Key Points
-
The central nervous system (CNS) has been characterized as an immunologically privileged site in the past, but it should more accurately be viewed as immunologically specialized.
-
It is probable that control of immune reactivity to components of the CNS cannot occur solely by sequestering neuroantigens behind the blood–brain barrier (BBB). Rather, trafficking of immunocompetent cells into the CNS must also be tightly regulated.
-
The CNS is protected, nourished and supported by a unique and diverse combination of vascular elements and by the cerebrospinal fluid (CSF). Consequently, mechanisms for recruitment of leukocytes across different vascular beds and into varied fluid compartments of the CNS will differ.
-
Despite the successful studies of T-cell homing to lymphoid organs, small intestines and skin, organ-selective trafficking determinants for the CNS have not been identified.
-
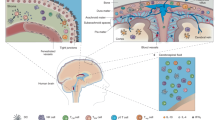
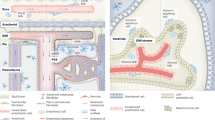
It is possible to define three distinct routes for leukocytes entry into the CNS: from blood to CSF across the choroid plexus; from blood to the subarachnoid space through meningeal vessels; and from blood to parenchymal perivascular spaces.
-
Adoptive transfer of primed encephalitogenic T cells leads to the accumulation of a small number of cells in the meninges, the choroid plexus and, perhaps, the parenchyma within two hours after transfer.
-
This low-efficiency first wave of cell migration might function to activate parenchymal vessels for interaction with the subsequent large-scale entry of leukocytes, as recent studies using intravital microscopy indicate that non-activated parenchymal vessels are refractory to communication with lymphocytes.
Abstract
Leukocyte migration into and through tissues is fundamental to normal physiology, immunopathology and host defence. Leukocyte entry into the central nervous system (CNS) is restricted, in part, because of the blood–brain barrier (BBB). During the past decade, crucial components that are involved in the process of leukocyte migration have been identified and progress has been made in understanding the mechanisms of neuroinflammatory reactions. In this review, present knowledge of the trafficking determinants that guide the migration of leukocytes is superimposed onto the vascular and compartmental anatomy of the CNS. We discuss three distinct routes for leukocytes to enter the CNS and consider how different populations of leukocytes use trafficking signals to gain entry.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Garden, G. A. Microglia in human immunodeficiency virus-associated neurodegeneration. Glia 40, 240–251 (2002).
Wiendl, H. et al. A functional role of HLA-G expression in human gliomas: an alternative strategy of immune escape. J. Immunol. 168, 4772–4780 (2002).
Eikelenboom, P. et al. Neuroinflammation in Alzheimer's disease and prion disease. Glia 40, 232–239 (2002).
Rogers, J., Strohmeyer, R., Kovelowski, C. J. & Li, R. Microglia and inflammatory mechanisms in the clearance of amyloid-β peptide. Glia 40, 260–269 (2002).
Strazielle, N. & Ghersi-Egea, J. F. Choroid plexus in the central nervous system: biology and physiopathology. J. Neuropathol. Exp. Neurol. 59, 561–574 (2000).
Cserr, H. F. & Knopf, P. M. Cervical lymphatics, the blood–brain barrier and the immunoreactivity of the brain: a new view. Immunol. Today 13, 507–512 (1992). A clear summary of the concept that cervical-lymphatic drainage of the cerebrospinal fluid (CSF) contributes to immune surveillance of the central nervous system (CNS).
Widner, H., Moller, G. & Johansson, B. B. Immune response in deep cervical lymph nodes and spleen in the mouse after antigen deposition in different intracerebral sites. Scand. J. Immunol. 28, 563–571 (1988).
Weller, R. O., Engelhardt, B. & Phillips, M. J. Lymphocyte targeting of the central nervous system: a review of afferent and efferent CNS-immune pathways. Brain Pathol. 6, 275–288 (1996).
Weller, R. O., Kida, S. & Zhang, E. T. Pathways of fluid drainage from the brain: morphological aspects and immunological significance in rat and man. Brain Pathol. 2, 277–284 (1992).
