Key Points
-
Factors involved in fistulizing perianal disease pathogenesis include a genetically determined altered immune response with increased production of cytokines, leading to upregulation of matrix metalloproteinases and epithelial-to-mesenchymal transition
-
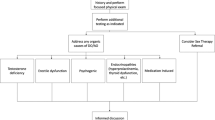
Essential evaluation of fistulas includes a clinical assessment of external openings, endoscopic assessment of proctitis and MRI to determine the anatomy of fistula tracts and presence of abscesses
-
A top-down approach with medical therapy might provide maximal benefit for treatment of this aggressive manifestation of Crohn's disease
-
Local injection of mesenchymal stem cells can induce remission in patients not responding to medical therapies, or avoid the exposure to systemic immunosuppression
-
Surgery is still required in a high proportion of patients and should not be delayed when criteria of drug failure is met
Abstract
Perianal fistulizing Crohn's disease has a major negative effect on patient quality of life and is a predictor of poor long-term outcomes. Factors involved in the pathogenesis of perianal fistulizing Crohn's disease include an increased production of transforming growth factor β, TNF and IL-13 in the inflammatory infiltrate that induce epithelial-to-mesenchymal transition and upregulation of matrix metalloproteinases, leading to tissue remodelling and fistula formation. Care of patients with perianal Crohn's disease requires a multidisciplinary approach. A complete assessment of fistula characteristics is the basis for optimal management and must include the clinical evaluation of fistula openings, endoscopic assessment of the presence of proctitis, and MRI to determine the anatomy of fistula tracts and presence of abscesses. Local injection of mesenchymal stem cells can induce remission in patients not responding to medical therapies, or to avoid the exposure to systemic immunosuppression in patients naive to biologics in the absence of active luminal disease. Surgery is still required in a high proportion of patients and should not be delayed when criteria for drug failure is met. In this Review, we provide an up-to-date overview on the pathogenesis and diagnosis of fistulizing Crohn's disease, as well as therapeutic strategies.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Penner, A. & Crohn, B. B. Perianal fistulae as a complication of regional ileitis. Ann. Surg. 108, 867–873 (1938).
Kasparek, M. S. et al. Long-term quality of life in patients with Crohn's disease and perianal fistulas: influence of fecal diversion. Dis. Colon Rectum 50, 2067–2074 (2007).
Beaugerie, L., Seksik, P., Nion-Larmurier, I., Gendre, J. P. & Cosnes, J. Predictors of Crohn's disease. Gastroenterology 130, 650–656 (2006).
Sandborn, W. J., Fazio, V. W., Feagan, B. G., Hanauer, S. B. & American Gastroenterological Association Clinical Practice Committee. AGA technical review on perianal Crohn's disease. Gastroenterology 125, 1508–1530 (2003).
Lewis, R. T. & Bleier, J. I. Surgical treatment of anorectal Crohn disease. Clin. Colon Rectal Surg. 26, 90–99 (2013).
Schwartz, D. A. et al. The natural history of fistulizing Crohn's disease in Olmsted County, Minnesota. Gastroenterology 122, 875–880 (2002).
Eglinton, T. W., Barclay, M. L., Gearry, R. B. & Frizelle, F. A. The spectrum of perianal Crohn's disease in a population-based cohort. Dis. Colon Rectum 55, 773–777 (2012).
Hellers, G., Bergstrand, O., Ewerth, S. & Holmstrom, B. Occurrence and outcome after primary treatment of anal fistulae in Crohn's disease. Gut 21, 525–527 (1980).
Fields, S., Rosainz, L., Korelitz, B. I., Panagopoulos, G. & Schneider, J. Rectal strictures in Crohn's disease and coexisting perirectal complications. Inflamm. Bowel Dis. 14, 29–31 (2008).
Buchmann, P., Keighley, M. R., Allan, R. N., Thompson, H. & Alexander-Williams, J. Natural history of perianal Crohn's disease. Ten year follow-up: a plea for conservatism. Am. J. Surg. 140, 642–644 (1980).
Makowiec, F., Jehle, E. C. & Starlinger, M. Clinical course of perianal fistulas in Crohn's disease. Gut 37, 696–701 (1995).
