Abstract
The C-type lectin dectin-1 binds to yeast and signals through the kinase Syk and the adaptor CARD9 to induce production of interleukin 10 (IL-10) and IL-2 in dendritic cells (DCs). However, whether this pathway promotes full DC activation remains unclear. Here we show that dectin-1–Syk–CARD9 signaling induced DC maturation and the secretion of proinflammatory cytokines, including IL-6, tumor necrosis factor and IL-23, but little IL-12. Dectin-1-activated DCs 'instructed' the differentiation of CD4+ IL-17-producing effector T cells (TH-17 cells) in vitro, and a dectin-1 agonist acted as an adjuvant promoting the differentiation of TH-17 and T helper type 1 cells in vivo. Infection with Candida albicans induced CARD9-dependent TH-17 responses to the organism. Our data indicate that signaling through Syk and CARD9 can couple innate to adaptive immunity independently of Toll-like receptor signals and that CARD9 is required for the development of TH-17 responses to some pathogens.
Similar content being viewed by others
Main
CD4+ T cells are the main regulators of adaptive immunity. Responses by interferon-γ (IFN-γ)–producing CD4+ T helper type 1 (TH1) cells promote immunity to viruses, intracellular bacteria and protozoan parasites, whereas TH2 cells making interleukin 4 (IL-4), IL-5 and IL-13 direct immunity to metazoan parasites1,2. Immunopathology is also often associated with particular classes of CD4+ effector T cells: TH2 cells are important in allergy, and TH1 cells have been thought to drive autoimmunity. The last conclusion has been called into question by the finding that defects in IFN-γ signaling exacerbate autoimmune disease in some mouse models3. It is now recognized that many autoimmune diseases previously attributed to TH1 cells are driven by a third class of effector CD4+ T cells that produce IL-17 rather than IFN-γ and are therefore called 'TH-17' cells3,4. IL-17 and/or its receptor have also been linked to resistance to infection by extracellular bacteria such as Klebsiella pneumoniae as well as by fungi such as Candida albicans5,6. However, the mechanisms leading to the generation of TH-17 cells during infection remain poorly understood.
The differentiation of TH1 or TH-17 cells is determined by exposure to IFN-γ or to transforming growth factor-β (TGF-β) and IL-6, respectively7,8,9,10. These cytokines act on newly primed CD4+ T cells to induce expression of the transcription factor T-bet, which promotes TH1 responses11, or RORγt, a transcription factor required for the differentiation of TH-17 cells12. T-bet and RORγt control expression of the IL-12 and IL-23 receptors, respectively12,13, and render T cells susceptible to IL-12 or IL-23, cytokines that sustain and amplify the TH cell differentiation process. The critical importance of these cytokines is emphasized by the fact that mice lacking IL-12 or IL-23 cytokine subunits are unable to mount TH1 or TH-17 responses, respectively3. IL-12, IL-23 and other factors that influence T cell effector fate are produced by dendritic cells (DCs) that have been activated by signals from pattern-recognition receptors (PRRs), which recognize components of microbes or viruses14. Members of the Toll-like receptor (TLR) family have been linked to the induction of IL-12 production by DCs and the initiation of TH1 responses15. Whether other pattern-recognition pathways control alternative forms of TH cell differentiation is not clear.
An alternative pattern-recognition pathway initiated by the engagement of a C-type lectin, dectin-1, by fungal β-glucans has been described16. Dectin-1 signals through a 'hemITAM' motif, an immunoreceptor tyrosine-based activation motif–like sequence containing a single 'YxxL' motif (where 'x' is any amino acid)16, that becomes phosphorylated by Src family kinases after receptor engagement17. This allows recruitment of the spleen tyrosine kinase Syk, which then activates 'downstream' signaling components, including the transcription factor NF-κB16,17,18. Activation of NF-κB by dectin-1 requires the CARMA1-related adaptor protein CARD9, which binds the adaptors MALT1 and Bcl-10 and promotes activation of the IKK kinase complex18.
Dectin-1–Syk signaling in DCs has thus far been associated only with the production of IL-10 and IL-2 (ref. 16), a cytokine pattern not generally associated with the induction of TH cell responses. Therefore, it remains unclear whether dectin-1 acts in a way similar to TLRs, allowing the 'translation' of innate information into adaptive immunity or, alternatively, whether it acts mainly to modulate signals from other PRRs. Here we show that dectin-1–Syk–CARD9 signaling promoted DC maturation and induced the secretion of proinflammatory cytokines, including IL-23, but little IL-12. Notably, DCs activated by dectin-1 engagement strongly biased TH cell differentiation to a TH-17 fate, and the use of dectin-1 agonists as adjuvants promoted TH-17 and TH1 responses in vivo. Furthermore, TH-17 cells developed naturally during experimental infection with C. albicans in wild-type but not Card9−/− mice. Thus, Syk-CARD9–coupled innate signaling pathways may promote DC activation independently of TLRs and may regulate TH-17 responses to certain infections.
Results
Dectin-1–Syk–CARD9 signaling activates DCs
Zymosan, a β-glucan-containing preparation of yeast cell walls, is widely used for 'probing' dectin-1-mediated innate responses. However, zymosan-induced production of IL-10 and IL-2 is almost normal in dectin-1-knockout DCs, indicating receptor redundancy19,20 (data not shown). We therefore sought to identify a selective dectin-1 agonist. Curdlan, a pure β-glucan that has been shown to stimulate DCs deficient in the TLR adaptor MyD88 (Myd88−/− DCs)21, elicited much more production of IL-10 and IL-2 from bone marrow–derived DCs (BMDCs) than did a selection of TLR agonists 'titrated' to induce similar quantities of IL-6 (Supplementary Fig. 1 online). Notably, IL-10 and IL-2 production was mostly independent of the TLR adaptors MyD88 and TRIF but was dependent on dectin-1, Syk and CARD9, suggesting that curdlan acts as a selective agonist of the dectin-1 signaling pathway (Fig. 1). We therefore used curdlan to delineate the consequences of dectin-1–Syk–CARD9 signaling on DC phenotype and function.