Boulton, M. et al. Contribution of extracranial lymphatics and arachnoid villi to the clearance of a CSF tracer in the rat. Am. J. Physiol. 276, R818–R823 (1999).
de Vos, A. F. et al. Transfer of central nervous system autoantigens and presentation in secondary lymphoid organs. J. Immunol. 169, 5415–5423 (2002).
Weller, R. O. Pathology of cerebrospinal fluid and interstitial fluid of the CNS: significance for Alzheimer disease, prion disorders and multiple sclerosis. J. Neuropathol. Exp. Neurol. 57, 885–894 (1998).
Svenningsson, A. et al. Adhesion molecule expression on cerebrospinal fluid T lymphocytes: evidence for common recruitment mechanisms in multiple sclerosis, aseptic meningitis, and normal controls. Ann. Neurol. 34, 155–161 (1993).
Huber, J. D., Egleton, R. D. & Davis, T. P. Molecular physiology and pathophysiology of tight junctions in the blood–brain barrier. Trends Neurosci. 24, 719–725 (2001).
Segal, M. B. Transport of nutrients across the choroid plexus. Microsc. Res. Tech. 52, 38–48 (2001).
Massacesi, L. Compartmentalization of the immune response in the central nervous system and natural history of multiple sclerosis. Implications for therapy. Clin. Neurol. Neurosurg. 104, 177–181 (2002).
Lee, S. C., Moore, G. R., Golenwsky, G. & Raine, C. S. Multiple sclerosis: a role for astroglia in active demyelination suggested by class II MHC expression and ultrastructural study. J. Neuropathol. Exp. Neurol. 49, 122–136 (1990).
Bö, L. et al. Detection of MHC class II-antigens on macrophages and microglia, but not on astrocytes and endothelia in active multiple sclerosis lesions. J. Neuroimmunol. 51, 135–146 (1994).
Jaeschke, H. et al. Mechanisms of hepatotoxicity. Toxicol. Sci. 65, 166–176 (2002).
Perry, V. H., Bell, M. D., Brown, H. C. & Matyszak, M. K. Inflammation in the nervous system. Curr. Opin. Neurobiol. 5, 636–641 (1995).
Perry, V. H. & Andersson, P. B. The inflammatory response in the CNS. Neuropathol. Appl. Neurobiol. 18, 454–459 (1992). This review explains the concept that inflammatory reactions in the CNS favour the recruitment and activation of mononuclear phagocytes, even after necrotizing tissue injury.
Head, J. R. & Griffin, W. S. Functional capacity of solid tissue transplants in the brain: evidence for immunological privilege. Proc. R. Soc. Lond. B Biol. Sci. 224, 375–387 (1985).
Stevenson, P. G., Austyn, J. M. & Hawke, S. Uncoupling of virus-induced inflammation and anti-viral immunity in the brain parenchyma. J. Gen. Virol. 83, 1735–1743 (2002).
Carrithers, M. D., Visintin, I., Viret, C. & Janeway, C. S. Jr. Role of genetic background in P selectin-dependent immune surveillance of the central nervous system. J. Neuroimmunol. 129, 51–57 (2002).
Svenningsson, A., Andersen, O., Edsbagge, M. & Stemme, S. Lymphocyte phenotype and subset distribution in normal cerebrospinal fluid. J. Neuroimmunol. 63, 39–46 (1995).
Hintzen, R. Q. et al. Analysis of CD27 surface expression on T cell subsets in MS patients and control individuals. J. Neuroimmunol. 56, 99–105 (1995).
Kivisäkk, P. et al. T cells in the cerebrospinal fluid express a similar repertoire of inflammatory chemokine receptors in the absence or presence of CNS inflammation: implications for CNS trafficking. Clin. Exp. Immunol. 129, 510–518 (2002).
Sallusto, F., Lenig, D., Mackay, C. R. & Lanzavecchia, A. Flexible programs of chemokine receptor expression on human polarized T helper 1 and 2 lymphocytes. J. Exp. Med. 187, 875–883 (1998).
Loetscher, M., Loetscher, P., Brass, N., Meese, E. & Moser, B. Lymphocyte-specific chemokine receptor CXCR3: regulation, chemokine binding and gene localization. Eur. J. Immunol. 28, 3696–3705 (1998).