Bell, S. J. et al. The clinical course of fistulating Crohn's disease. Aliment. Pharmacol. Ther. 17, 1145–1151 (2003).
Michelassi, F., Melis, M., Rubin, M. & Hurst, R. D. Surgical treatment of anorectal complications in Crohn's disease. Surgery 128, 597–603 (2000).
Molendijk, I., Nuij, V. J., van der Meulen-de Jong, A. E. & van der Woude, C. J. Disappointing durable remission rates in complex Crohn's disease fistula. Inflamm. Bowel Dis. 20, 2022–2028 (2014).
Schwartz, D. A. & Herdman, C. R. Review article: The medical treatment of Crohn's perianal fistulas. Aliment. Pharmacol. Ther. 19, 953–967 (2004).
Iesalnieks, I. et al. Fistula-associated anal adenocarcinoma in Crohn's disease. Inflamm. Bowel Dis. 16, 1643–1648 (2010).
Baars, J. E. et al. Malignant transformation of perianal and enterocutaneous fistulas is rare: results of 17 years of follow-up from The Netherlands. Scand. J. Gastroenterol. 46, 319–325 (2011).
Papaconstantinou, I., Mantzos, D. S., Kondi-Pafiti, A. & Koutroubakis, I. E. Anal adenocarcinoma complicating chronic Crohn's disease. Int. J. Surg. Case Rep. 10, 201–203 (2015).
Siegmund, B. et al. Results of the Fifth Scientific Workshop of the ECCO (II): Pathophysiology of Perianal Fistulizing Disease. J. Crohns Colitis 10, 377–386 (2016).
Scharl, M. et al. Interleukin-13 and transforming growth factor β synergise in the pathogenesis of human intestinal fistulae. Gut 62, 63–72 (2013).
Nieto, M. A., Huang, R. Y., Jackson, R. A. & Thiery, J. P. Emt: 2016. Cell 166, 21–45 (2016).
Frei, S. M. et al. A role for tumor necrosis factor and bacterial antigens in the pathogenesis of Crohn's disease-associated fistulae. Inflamm. Bowel Dis. 19, 2878–2887 (2013).
Scharl, M. et al. Potential role for SNAIL family transcription factors in the etiology of Crohn's disease-associated fistulae. Inflamm. Bowel Dis. 17, 1907–1916 (2011).
Frei, S. M. et al. The role for dickkopf-homolog-1 in the pathogenesis of Crohn's disease-associated fistulae. PLoS ONE 8, e78882 (2013).
Scharl, M. et al. Epithelial-to-mesenchymal transition in a fistula-associated anal adenocarcinoma in a patient with long-standing Crohn's disease. Eur. J. Gastroenterol. Hepatol. 26, 114–118 (2014).
von Lampe, B., Barthel, B., Coupland, S. E., Riecken, E. O. & Rosewicz, S. Differential expression of matrix metalloproteinases and their tissue inhibitors in colon mucosa of patients with inflammatory bowel disease. Gut 47, 63–73 (2000).
Castaneda, F. E. et al. Targeted deletion of metalloproteinase 9 attenuates experimental colitis in mice: central role of epithelial-derived MMP. Gastroenterology 129, 1991–2008 (2005).
Kirkegaard, T., Hansen, A., Bruun, E. & Brynskov, J. Expression and localisation of matrix metalloproteinases and their natural inhibitors in fistulae of patients with Crohn's disease. Gut 53, 701–709 (2004).
Seow-Choen, F., Hay, A. J., Heard, S. & Phillips, R. K. Bacteriology of anal fistulae. Br. J. Surg. 79, 27–28 (1992).
Yassin, N. A. et al. The gut microbiome–immune system interaction as an aetiological factor for fistulising perianal Crohn's disease. J. Crohns Colitis 9, S81–S82 (2015).
Cleynen, I. et al. Genetic factors conferring an increased susceptibility to develop Crohn's disease also influence disease phenotype: results from the IBDchip European Project. Gut 62, 1556–1565 (2013).