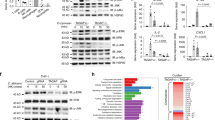
ELISA of IL-10 and IL-2 production by BMDCs of various genotypes after stimulation with curdlan, CpG and/or LPS. (a) C57BL/6 wild-type (WT) or dectin-1-knockout (Dectin-1 KO) BMDCs left unstimulated (Unstim) or stimulated with curdlan or CpG. (b) C57BL/6 wild-type or Myd88−/− BMDCs stimulated with various amounts of curdlan (horizontal axis). (c) C57BL/6 wild-type or MyD88-TRIF–double-knockout (MyD88-TRIF DKO) BMDCs left unstimulated or stimulated with curdlan (Curdl), CpG or lipopolysaccharide (LPS). (d,e) C57BL/6 wild-type or Syk−/− BMDCs (d) or Card9−/− or Card9+/− BMDCs (e) stimulated with various amounts of curdlan (horizontal axis). Data are the mean ± s.d. of triplicate stimulations and are representative of two to six independent experiments.
Curdlan stimulation induced rapid Syk-dependent phosphorylation of the mitogen-activated protein kinases p38, Erk and Jnk and activation of NF-κB in BMDCs (Fig. 2). Consistent with the fact that mitogen-activated protein kinases and NF-κB regulate the expression of genes involved in the innate response, curdlan stimulation also led to Syk-dependent but MyD88-independent upregulation of the CD86, CD40 and CD80 surface proteins, similar to that achieved by stimulation through the TLR9-MyD88 pathway with CpG oligodeoxynucleotides (Fig. 3a,b). In addition, curdlan stimulation led to the production of large quantities of proinflammatory cytokines, including IL-6, tumor necrosis factor (TNF) and IL-12p40 (a subunit of both IL-12 and IL-23; Fig. 3c–e). Notably, most of the DCs that produced IL-12p40 in response to curdlan simultaneously produced TNF and IL-6, whereas DCs producing only IL-12p40 predominated after CpG stimulation (Fig. 3f and data not shown). Induction of IL-12p40 by curdlan was accompanied by the production of transcripts encoding IL-12p19 (a subunit of IL-23) and secretion of IL-23 protein; however, in contrast to CpG stimulation, curdlan elicited little production of transcripts encoding IL-12p35 (a subunit of IL-12) or IL-12p70 protein (Fig. 3g and Supplementary Fig. 2 online). Cytokine induction by curdlan was independent of MyD88 but depended on dectin-1, Syk and CARD9 (Fig. 3c–e,g and Supplementary Fig. 2). In contrast, CpG-induced cytokine production was dependent on MyD88 and independent of Syk, except for the production of IL-12p35 and IL-12p70, which was dependent on both MyD88 and Syk (Fig. 3g and Supplementary Fig. 2).
(a) Analysis of the activation of p38, Erk and Jnk by immunoblot of lysates of C57BL/6 wild-type or Syk−/− BMDCs stimulated with curdlan or CpG (time, above lanes), assessed with antibodies to phosphorylated forms of the kinases (p-), followed by reprobing of blots for total kinase content (loading control). (b) Luciferase assay of NF-κB activation in protein extracts from a. RLU, relative light units. Data are representative of at least two independent experiments.
(a,b) Flow cytometry for surface expression of CD86, CD40 and CD80 on C57BL/6 BMDCs after no stimulation or stimulation for 24 h with curdlan or CpG (a) or on C57BL/6 wild-type, Myd88−/− or Syk−/− BMDCs left unstimulated or stimulated with curdlan or CpG (b). (c–e) ELISA of supernatants of C57BL/6 wild-type or dectin-1-knockout BMDCs left unstimulated or stimulated with curdlan or CpG (c); C57BL/6 wild-type, Myd88−/− or Syk−/− BMDCs left unstimulated or stimulated with 10 or 100 μg/ml of curdlan or with 50 or 500 ng/ml of CpG (d); or Card9+/− or Card9−/− BMDCs left unstimulated or stimulated with 10 or 100 μg/ml of curdlan or with 5 μg/ml of CpG (e). (f) Flow cytometry of intracellular cytokine expression by C57BL/6 wild-type BMDCs stimulated with curdlan or CpG. Numbers in quadrants indicate percent cells in each. (g) ELISA of cytokine production by C57BL/6 wild-type, Myd88−/− or Syk−/− BMDCs stimulated with 10 or 100 μg/ml of curdlan or with 50 or 500 ng/ml of CpG. Wedges (d,e,g) indicate increasing concentrations of reagent. Data are the mean ± s.d. of triplicate stimulations (c–e,g) and are representative of two to six independent experiments.
As an alternative approach to examine the effects of dectin-1 signaling, we transduced BMDCs with retroviruses encoding dectin-1 molecules bearing a streptavidin-binding peptide tag17 and stimulated the cells with streptavidin-sepharose. Streptavidin-sepharose triggered phenotypic maturation of and cytokine production by BMDCs expressing full-length dectin-1 but not those expressing a signaling-deficient dectin-1 mutant (Fig. 4). Those responses were unaffected by lack of MyD88 and TRIF, which excluded the possibility of a contribution by contaminating TLR agonists and confirmed that triggering of dectin-1 alone was sufficient for DC activation. We conclude that, like TLR signaling, selective triggering of the dectin-1–Syk–CARD9 signaling pathway in DCs induces activation but results in an altered cytokine profile characterized by large amounts of IL-2, IL-10, IL-6 and TNF and a bias in production of IL-23 rather than IL-12.
(a) Flow cytometry of CD40 surface expression by C57BL/6 wild-type or MyD88-TRIF double-knockout BMDCs transduced with retrovirus encoding a streptavidin-binding peptide–tagged version of wild-type (WT) or mutant (Y15F) dectin-1 and then left unstimulated or stimulated for 24 h with streptavidin-sepharose (Strep-seph). MFI, mean fluorescence intensity. (b) ELISA of TNF, IL-6 and IL-12 p40 in supernatants of the cells in a. SPB, streptavidin-binding peptide. Data are the mean ± s.d. of triplicate stimulations and are representative of two to four independent experiments.
Dectin-1-activated DCs prime TH1 and TH-17 cells
To assess whether dectin-1–stimulated DCs can 'instruct' CD4+ T cell proliferation and effector differentiation, we cultured ovalbumin-specific OT-II CD4+ T cells with antigen and BMDCs in the presence of curdlan or CpG. Both curdlan and CpG led to more T cell proliferation than did antigen alone (data not shown). However, whereas CpG induced differentiation skewed mainly toward the generation of IFN-γ-producing TH1 cells, the presence of curdlan also led to the accumulation of IL-17-producing T cells (Fig. 5a). Compared with a range of specific TLR agonists, curdlan and, to a lesser extent, zymosan, induced a much higher ratio of IL-17 production to IFN-γ production (Supplementary Fig. 3 online). Neither stimulus induced the development of IL-4-producing T cells (data not shown). The effect of curdlan and CpG was mediated by the antigen-presenting cells and not the T cells, as the effect was abrogated by the use of BMDCs lacking Syk or MyD88, respectively (Fig. 5b). In addition, the cytokine bias induced by curdlan versus CpG was not simply a reflection of quantitative differences in DC activation, as 'titration' of either compound did not allow interconversion of its effect (Supplementary Fig. 4 online).