Echchannaoui, H. et al. Toll-like receptor 2-deficient mice are highly susceptible to Streptococcus pneumoniae meningitis because of reduced bacterial clearing and enhanced inflammation. J. Infect. Dis. 186, 798–806 (2002).
Qing, Z. et al. Inhibition of antigen-specific T cell trafficking into the central nervous system via blocking PECAM1/CD31 molecule. J. Neuropathol. Exp. Neurol. 60, 798–807 (2001).
Graesser, D. et al. Altered vascular permeability and early onset of experimental autoimmune encephalomyelitis in PECAM-1-deficient mice. J. Clin. Invest. 109, 383–392 (2002).
Hickey, W. F. & Kimura, H. Perivascular microglial cells of the CNS are bone marrow-derived and present antigen in vivo. Science 239, 290–292 (1988). Using bone-marrow chimaeras, the authors show that perivascular mononuclear phagocytes that are derived from the marrow are sufficient to restimulate encephalitogenic T cells in the CNS.
Hickey, W. F. Leukocyte traffic in the central nervous system: the participants and their roles. Semin. Immunol. 11, 125–137 (1999).
Lassmann, H., Schmied, M., Vass, K. & Hickey, W. F. Bone marrow derived elements and resident microglia in brain inflammation. Glia 7, 19–24 (1993).
Kerfoot, S. M. & Kubes, P. Overlapping roles of P-selectin and α4 integrin to recruit leukocytes to the central nervous system in experimental autoimmune encephalomyelitis. J. Immunol. 169, 1000–1006 (2002).
Wekerle, H. & Fierz, W. T cell approach to demyelinating diseases. Springer Semin. Immunopathol. 8, 97–110 (1985).
Piccio, L. et al. Molecular mechanisms involved in lymphocyte recruitment in inflamed brain microvessels: critical roles for P-selectin glycoprotein ligand-1 and heterotrimeric G(i)-linked receptors. J. Immunol. 168, 1940–1949 (2002). This paper describes a new intravital-microscopy approach to examine the microvessels of the brain parenchyma, and shows that interaction between encephalitogenic T-cell blasts and unactivated cerebral microvessels is a low-efficiency event.
Vajkoczy, P., Laschinger, M. & Engelhardt, B. α4-integrin-VCAM-1 binding mediates G protein-independent capture of encephalitogenic T cell blasts to CNS white matter microvessels. J. Clin. Invest. 108, 557–565 (2001). Using intravital microscopy to analyse the trafficking to spinal-cord white matter, this paper indicates an unusual mechanism of integrin-mediated direct capture of T-cell blasts.
Linthicum, D. S., Munoz, J. J. & Blaskett, A. Acute experimental autoimmune encephalomyelitis in mice. I. Adjuvant action of Bordetella pertussis is due to vasoactive amine sensitization and increased vascular permeability of the central nervous system. Cell. Immunol. 73, 299–310 (1982).
Zeine, R. & Owens, T. Direct demonstration of the infiltration of murine central nervous system by Pgp-1/CD44high CD45RBlow CD4+ T cells that induce experimental allergic encephalomyelitis. J. Neuroimmunol. 40, 57–69 (1992).
Yednock, T. A. et al. Prevention of experimental autoimmune encephalomyelitis by antibodies against α4β1 integrin. Nature 356, 63–66 (1992).
Kent, S. J. et al. A monoclonal antibody to α4 integrin suppresses and reverses active experimental allergic encephalomyelitis. J. Neuroimmunol. 58, 1–10 (1995).
Keszthelyi, E. et al. Evidence for a prolonged role of α4 integrin throughout active experimental allergic encephalomyelitis. Neurology 47, 1053–1059 (1996).
Theien, B. E. et al. Discordant effects of anti-VLA-4 treatment before and after onset of relapsing experimental autoimmune encephalomyelitis. J. Clin. Invest. 107, 995–1006 (2001).
Tubridy, N. et al. The effect of anti-α4 integrin antibody on brain lesion activity in MS. The UK Antegren Study Group. Neurology 53, 466–472 (1999).
Miller, D. H. et al. A controlled trial of natalizumab for relapsing multiple sclerosis. N. Engl. J. Med. 348, 15–23 (2003). After a decade of research, this paper reports on a successful Phase II clinical trial for multiple sclerosis using blockade of a specific trafficking determinant.