Henckaerts, L. et al. Genetic risk profiling and prediction of disease course in Crohn's disease patients. Clin. Gastroenterol. Hepatol. 7, 972–980.e2 (2009).
Kaur, M. et al. Perianal Crohn's disease is associated with distal colonic disease, stricturing disease behavior, IBD-associated serologies and genetic variation in the JAK–STAT pathway. Inflamm. Bowel Dis. 22, 862–869 (2016).
Parks, A. G., Gordon, P. H. & Hardcastle, J. D. A classification of fistula-in-ano. Br. J. Surg. 63, 1–12 (1976).
Spencer, J. A., Ward, J., Beckingham, I. J., Adams, C. & Ambrose, N. S. Dynamic contrast-enhanced MR imaging of perianal fistulas. AJR Am. J. Roentgenol. 167, 735–741 (1996).
Morris, J., Spencer, J. A. & Ambrose, N. S. MR imaging classification of perianal fistulas and its implications for patient management. Radiographics 20, 623–635 (2000).
Tozer, P. et al. Long-term MRI-guided combined anti-TNF-α and thiopurine therapy for Crohn's perianal fistulas. Inflamm. Bowel Dis. 18, 1825–1834 (2012).
Sheedy, S. P., Bruining, D. H., Dozois, E. J., Faubion, W. A. & Fletcher, J. G. MR imaging of perianal Crohn disease. Radiology 282, 628–645 (2017).
Irvine, E. J. Usual therapy improves perianal Crohn's disease as measured by a new disease activity index. McMaster IBD Study Group. J. Clin. Gastroenterol. 20, 27–32 (1995).
Allan, A., Linares, L., Spooner, H. A. & Alexander-Williams, J. Clinical index to quantitate symptoms of perianal Crohn's disease. Dis. Colon Rectum 35, 656–661 (1992).
Ng, S. C. et al. Prospective evaluation of anti-tumor necrosis factor therapy guided by magnetic resonance imaging for Crohn's perineal fistulas. Am. J. Gastroenterol. 104, 2973–2986 (2009).
Horsthuis, K. et al. Evaluation of an MRI-based score of disease activity in perianal fistulizing Crohn's disease. Clin. Imag. 35, 360–365 (2011).
Van Assche, G. et al. Magnetic resonance imaging of the effects of infliximab on perianal fistulizing Crohn's disease. Am. J. Gastroenterol. 98, 332–339 (2003).
Horsthuis, K., Lavini, C., Bipat, S., Stokkers, P. C. & Stoker, J. Perianal Crohn disease: evaluation of dynamic contrast-enhanced MR imaging as an indicator of disease activity. Radiology 251, 380–387 (2009).
Karmiris, K. et al. Long-term monitoring of infliximab therapy for perianal fistulizing Crohn's disease by using magnetic resonance imaging. Clin. Gastroenterol. Hepatol. 9, 130–136 (2011).
Savoye-Collet, C., Savoye, G., Koning, E., Dacher, J. N. & Lerebours, E. Fistulizing perianal Crohn's disease: contrast-enhanced magnetic resonance imaging assessment at 1 year on maintenance anti-TNF-α therapy. Inflamm. Bowel Dis. 17, 1751–1758 (2011).
Schwartz, D. A. et al. A comparison of endoscopic ultrasound, magnetic resonance imaging, and exam under anesthesia for evaluation of Crohn's perianal fistulas. Gastroenterology 121, 1064–1072 (2001).
Fichera, A., Zoccali, M. & Crohn's & Colitis Foundation of America, Inc. Guidelines for the surgical treatment of Crohn's perianal fistulas. Inflamm. Bowel Dis. 21, 753–758 (2015).
Schwartz, D. A. et al. Guidelines for the multidisciplinary management of Crohn's perianal fistulas: summary statement. Inflamm. Bowel Dis. 21, 723–730 (2015).
Gecse, K. B. et al. A global consensus on the classification, diagnosis and multidisciplinary treatment of perianal fistulising Crohn's disease. Gut 63, 1381–1392 (2014).
Schwartz, D. A., Ghazi, L. J. & Regueiro, M. Guidelines for medical treatment of Crohn's perianal fistulas: critical evaluation of therapeutic trials. Inflamm. Bowel Dis. 21, 737–752 (2015).