(a) Flow cytometry of intracellular cytokine production by total CD4+ OT-II T cells cultured with C57BL/6 wild-type BMDCs and ovalbumin protein plus curdlan or CpG. Numbers in quadrants indicate percent gated CD4+ T cells in each after restimulation. Cells producing IFN-γ and IL-17 did not express the lineage marker Foxp3 (data not shown). (b) ELISA of cytokines in supernatants of total CD4+ OT-II T cells cultured together with C57BL/6 wild-type, Myd88−/− or Syk−/− BMDCs and ovalbumin peptide plus curdlan or CpG, evaluated after restimulation. (c) ELISA of cytokines in supernatants of restimulated CD4+CD25− OT-II T cells that had been cultured together with C57BL/6 wild-type BMDCs and ovalbumin protein plus curdlan together with CD4+CD25+ OT-II Treg cells at various ratios (horizontal axis). (d) Real-time RT-PCR analysis of transcripts encoding IL-17A, IL-17F and RORγt in CD4+CD25− OT-II T cells 5 d after culture with C57BL/6 wild-type BMDCs and ovalbumin peptide plus curdlan or CpG, with (+ Treg cells) or without (− Treg cells) the addition of CD4+CD25+ OT-II Treg cells. (e–h) ELISA of cocultures as described in b but with the addition of anti-TGF-β (α-TGF-β) on day 0 (e); increasing concentrations (wedge) of recombinant TGF-β (f); anti-IL-23p19 (α-IL-23p19) or isotype control antibody (Isotype) on days 0 and 3 (g); or anti-TNF (α-TNF) on day 0 (h). Data are the mean ± s.d. of triplicate (b,c,e–h) or duplicate (d) cultures and are representative of two to four independent experiments.
Notably, depleting the OT-II CD4+ T cell preparation of CD25+ regulatory T cells (Treg cells) led to the differentiation of TH1 cells even in the presence of curdlan (Fig. 5c). As reported for TLR-stimulated DCs8, only when Treg cells were 'added back' to the starting T cell population did the IFN-γ-dominated response subside and IL-17-producing cells emerge (Fig. 5c and Supplementary Fig. 3). Similarly, we detected transcripts encoding IL-17A, IL-17F and RORγt only in curdlan-containing cultures when Treg cells were present (Fig. 5d). The effect of Treg cells was not simply to prevent TH1 cell differentiation, as it could not be mimicked by the neutralization of IFN-γ (Supplementary Fig. 5 online). Instead, as reported before8, Treg cells served at least in part as a source of TGF-β; their effect could be blocked by antibody to TGF-β (anti-TGF-β) and could be mimicked, albeit only partially, by exogenous TGF-β (Fig. 5e,f). The differentiation of TH-17 cells induced by curdlan and Treg cells was also dependent on IL-23 and TNF, as this differentiation was blocked by antibodies neutralizing either cytokine (Fig. 5g,h). Finally, the addition of excess IL-12p70 prevented the differentiation of TH-17 cells induced by curdlan-stimulated DCs, whereas the addition of IL-23 led to TH-17 skewing in cultures of CpG-stimulated DCs (Supplementary Fig. 6 online). We conclude that DCs stimulated with curdlan can bias the differentiation of CD4+ T cells toward a TH-17 fate through a pathway requiring Treg cells and involving TGF-β, TNF and IL-23.
Dectin-1 agonists are adjuvants for TH1 and TH-17 priming
To assess whether dectin-1 stimulation also leads to the induction of TH-17 responses in vivo, we tested curdlan as an adjuvant. Adoptively transferred OT-II cells proliferated more extensively in response to antigen mixed with curdlan or CpG than in response to antigen alone (Fig. 6a). Cells from draining lymph nodes of mice that had received antigen and CpG produced considerable IFN-γ but little IL-17 after restimulation with antigen in vitro (Fig. 6b). In contrast, substantial IL-17, as well as IFN-γ, was produced by cells from mice immunized with antigen and curdlan (Fig. 6b,c). Intracellular cytokine staining showed the presence of TH1 and TH-17 cells, which existed together as separate populations (data not shown). Notably, the TH-17 and TH1 responses induced by antigen and curdlan in vivo were dependent on dectin-1, as they were abrogated in chimeric mice containing dectin-1-knockout hematopoietic cells (Fig. 6c). In contrast, the TH1 response induced by CpG was unaffected by dectin-1 deficiency (data not shown). Consistent with the finding that curdlan and CpG induced TH1 cells, both stimuli triggered the production of ovalbumin-specific immunoglobulin G2c (IgG2c) antibodies (Fig. 6d). However, curdlan also promoted the production of high titers of ovalbumin-specific IgG1 antibodies (Fig. 6d). In addition, mice that received curdlan developed anti-β-glucan IgM, which could be used to stain C. albicans yeast (Supplementary Fig. 7 online). We conclude that selective engagement of dectin-1 in vivo is able to link innate immunity with the induction of T cell and B cell responses.
(a) CFSE dilution analysis of OT-II T cells from the spleens of mice immunized with egg white (OVA(egg)) alone or in combination with curdlan or CpG. (b) ELISA of cytokine production by cells isolated from draining popliteal lymph nodes (DR) and nondraining lymph nodes (NDR) from mice that received OT-II T cells and then were immunized as described in a (below graph); cells were left unstimulated (Medium) or were restimulated with egg white (key). (c) ELISA of cytokine production by cells from wild-type recipients of dectin-1 wild-type bone marrow (WT → WT) or dectin-1-knockout bone marrow (WT → KO), immunized with egg white and increasing amounts (wedges) of curdlan and restimulated as described in b. (d) ELISA of ovalbumin-specific IgG2c and IgG1 in serum from wild-type mice at day 14 after two immunizations (day 0 and day 7) as described in a (horizontal axis). Data are mean ± s.d. of duplicate restimulations (b,c) or of two to three mice per group (d) and are representative of at least three independent experiments.