Lin, K. C. & Castro, A. C. Very late antigen 4 (VLA4) antagonists as anti-inflammatory agents. Curr. Opin. Chem. Biol. 2, 453–457 (1998).
Brennan, F. R. et al. CD44 is involved in selective leucocyte extravasation during inflammatory central nervous system disease. Immunol. 98, 427–435 (1999).
Welsh, C. T., Rose, J. W., Hill, K. E. & Townsend, J. J. Augmentation of adoptively transferred experimental allergic encephalomyelitis by administration of a monoclonal antibody specific for LFA-1α. J. Neuroimmunol. 43, 161–167 (1993).
Cannella, B., Cross, A. H. & Raine, C. S. Anti-adhesion molecule therapy in experimental autoimmune encephalomyelitis. J. Neuroimmunol. 46, 43–55 (1993).
Kobayashi, Y. et al. Antibodies against leukocyte function-associated antigen-1 and against intercellular adhesion molecule-1 together suppress the progression of experimental allergic encephalomyelitis. Cell. Immunol. 164, 295–305 (1995).
Gordon, E. J., Myers, K. J., Dougherty, J. P., Rosen, H. & Ron, Y. Both anti-CD11a (LFA-1) and anti-CD11b (MAC-1) therapy delay the onset and diminish the severity of experimental autoimmune encephalomyelitis. J. Neuroimmunol. 62, 153–160 (1995).
Brocke, S., Piercy, C., Steinman, L., Weissman, I. L. & Veromaa, T. Antibodies to CD44 and integrin α4, but not L-selectin, prevent central nervous system inflammation and experimental encephalomyelitis by blocking secondary leukocyte recruitment. Proc. Natl Acad. Sci. USA 96, 6896–6901 (1999).
Engelhardt, B., Vestweber, D., Hallmann, R. & Schulz, M. E- and P-selectin are not involved in the recruitment of inflammatory cells across the blood–brain barrier in experimental autoimmune encephalomyelitis. Blood 90, 4459–4472 (1997).
Carvalho-Tavares, J. et al. A role for platelets and endothelial selectins in tumor necrosis factor-α-induced leukocyte recruitment in the brain microvasculature. Circ. Res. 87, 1141–1148 (2000).
Grewal, I. S. et al. CD62L is required on effector cells for local interactions in the CNS to cause myelin damage in experimental allergic encephalomyelitis. Immunity 14, 291–302 (2001).
Fife, B. T. et al. CXCL10 (IFN-γ-inducible protein-10) control of encephalitogenic CD4+ T cell accumulation in the central nervous system during experimental autoimmune encephalomyelitis. J. Immunol. 166, 7617–7624 (2001).
Karpus, W. J. et al. An important role for the chemokine macrophage inflammatory protein-1 α in the pathogenesis of the T cell-mediated autoimmune disease, experimental autoimmune encephalomyelitis. J. Immunol. 155, 5003–5010 (1995). The first paper to show an essential role for one chemokine in mouse adoptive-transfer experimental autoimmune encephalomyelitis (EAE).
Tran, E. H., Kuziel, W. A. & Owens, T. Induction of experimental autoimmune encephalomyelitis in C57BL/6 mice deficient in either the chemokine macrophage inflammatory protein-1α or its CCR5 receptor. Eur. J. Immunol. 30, 1410–1415 (2000).
Yoneyama, H. et al. Pivotal role of dendritic cell-derived CXCL10 in the retention of T helper cell 1 lymphocytes in secondary lymph nodes. J. Exp. Med. 195, 1257–1266 (2002).
Narumi, S. et al. Neutralization of IFN-inducible protein 10/CXCL10 exacerbates experimental autoimmune encephalomyelitis. Eur. J. Immunol. 32, 1784–1791 (2002).
Skundric, D. S., Kim, C., Tse, H. Y. & Raine, C. S. Homing of T cells to the central nervous system throughout the course of relapsing experimental autoimmune encephalomyelitis in Thy-1 congenic mice. J. Neuroimmunol. 46, 113–121 (1993).
