Abstract
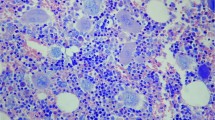
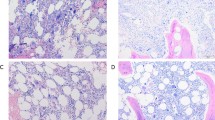
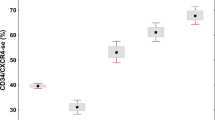
Paediatric chronic myeloid leukaemia (ped-CML) is rare and ped-CML with fibre accumulation in the bone marrow (MF) is thought to be even rarer. In adults (ad-CML), fibrosis represents an adverse prognostic factor. So far, the pro-fibrotic changes in the bone marrow microenvironment have not been investigated in detail in ped-CML. From a total of 66 ped-CML in chronic phase, biopsies were analysable and 10 had MF1/2 (MF1, n=8/10; MF2, n=2/10). We randomly selected 16 ped-CML and 16 ad-CML cases with and without fibrosis (each n=8) as well as 18 non-neoplastic controls. Bone marrow samples were analysed with a real-time PCR-based assay (including 127 genes for paediatric cases) and by immunohistochemistry. We found increased expression of megakaryocytic genes in ped-CML. The number of megakaryocytes and pro-platelets are increased in CML patients, but the most significant increase was noted for ped-CML-MF1/2. Anti-fibrotic MMP9 expression was lower in children than in adults. Cell mobilisation-related CXCL12 was decreased in young and adult patients with CML but not the corresponding receptor CXCR4. In summary, fibre accumulation in ped-CML-MF1/2 is associated with increased megakaryocytic proliferation and increased interstitial pro-platelet deposition. Deregulated expression of matrix-modulating factors shifts the bone marrow microenvironment towards fibrosis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Swerdlow SH, Campo C, Harris NL, Jaffe ES, Pileri SA, Stein H et al (eds) WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues. IARC Press: Lyon, France, 2008.
Hofmann I . Myeloproliferative neoplasms in children. J Hematop 2015; 8: 143–157.
Kucine N, Chastain KM, Mahler MB, Bussel JB . Primary thrombocytosis in children. Haematologica 2014; 99: 620–628.
Teofili L, Giona F, Torti L, Cenci T, Ricerca BM, Rumi C et al. Hereditary thrombocytosis caused by MPLSer505Asn is associated with a high thrombotic risk, splenomegaly and progression to bone marrow fibrosis. Haematologica 2010; 95: 65–70.
Sieff CA, Malleson P . Familial myelofibrosis. Arch Dis Child 1980; 55: 888–893.
Castro-Malaspina H, Schaison G, Briere J, Passe S, Briere J, Pasquier A et al. Philadelphia chromosome-positive chronic myelocytic leukemia in children. Cancer 1983; 52: 721–727.
Stieglitz E, Loh ML . Genetic predispositions to childhood leukemia. Ther Adv Hematol 2013; 4: 270–290.
Rau AT, Shreedhara AK, Kumar S . Myelodysplastic syndromes in children: where are we today? Ochsner J 2012; 12: 216–220.
Choi JK . Hematopoietic disorders in Down syndrome. Int J Clin Exp Pathol 2008; 1: 387–395.
Barosi G, Rosti V, Bonetti E, Campanelli R, Carolei A, Catarsi P et al. Evidence that prefibrotic myelofibrosis is aligned along a clinical and biological continuum featuring primary myelofibrosis. PLoS One 2012; 7: e35631.
Kvasnicka HM, Beham-Schmid C, Bob R, Dirnhofer S, Hussein K, Kreipe H et al. Problems and pitfalls in grading of bone marrow fibrosis, collagen deposition and osteosclerosis - a consensus-based study. Histopathology 2016; 68: 905–915.
Eliacik E, Isik A, Aydin C, Uner A, Aksu S, Sayinalp N et al. Bone marrow fibrosis may be an effective independent predictor of the 'TKI drug response level' in chronic myeloid leukemia. Hematology 2015; 20: 392–396.
