Abstract
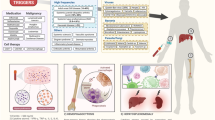
Hemophagocytic syndrome (HPS) is a rare but distinct condition caused by inappropriate and dysregulated activation of the immune system. HPS is characterized by febrile hepatosplenomegaly, pancytopenia, hypofibrinemia and liver dysfunction; these changes are associated with the infiltration of bone marrow and organs by nonmalignant macrophages that phagocytose blood cells. Primary HPS is linked to inherited immune dysregulation, whereas secondary HPS tends to be triggered by an infectious or neoplastic disease. Multiorgan failure can complicate this life-threatening condition and renal involvement has frequently been reported; however, precise descriptions of the renal manifestations of HPS are lacking. Acute kidney injury due to tubular necrosis is the most common renal presentation, but nephrotic syndrome can also occur. HPS can be observed in immunocompromised patients and nephrologists must be aware that this condition can occur in renal transplant recipients. Mortality in patients with HPS can be as high as 50%. Despite considerable advances in the treatment of familial HPS, no specific therapy has demonstrated a consistent capacity to control reactive HPS when combined with suppression of the triggering factor. This Review summarizes the presentation, causes, pathophysiology and renal features of HPS for the benefit of the practicing nephrologist.
Key Points
-
Hemophagocytic syndrome (HPS) is characterized by proliferation of and organ infiltration with benign activated macrophages, which results in febrile cytopenia and a dysregulated inflammatory response that can lead to multiorgan failure
-
Primary HPS occurs in children with inherited dysfunction of the immune response, whereas secondary HPS is triggered by factors such as infectious agents, autoimmune disease and neoplasia
-
Acute kidney injury due to tubular necrosis is the most frequent type of kidney involvement in HPS
-
Nephrotic syndrome can be observed in the acute phase of HPS; the associated renal pathology is usually minimal-change disease or collapsing glomerulopathy, although thrombotic microangiopathy has also been described
-
Patients who receive immunosuppressive treatment after organ transplantation or for autoimmune disease are at increased risk of HPS
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Risdall, R. J. et al. Virus-associated hemophagocytic syndrome: a benign histiocytic proliferation distinct from malignant histiocytosis. Cancer 44, 993–1002 (1979).
Wong, K. & Chan, J. K. Reactive hemophagocytic syndrome: a clinicopathologic study of 40 patients in an Oriental population. Am. J. Med. 93, 177–180 (1992).
Reiner, A. & Spivak, J. L. Hemophagocytic histiocytosis: a report of 23 new patients and a review of the literature. Medicine (Baltimore) 67, 369–388 (1988).
Tsuda, H. Hemophagocytic syndrome in children and adults. Int. J. Hematol. 65, 215–226 (1997).
Kaito, K. et al. Prognostic factors of hemophagocytic syndrome in adults: analysis of 34 cases. Eur. J. Haematol. 59, 247–253 (1997).
Scott, R. B. et al. Histiocytic medullary reticulocytosis. Lancet 2, 194–198 (1939).
Farquhar, J. W. et al. Familial hemophagocytic reticulocytosis. Arch. Dis. Child. 27, 519–525 (1952).
Gauvin, F., Toledano, B., Champagne, J. & Lacroix, J. Reactive hemophagocytic syndrome presenting as a component of multiple organ dysfunction syndrome. Crit. Care Med. 28, 3341–3345 (2000).
Ohga, S. Inflammatory cytokines in virus-associated hemophagocytic syndrome. Am. J. Pediatr. Hematol. Oncol. 15, 291–298 (1993).
De Kerguenec, C. et al. Hepatic manifestations of hemophagocytic syndrome: a study of 30 cases. Am. J. Gastroenterol. 96, 852–857 (2001).
Esumi, N. Ikushima, S., Todo, S. & Imashuku, S. Hyperferritinemia in malignant histiocytosis and virus-associated hemophagocytic syndrome. N. Engl. J. Med. 316, 346–347 (1987).
Henter, J. I. et al. Treatment of hemophagocytic lymphohistiocytosis with HLH-94 immunotherapy and bone marrow transplantation. Blood 100, 2367–2373 (2002).
Strauss R. et al. Multifactorial risk analysis of bone marrow histiocytic hyperplasia with hemophagocytosis in critically ill medical patient: a postmortem clinicopathologic analysis. Crit. Care Med. 32, 1316–1321 (2004).
Janka, G. E. Hemophagocytic syndromes. Blood Rev. 21, 245–253 (2007).
Aricó, M. et al. Pathogenesis of haemophagocytic lymphohistiocytosis. Br. J. Haematol. 114, 761–769 (2001).
Stepp, S. E. et al. Perforin gene defects in familial hemophagocytic lymphohistiocytosis. Science 286, 1957–1959 (1999).
Feldmann, J. et al. Munc13-4 is essential for cytolytic granules fusion and is mutated in a form of familial hemophagocytic lymphohistiocytosis (FHL3). Cell 115, 461–473 (2003).