Brabb, T. et al. In situ tolerance within the central nervous system as a mechanism for preventing autoimmunity. J. Exp. Med. 192, 871–880 (2000). This paper reports the remarkable observation that T-cell receptor (TCR)-transgenic T cells of a naive phenotype migrate efficiently and spontaneously to the CNS.
Flügel, A. et al. Migratory activity and functional changes of green fluorescent effector cells before and during experimental autoimmune encephalomyelitis. Immunity 14, 547–560 (2001). The authors describe a stringently regulated programme of expression of activation and migration determinants that accompanies the journey of encephalitogenic T cells from the blood to the lymphoid organs to the brain.
Hickey, W. F. Migration of hematogenous cells through the blood–brain barrier and the initiation of CNS inflammation. Brain Pathol. 1, 97–105 (1991). This report includes a summary of the early work on the accumulation of activated T-cell blasts in the CNS.
Carrithers, M. D., Visintin, I., Kang, S. J. & Janeway, C. A. Jr. Differential adhesion molecule requirements for immune surveillance and inflammatory recruitment. Brain 123, 1092–1101 (2000).
Huseby, E. S. et al. A pathogenic role for myelin-specific CD8+ T cells in a model for multiple sclerosis. J. Exp. Med. 194, 669–676 (2001).
Babbe, H. et al. Clonal expansions of CD8+ T cells dominate the T cell infiltrate in active multiple sclerosis lesions as shown by micromanipulation and single cell polymerase chain reaction. J. Exp. Med. 192, 393–404 (2000).
Neumann, H., Medana, I. M., Bauer, J. & Lassmann, H. Cytotoxic T lymphocytes in autoimmune and degenerative CNS diseases. Trends Neurosci. 25, 313–319 (2002).
Campbell, J. J. et al. Unique subpopulations of CD56+ NK and NK-T peripheral blood lymphocytes identified by chemokine receptor expression repertoire. J. Immunol. 166, 6477–6482 (2001).
Gao, Y. L., Rajan, A. J., Raine, C. S. & Brosnan, C. F. γδ T cells express activation markers in the central nervous system of mice with chronic-relapsing experimental autoimmune encephalomyelitis. J. Autoimmun. 17, 261–271 (2001).
Rajan, A. J., Asensio, V. C., Campbell, I. L. & Brosnan, C. F. Experimental autoimmune encephalomyelitis on the SJL mouse: effect of γδ T cell depletion on chemokine and chemokine receptor expression in the central nervous system. J. Immunol. 164, 2120–2130 (2000).
Cardona, A. E., Restrepo, B. I., Jaramillo, J. M. & Teale, J. M. Development of an animal model for neurocysticercosis: immune response in the central nervous system is characterized by a predominance of γδ T cells. J. Immunol. 162, 995–1002 (1999).
Cardona, A. E. & Teale, J. M. γδ T cell-deficient mice exhibit reduced disease severity and decreased inflammatory response in the brain in murine neurocysticercosis. J. Immunol. 169, 3163–3171 (2002).
Brosnan, C. F., Bornstein, M. B. & Bloom, B. R. The effects of macrophage depletion on the clinical and pathologic expression of experimental allergic encephalomyelitis. J. Immunol. 126, 614–620 (1981).
Huitinga, I., van Rooijen, N., de Groot, C. J., Uitdehaag, B. M. & Dijkstra, C. D. Suppression of experimental allergic encephalomyelitis in Lewis rats after elimination of macrophages. J. Exp. Med. 172, 1025–1033 (1990).
Fife, B. T., Huffnagle, G. B., Kuziel, W. A. & Karpus, W. J. CC chemokine receptor 2 is critical for induction of experimental autoimmune encephalomyelitis. J. Exp. Med. 192, 899–905 (2000).
Huang, D. R., Wang, J., Kivisäkk, P., Rollins, B. J. & Ransohoff, R. M. Absence of monocyte chemoattractant protein 1 in mice leads to decreased local macrophage recruitment and antigen-specific T helper cell type 1 immune response in experimental autoimmune encephalomyelitis. J. Exp. Med. 193, 713–726 (2001).
Izikson, L., Klein, R. S., Charo, I. F., Weiner, H. L. & Luster, A. D. Resistance to experimental autoimmune encephalomyelitis in mice lacking the CC chemokine receptor (CCR)2. J. Exp. Med. 192, 1075–1080 (2000)
Ma, M. et al. Monocyte recruitment and myelin removal are delayed following spinal cord injury in mice with CCR2 chemokine receptor deletion. J. Neurosci. Res. 68, 691–702 (2002).