CARD9 regulates TH-17 responses to C. albicans
Finally, we sought to determine whether CD4+ TH-17 cell responses are induced during fungal infection and to what extent this depends on the dectin-1–Syk–CARD9 signaling pathway. Large amounts of IFN-γ and IL-17 were produced by CD4+ spleen cells from mice infected with C. albicans after restimulation with heat-killed organisms (Fig. 7a). Dectin-1 was redundant for this response (data not shown), consistent with the fact that it is also not essential for DC responses to zymosan19,20. In contrast, CARD9 was indispensable for the TH-17 response and partially contributed to the TH1 response (Fig. 7b). We conclude that adaptive immune responses to C. albicans infection include the induction of TH-17 cells and that this process is dependent on innate signaling via CARD9.
(a) ELISA of IFN-γ and IL-17 production by total splenocytes (Total spleen) or splenocyte samples depleted of CD4+ cells (CD4+ depl); cells were obtained from wild-type mice infected with C. albicans and were restimulated with heat-killed organisms. (b) ELISA of IFN-γ and IL-17 production by total splenocytes from Card9−/− or Card9+/− mice infected with C. albicans before restimulation of cells with heat-killed organisms. Each symbol represents one mouse (mean of triplicate restimulations); horizontal bars, median. *, P < 0.05; **, P < 0.01; ***, P < 0.001. Data are from six to fourteen mice per group pooled from three independent experiments.
Discussion
Pattern recognition is critical for the mobilization of defense mechanisms after invasion by potential pathogens14. In addition to stimulating the microbicidal effector functions of myeloid cells, some classes of PRRs can signal to regulate the expression of genes involved in the innate response and to facilitate the induction of adaptive immune responses by DCs15. However, of the many possible PRRs expressed at the cell surface, only the TLR family members have been conclusively proven to generate immunogenic DCs. Here we have added Syk-coupled C-type lectin PRRs to that list and have shown that dectin-1 signaling through the Syk-CARD9 pathway induced the maturation of DCs into effector antigen-presenting cells capable of eliciting the differentiation of TH-17 and TH1 cells. Furthermore, we have shown that the same signaling pathway was critical for the development of TH-17 responses during infection with C. albicans. Thus, our results identify the Syk-CARD9 axis as a TLR-independent innate signaling pathway for activating DCs that is nonredundant for directing potent TH-17 responses to infection.
Dectin-1 signaling in DCs resulted in maturation and the production of a distinct combination of cytokines, including considerable IL-2, IL-10, TNF and IL-23. All DC responses to dectin-1 agonists were strictly dependent on Syk, distinguishing them from responses to TLR signals, which are independent of Syk. One apparent exception was the induction of IL-12p35 and IL-12p70 by CpG, which seemed to be dependent on Syk. IL-12p35 production is regulated at many levels and is strongly enhanced by synergistic interaction between different TLRs, costimulation by IFN-γ or CD40 ligand, or type I interferon receptor signaling22. The Syk dependence of the production of IL-12p35 and IL-12p70 in response to CpG may therefore indicate involvement of a Syk-coupled cellular receptor that can act in synergy with TLR9 for IL-12p35 induction. In addition, dectin-1 signaling for cytokine production was dependent on CARD9, again distinguishing it from TLR signaling, which is CARD9 independent18,23. The CARD9 dependence of cytokine induction is consistent with the importance of this adaptor in coupling dectin-1–Syk signals to NF-κB activation18. However, CARD9 has also been associated with linking signaling by the receptor Nod2 to activation of p38 and Jnk23. It is therefore possible that CARD9 also coordinates activation of the mitogen-activated protein kinase cascade 'downstream' of dectin-1–Syk. Experiments with curdlan stimulation of CARD9-deficient cells will help address this issue.
TLR stimulation of DCs can induce TH-17 responses8, but activation through the dectin-1–Syk–CARD9 pathway induced greater TH-17 skewing. However, in both cases the mechanism involved was similar, being dependent on the presence of Treg cells and requiring TGF-β8. This is consistent with reports suggesting that TGF-β (in concert with IL-6) acts in the first step of TH-17 instruction8,9,10 and that IL-23 acts secondarily to support the proliferation and differentiation of TH-17 cells24,25. DCs stimulated through the dectin-1–Syk–CARD9 pathway had a propensity to produce IL-23 rather than IL-12. The lack of IL-12, together with the production of IL-10, may limit TH1 skewing, thereby diminishing the amount of negative feedback on TH-17 cell differentiation. Indeed, the addition of IL-12p70 abrogated the induction of TH-17 cells by curdlan-stimulated DCs, probably because IL-12 boosts the differentiation of TH1 cells, which produce IFN-γ and inhibit the differentiation of TH-17 cells26,27. However, the IL-23–versus–IL-12p70 balance is not sufficient to explain the effect of curdlan, as, for example, Syk−/− DCs stimulated with CpG, which also make IL-23 but little IL-12p70, elicited little TH-17 cell differentiation. In this context, the finding that DCs produce large quantities of TNF, IL-12p40 and IL-6 after curdlan stimulation is notable, as IL-23, TNF and IL-6 all have synergistic effects on the induction of TH-17 cells8. Consistent with that idea, blockade of TNF or IL-23 decreased the curdlan-dependent differentiation of TH-17 cells. Notably, even though zymosan induces TGF-β production by macrophages28 and DCs can secrete TGF-β8,29, the amount of TGF-β induced by curdlan alone was insufficient to promote the differentiation of TH-17 cells in the absence of Treg cells. Treg cells act by providing TGF-β or signals that potentiate the ability of DCs to secrete this cytokine8. In addition, curdlan-stimulated DCs produce considerable IL-2, which might help maintain Treg cell function and establish a positive feedback loop30,31. The combination of all these factors may explain why DCs stimulated through the dectin-1–Syk–CARD9 pathway were more efficient than TLR-stimulated DCs at inducing the differentiation of TH-17 cells.
The importance of adaptive immunity in protection from C. albicans is emphasized by the notable susceptibility of immunodeficient patients to this otherwise nonpathogenic commensal organism32. Furthermore, protective T cell responses to Aspergillus fumigatus33,34,35 are partially MyD88 independent36, consistent with the possibility that many antifungal responses may be induced through the Syk-CARD9 pathway. However, the induction of TH-17 responses to fungal infection has not been reported before to our knowledge, even though both TGF-β and IL-17 are critical for resistance to C. albicans infection6,37. How TH-17 cells might contribute to fungal clearance is unknown, but it is notable that IL-17 is a potent recruitment factor for neutrophils and that neutropenia is a chief risk factor for invasive candidiasis38. Notably, the induction of TH-17 cells through the Syk-CARD9 pathway may also explain why subclinical fungal infections and fungal β-glucans precipitate disease in mouse models of rheumatoid arthritis21,39 and other autoimmune diseases40,41. How this conforms with the observation that zymosan can also promote immunological tolerance is unclear28.