Zur Stadt, U. et al. Linkage of familial hemophagocytic lymphohistiocytosis (FHL) type-4 to chromosome 6q24 and identification of mutations in syntaxin 11. Hum. Mol. Genet. 14, 827–834 (2005).
Certain, S. et al. Protein truncation test of LYST reveals heterogeneous mutations in patients with Chediak–Higashi syndrome. Blood 95, 979–983 (2000).
Menasché, G. et al. Mutations in RAB27A cause Griscelli syndrome associated with haemophagocytic syndrome. Nat. Genet. 25, 173–176 (2000).
Arico, M. et al. Hemophagocytic lymphohistiocytosis due to germline mutations in SH2D1A, the X-linked lymphoproliferative disease gene. Blood 97, 1131–1133 (2001).
Fisman, D. N. Hemophagocytic syndromes and infection. Emerg. Infect. Dis. 6, 601–608 (2000).
Rouphael, N. G. et al. Infections associated with haemophagocytic syndrome. Lancet Infect. Dis. 7, 814–822 (2007).
Han, A. R. et al. Lymphoma-associated hemophagocytic syndrome: clinical features and treatment outcome. Ann. Hematol. 86, 493–498 (2007).
Fardet, L. et al. HHV-8 associated hemophagocytic lymphohistiocytosis in HIV-infected patients. Clin. Infect. Dis. 37, 285–291 (2003).
Chuang, H. C. et al. EBV latent membrane protein-1 down-regulates TNF-α receptor-1 and confers resistance to TNF-α-induced apoptosis in T cells: implication for the progression to T-cell lymphoma in EBV-associated hemophagocytic syndrome. Am. J. Pathol. 170, 1607–1617 (2007).
Karras, A. et al. Syndrome d'activation macrophagique/hemophagocytic syndrome [French]. Rev. Med. Interne. 23, 768–778 (2002).
Dhote, R. et al. Reactive hemophagocytic syndrome in adult systemic disease: report of twenty-six cases and literature review. Arthritis Rheum. 49, 633–639 (2003).
Stéphan, J. L. et al. Reactive haemophagocytic syndrome in children with inflammatory disorders: a retrospective study of 24 patients. Rheumatology (Oxford) 40, 1285–1292 (2001).
Lambotte, O. et al. Characteristics and long-term outcome of 15 episodes of systemic lupus erythematosus-associated hemophagocytic syndrome. Medicine (Baltimore) 85, 169–182 (2006).
Arlet, J. B. et al. Reactive haemophagocytic syndrome in adult-onset Still's disease: a report of six patients and a review of the literature. Ann. Rheum. Dis. 65, 1596–1601 (2006).
Lee, S. M. et al. Characterization of diverse PRF1 mutations leading to decreased natural killer cell activity in North American families with hemophagocytic lymphohistiocytosis. J. Med. Genet. 41, 137–144 (2004).
Osugi, Y. et al. Cytokine production regulating TH1 and TH2 cytokines in hemophagocytic lymphohistiocytosis. Blood 89, 4100–4103 (1997).
Akashi, K. et al. Involvement of interferon-γ and macrophage colony-stimulating factor in pathogenesis of haemophagocytic lymphohistiocytosis in adults. Br. J. Haematol. 87, 243–250 (1994).
Ueda, I. et al. Late-onset cases of familial hemophagocytic lymphohistiocytosis with missense perforin gene mutations. Am. J. Hematol. 82, 427–432 (2007).
Hazen, M. M. et al. Mutations of the hemophagocytic lymphohistiocytosis-associated gene UNC13D in a patient with systemic juvenile idiopathic arthritis. Arthritis Rheum. 58, 567–570 (2008).
Nahum, E. et al. Hemophagocytic lymphohistiocytic syndrome: unrecognized cause of multiple organ failure. Pediatr. Crit. Care Med. 1, 51–54 (2000).
Sawhney, S., Woo, P. & Murray, K. J. Macrophage activation syndrome: a potentially fatal complication of rheumatic disorders. Arch. Dis. Child. 85, 421–426 (2001).
Fitzgerald, N. E. & MacClain, K. L. Imaging charcteristics of hemophagocytic lymphohistiocytosis. Pediatr. Radiol. 33, 392–401 (2003).
Wan, L., Bellomo, R., Di Giantomasso, D. & Ronco, C. The pathogenesis of septic acute renal failure. Curr. Opin. Crit. Care 9, 496–502 (2003).
Thaunat, O. et al. Nephrotic syndrome associated with hemophagocytic syndrome. Kidney Int. 69, 1892–1898 (2006).
Karras, A. et al. Hemophagocytic syndrome in renal transplant recipients: report of 17 cases and review of literature. Transplantation 77, 238–243 (2004).