Gomollon, F. et al. 3 rd European evidence-based consensus on the diagnosis and management of Crohn's disease 2016: Part 1: diagnosis and medical management. J. Crohns Colitis 11, 3–25 (2017).
Hinterleitner, T. A. et al. Combination of cyclosporine, azathioprine and prednisolone for perianal fistulas in Crohn's disease. Z. Gastroenterol. 35, 603–608 (1997).
Lennard-Jones, J. E. Toward optimal use of corticosteroids in ulcerative colitis and Crohn's disease. Gut 24, 177–181 (1983).
Brandt, L. J., Bernstein, L. H., Boley, S. J. & Frank, M. S. Metronidazole therapy for perineal Crohn's disease: a follow-up study. Gastroenterology 83, 383–387 (1982).
Solomon, M. J. et al. Combination of ciprofloxacin and metronidazole in severe perianal Crohn's disease. Can. J. Gastroenterol. 7, 571–573 (1993).
Thia, K. T. et al. Ciprofloxacin or metronidazole for the treatment of perianal fistulas in patients with Crohn's disease: a randomized, double-blind, placebo-controlled pilot study. Inflamm. Bowel Dis. 15, 17–24 (2009).
Maeda, Y. et al. Randomized clinical trial of metronidazole ointment versus placebo in perianal Crohn's disease. Br. J. Surg. 97, 1340–1347 (2010).
West, R. L. et al. Clinical and endosonographic effect of ciprofloxacin on the treatment of perianal fistulae in Crohn's disease with infliximab: a double-blind placebo-controlled study. Aliment. Pharmacol. Ther. 20, 1329–1336 (2004).
Dewint, P. et al. Adalimumab combined with ciprofloxacin is superior to adalimumab monotherapy in perianal fistula closure in Crohn's disease: a randomised, double-blind, placebo controlled trial (ADAFI). Gut 63, 292–299 (2014).
Pearson, D. C., May, G. R., Fick, G. H. & Sutherland, L. R. Azathioprine and 6-mercaptopurine in Crohn disease. A meta-analysis. Ann. Intern. Med. 123, 132–142 (1995).
Dejaco, C. et al. Antibiotics and azathioprine for the treatment of perianal fistulas in Crohn's disease. Aliment. Pharmacol. Ther. 18, 1113–1120 (2003).
Sandborn, W. J. et al. Tacrolimus for the treatment of fistulas in patients with Crohn's disease: a randomized, placebo-controlled trial. Gastroenterology 125, 380–388 (2003).
Hart, A. L., Plamondon, S. & Kamm, M. A. Topical tacrolimus in the treatment of perianal Crohn's disease: exploratory randomized controlled trial. Inflamm. Bowel Dis. 13, 245–253 (2007).
Hanauer, S. B. & Smith, M. B. Rapid closure of Crohn's disease fistulas with continuous intravenous cyclosporin A. Am. J. Gastroenterol. 88, 646–649 (1993).
Present, D. H. & Lichtiger, S. Efficacy of cyclosporine in treatment of fistula of Crohn's disease. Dig. Dis. Sci. 39, 374–380 (1994).
Mahadevan, U., Marion, J. F. & Present, D. H. Fistula response to methotrexate in Crohn's disease: a case series. Aliment. Pharmacol. Ther. 18, 1003–1008 (2003).
Schroder, O., Blumenstein, I., Schulte-Bockholt, A. & Stein, J. Combining infliximab and methotrexate in fistulizing Crohn's disease resistant or intolerant to azathioprine. Aliment. Pharmacol. Ther. 19, 295–301 (2004).
Present, D. H. et al. Infliximab for the treatment of fistulas in patients with Crohn's disease. N. Engl. J. Med. 340, 1398–1405 (1999).
Sands, B. E. et al. Infliximab maintenance therapy for fistulizing Crohn's disease. N. Engl. J. Med. 350, 876–885 (2004).
Hanauer, S. B. et al. Human anti-tumor necrosis factor monoclonal antibody (adalimumab) in Crohn's disease: the CLASSIC-I trial. Gastroenterology 130, 323–333 (2006).