Tanrikulu Simsek E, Eskazan AE, Cengiz M, Ar MC, Ekizoglu S, Salihoglu A et al. Imatinib reduces bone marrow fibrosis and overwhelms the adverse prognostic impact of reticulin formation in patients with chronic myeloid leukaemia. J Clin Pathol 2016; 69: 810–816.
Buesche G, Ganser A, Schlegelberger B, von Neuhoff N, Gadzicki D, Hecker H et al. Marrow fibrosis and its relevance during imatinib treatment of chronic myeloid leukemia. Leukemia 2007; 21: 2420–2427.
Buesche G, Freund M, Hehlmann R, Georgii A, Ganser A, Hecker H et al. Treatment intensity significantly influencing fibrosis in bone marrow independently of the cytogenetic response: meta-analysis of the long-term results from two prospective controlled trials on chronic myeloid leukemia. Leukemia 2004; 18: 1460–1467.
Hussein K, Büsche G, Schlue J, Lehmann U, Kreipe H . Myeloproliferative neoplasms: histopathological and molecular pathological diagnosis. Pathologe 2012; 33: 508–517.
Tefferi A . Myeloproliferative neoplasms: a decade of discoveries and treatment advances. Am J Hematol 2016; 91: 50–58.
Hussein K, Bock O, Seegers A, Flasshove M, Henneke F, Buesche G et al. Myelofibrosis evolving during imatinib treatment of a chronic myeloproliferative disease with coexisting BCR-ABL translocation and JAK2V617F mutation. Blood 2007; 109: 4106–4107.
Hussein K, Bock O, Theophile K, Seegers A, Arps H, Basten O et al. Chronic myeloproliferative diseases with concurrent BCR-ABL junction and JAK2V617F mutation. Leukemia 2008; 22: 1059–1062.
Mondet J, Hussein K, Mossuz P . Circulating cytokine levels as markers of inflammation in philadelphia negative myeloproliferative neoplasms: diagnostic and prognostic interest. Mediators Inflamm 2015; 2015: 670580.
Kreipe H, Büsche G, Bock O, Hussein K . Myelofibrosis: molecular and cell biological aspects. Fibrogenesis Tissue Rep 2012; 5: S21.
Poulter NS, Thomas SG . Cytoskeletal regulation of platelet formation: coordination of F-actin and microtubules. Int J Biochem Cell Biol 2015; 66: 69–74.
Muth M, Büsche G, Bock O, Hussein K, Kreipe H . Aberrant proplatelet formation in chronic myeloproliferative neoplasms. Leuk Res 2010; 34: 1424–1429.
Fabarius A, Kalmanti L, Dietz CT, Lauseker M, Rinaldetti S, Haferlach C et al. Impact of unbalanced minor route versus major route karyotypes at diagnosis on prognosis of CML. Ann Hematol 2015; 94: 2015–2024.
Hussein K, Bock O, Theophile K, von Neuhoff N, Buhr T, Schlué J et al. JAK2(V617F) allele burden discriminates essential thrombocythemia from a subset of prefibrotic-stage primary myelofibrosis. Exp Hematol 2009; 37: 1186–1193.
Bartels S, Lehmann U, Büsche G, Schlue J, Mozer M, Stadler J et al. SRSF2 and U2AF1 mutations in primary myelofibrosis are associated with JAK2 and MPL but not calreticulin mutation and may independently reoccur after allogeneic stem cell transplantation. Leukemia 2015; 29: 253–255.
Nangalia J, Massie CE, Baxter EJ, Nice FL, Gundem G, Wedge DC et al. Somatic CALR mutations in myeloproliferative neoplasms with nonmutated JAK2. N Engl J Med 2013; 369: 2391–2405.
Zell S, Schmitt R, Witting S, Kreipe HH, Hussein K, Becker JU . Hypoxia induces mesenchymal gene expression in renal tubular epithelial cells: An in vitro model of kidney transplant fibrosis. Nephron Extra 2013; 3: 50–58.
Hussein K, Stucki-Koch A, Alchalby H, Triviai I, Kröger N, Kreipe H . Cytokine expression pattern in bone marrow microenvironment after allogeneic stem cell transplantation in primary myelofibrosis. Biol Blood Marrow Transplant 2016; 22: 644–650.