Ponzoni, M. et al. Definition, diagnosis and management of intravascular large B-cell lymphoma: proposals and perspectives from an international consensus meeting. J. Clin. Oncol. 25, 3168–3173 (2007).
Braun, M. C., Cohn, R. A. & Kletzel, M. Nephrotic syndrome accompanying familial hemophagocytic syndrome. J. Pediatr. Hematol. Oncol. 18, 195–197 (1996).
Chiang, W. C. et al. Thrombotic microangiopathy in hemophagocytic syndrome: a case report. J. Formos. Med. Assoc. 101, 362–367 (2002).
McCarthy, E. T. et al. TNF-α increases albumin permeability of isolated rat glomeruli through the generation of superoxide. J. Am. Soc. Nephrol. 9, 433–438 (1998).
Koukouritaki, S. B. et al. TNF-α induces actin cytoskeleton reorganization in glomerular epithelial cells involving tyrosine phosphorylation of paxillin and focal adhesion kinase. Mol. Med. 5, 382–392 (1999).
Nakabayashi, M., Adachi, T., Izuchi, S. & Sugisaki, A. Association of hypercytokinemia in the development of severe preeclampsia in a case of hemophagocytic syndrome. Semin. Thromb. Hemost. 25, 467–471 (1999).
Pérard, L. et al. Hemophagocytic syndrome in a pregnant patient with systemic lupus erythematosus, complicated with preeclampsia and cerebral hemorrhage. Ann. Hematol. 86, 541–544 (2007).
Fischer, A. et al. Treatment of four patients with erythrophagocytic lymphohistiocytosis by a combination of epipodophyllotoxin, steroids, intrathecal methotrexate and cranial irradiation. Pediatrics 76, 263–268 (1985).
Tsuda, H. & Shirono, K. Successful treatment of virus-associated haemophagocytic syndrome in adults by cyclosporin A supported by G-CSF. Br. J. Haematol. 93, 572–575 (1996).
Gill, D. S., Spencer, A. & Cobcroft, R. G. High-dose γ-globulin therapy in the reactive haemophagocytic syndrome. Br. J. Haematol. 88, 204–206 (1994).
Henzan, T. et al. Success with infliximab in treating refractory hemophagocytic lymphohistiocytosis. Am. J. Hematol. 81, 59–61 (2006).
Takahashi, N., Naniwa, T. & Banno, S. Successful use of etanercept in the treatment of acute lupus hemophagocytic syndrome. Mod. Rheumatol. 18, 72–75 (2008).
Olin, R. L. et al. Successful use of the anti-CD25 antibody daclizumab in an adult patient with hemophagocytic lymphohistiocytosis. Am. J. Hematol. 83, 747–749 (2008).
Balamuth, N. J., Nichols, K. E., Paessler, M. & Teachey, D. T. Use of rituximab in conjunction with immunosuppressive chemotherapy as a novel therapy for Epstein–Barr virus-associated hemophagocytic lymphohistiocytosis. J. Pediatr. Hematol. Oncol. 29, 569–573 (2007).
Behrens, E. M., Kreiger, P. A., Cherian, S. & Cron, R. Q. Interleukin 1 receptor antagonist to treat cytophagic histiocytic panniculitis with secondary hemophagocytic lymphohistiocytosis. J. Rheumatol. 33, 2081–2084 (2006).
Rostaing, L., Fillola, G., Baron, E., Cisterne, J. M. & Durand, D. Course of hemophagocytic syndrome in renal transplant patients. Transplantation 60, 506–509 (1995).
Kürsat, S. et al. Haemophagocytic–histiocytic syndrome in renal transplantation. Nephrol. Dial. Transplant. 12, 1058–1060 (1997).
Asci, G. et al. High-dose immunoglobulin therapy in renal transplant recipients with hemophagocytic histiocytic syndrome. J. Nephrol. 19, 322–326 (2006).
Henter, J. I. et al. HLH-2004: diagnostic and therapeutic guidelines for hemophagocytic lymphohistiocytosis. Pediatr. Blood Cancer. 48, 124–131 (2007).
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
Karras, A. What nephrologists need to know about hemophagocytic syndrome. Nat Rev Nephrol 5, 329–336 (2009). https://doi.org/10.1038/nrneph.2009.73
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneph.2009.73
This article is cited by
-
Isolated massive histiocytes renal interstitial infiltration: a case report of an unexpected cause of acute kidney injury in a kidney transplant recipient
BMC Nephrology (2023)
-
Clinical features and prognostic factors of acute kidney injury caused by adult secondary hemophagocytic lymphohistiocytosis
Journal of Nephrology (2022)
-
Hemophagocytic syndrome with acute kidney injury accompanied by erythrophagocytic macrophages in the tubular lumen
CEN Case Reports (2019)
-
A young child with fever and unexplained acute kidney injury: Answers
Pediatric Nephrology (2018)
-
Acute kidney injury induced by thrombotic microangiopathy in a patient with hemophagocytic lymphohistiocytosis
BMC Nephrology (2016)