Abstract
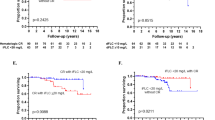
Immunoparesis is an adverse prognostic marker in plasma cell proliferative disorders. Its impact in AL amyloidosis has not been explored in depth. Newly diagnosed AL amyloidosis patients (n=998) were evaluated for immunoparesis by two methods. The first method was qualitative, considering the number of suppressed uninvolved immunoglobulins below the lower limit of normal (LLN) (none, partial, all). The second method was quantitative, assessing the average relative difference (ARD) of the uninvolved immunoglobulins from the LLN. Patients with suppression of all the uninvolved immunoglobulins were less likely to achieve very good partial response (VGPR) or better to first-line treatment (44%) compared with patients with partial suppression (68%) or preserved uninvolved immunoglobulins (64%; P<0.0001). In addition, patients with suppression of all the uninvolved immunoglobulins had a shorter survival compared with the respective comparators (median 18 vs 54 vs 52 months; P<0.0001). In the quantitative method, patients with a negative ARD were less likely to achieve VGPR or better (48%) and had a shorter survival (median 24 months) compared with patients with a positive ARD (69%, 57 months, respectively; P<0.0001). In a multivariate analysis for survival, both assessment methods retained an independent impact. Significant immunoparesis has a negative impact on response and survival in newly diagnosed AL amyloidosis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Kastritis E, Zagouri F, Symeonidis A, Roussou M, Sioni A, Pouli A et al. Preserved levels of uninvolved immunoglobulins are independently associated with favorable outcome in patients with symptomatic multiple myeloma. Leukemia 2014; 28: 2075–2079.
Ludwig H, Milosavljevic D, Berlanga O, Zojer N, Hubl W, Fritz V et al. Suppression of the non-involved pair of the myeloma isotype (HLC-matched pair) correlates with poor survival in newly diagnosed and relapsed/refractory patients with myeloma. Am J Hematol 2015; 91: 295–301.
Katodritou E, Terpos E, Symeonidis AS, Pouli A, Kelaidi C, Kyrtsonis MC et al. Clinical features, outcome, and prognostic factors for survival and evolution to multiple myeloma of solitary plasmacytomas: a report of the Greek myeloma study group in 97 patients. Am J Hematol 2014; 89: 803–808.
Perez-Persona E, Vidriales MB, Mateo G, Garcia-Sanz R, Mateos MV, de Coca AG et al. New criteria to identify risk of progression in monoclonal gammopathy of uncertain significance and smoldering multiple myeloma based on multiparameter flow cytometry analysis of bone marrow plasma cells. Blood 2007; 110: 2586–2592.
Jackson A, Scarffe JH . Prognostic significance of osteopenia and immunoparesis at presentation in patients with solitary myeloma of bone. Eur J Cancer 1990; 26: 363–371.
Muchtar E, Magen H, Itchaki G, Cohen A, Rosenfeld R, Shochat T et al. Uninvolved immunoglobulins predicting hematological response in newly diagnosed AL amyloidosis. Leuk Res 2015; 41: 56–61.
Gertz MA, Comenzo R, Falk RH, Fermand JP, Hazenberg BP, Hawkins PN et al. Definition of organ involvement and treatment response in immunoglobulin light chain amyloidosis (AL): a consensus opinion from the 10th International Symposium on Amyloid and Amyloidosis, Tours, France, 18-22 April 2004. Am J Hematol 2005; 79: 319–328.
Palladini G, Dispenzieri A, Gertz MA, Kumar S, Wechalekar A, Hawkins PN et al. New criteria for response to treatment in immunoglobulin light chain amyloidosis based on free light chain measurement and cardiac biomarkers: impact on survival outcomes. J Clin Oncol 2012; 30: 4541–4549.
Rajkumar SV, Fonseca R, Dispenzieri A, Lacy MQ, Lust JA, Witzig TE et al. Methods for estimation of bone marrow plasma cell involvement in myeloma: predictive value for response and survival in patients undergoing autologous stem cell transplantation. Am J Hematol 2001; 68: 269–275.