Hauck G, Jonigk D, Göhring G, Kreipe H, Hussein K . Myelofibrosis in Philadelphia chromosome-negative myeloproliferative neoplasms is associated with aberrant karyotypes. Cancer Genet 2013; 206: 116–123.
Agirre X, Jiménez-Velasco A, San José-Enériz E, Garate L, Bandrés E, Cordeu L et al. Down-regulation of hsa-miR-10a in chronic myeloid leukemia CD34+ cells increases USF2-mediated cell growth. Mol Cancer Res 2008; 6: 1830–1840.
Ha JS, Jung HR . Up-regulation of microRNA 146b is associated with myelofibrosis in myeloproliferative neoplasms. Ann Clin Lab Sci 2015; 45: 308–314.
Hussein K, Büsche G, Muth M, Göhring G, Kreipe H, Bock O . Expression of myelopoiesis-associated microRNA in bone marrow cells of atypical chronic myeloid leukaemia and chronic myelomonocytic leukaemia. Ann Hematol 2011; 90: 307–313.
Crews LA, Jamieson CH . Chronic myeloid leukemia stem cell biology. Curr Hematol Malig Rep 2012; 7: 125–132.
Cogle CR, Saki N, Khodadi E, Li J, Shahjahani M, Azizidoost S . Bone marrow niche in the myelodysplastic syndromes. Leuk Res 2015; 39: 1020–1027.
Bulycheva E, Rauner M, Medyouf H, Theurl I, Bornhäuser M, Hofbauer LC et al. Myelodysplasia is in the niche: novel concepts and emerging therapies. Leukemia 2015; 29: 259–268.
Hijiya N, Schultz KR, Metzler M, Millot F, Suttorp M . Pediatric chronic myeloid leukemia is a unique disease that requires a different approach. Blood 2016; 127: 392–399.
Castagnetti F, Gugliotta G, Baccarani M, Breccia M, Specchia G, Levato L et al. Differences among young adults, adults and elderly chronic myeloid leukemia patients. Ann Oncol 2015; 26: 185–192.
Suttorp M, Thiede C, Tauer JT, Roettgers S, Sedlacek P, Harbott J . Chronic myeloid leukemia in pediatrics-first results from study CML-PAED II. Blood 2009; 114: 342.
Pemmaraju N, Kantarjian H, Shan J, Jabbour E, Quintas-Cardama A, Verstovsek S et al. Analysis of outcomes in adolescents and young adults with chronic myelogenous leukemia treated with upfront tyrosine kinase inhibitor therapy. Haematologica 2012; 97: 1029–1035.
Kalmanti L, Saussele S, Lauseker M, Proetel U, Müller MC, Hanfstein B et al. Younger patients with chronic myeloid leukemia do well in spite of poor prognostic indicators: results from the randomized CML study IV. Ann Hematol 2014; 93: 71–80.
Theophile K, Hussein K, Kreipe H, Bock O . Expression profiling of apoptosis-related genes in megakaryocytes: BNIP3 is downregulated in primary myelofibrosis. Exp Hematol 2008; 36: 1728–1738.
Hussein K, Theophile K, Dralle W, Wiese B, Kreipe H, Bock O . MicroRNA expression profiling of megakaryocytes in primary myelofibrosis and essential thrombocythemia. Platelets 2009; 20: 391–400.
Muth M, Engelhardt BM, Kröger N, Hussein K, Schlué J, Büsche G et al. Thrombospondin-1 (TSP-1) in primary myelofibrosis (PMF) - a megakaryocyte-derived biomarker which largely discriminates PMF from essential thrombocythemia. Ann Hematol 2011; 90: 33–40.
Bock O, Neuse J, Hussein K, Brakensiek K, Buesche G, Buhr T et al. Aberrant collagenase expression in chronic idiopathic myelofibrosis is related to the stage of disease but not to the JAK2 mutation status. Am J Pathol 2006; 169: 471–481.