The finding that dectin-1–Syk–CARD9 signaling in DCs acts as an autonomous pattern-recognition pathway capable of linking the innate and adaptive immune system has notable implications. It is becoming increasingly apparent that dectin-1 is not the only C-type lectin that can signal by means of Syk42. The possibility that other Syk-coupled receptors act as PRRs in myeloid cells could help explain the development of TH-17 responses not only during infection with fungi but also during infection with extracellular bacteria such as K. pneumoniae and Citrobacter rodentium5,9. All of these organisms engage many receptors, in particular those of the TLR family, so it will be useful to study how signaling by means of C-type lectins is integrated with signaling from other PRRs42. Nevertheless, the identification of a PRR family that accomplishes a function analogous to that of TLRs but more is powerful in 'instructing' TH-17 cell development reinforces the idea that innate recognition is central to immune regulation and opens the possibility for therapeutic intervention. Thus, agonists of the Syk-CARD9 pathway might be useful in vaccine development, whereas antagonists might find a place in the treatment of immunopathology. Finally, the central function of Syk in DC activation by means of C-type lectin PRRs raises the issue of whether other receptors that engage Syk in myeloid cells, such as TREM proteins43, Fc receptors44 and integrins45, can also couple innate and adaptive immunity. Syk coupling by myeloid receptors could therefore extend the function of immunoreceptor tyrosine-based activation motif signaling, the central pivot of adaptive immunity, to the earlier step of innate recognition42.
Methods
Mice.
C57BL/6 mice were from Charles River. Mice lacking both MyD88 and TRIF were generated by intercrossing of MyD88-knockout and TRIF-knockout mice. OT-II TCR-transgenic mice on a B6.SJL background (congenic CD45.1+) were generated by intercrossing of OT-II TCR-transgenic mice on C57BL/6 background with B6.SJL mice. All of these mice, as well as MyD88-knockout, TRIF-knockout and OT-II TCR-transgenic mice on a C57BL/6 background, were bred at Cancer Research UK in specific pathogen–free conditions. Dectin-1-knockout mice19 were bred at the University of Cape Town, South Africa. CARD9-knockout mice18 were bred at the Technische Universität München, Germany. Radiation chimeras were generated as described16. All animal experiments were in accordance with national and institutional guidelines for animal care.
Reagents.
Culture medium was RPMI 1640 medium supplemented with glutamine, penicillin, streptomycin, 2-mercaptoethanol (all from Invitrogen) and 10% (vol/vol) heat-inactivated FCS (Bioclear). Curdlan (Wako) was suspended in PBS at a concentration of 10 mg/ml. Zymosan, MALP2, FSL and Pam3CSK4 were from Invivogen. CpG oligonucleotide 1668 was synthesized by Sigma. Streptavidin-sepharose was from GE Healthcare. Ovalbumin peptide (residues 323–339) was synthesized and purified by high-performance liquid chromatography at Cancer Research UK. Ovalbumin protein used for in vitro assays was from Calbiochem, and sterile-filtered egg white for in vivo use was prepared as described46. The amount of egg white presented here always represents the ovalbumin equivalent. Granulocyte-macrophage colony-stimulating factor (GM-CSF) was made by the Cancer Research UK protein purification service and batches were 'titrated' to produce optimal growth conditions for BMDCs. Antibodies used for flow cytometry were from BD Pharmingen and included those specific for CD11c (clone HL3), CD86 (GL1), CD80 (16-10A1), CD40 (3/23), CD4 (RM4-5), CD25 (PC61), CD45.1 (A20), IFN-γ (XMG1.2) and IL-17 (TC11-18H10.1). Neutralizing antibodies were anti-TGF-β (1D11; R&D Systems), anti-p19 (G23.8; eBioscience), anti-TNF (MP6-XT3; BD Pharmingen) and anti-IFN-γ (XMG1.2; BD Pharmingen). Purified 2.4G2 (anti-FcγRIII/II used to block nonspecific antibody binding) was from the Cancer Research UK antibody production service. Antibodies used for immunoblot analysis were rabbit polyclonal antibodies, except the p38-specific antibody (L53F8), and were from Cell Signaling.
BMDC culture and stimulation.
BMDCs were generated as described47, and DCs were purified from bulk cultures with anti-CD11c microbeads before use (Miltenyi Biotec). BMDC purity was checked by flow cytometry and was routinely over 98% (data not shown). For expression of streptavidin-binding peptide–tagged dectin-1 (ref. 17) in BMDCs, the streptavidin-binding peptide tag48 was fused to the carboxyl terminus of wild-type dectin-1 or dectin-1 with a substitution in its signaling domain (Y15F) and was cloned into the retroviral vector pFB-IRES-GFP. Retrovirus production and BMDC infection were done as described49. Of the CD11c+ cells, 80–95% were routinely positive for green fluorescent protein (data not shown). For analysis of cytokine production and surface marker expression, 5 × 104 to 10 × 104 BMDCs per well were cultured for 18–24 h in 96-well round-bottomed plates in 200 μl culture medium containing GM-CSF in the presence of curdlan (100 μg/ml), CpG (500 ng/ml) and/or lipopolysaccharide (50 ng/ml) or as described in the legends to Figures 1b,d,e and 3d,e,g. Streptavidin-sepharose was used at a concentration of 25 μl/ml. All stimuli were 'pretitrated' and were used near their optimal concentration, as determined by induction of maximum cytokine production and DC maturation. Cytokines in the supernatants were measured by sandwich ELISA. For RNA isolation, 4 × 105 BMDCs per well were cultured for 3 h in 48-well plates in 0.5 ml culture medium containing GM-CSF and various stimuli as described in the legend to Supplementary Figure 2. For biochemical assays, 1 × 106 to 2 × 106 BMDCs per well were cultured overnight in 24-well plates in 1 ml culture medium containing GM-CSF before stimulation for various times with or without curdlan (500 μg/ml) or CpG (10 μg/ml).
Flow cytometry.
Cell suspensions were stained in ice-cold PBS supplemented with 2 mM EDTA, 1% (vol/vol) FCS and 0.02% (wt/vol) sodium azide. For intracellular cytokine staining, cells were stained with anti-CD4 or anti-CD11c, were fixed with Fix and Perm Reagent A (Caltag Laboratories) and then were resuspended in Fix and Perm Reagent B (Caltag Laboratories) containing labeled antibodies. Data were acquired on a FACSCalibur (BD Biosciences) and were analyzed with FlowJo software (TreeStar).