Dispenzieri A, Gertz MA, Kyle RA, Lacy MQ, Burritt MF, Therneau TM et al. Prognostication of survival using cardiac troponins and N-terminal pro-brain natriuretic peptide in patients with primary systemic amyloidosis undergoing peripheral blood stem cell transplantation. Blood 2004; 104: 1881–1887.
Kumar S, Dispenzieri A, Lacy MQ, Hayman SR, Buadi FK, Colby C et al. Revised prognostic staging system for light chain amyloidosis incorporating cardiac biomarkers and serum free light chain measurements. J Clin Oncol 2012; 30: 989–995.
Comenzo RL, Reece D, Palladini G, Seldin D, Sanchorawala V, Landau H et al. Consensus guidelines for the conduct and reporting of clinical trials in systemic light-chain amyloidosis. Leukemia 2012; 26: 2317–2325.
D'Souza A, Dispenzieri A, Wirk B, Zhang MJ, Huang J, Gertz MA et al. Improved outcomes after autologous hematopoietic cell transplantation for light chain amyloidosis: a Center for International Blood and Marrow Transplant Research Study. J Clin Oncol 2015; 33: 3741–3749.
Kaysen GA, al Bander H . Metabolism of albumin and immunoglobulins in the nephrotic syndrome. Am J Nephrol 1990; 10: 36–42.
Bogers WM, Stad RK, Van Es LA, Daha MR . Both Kupffer cells and liver endothelial cells play an important role in the clearance of IgA and IgG immune complexes. Res Immunol 1992; 143: 219–224.
Martin DM, Vroon DH, Nasrallah SM . Value of serum immunoglobulins in the diagnosis of liver disease. Liver 1984; 4: 214–218.
McPherson S, Henderson E, Burt AD, Day CP, Anstee QM . Serum immunoglobulin levels predict fibrosis in patients with non-alcoholic fatty liver disease. J Hepatol 2014; 60: 1055–1062.
Gertz MA, Kyle RA . Amyloidosis: prognosis and treatment. Semin Arthritis Rheum 1994; 24: 124–138.
Palladini G, Hegenbart U, Milani P, Kimmich C, Foli A, Ho AD et al. A staging system for renal outcome and early markers of renal response to chemotherapy in AL amyloidosis. Blood 2014; 124: 2325–2332.
Acknowledgements
We would like to thank two patients, UN and PG, for inspiring the idea of the role of immunoparesis in AL amyloidosis
Author contributions
EM designed the study, analyzed the data, wrote the first draft and approved the final version of the manuscript; AD, SKK, FKB, MQL, SZ, SRH, NL, TVK, WG, SR, DD, JAL, YL, PK, RG and VSK performed patient management, revised the manuscript critically and participated in final data analysis and approval of the final version of the manuscript. RC analyzed data, provided critical review of the manuscript and approved the last version of the manuscript; RAK performed patients’ follow-up, revised the manuscript critically and participated in final data analysis and approval of the final version of the manuscript; MAG performed patient management, designed the study, analyzed the data, wrote the first draft and approved the final version of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Leukemia website
Rights and permissions
About this article
Cite this article
Muchtar, E., Dispenzieri, A., Kumar, S. et al. Immunoparesis in newly diagnosed AL amyloidosis is a marker for response and survival. Leukemia 31, 92–99 (2017). https://doi.org/10.1038/leu.2016.140
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2016.140
This article is cited by
-
Immunoglobulin light chain amyloidosis
memo - Magazine of European Medical Oncology (2021)
-
Bone marrow plasma cells 20% or greater discriminate presentation, response, and survival in AL amyloidosis
Leukemia (2020)
-
Comparative analysis of staging systems in AL amyloidosis
Leukemia (2019)
-
Changes in uninvolved immunoglobulins during induction therapy for newly diagnosed multiple myeloma
Blood Cancer Journal (2017)