Wan DC, Aalami OO, Wang Z, Nacamuli RP, Lorget F, Derynck R et al. Differential gene expression between juvenile and adult dura mater: a window into what genes play a role in the regeneration of membranous bone. Plast Reconstr Surg 2006; 118: 851–861.
Dangwal S, Thum T . MicroRNAs in platelet physiology and pathology. Hamostaseologie 2013; 33: 17–20.
Hussein K . Pathobiology of the microRNA system. Pathologe 2012; 33: 70–78.
Wang J, Wang Y, Han J, Li Y, Xie C, Xie L et al. Integrated analysis of microRNA and mRNA expression profiles in the left atrium of patients with nonvalvular paroxysmal atrial fibrillation: role of miR-146b-5p in atrial fibrosis. Heart Rhythm 2015; 12: 1018–1026.
Stucki-Koch A, Hauck G, Kreipe H, Hussein K . MicroRNA expression profiles in BCR-ABL-negative primary myelofibrosis with chromosome 7q defects. J Hematopathol 2015; 8: 203–208.
Hershkovitz-Rokah O, Modai S, Pasmanik-Chor M, Toren A, Shomron N, Raanani P et al. Restoration of miR-424 suppresses BCR-ABL activity and sensitizes CML cells to imatinib treatment. Cancer Lett 2015; 360: 245–256.
Zhao JL, Rao DS, Boldin MP, Taganov KD, O'Connell RM, Baltimore D . NF-kappaB dysregulation in microRNA-146a-deficient mice drives the development of myeloid malignancies. Proc Natl Acad Sci USA 2011; 108: 9184–9189.
Karpova D, Bonig H . Concise Review: CXCR4/CXCL12 Signaling in immature hematopoiesis- lessons from pharmacological and genetic models. Stem Cells 2015; 33: 2391–2399.
Zhang B, Ho YW, Huang Q, Maeda T, Lin A, Lee SU et al. Altered microenvironmental regulation of leukemic and normal stem cells in chronic myelogenous leukemia. Cancer Cell 2012; 21: 577–592.
Peled A, Hardan I, Trakhtenbrot L, Gur E, Magid M, Darash-Yahana M et al. Immature leukemic CD34+CXCR4+ cells from CML patients have lower integrin-dependent migration and adhesion in response to the chemokine SDF-1. Stem Cells 2002; 20: 259–266.
Krause DS, Fulzele K, Catic A, Sun CC, Dombkowski D, Hurley MP et al. Differential regulation of myeloid leukemias by the bone marrow microenvironment. Nat Med 2013; 19: 1513–1517.
Krause DS, Lazarides K, von Andrian UH, Van Etten RA . Requirement for CD44 in homing and engraftment of BCR-ABL-expressing leukemic stem cells. Nat Med 2006; 12: 1175–1180.
Acknowledgements
This study was funded by Deutsche Krebshilfe and Freundeskreis der MHH.
Author contributions
Conception and design: K Hussein, H Kreipe, M Suttorp, administrative support: H Kreipe, M Suttorp, provision of study materials and patient data: K Hussein, H Kreipe, M Suttorp, collection and assembly of data: K Hussein, G Göhring, M Suttorp, molecular analysis and immunohistochemistry: A Stucki-Koch, K Hussein, data analysis and interpretation: all authors, manuscript writing: K Hussein, M Suttorp, final approval of manuscript: all authors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Leukaemia website
Rights and permissions
About this article
Cite this article
Hussein, K., Stucki-Koch, A., Göhring, G. et al. Increased megakaryocytic proliferation, pro-platelet deposition and expression of fibrosis-associated factors in children with chronic myeloid leukaemia with bone marrow fibrosis. Leukemia 31, 1540–1546 (2017). https://doi.org/10.1038/leu.2017.73
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2017.73
This article is cited by
-
Cancer non-stem cells as a potent regulator of tumor microenvironment: a lesson from chronic myeloid leukemia
Molecular Biomedicine (2021)
-
Profile of fibrosis-related gene transcripts and megakaryocytic changes in the bone marrow of myelodysplastic syndromes with fibrosis
Annals of Hematology (2018)