RNA isolation and real-time RT-PCR.
Total RNA was prepared with TRIzol reagent (Invitrogen). The cDNA was synthesized from total RNA with random hexamers and Superscript II reverse transcriptase (Invitrogen). Quantitative real-time PCR was accomplished with SYBR Green incorporation (for transcripts encoding IL-17A, IL-17F, RORγt, IL-23p19, IL-2, IL-6 and TNF) or Taqman (for transcripts encoding IL-12p35, IL-12p40 and IL-10). For SYBR Green reactions, primer sequences were as described12,50,51; for IL-6, primer sequences were as follows: forward, 5′-GTTCTCTGGGAAATCGTGGA-3′; reverse, 5′-TGTACTCCAGGTAGCTATGG-3′. For Taqman reactions, primers and probes were from Applied Biosystems. Measurements were made in duplicate wells with the ABI PRISM 7700 sequence detection system (Applied Biosystems). Results were normalized to those obtained with 18S rRNA (primers and probe from Applied Biosystems) and results are presented as relative quantities of mRNA.
Immunoblot analysis and NF-κB assay.
Cells were collected by being scraped into ice-cold PBS supplemented with 5 mM EDTA. After centrifugation, the cell pellet was lysed for 30 min on ice with buffer (50 mM Tris, pH 7.5, 1% (vol/vol) Nonidet-P40, 0.5% (wt/vol) deoxycholic acid, 0.1% (wt/vol) SDS, 150 mM NaCl, 10 mM NaF, 1 mM Na3VO4 and 2 mM Na4P2O7, plus a mixture of protease inhibitors; Roche Molecular Biochemicals). Cell debris were removed by centrifugation and extracts were quantified by protein assay (Bio Rad). For immunoblot analysis, a fixed amount of total protein was mixed with sample buffer (0.125 M Tris, pH 6.8, 4% (wt/vol) SDS, 20% (vol/vol) glycerol, 5% (vol/vol) 2-mercaptoethanol) and was resolved by SDS-PAGE (4–20% acrylamide gradient, Tris-glycine; Invitrogen). After transfer to a polyvinyldifluoride membrane (Millipore), proteins were analyzed by immunoblot and were visualized by enhanced chemiluminescence (Pierce). NF-κB was measured in the extracts by analysis of a fixed amount of total protein with the NF-κB p65 transcription factor assay kit according to the manufacturer's instructions (Pierce).
In vitro T cell differentiation.
CD4+ T cells from the lymph nodes of OT-II mice (C57BL/6 background) were purified by a two-step procedure with MACS beads (Miltenyi Biotec), which included depletion of antigen-presenting cells followed by enrichment for CD4+ cells. Alternatively, CD4+CD11c−CD25− and CD4+CD11c−CD25+ cells were sorted from the spleens of OT-II mice (C57BL/6 background) by flow cytometry with a MoFlo (Dako Cytomation) or a FACSAria (BD Biosciences). Purified OT-II T cells (5 × 104) were cultured together with BMDCs (1 × 104) and 10–50 μg/ml of ovalbumin protein or 2–10 nM ovalbumin peptide (residues 323–339) in the presence or absence of curdlan (50 μg/ml) or CpG (0.5 μg/ml) in complete culture medium further supplemented with sodium pyruvate, nonessential amino acids and HEPES (all from Invitrogen). In some experiments, neutralizing antibodies (10 μg/ml) or recombinant cytokines (TGF-β, 1-10 ng/ml (Sigma); IL-12 p70, 5 ng/ml (Biosource); IL-23, 10 ng/ml (eBioscience)) were added. Cultures were split at a ratio of 1:2 on day 3 and were restimulated on day 5 for 5 h with phorbol 12-myristate 13-acetate (10 ng/ml; Sigma), ionomycin (1 μg/ml; Calbiochem) and GolgiStop (BD Pharmingen), and intracellular cytokines were analyzed by flow cytometry. Alternatively, the entire content of each well was restimulated on day 5 on plate-bound anti-CD3ε (Cancer Research UK antibody production service) for 48 h before cytokines in the supernatant were analyzed by sandwich ELISA.
Immunizations.
Naive C57BL/6 mice were immunized intraperitoneally with 5 mg curdlan alone or with 50 μg egg white plus 2 mg curdlan or 5 μg CpG or were immunized in the footpads with 3 μg egg white plus 50–500 μg curdlan or 0.5–2.5 μg CpG. For T cell differentiation assays, CD4+ OT-II populations (from OT-II mice on B6.SJL background; 1 × 106 to 4 × 106 cells per mouse), depleted of antigen-presenting cells and labeled with CFSE, were transferred into host mice by intravenous injection 1 d before immunization. CFSE dilution of CD4+CD45.1+ spleen cells was analyzed by flow cytometry 3 d after immunization. Alternatively, 1 × 106 to 2 × 106 total popliteal lymph node cells were restimulated for 48 h with egg white before cytokines in the supernatant were measured by sandwich ELISA.
Infection.
Card9−/− mice and Card9+/− control mice were infected intravenously with 4 × 103 to 1.2 × 104 colony-forming units of C. albicans strain SC5314. On days 6–8 after infection, mice were killed and total splenocytes or splenocyte samples depleted of CD4+ cells (2 × 106 cells per well) were restimulated in 96-well U-bottomed plates with heat-inactivated C. albicans (1 × 106 to 1 × 108 per ml). After 48 h, IFN-γ and IL-17 in the supernatants were measured by sandwich ELISA.
Antibody measurement.
Relative titers of ovalbumin-specific IgG2c and IgG1 in serum samples from experimental mice were measured by capture ELISA with anti–mouse IgG1 (BD Pharmingen, clone A85-1) or anti–mouse IgG2c (Jackson Immunoresearch) on plates coated with ovalbumin protein. The β-glucan-specific immunoglobulins were detected by ELISA with anti–mouse immunoglobulin (Jackson Immunoresearch) and plates coated with curdlan made soluble in NaOH. For staining of C. albicans, heat-inactivated yeast cells were incubated with diluted serum followed by anti–mouse immunoglobulin. Confocal images were acquired on a Zeiss LSM510 microscope.
Statistics.
Statistical significance was determined by a two-tailed unpaired t-test with Graphpad Prism (GraphPad Software).
