mM Tris (pH 7.4)). Cells were permeabilized with 0.005% digitonin, and MPT was induced by the addition of 0.5 mM CaCl2. Ca2+ concentration changes were registered using a calcium-sensitive electrode (Thermo Orion, Beverly, MA, USA) and visualized with a chart recorder.
Recombinant proteins
Truncated human Bid (tBid) was expressed in Escherichia coli strain (BL21 DE3) as N-terminal (his)6-tagged protein from vector pET23tBid. tBid was IMAC purified in the absence of any detergent, using standard chromatographic techniques. The proteins were dialyzed against 30% glycerol, 100 mM NaCl, 0.2 mM EDTA, 25 mM Hepes/KOH (pH 7.4), and tBid was applied at a concentration of 10 nM.
Abbreviations
- AIF:
-
apoptosis-inducing factor
- Atg5:
-
autophagy-related gene 5
- IMS:
-
intermembrane space
- IP3:
-
inositol 1,4,5-trisphosphate
- MEF:
-
mouse embryonic fibroblast
- MPT:
-
mitochondrial permeability transition
- NSCLC:
-
non-small-cell lung carcinoma
- OMM:
-
outer mitochondrial membrane
- PKC 412:
-
protein kinase C inhibitor
- STS:
-
staurosporine
- tBid:
-
truncated Bid
References
Thompson CB . Apoptosis in the pathogenesis and treatment of disease. Science 1995; 267: 1456–1462.
Arends MJ, Wyllie AH . Apoptosis: mechanisms and roles in pathology. Int Rev Exp Pathol 1991; 32: 223–254.
Cande C, Vahsen N, Kouranti I, Schmitt E, Daugas E, Spahr C et al. AIF and cyclophilin A cooperate in apoptosis-associated chromatinolysis. Oncogene 2004; 23: 1514–1521.
Du C, Fang M, Li Y, Li L, Wang X . Smac, a mitochondrial protein that promotes cytochrome c-dependent caspase activation by eliminating IAP inhibition. Cell 2000; 102: 33–42.
Liu X, Kim CN, Yang J, Jemmerson R, Wang X . Induction of apoptotic program in cell-free extracts: requirement for dATP and cytochrome c. Cell 1996; 86: 147–157.
Hegde R, Srinivasula SM, Zhang Z, Wassell R, Mukattash R, Cilenti L et al. Identification of Omi/HtrA2 as a mitochondrial apoptotic serine protease that disrupts inhibitor of apoptosis protein–caspase interaction. J Biol Chem 2002; 277: 432–438.
Susin SA, Lorenzo HK, Zamzami N, Marzo I, Snow BE, Brothers GM et al. Molecular characterization of mitochondrial apoptosis-inducing factor. Nature 1999; 397: 441–446.
Verhagen AM, Ekert PG, Pakusch M, Silke J, Connolly LM, Reid GE et al. Identification of DIABLO, a mammalian protein that promotes apoptosis by binding to and antagonizing IAP proteins. Cell 2000; 102: 43–53.
Suzuki Y, Imai Y, Nakayama H, Takahashi K, Takio K, Takahashi R . A serine protease, HtrA2, is released from the mitochondria and interacts with XIAP, inducing cell death. Mol Cell 2001; 8: 613–621.
Ravagnan L, Gurbuxani S, Susin SA, Maisse C, Daugas E, Zamzami N et al. Heat-shock protein 70 antagonizes apoptosis-inducing factor. Nat Cell Biol 2001; 3: 839–843.
Joseph B, Ekedahl J, Lewensohn R, Marchetti P, Formstecher P, Zhivotovsky B . Defective caspase-3 relocalization in non-small cell lung carcinoma. Oncogene 2001; 20: 2877–2888.
Gallego MA, Joseph B, Hemstrom TH, Tamiji S, Mortier L, Kroemer G et al. Apoptosis-inducing factor determines the chemoresistance of non-small-cell lung carcinomas. Oncogene 2004; 23: 6282–6291.
Hemstrom TH, Joseph B, Schulte G, Lewensohn R, Zhivotovsky B . PKC 412 sensitizes U1810 non-small cell lung cancer cells to DNA damage. Exp Cell Res 2005; 305: 200–213.
Miramar MD, Costantini P, Ravagnan L, Saraiva LM, Haouzi D, Brothers G et al. NADH oxidase activity of mitochondrial apoptosis-inducing factor. J Biol Chem 2001; 276: 16391–16398.
Klein JA, Longo-Guess CM, Rossmann MP, Seburn KL, Hurd RE, Frankel WN et al. The harlequin mouse mutation downregulates apoptosis-inducing factor. Nature 2002; 419: 367–374.
Vahsen N, Cande C, Briere JJ, Benit P, Joza N, Larochette N et al. AIF deficiency compromises oxidative phosphorylation. EMBO J 2004; 23: 4679–4689.
Loeffler M, Daugas E, Susin SA, Zamzami N, Metivier D, Nieminen AL et al. Dominant cell death induction by extramitochondrially targeted apoptosis-inducing factor. FASEB J 2001; 15: 758–767.
Otera H, Ohsakaya S, Nagaura Z, Ishihara N, Mihara K . Export of mitochondrial AIF in response to proapoptotic stimuli depends on processing at the intermembrane space. EMBO J 2005; 24: 1375–1386.
