Abstract
Objective:
To investigate whether ventilatory factors limit exercise in overweight and obese children during a 6-min step test and to compare ventilatory responses during this test with those of healthy weight children.
Design:
Cross-sectional, prospective comparative study.
Subjects:
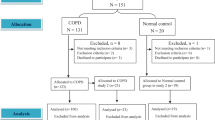
Twenty-six overweight/obese subjects and 25 healthy weight subjects with no known respiratory illness.
Measurements:
Various fatness and fat distribution parameters (using air displacement plethysmography and anthropometry), pulmonary function tests, breath-by-breath gas analysis during exercise, perceived exertion.
Results:
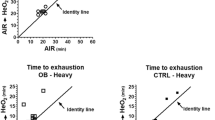
Young people who are overweight or obese are more likely to experience expiratory flow limitation (expFL) during submaximal exercise compared with their healthy weight peers [OR 7.2 (1.4, 37.3), P=0.019]. Subjects who had lower lung volumes at rest were even more likely to experience exercise-induced expFLs [OR 8.35 (1.4–49.3)]. Both groups displayed similar breathing strategies during submaximal exercise.
Conclusion:
Young people who are overweight/obese are more likely to display expFL during submaximal exercise compared with children of healthy weight . Use of compensatory breathing strategies appeared to enable overweight children to avoid the experience of breathlessness at this intensity of exercise.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Olds TS, Tomkinson GR, Ferrar KE, Maher CA . Trends in the prevalence of childhood overweight and obesity in Australia between 1985 and 2008. Int J Obes 2009; 34: 57–66.
OECD. Health at a Glance: OECD Indicators In: OECD Publishing, 2011.
Burke V . Obesity in childhood and cardiovascular risk. Clin Exp Pharmacol Physiol 2006; 33: 831–837.
Wijga AH, Scholtens S, Bemelmans WJ, de Jongste JC, Kerkhof M, Schipper M et al. Comorbidities of obesity in school children: a cross-sectional study in the PIAMA birth cohort. BMC Public Health 2010; 10: 184.
Zhang Z, Lai HJ, Roberg KA, Gangnon RE, Evans MD, Anderson EL et al. Early childhood weight status in relation to asthma development in high-risk children. J Allergy Clin Immunol 2010; 126: 1157–1162.
Allender S, Kremer P, de Silva-Sanigorski A, Lacy K, Millar L, Mathews L et al. Associations between activity-related behaviours and standardized BMI among Australian adolescents. J Sci Med Sport 2011; 14: 512–521.
Ortega FB, Ruiz JR, Castillo MJ, Sjostrom M . Physical fitness in childhood and adolescence: a powerful marker of health. Int J Obes 2007; 32: 1–11.
Steinbeck KS . The importance of physical activity in the prevention of overweight and obesity in childhood: a review and an opinion. Obes Rev 2001; 2: 117–130.
Hallal PC, Bauman AE, Heath GW, Kohl HW, Lee IM, Pratt M . Physical activity: more of the same is not enough. Lancet 2012; 380: 190–191.
Saris WHM, Blair SN, Van Baak MA, Eaton SB, Davies PSW, Di Pietro L et al. How much physical activity is enough to prevent unhealthy weight gain? Outcome of the IASO 1st stock conference and consensus statement. Obes Rev 2003; 4: 101–114.
Saavedra JM, Escalante Y, Garcia-Hermoso A . Improvement of aerobic fitness in obese children: a meta-analysis. Int J Pediatr Obes 2011; 6: 169–177.
Stubbs J, Whybrow S, Teixeira P, Blundell J, Lawton C, Westenhoefer J et al. Problems in identifying predictors and correlates of weight loss and maintenance: implications for weight control therapies based on behaviour change. Obes Rev 2011; 12: 688–708.
Schachter LM, Salome CM, Peat JK, Woolcock AJ . Obesity is a risk for asthma and wheeze but not airway hyperresponsiveness. Thorax 2001; 56: 4–8.
Marinov B, Kostianev S, Turnovska T . Ventilatory efficiency and rate of perceived exertion in obese and non-obese children performing standardized exercise. Clin Physiol Funct Imaging 2002; 22: 254–260.
Leung TF, Li CY, Lam CW, Au CS, Yung E, Chan IH et al. The relation between obesity and asthmatic airway inflammation. Pediatr Allergy Immunol 2004; 15: 344–350.
Li AM, Chan D, Wong E, Yin J, Nelson EAS, Fok TF . The effects of obesity on pulmonary function. Arch Dis Child 2003; 88: 361–363.
Spathopoulos D, Paraskakis E, Trypsianis G, Tsalkidis A, Arvanitidou V, Emporiadou M et al. The effect of obesity on pulmonary lung function of school aged children in Greece. Pediatr Pulmonol 2009; 44: 273–280.
WHO. Global recommendations on physical activity for health. Geneva, 2011.
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH . Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000; 320: 1240.
Ginde SR, Geliebter A, Rubiano F, Silva AM, Wang J, Heshka S et al. Air displacement plethysmography: validation in overweight and obese subjects[ast][ast]. Obesity 2005; 13: 1232–1237.
Miller MR, Hankinson J, Brusasco V, Burgos F, Casaburi R, Coates A et al. Standardisation of spirometry. Eur Respir J 2005; 26: 319–338.
Wanger J, Clausen JL, Coates A, Pedersen OF, Brusasco V, Burgos F et al. Standardisation of the measurement of lung volumes. Eur Resp J 2005; 26: 511–522.
Stanojevic S, Wade A, Cole TJ, Lum S, Custovic A, Silverman M et al. Spirometry centile charts for young caucasian children. Am J Resp Crit Care Med 2009; 180: 547–552.
Cook CD, Hamann JF . Relation of lung volumes to height in healthy persons between the ages of 5 and 38 years. J Pediatr 1961; 59: 710–714.
Narang I, Pike S, Rosenthal M, Balfour-Lynn IM, Bush A . Three minute step test to assess exercise capacity in children with cystic fibrosis with mild lung disease. Pediatr Pulmonol 2003; 35: 108–113.
Nourry C, Deruelle F, Fabre C, Baquet G, Bart F, Grosbois JM et al. Evidence of ventilatory constraints in healthy exercising prepubescent children. Pediatr Pulmonol 2006; 41: 133–140.
Johnson BD, Weisman IM, Zeballos RJ, Beck KC . Emerging concepts in the evaluation of ventilatory limitation during exercise: the exercise tidal flow-volume loop. Chest 1999; 116: 488–503.
Lamb KL . Children’s ratings of effort during cycle ergometry: an examination of the validity of two effort rating scales. Pediatr Exerc Sci 1995; 7: 407–421.
Ofir D, Laveneziana P, Webb KA, O’Donnell DE . Ventilatory and perceptual responses to cycle exercise in obese women. J Appl Physiol 2007; 102: 2217–2226.
Acknowledgements
This study was funded by a Princess Margaret Hospital Foundation Clinical Project Grant. We wish to acknowledge the contribution of Diane Awcock who assisted with data collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Gibson, N., Johnston, K., Bear, N. et al. Expiratory flow limitation and breathing strategies in overweight adolescents during submaximal exercise. Int J Obes 38, 22–26 (2014). https://doi.org/10.1038/ijo.2013.137
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2013.137
Keywords
This article is cited by
-
Lung function in obese children and adolescents without respiratory disease: a systematic review
BMC Pulmonary Medicine (2020)
-
Obesity: systemic and pulmonary complications, biochemical abnormalities, and impairment of lung function
Multidisciplinary Respiratory Medicine (2016)