Rottman, J. B. et al. Leukocyte recruitment during onset of experimental allergic encephalomyelitis is CCR1 dependent. Eur. J. Immunol. 30, 2372–2377 (2000).
Huo, Y. et al. The chemokine KC, but not monocyte chemoattractant protein-1, triggers monocyte arrest on early atherosclerotic endothelium. J. Clin. Invest. 108, 1307–1314 (2001).
Rollins, B. J. Chemokines and atherosclerosis: what Adam Smith has to say about vascular disease. J. Clin. Invest. 108, 1269–1271 (2001).
Kelsall, B. L., Biron, C. A., Sharma, O. & Kaye, P. M. Dendritic cells at the host-pathogen interface. Nature Immunol. 3, 699–702 (2002).
McMenamin, P. G. Distribution and phenotype of dendritic cells and resident tissue macrophages in the dura mater, leptomeninges, and choroid plexus of the rat brain as demonstrated in wholemount preparations. J. Comp. Neurol. 405, 553–562 (1999).
Matyszak, M. K. & Perry, V. H. The potential role of dendritic cells in immune-mediated inflammatory diseases in the central nervous system. Neuroscience 74, 599–608 (1996).
Serafini, B., Columba-Cabezas, S., Di Rosa, F. & Aloisi, F. Intracerebral recruitment and maturation of dendritic cells in the onset and progression of experimental autoimmune encephalomyelitis. Am. J. Pathol. 157, 1991–2002 (2000).
Fischer, H. G., Bonifas, U. & Reichmann, G. Phenotype and functions of brain dendritic cells emerging during chronic infection of mice with Toxoplasma gondii. J. Immunol. 164, 4826–4834 (2000).
Reichmann, G., Schroeter, M., Jander, S. & Fischer, H. G. Dendritic cells and dendritic-like microglia in focal cortical ischemia of the mouse brain. J. Neuroimmunol. 129, 125–132 (2002).
Pashenkov, M. et al. Recruitment of dendritic cells to the cerebrospinal fluid in bacterial neuroinfections. J. Neuroimmunol. 122, 106–116 (2002).
Pashenkov, M. et al. Two subsets of dendritic cells are present in human cerebrospinal fluid. Brain 124, 480–492 (2001).
Sallusto, F. et al. Rapid and coordinated switch in chemokine receptor expression during dendritic cell maturation. Eur. J. Immunol. 28, 2760–2769 (1998).
Knopf, P. M. et al. Antigen-dependent intrathecal antibody synthesis in the normal rat brain: tissue entry and local retention of antigen-specific B cells. J. Immunol. 161, 692–701 (1998).
Anthony, D. et al. CXC chemokines generate age-related increases in neutrophil-mediated brain inflammation and blood–brain barrier breakdown. Curr. Biol. 8, 923–926 (1998).
Bell, M. D. et al. Recombinant human adenovirus with rat MIP-2 gene insertion causes prolonged PMN recruitment to the murine brain. Eur. J. Neurosci. 8, 1803–1811 (1996).
Tani, M. et al. Neutrophil infiltration, glial reaction, and neurological disease in transgenic mice expressing the chemokine N51/KC in oligodendrocytes. J. Clin. Invest. 98, 529–539 (1996).
Kielian, T. & Hickey, W. F. Proinflammatory cytokine, chemokine, and cellular adhesion molecule expression during the acute phase of experimental brain abscess development. Am. J. Pathol. 157, 647–658 (2000).
Kielian, T., Barry, B. & Hickey, W. F. CXC chemokine receptor-2 ligands are required for neutrophil-mediated host defense in experimental brain abscesses. J. Immunol. 166, 4634–4643 (2001).
Luther, S. A. & Cyster, J. G. Chemokines as regulators of T cell differentiation. Nature Immunol. 2, 102–107 (2001).
Baron, J. L., Madri, J. A., Ruddle, N. H., Hashim, G. & Janeway, C. A. Jr. Surface expression of α4 integrin by CD4 T cells is required for their entry into brain parenchyma. J. Exp. Med. 177, 57–68 (1993).