Note: Supplementary information is available on the Nature Immunology website.
References
Sher, A. & Coffman, R.L. Regulation of immunity to parasites by T cells and T cell-derived cytokines. Annu. Rev. Immunol. 10, 385–409 (1992).
Abbas, A.K., Murphy, K.M. & Sher, A. Functional diversity of helper T lymphocytes. Nature 383, 787–793 (1996).
Harrington, L.E., Mangan, P.R. & Weaver, C.T. Expanding the effector CD4 T-cell repertoire: the Th17 lineage. Curr. Opin. Immunol. 18, 349–356 (2006).
Weaver, C.T., Harrington, L.E., Mangan, P.R., Gavrieli, M. & Murphy, K.M. Th17: an effector CD4 T cell lineage with regulatory T cell ties. Immunity 24, 677–688 (2006).
Ye, P. et al. Requirement of interleukin 17 receptor signaling for lung CXC chemokine and granulocyte colony-stimulating factor expression, neutrophil recruitment, and host defense. J. Exp. Med. 194, 519–527 (2001).
Huang, W., Na, L., Fidel, P.L. & Schwarzenberger, P. Requirement of interleukin-17A for systemic anti-Candida albicans host defense in mice. J. Infect. Dis. 190, 624–631 (2004).
Szabo, S.J., Dighe, A.S., Gubler, U. & Murphy, K.M. Regulation of the interleukin (IL)-12Rβ2 subunit expression in developing T helper 1 (Th1) and Th2 cells. J. Exp. Med. 185, 817–824 (1997).
Veldhoen, M., Hocking, R.J., Atkins, C.J., Locksley, R.M. & Stockinger, B. TGFβ in the context of an inflammatory cytokine milieu supports de novo differentiation of IL-17-producing T cells. Immunity 24, 179–189 (2006).
Mangan, P.R. et al. Transforming growth factor-β induces development of the TH17 lineage. Nature 441, 231–234 (2006).
Bettelli, E. et al. Reciprocal developmental pathways for the generation of pathogenic effector TH17 and regulatory T cells. Nature 441, 235–238 (2006).
Szabo, S.J. et al. A novel transcription factor, T-bet, directs Th1 lineage commitment. Cell 100, 655–669 (2000).
Ivanov, I.I. et al. The orphan nuclear receptor RORγt directs the differentiation program of proinflammatory IL-17+ T helper cells. Cell 126, 1121–1133 (2006).
Szabo, S.J., Sullivan, B.M., Peng, S.L. & Glimcher, L.H. Molecular mechanisms regulating Th1 immune responses. Annu. Rev. Immunol. 21, 713–758 (2003).
Janeway, C.A., Jr . Approaching the asymptote? Evolution and revolution in immunology. Cold Spring Harb. Symp. Quant. Biol. 54, 1–13 (1989).
Iwasaki, A. & Medzhitov, R. Toll-like receptor control of the adaptive immune responses. Nat. Immunol. 5, 987–995 (2004).
Rogers, N.C. et al. Syk-dependent cytokine induction by dectin-1 reveals a novel pattern recognition pathway for C type lectins. Immunity 22, 507–517 (2005).
Underhill, D.M., Rossnagle, E., Lowell, C.A. & Simmons, R.M. Dectin-1 activates Syk tyrosine kinase in a dynamic subset of macrophages for reactive oxygen production. Blood 106, 2543–2550 (2005).
Gross, O. et al. CARD9 controls a non-TLR signalling pathway for innate anti-fungal immunity. Nature 442, 651–656 (2006).
Taylor, P.R. et al. A critical role for β-glucan recognition in the control of fungal infection. Nat. Immunol. 8, 31–38 (2007).
Saijo, S. et al. Dectin-1 is required for host defense against Pneumocystis carinii but not against Candida albicans. Nat. Immunol. 8, 39–46 (2007).
Yoshitomi, H. et al. A role for fungal β-glucans and their receptor dectin-1 in the induction of autoimmune arthritis in genetically susceptible mice. J. Exp. Med. 201, 949–960 (2005).
Trinchieri, G. & Sher, A. Cooperation of Toll-like receptor signals in innate immune defence. Nat. Rev. Immunol. 7, 179–190 (2007).
Hsu, Y.M. et al. The adaptor protein CARD9 is required for innate immune responses to intracellular pathogens. Nat. Immunol. 8, 198–205 (2007).
Aggarwal, S., Ghilardi, N., Xie, M.H., de Sauvage, F.J. & Gurney, A.L. Interleukin-23 promotes a distinct CD4 T cell activation state characterized by the production of interleukin-17. J. Biol. Chem. 278, 1910–1914 (2003).
Langrish, C.L. et al. IL-23 drives a pathogenic T cell population that induces autoimmune inflammation. J. Exp. Med. 201, 233–240 (2005).
Harrington, L.E. et al. Interleukin 17–producing CD4+ effector T cells develop via a lineage distinct from the T helper type 1 and 2 lineages. Nat. Immunol. 6, 1123–1132 (2005).
Park, H. et al. A distinct lineage of CD4 T cells regulates tissue inflammation by producing interleukin 17. Nat. Immunol. 6, 1133–1141 (2005).
Dillon, S. et al. Yeast zymosan, a stimulus for TLR2 and dectin-1, induces regulatory antigen-presenting cells and immunological tolerance. J. Clin. Invest. 116, 916–928 (2006).
Morelli, A.E. et al. Cytokine production by mouse myeloid dendritic cells in relation to differentiation and terminal maturation induced by lipopolysaccharide or CD40 ligation. Blood 98, 1512–1523 (2001).
D'Cruz, L.M. & Klein, L. Development and function of agonist-induced CD25+Foxp3+ regulatory T cells in the absence of interleukin 2 signaling. Nat. Immunol. 6, 1152–1159 (2005).
Fontenot, J.D., Rasmussen, J.P., Gavin, M.A. & Rudensky, A.Y. A function for interleukin 2 in Foxp3-expressing regulatory T cells. Nat. Immunol. 6, 1142–1151 (2005).
Hohl, T.M., Rivera, A. & Pamer, E.G. Immunity to fungi. Curr. Opin. Immunol. 18, 465–472 (2006).
Cenci, E. et al. T cell vaccination in mice with invasive pulmonary aspergillosis. J. Immunol. 165, 381–388 (2000).
Cenci, E. et al. Th1 and Th2 cytokines in mice with invasive aspergillosis. Infect. Immun. 65, 564–570 (1997).