Sandborn, W. J. et al. Adalimumab induction therapy for Crohn disease previously treated with infliximab: a randomized trial. Ann. Intern. Med. 146, 829–838 (2007).
Colombel, J. F. et al. Adalimumab for the treatment of fistulas in patients with Crohn's disease. Gut 58, 940–948 (2009).
Sandborn, W. J. et al. Certolizumab pegol for the treatment of Crohn's disease. N. Engl. J. Med. 357, 228–238 (2007).
Schreiber, S. et al. Maintenance therapy with certolizumab pegol for Crohn's disease. N. Engl. J. Med. 357, 239–250 (2007).
Schreiber, S. et al. Randomised clinical trial: certolizumab pegol for fistulas in Crohn's disease - subgroup results from a placebo-controlled study. Aliment. Pharmacol. Ther. 33, 185–193 (2011).
Bouguen, G. et al. Long-term outcome of perianal fistulizing Crohn's disease treated with infliximab. Clin. Gastroenterol. Hepatol. 11, 975–981.e1-4 (2013).
Sandborn, W. J. et al. Vedolizumab as induction and maintenance therapy for Crohn's disease. N. Engl. J. Med. 369, 711–721 (2013).
Ehrenpreis, E. D., Kane, S. V., Cohen, L. B., Cohen, R. D. & Hanauer, S. B. Thalidomide therapy for patients with refractory Crohn's disease: An open-label trial. Gastroenterology 117, 1271–1277 (1999).
Lavy, A. et al. Hyperbaric oxygen for perianal Crohn's disease. J. Clin. Gastroenterol. 19, 202–205 (1994).
Colombel, J. F. et al. Hyperbaric oxygenation in severe perineal Crohn's disease. Dis. Colon Rectum 38, 609–614 (1995).
Weisz, G. et al. Modification of in vivo and in vitro TNF-α, IL-1, and IL-6 secretion by circulating monocytes during hyperbaric oxygen treatment in patients with perianal Crohn's disease. J. Clin. Immunol. 17, 154–159 (1997).
Fukuda, Y. et al. Oral spherical adsorptive carbon for the treatment of intractable anal fistulas in Crohn's disease: a multicenter, randomized, double-blind, placebo-controlled trial. Am. J. Gastroenterol. 103, 1721–1729 (2008).
Reinisch, W. et al. AST-120 (spherical carbon adsorbent) in the treatment of perianal fistulae in mild-to-moderate Crohn's disease: FHAST-1, a phase 3, multicenter, placebo-controlled study. Inflamm. Bowel Dis. 20, 872–881 (2014).
Bernardo, M. E., Locatelli, F. & Fibbe, W. E. Mesenchymal stromal cells. Ann. NY Acad. Sci. 1176, 101–117 (2009).
Nauta, A. J. & Fibbe, W. E. Immunomodulatory properties of mesenchymal stromal cells. Blood 110, 3499–3506 (2007).
Gonzalez-Rey, E., Gonzalez, M. A., Rico, L., Buscher, D. & Delgado, M. Human adult stem cells derived from adipose tissue protect against experimental colitis and sepsis. Gut 58, 929–939 (2009).
Panes, J., Ordas, I. & Ricart, E. Stem cell treatment for Crohn's disease. Expert Rev. Clin. Immunol. 6, 597–605 (2010).
Garcia-Olmo, D. et al. A phase I clinical trial of the treatment of Crohn's fistula by adipose mesenchymal stem cell transplantation. Dis. Colon Rectum. 48, 1416–1423 (2005).
Garcia-Olmo, D. et al. Expanded adipose-derived stem cells for the treatment of complex perianal fistula: a phase II clinical trial. Dis. Colon Rectum. 52, 79–86 (2009).
Guadalajara, H. et al. Long-term follow-up of patients undergoing adipose-derived adult stem cell administration to treat complex perianal fistulas. Int. J. Colorectal Dis. 27, 595–600 (2012).