Joza N, Susin SA, Daugas E, Stanford WL, Cho SK, Li CY et al. Essential role of the mitochondrial apoptosis-inducing factor in programmed cell death. Nature 2001; 410: 549–554.
Polster BM, Basanez G, Etxebarria A, Hardwick JM, Nicholls DG . Calpain I induces cleavage and release of apoptosis-inducing factor from isolated mitochondria. J Biol Chem 2005; 280: 6447–6454.
Yuste VJ, Moubarak RS, Delettre C, Bras M, Sancho P, Robert N et al. Cysteine protease inhibition prevents mitochondrial apoptosis-inducing factor (AIF) release. Cell Death Differ 2005; 12: 1445–1448.
Cao G, Xing J, Xiao X, Liou AK, Gao Y, Yin XM et al. Critical role of calpain I in mitochondrial release of apoptosis-inducing factor in ischemic neuronal injury. J Neurosci 2007; 27: 9278–9293.
Badugu R, Garcia M, Bondada V, Joshi A, Geddes JW . N terminus of calpain 1 is a mitochondrial targeting sequence. J Biol Chem 2008; 283: 3409–3417.
McConkey DJ, Orrenius S . The role of calcium in the regulation of apoptosis. J Leukoc Biol 1996; 59: 775–783.
Nicotera P, Zhivotovsky B, Orrenius S . Nuclear calcium transport and the role of calcium in apoptosis. Cell Calcium 1994; 16: 279–288.
Orrenius S, Zhivotovsky B, Nicotera P . Regulation of cell death: the calcium-apoptosis link. Nat Rev Mol Cell Biol 2003; 4: 552–565.
Yousefi S, Perozzo R, Schmid I, Ziemiecki A, Schaffner T, Scapozza L et al. Calpain-mediated cleavage of Atg5 switches autophagy to apoptosis. Nat Cell Biol 2006; 8: 1124–1132.
Hood JL, Logan BB, Sinai AP, Brooks WH, Roszman TL . Association of the calpain/calpastatin network with subcellular organelles. Biochem Biophys Res Commun 2003; 310: 1200–1212.
Hood JL, Brooks WH, Roszman TL . Differential compartmentalization of the calpain/calpastatin network with the endoplasmic reticulum and Golgi apparatus. J Biol Chem 2004; 279: 43126–43135.
Molinari M, Carafoli E . Calpain: a cytosolic proteinase active at the membranes. J Membr Biol 1997; 156: 1–8.
Goll DE, Thompson VF, Li H, Wei W, Cong J . The calpain system. Physiol Rev 2003; 83: 731–801.
Arrington DD, Van Vleet TR, Schnellmann RG . Calpain 10: a mitochondrial calpain and its role in calcium-induced mitochondrial dysfunction. Am J Physiol Cell Physiol 2006; 291: C1159–C1171.
Churbanova IY, Sevrioukova IF . Redox-dependent changes in molecular properties of mitochondrial apoptosis-inducing factor. J Biol Chem 2008; 283: 5622–5631.
Kruman I, Guo Q, Mattson MP . Calcium and reactive oxygen species mediate staurosporine-induced mitochondrial dysfunction and apoptosis in PC12 cells. J Neurosci Res 1998; 51: 293–308.
Murphy RC, Schneider E, Kinnally KW . Overexpression of Bcl-2 suppresses the calcium activation of a mitochondrial megachannel. FEBS Lett 2001; 497: 73–76.
Acknowledgements
This work was supported by grants from the Swedish Research Council, the Swedish and the Stockholm Cancer Societies, the Swedish Childhood Cancer Foundation, the EC FP-6 (Oncodeath and Chemores) as well as the FP7 (Apo-Sys) programs. MO is a post-doctoral fellow of the Wenner-Gren Foundation, Stockholm, Sweden. MH is the recipient of a stipend for academic exchange from the DAAD, Germany. We thank Bruno Antonsson for the generous gift of plasmid pET23tBid and the late Stan Korsmeyer for Bax/Bak DKO MEFs.
Author information
Authors and Affiliations
Corresponding author
Additional information
Edited by G Melino
Rights and permissions
About this article
Cite this article
Norberg, E., Gogvadze, V., Ott, M. et al. An increase in intracellular Ca2+ is required for the activation of mitochondrial calpain to release AIF during cell death. Cell Death Differ 15, 1857–1864 (2008). https://doi.org/10.1038/cdd.2008.123
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cdd.2008.123
Keywords
This article is cited by
-
Recent advances and applications of peptide–agent conjugates for targeting tumor cells
Journal of Cancer Research and Clinical Oncology (2023)
-
Upregulation of Ca2+-binding proteins contributes to VTA dopamine neuron survival in the early phases of Alzheimer’s disease in Tg2576 mice
Molecular Neurodegeneration (2022)
-
The role of cGMP-signalling and calcium-signalling in photoreceptor cell death: perspectives for therapy development
Pflügers Archiv - European Journal of Physiology (2021)
-
Modelling human CNS injury with human neural stem cells in 2- and 3-Dimensional cultures
Scientific Reports (2020)
-
Neuroprotective Effects of Dexmedetomidine Preconditioning on Oxygen-glucose Deprivation-reoxygenation Injury in PC12 Cells via Regulation of Ca2+-STIM1/Orai1 Signaling
Current Medical Science (2020)