Perruccio, K. et al. Transferring functional immune responses to pathogens after haploidentical hematopoietic transplantation. Blood 106, 4397–4406 (2005).
Rivera, A. et al. Innate immune activation and CD4+ T cell priming during respiratory fungal infection. Immunity 25, 665–675 (2006).
Spaccapelo, R. et al. TGF-β is important in determining the in vivo patterns of susceptibility or resistance in mice infected with Candida albicans. J. Immunol. 155, 1349–1360 (1995).
Huffnagle, G.B. & Deepe, J.G.S. Innate and adaptive determinants of host susceptibility to medically important fungi. Curr. Opin. Microbiol. 6, 344–350 (2003).
Hirota, K. et al. T cell self-reactivity forms a cytokine milieu for spontaneous development of IL-17+ Th cells that cause autoimmune arthritis. J. Exp. Med. 204, 41–47 (2007).
Hida, S., Nagi-Miura, N., Adachi, Y. & Ohno, N. Beta-glucan derived from zymosan acts as an adjuvant for collagen-induced arthritis. Microbiol. Immunol. 50, 453–461 (2006).
Veldhoen, M., Hocking, R.J., Flavell, R.A. & Stockinger, B. Signals mediated by transforming growth factor-β initiate autoimmune encephalomyelitis, but chronic inflammation is needed to sustain disease. Nat. Immunol. 7, 1151–1156 (2006).
Robinson, M.J., Sancho, D., Slack, E.C., LeibundGut-Landmann, S. & Reis e Sousa, C. Myeloid C-type lectins in innate immunity. Nat. Immunol. 7, 1258–1265 (2006).
Klesney-Tait, J., Turnbull, I. & Colonna, M. The TREM receptor family and signal integration. Nat. Immunol. 7, 1266–1273 (2006).
Ravetch, J.V. & Bolland, S. IgG Fc receptors. Annu. Rev. Immunol. 19, 275–290 (2001).
Mocsai, A. et al. Integrin signaling in neutrophils and macrophages uses adaptors containing immunoreceptor tyrosine-based activation motifs. Nat. Immunol. 7, 1326–1333 (2006).
Boes, M. et al. T cells induce extended class II MHC compartments in dendritic cells in a Toll-like receptor-dependent manner. J. Immunol. 171, 4081–4088 (2003).
Inaba, K. et al. Generation of large numbers of dendritic cells from mouse bone marrow cultures supplemented with granulocyte/macrophage colony-stimulating factor. J. Exp. Med. 176, 1693–1702 (1992).
Keefe, A.D., Wilson, D.S., Seelig, B. & Szostak, J.W. One-step purification of recombinant proteins using a nanomolar-affinity streptavidin-binding peptide, the SBP-Tag. Protein Expr. Purif. 23, 440–446 (2001).
Mackey, M.F., Wang, Z., Eichelberg, K. & Germain, R.N. Distinct contributions of different CD40 TRAF binding sites to CD154-induced dendritic cell maturation and IL-12 secretion. Eur. J. Immunol. 33, 779–789 (2003).
Holscher, C. et al. A protective and agonistic function of IL-12p40 in mycobacterial infection. J. Immunol. 167, 6957–6966 (2001).
Overbergh, L. et al. The use of real-time reverse transcriptase PCR for the quantification of cytokine gene expression. J. Biomol. Tech. 14, 33–43 (2003).
Acknowledgements
We thank M. Weber for the acquisition of confocal images, and F. Batista, A. O'Garra and members of the Immunobiology Laboratory (Cancer Research UK) for advice and discussions. MyD88-knockout and TRIF-knockout mice were from S. Akira (Osaka University), OT-II TCR-transgenic mice on a C57BL/6 background were from W. Heath (Walter and Eliza Hall Institute), lipopolysaccharide was from S. Vogel (University of Maryland), and pFB-IRES-GFP was from R. Germain (National Institute of Allergy and Infectious Diseases). Supported by Cancer Research UK and EMBO (S.LG-L).
Author information
Authors and Affiliations
Contributions
S.LG.-L. and C.R.S. designed the study, analyzed data and wrote the paper; S.LG.-L. coordinated the study, did experiments and analyzed data; M.J.R., F.O. and E.C.S. contributed additional experiments and intellectual input; O.G. and J.R. did the experiments with CARD9-knockout cells and mice; S.V.T. and G.D.B. provided dectin-1-knockout bone marrow and infected dectin-1-knockout mice; and E.S. and V.T. provided Syk-knockout fetal livers.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Fig. 1
Dectin-1 agonists elicit high quantities of IL-10 and IL-2 from DCs. (PDF 1164 kb)
Supplementary Fig. 2
Dectin-1-sitmulated BDMCs selectively express transcripts encoding IL-23p19 but not IL-12p35. (PDF 1071 kb)
Supplementary Fig. 3
Dectin-1 agonists are superior to TLR agonists in skewing T cell differentiation towards TH-17. (PDF 1076 kb)
Supplementary Fig. 4
Titration of curdlan and CpG does not allow interconversion of their effects on TH cell differentiation. (PDF 1044 kb)
Supplementary Fig. 5
Neutralization of IFN-γ is not sufficient for TH-17 differentiation in response to curdlan. (PDF 1177 kb)
Supplementary Fig. 6
Exogenous IL-12 blocks TH-17 skewing by curdlan-stimulated DCs. (PDF 1030 kb)
Supplementary Fig. 7
Immunization with curdlan induces β-glucan-specific antibodies. (PDF 1714 kb)
Rights and permissions
About this article
Cite this article
LeibundGut-Landmann, S., Groß, O., Robinson, M. et al. Syk- and CARD9-dependent coupling of innate immunity to the induction of T helper cells that produce interleukin 17. Nat Immunol 8, 630–638 (2007). https://doi.org/10.1038/ni1460
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni1460
This article is cited by
-
Involvement of IL-17 A/IL-17 Receptor A with Neutrophil Recruitment and the Severity of Coronary Arteritis in Kawasaki Disease
Journal of Clinical Immunology (2024)
-
Inherited Human BCL10 Deficiencies
Journal of Clinical Immunology (2024)
-
Genetic association of PRKCD and CARD9 polymorphisms with Vogt–Koyanagi–Harada disease in the Chinese Han population
Human Genomics (2023)
-
Commensal fungi in intestinal health and disease
Nature Reviews Gastroenterology & Hepatology (2023)
-
C-type lectin receptor 2d forms homodimers and heterodimers with TLR2 to negatively regulate IRF5-mediated antifungal immunity
Nature Communications (2023)