Ciccocioppo, R. et al. Autologous bone marrow-derived mesenchymal stromal cells in the treatment of fistulizing Crohn's disease. Gut 60, 788–798 (2011).
de la Portilla, F. et al. Expanded allogeneic adipose-derived stem cells (eASCs) for the treatment of complex perianal fistula in Crohn's disease: results from a multicenter phase I/IIa clinical trial. Int. J. Colorectal Dis. 28, 313–323 (2013).
Molendijk, I. et al. Allogeneic bone marrow-derived mesenchymal stromal cells promote healing of refractory perianal fistulas in patients with Crohn's disease. Gastroenterology 149, 918–927.e6 (2015).
Panes, J. et al. Expanded allogeneic adipose-derived mesenchymal stem cells (Cx601) for complex perianal fistulas in Crohn's disease: a phase 3 randomised, double-blind controlled trial. Lancet 388, 1281–1290 (2016).
Dietz, A. B. et al. Autologous mesenchymal stem cells, applied in a bioabsorbable matrix, for treatment of perianal fistulas in patients with Crohn's disease. Gastroenterology 153, 59–62.e2 (2017).
Solomon, M. J. Fistulae and abscesses in symptomatic perianal Crohn's disease. Int. J. Colorectal Dis. 11, 222–226 (1996).
Regueiro, M. & Mardini, H. Treatment of perianal fistulizing Crohn's disease with infliximab alone or as an adjunct to exam under anesthesia with seton placement. Inflamm. Bowel Dis. 9, 98–103 (2003).
Sciaudone, G. et al. Treatment of complex perianal fistulas in Crohn disease: infliximab, surgery or combined approach. Can. J. Surg. 53, 299–304 (2010).
Parks, A. G. & Stitz, R. W. The treatment of high fistula-in-ano. Dis. Colon Rectum 19, 487–499 (1976).
Hyder, S. A., Travis, S. P., Jewell, D. P., McC Mortensen, N. J. & George, B. D. Fistulating anal Crohn's disease: results of combined surgical and infliximab treatment. Dis. Colon Rectum 49, 1837–1841 (2006).
van Koperen, P. J., Safiruddin, F., Bemelman, W. A. & Slors, J. F. Outcome of surgical treatment for fistula in ano in Crohn's disease. Br. J. Surg. 96, 675–679 (2009).
Williams, J. G., Rothenberger, D. A., Nemer, F. D. & Goldberg, S. M. Fistula-in-ano in Crohn's disease. Results of aggressive surgical treatment. Dis. Colon Rectum 34, 378–384 (1991).
de Parades, V. et al. Seton drainage and fibrin glue injection for complex anal fistulas. Colorectal Dis. 12, 459–463 (2010).
Gaertner, W. B. et al. Results of combined medical and surgical treatment of recto-vaginal fistula in Crohn's disease. Colorectal Dis. 13, 678–683 (2011).
Abel, M. E., Chiu, Y. S., Russell, T. R. & Volpe, P. A. Autologous fibrin glue in the treatment of rectovaginal and complex fistulas. Dis. Colon Rectum 36, 447–449 (1993).
Zmora, O. et al. Fibrin glue sealing in the treatment of perineal fistulas. Dis. Colon Rectum 46, 584–589 (2003).
Loungnarath, R. et al. Fibrin glue treatment of complex anal fistulas has low success rate. Dis. Colon Rectum 47, 432–436 (2004).
Lindsey, I., Smilgin-Humphreys, M. M., Cunningham, C., Mortensen, N. J. & George, B. D. A randomized, controlled trial of fibrin glue versus conventional treatment for anal fistula. Dis. Colon Rectum 45, 1608–1615 (2002).
Grimaud, J. C. et al. Fibrin glue is effective healing perianal fistulas in patients with Crohn's disease. Gastroenterology 138, 2275–2281.e1 (2010).
Singer, M. et al. Treatment of fistulas-in-ano with fibrin sealant in combination with intra-adhesive antibiotics and/or surgical closure of the internal fistula opening. Dis. Colon Rectum 48, 799–808 (2005).
O'Riordan, J. M., Datta, I., Johnston, C. & Baxter, N. N. A systematic review of the anal fistula plug for patients with Crohn's and non-Crohn's related fistula-in-ano. Dis. Colon Rectum 55, 351–358 (2012).