Kuchroo, V. K. et al. Cytokines and adhesion molecules contribute to the ability of myelin proteolipid protein-specific T cell clones to mediate experimental allergic encephalomyelitis. J. Immunol. 151, 4371–4382 (1993).
Steffen, B. J., Butcher, E. C. & Engelhardt, B. Evidence for involvement of ICAM-1 and VCAM-1 in lymphocyte interaction with endothelium in experimental autoimmune encephalomyelitis in the central nervous system in the SJL/J mouse. Am. J. Pathol. 145, 189–201 (1994).
Tang, T., Frenette, P. S., Hynes, R. O., Wagner, D. D. & Mayadas, T. N. Cytokine-induced meningitis is dramatically attenuated in mice deficient in endothelial selectins. J. Clin. Invest. 97, 2485–2490 (1996).
Archelos, J. J. et al. Inhibition of experimental autoimmune encephalomyelitis by an antibody to the intercellular adhesion molecule ICAM-1. Ann. Neurol. 34, 145–154 (1993).
Willenborg, D. O., Simmons, R. D., Tamatani, T. & Miyasaka, M. ICAM-1-dependent pathway is not critically involved in the inflammatory process of autoimmune encephalomyelitis or in cytokine-induced inflammation of the central nervous system. J. Neuroimmunol. 45, 147–154 (1993).
Dopp, J. M., Breneman, S. M. & Olschowka, J. A. Expression of ICAM-1, VCAM-1, L-selectin, and leukosialin in the mouse central nervous system during the induction and remission stages of experimental allergic encephalomyelitis. J. Neuroimmunol. 54, 129–144 (1994).
Samoilova, E. B., Horton, J. L. & Chen, Y. Experimental autoimmune encephalomyelitis in intercellular adhesion molecule-1-deficient mice. Cell. Immunol. 190, 83–89 (1998).
Engelhardt, B. et al. The development of experimental autoimmune encephalomyelitis in the mouse requires α4-integrin but not α4β7-integrin. J. Clin. Invest. 102, 2096–2105 (1998).
Kanwar, J. R., Kanwar, R. K., Wang, D. & Krissansen, G. W. Prevention of a chronic progressive form of experimental autoimmune encephalomyelitis by an antibody against mucosal addressin cell adhesion molecule-1, given early in the course of disease progression. Immunol. Cell Biol. 78, 641–645 (2000).
Kanwar, J. R. et al. β7 integrins contribute to demyelinating disease of the central nervous system. J. Neuroimmunol. 103, 146–152 (2000).
Stein, J. V. et al. L-selectin-mediated leukocyte adhesion in vivo: microvillous distribution determines tethering efficiency, but not rolling velocity. J. Exp. Med. 189, 37–50 (1999).
von Andrian, U. H., Hasslen, S. R., Nelson, R. D., Erlandsen, S. L. & Butcher, E. C. A central role for microvillous receptor presentation in leukocyte adhesion under flow. Cell 82, 989–999 (1995).
Berlin, C. et al. α4 integrins mediate lymphocyte attachment and rolling under physiologic flow. Cell 80, 413–422 (1995).
Springer, T. A. Traffic signals for lymphocyte recirculation and leukocyte emigration: the multistep paradigm. Cell 76, 301–314 (1994).
Hughes, P. E. & Pfaff, M. Integrin affinity modulation. Trends Cell Biol. 8, 359–364 (1998).
Schwartz, M. A., Schaller, M. D. & Ginsberg, M. H. Integrins: emerging paradigms of signal transduction. Annu. Rev. Cell Dev. Biol. 11, 549–599 (1995).
Foxman, E. F., Campbell, J. J. & Butcher, E. C. Multistep navigation and the combinatorial control of leukocyte chemotaxis. J. Cell Biol. 139, 1349–1360 (1997).
Campbell, J. J. & Butcher, E. C. Chemokines in tissue-specific and microenvironment-specific lymphocyte homing. Curr. Opin. Immunol. 12, 336–341 (2000).
Ansel, K. M., Harris, R. B. & Cyster, J. G. CXCL13 is required for B1 cell homing, natural antibody production, and body cavity immunity. Immunity 16, 67–76 (2002). The first description of subset-specific leukocyte migration from the blood into a tissue cavity.