Senejoux, A. et al. Fistula plug in fistulising ano-perineal Crohn's disease: a randomised controlled trial. J. Crohns Colitis 10, 141–148 (2016).
Soltani, A. & Kaiser, A. M. Endorectal advancement flap for cryptoglandular or Crohn's fistula-in-ano. Dis. Colon Rectum 53, 486–495 (2010).
Gionchetti, P. et al. 3rd European evidence-based consensus on the diagnosis and management of Crohn's disease 2016: Part 2: Surgical management and special situations. J. Crohns Colitis 11, 135–149 (2016).
Rojanasakul, A. LIFT procedure: a simplified technique for fistula-in-ano. Tech. Coloproctol. 13, 237–240 (2009).
Gingold, D. S., Murrell, Z. A. & Fleshner, P. R. A prospective evaluation of the ligation of the intersphincteric tract procedure for complex anal fistula in patients with Crohn's disease. Ann. Surg. 260, 1057–1061 (2014).
D'Haens, G. R. et al. Early lesions of recurrent Crohn's disease caused by infusion of intestinal contents in excluded ileum. Gastroenterology 114, 262–267 (1998).
Yamamoto, T., Allan, R. N. & Keighley, M. R. Effect of fecal diversion alone on perianal Crohn's disease. World J. Surg. 24, 1258–1262; discussion 1262–1263 (2000).
Singh, S. et al. Systematic review with meta-analysis: faecal diversion for management of perianal Crohn's disease. Aliment. Pharmacol. Ther. 42, 783–792 (2015).
Gaertner, W. B. et al. Does infliximab infusion impact results of operative treatment for Crohn's perianal fistulas? Dis. Colon Rectum 50, 1754–1760 (2007).
Gecse, K. B. et al. Results of the Fifth Scientific Workshop of the ECCO [II]: clinical aspects of perianal fistulising crohn's disease-the unmet needs. J. Crohns Colitis 10, 758–765 (2016).
Acknowledgements
The author's work is supported in part by grant 2015/ 66379-R from Ministerio de Economia y Competitividad, Spain, and the Helmsley Trust (to J.P.), and grant PI16/00721 from Ministerio de Sanidad, Spain (to J.R.)
Author information
Authors and Affiliations
Contributions
J.P. conceived the structure of the article, J.R. performed the literature review. J.P. and J.R. contributed equally to writing the manuscript and to reviewing and/or editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
J.P. has received consulting fees from Abbvie, Almirall, Boehringer-Ingelheim, Celgene, Ferring, Janssen, MSD, Novartis, Pfizer, Robarts, Roche, Second Genome, Shire, Takeda, TiGenix and Topivert; and speaker fees from Abbvie, Biogen, Ferring, Janssen, MSD and Pfizer. J.R. has received consulting and speaker fees from Abbvie, Bioclinica, Boehringer-Ingelheim, MSD, Robarts Clinical Trials, Roche, Takeda, and TiGenix.
Supplementary information
Supplementary Information S1
Controlled trials on treatments for perianal fistulizing Crohn's disease (PDF 103 kb)
Rights and permissions
About this article
Cite this article
Panés, J., Rimola, J. Perianal fistulizing Crohn's disease: pathogenesis, diagnosis and therapy. Nat Rev Gastroenterol Hepatol 14, 652–664 (2017). https://doi.org/10.1038/nrgastro.2017.104
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrgastro.2017.104
This article is cited by
-
Comparison of different sources of mesenchymal stem cells: focus on inflammatory bowel disease
Inflammopharmacology (2024)
-
Perianal fistulizing Crohn’s disease: Current perspectives on diagnosis, monitoring and management with a focus on emerging therapies
Indian Journal of Gastroenterology (2024)
-
Antibiotics for inflammatory bowel disease: Current status
Indian Journal of Gastroenterology (2024)
-
Surgical management of complex perianal fistula revisited in a systematic review: a critical view of available scientific evidence
BMC Surgery (2023)
-
Mesenchymal stem cells transplantation for perianal fistulas: a systematic review and meta-analysis of clinical trials
Stem Cell Research & Therapy (2023)