Kivisäkk, P. et al. Human cerebrospinal fluid central memory CD4+ T cells: evidence for trafficking through choroid plexus and meninges via P-selectin. Proc. Natl Acad. Sci. USA (in the press)
Acknowledgements
The authors would like to thank S. M. Staugaitis and J. J. Campbell for an insightful critique of this paper. We also acknowledge J. Teale, A. Cardona and A. Luster for communicating results before publication. Research in Dr. Ransohoff's laboratory is supported by the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Related links
Glossary
- BLOOD-BRAIN BARRIER (BBB).
-
The physiological barrier that separates blood from brain parenchyma. It consists of endothelial cells with tight junctions that are surrounded by a continuous basement membrane and astroglial end-feet.
- MICROGLIA
-
Interstitial cells of mesodermal origin that form part of the supporting structure of the central nervous system. They have a migratory capacity and function as phagocytes of the nervous tissue.
- ASTROGLIA
-
Star-shaped cells of ectodermal origin that provide nutrients, support and insulation for neurons.
- SUBARACHNOID SPACE
-
A space between the arachnoid and pial membranes that surround the brain and spinal cord that is filled with cerebrospinal fluid. It contains fibrous trabeculae, blood vessels and antigen-presenting cells.
- EXPERIMENTAL AUTOIMMUNE ENCEPHALOMYELITIS (EAE).
-
An animal model that mimics some of the clinical and histopathological characteristics of multiple sclerosis. EAE can be induced in various species by immunization with myelin antigens or adoptive transfer of neuroantigen-specific T cells.
- TIGHT JUNCTIONS
-
Intercellular junctions where adjacent plasma membranes are joined tightly together, occluding the intercellular space and limiting the intercellular passage of molecules.
- VIRCHOW–ROBIN SPACE
-
A space that surrounds blood vessels for a short distance as they enter the brain from the cortical surface, defined by extensions of the arachnoid and pial membranes.
- MICROVILLI
-
Small processes or protrusions from the cell surface that increase the surface size of the cell.
- CENTRAL MEMORY T CELLS
-
Previously activated memory T cells that have encountered antigen in secondary lymphoid organs and obtained the capacity to migrate through extralymphoid tissues, but retain receptors and ligands, such as CC-chemokine receptor 7 and L-selectin, allowing the cells to return to the lymphoid compartment.
- T HELPER 1/2 CELLS (TH1/TH2).
-
Activated CD4+ T cells differentiate into two distinct phenotypes that are associated with highly polarized immune responses. Generally, TH1 cells produce high levels of interferon-γ, lymphotoxin and tumour-necrosis factor, and are associated with cell-mediated immunity, whereas TH2 cells produce high levels of interleukin-4 (IL-4), IL-5 and IL-13, and are associated with humoral immunity.
- TOLL-LIKE RECEPTORS (TLRs).
-
A family of receptors that recognize conserved products that are unique to microorganisms, such as lipopolysaccharide. Stimulation through TLRs induces maturation and activation of dendritic cells, leading to optimal activation of the adaptive immune response.
Rights and permissions
About this article
Cite this article
Ransohoff, R., Kivisäkk, P. & Kidd, G. Three or more routes for leukocyte migration into the central nervous system. Nat Rev Immunol 3, 569–581 (2003). https://doi.org/10.1038/nri1130
Issue Date:
DOI: https://doi.org/10.1038/nri1130
This article is cited by
-
Imaging of brain barrier inflammation and brain fluid drainage in human neurological diseases
Cellular and Molecular Life Sciences (2024)
-
The novel HS-mimetic, Tet-29, regulates immune cell trafficking across barriers of the CNS during inflammation
Journal of Neuroinflammation (2023)
-
Neonatal immune challenge poses a sex-specific risk for epigenetic microglial reprogramming and behavioral impairment
Nature Communications (2023)
-
Astrocyte reactivity and inflammation-induced depression-like behaviors are regulated by Orai1 calcium channels
Nature Communications (2023)
-
Mechanisms of myeloid cell entry to the healthy and diseased central nervous system
Nature Immunology (2023)