Abstract
Radical cystectomy (RC) with subsequent urinary diversion has been assessed to be the most difficult surgical procedure in the field of urology. No randomized trials have been performed to compare the outcomes of noncontinent conduit diversion, neobladder construction and continent cutaneous diversion. Almost all studies are of level 3 evidence, meaning the recommendations given in this Review are of grade C only. Until recently, significant disparity in the quality of surgical complication reporting, as well as the lack of universally accepted reporting guidelines, definitions and grading systems, have made it impossible to compare the surgical morbidity and outcomes of RC. There is a clear case for the standardized reporting of complications. The Clavien system is a straightforward and validated instrument that has already been successfully adopted by several urological centers. Surgical morbidity following RC is significant and, when strict reporting guidelines are incorporated, much higher than previously published. Complications can occur up to 20 years after surgery, emphasizing the need for more long-term studies to determine the full morbidity spectrum. In general, renal function after construction of continent detubularized reservoirs compares favorably with ileal conduit diversion, although the literature is insufficient to recommend one over the other. The challenge of optimum care for elderly patients with comorbidities is best mastered at a high-volume hospital by a high-volume surgeon.
Key Points
-
Radical cystectomy (RC) and subsequent urinary diversion has been assessed to be the most difficult surgical procedure in the field of urology
-
No randomized trials have been performed to compare the outcomes of noncontinent conduit diversion, neobladder construction and continent cutaneous diversion
-
Significant disparity in the quality of surgical complication reporting has made it impossible to compare surgical morbidity in patients who have undergone RC; there is a clear case for the standardized reporting of complications
-
Overall, the perioperative surgical morbidity following RC and urinary diversion is significant and, when strict reporting guidelines are incorporated, much higher than previously published
-
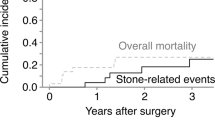
Complications can occur up to 20 years after surgery, emphasizing the need for close monitoring of these patients and more long-term studies to determine the full morbidity spectrum
-
Evidence suggests an association between volume and outcome in cystectomy procedures; the challenge of optimum care for elderly patients with comorbidities is best mastered at high-volume hospitals by high-volume surgeons
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Montie, J. E. in Textbook of Operative Urology (ed. Marshall, F. F.) 396–407 (Saunders, Philadelphia, 1996).
Hautmann, R. E. et al. in Bladder Cancer (eds Soloway, M., Abrams, P. & Khoury, S.) in press (Health Publication Ltd, Paris, 2011).
Hautmann, R. E., de Petriconi R. C. & Volkmer, B. G. Lessons learned from 1,000 neobladders: the 90-day complication rate. J. Urol. 184, 990–994 (2010).
Madersbacher, S. et al. Long-term outcome of ileal conduit diversion. J. Urol. 169, 985–990 (2003).
Shimko, M. S. et al. Long-term complications of conduit urinary diversion. J. Urol. 185, 562–567 (2011).
Froehner, M., Brausi, M. A., Herr, H. W., Muto, G. & Studer, U. E. Complications following radical cystectomy for bladder cancer in the elderly. Eur. Urol. 56, 443–454 (2009).
Konety B. R., Allareddy, V. & Herr, H. Complications after radical cystectomy: analysis of population-based data. Urology 68, 58–64 (2006).
Chang, S. S., Cookson, M. S., Baumgartner, R. G., Wells, N. & Smith, J. A. Jr . Analysis of early complications after radical cystectomy: results of a collaborative care pathway. J. Urol. 167, 2012–2016 (2002).
Cookson, M. S., Chang, S. S., Wells, N., Parekh, D. J. & Smith, J. A. Jr . Complications of radical cystectomy for nonmuscle invasive disease: comparison with muscle invasive disease. J. Urol. 169, 101–104 (2003).
Frazier, H. A., Robertson, J. E. & Paulson, D. F. Complications of radical cystectomy and urinary diversion: a retrospective review of 675 cases in 2 decades. J. Urol. 148, 1401–1405 (1992).
Ghoneim, M. A., el-Mekresh, M. M., el-Baz, M. A., el-Attar, I. A. & Ashamallah, A. Radical cystectomy for carcinoma of the bladder: critical evaluation of the results in 1,026 cases. J. Urol. 158, 393–399 (1997).
Hollenbeck, B. K. et al. Identifying risk factors for potentially avoidable complications following radical cystectomy. J. Urol. 174, 1231–1237 (2005).
Joniau, S. et al. Clinical experience with the N-shaped ileal neobladder: assessment of complications, voiding patterns, and quality of life in our series of 58 patients. Eur. Urol. 47, 666–673 (2005).
Meller, A. E., Nesrallah, L. J., Dall'Oglio, M. F. & Srougi, M. Complications in radical cystectomy performed at a teaching hospital. Int. Braz. J. Urol. 28, 522–525 (2002).
Meyer, J. P. et al. A three-centre experience of orthotopic neobladder reconstruction after radical cystectomy: initial results. BJU Int. 94, 1317–1321 (2004).
Quek, M. L. et al. A critical analysis of perioperative mortality from radical cystectomy. J. Urol. 175, 886–890 (2006).
Breau, R. H. et al. Reporting of harm in randomized controlled trials published in the urological literature. J. Urol. 183, 1693–1697 (2010).
Hautmann, R. E. et al. Urinary diversion. Urology 69 (Suppl. 1), 17–49 (2007).
Gore, J. L. & Litwin, M. S. Quality of care in bladder cancer: trends in urinary diversion following radical cystectomy. World J. Urol. 27, 45–50 (2009).
Donat, S. M. Standards for surgical complication reporting in urologic oncology: time for a change. Urology 69, 221–225 (2007).
Shabsigh, A. et al. Defining early morbidity of radical cystectomy for patients with bladder cancer using a standardized reporting methodology. Eur. Urol. 55, 164–174 (2009).
Hautmann, R. E., de Petriconi R. C. & Volkmer, B. G. Lessons learned from 1,000 neobladders: the 90-day complication rate. J. Urol. 184, 990–994 (2010).
Morgan, M., Smith, N., Thomas, K. & Murphy, D. G. Is Clavien the new standard for reporting urological complications? BJU Int. 104, 434–436 (2009).
Dindo, D., Demartines, N. & Clavien, P. A. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann. Surg. 240, 205–213 (2004).
Stolzenburg, J. U. et al. Categorisation of complications of endoscopic extraperitoneal and laparoscopic transperitoneal radical prostatectomy. World J. Urol. 24, 88–93 (2006).
Constantinides, C. A. et al. Short- and long-term complications of open radical prostatectomy according to the Clavien classification system. BJU Int. 103, 336–340 (2009).
Murphy, D. G., Kerger, M., Crowe, H., Peters, J. S. & Costello, A. J. Operative details and oncological and functional outcome of robotic-assisted laparoscopic radical prostatectomy: 400 cases with a minimum of 12 months follow-up. Eur. Urol. 55, 1358–1366 (2009).
Hayn, M. H., Hellenthal, N. J., Hussain, A., Stegemann, A. P. & Guro, K. A. Defining morbidity of robot-assisted radical cystectomy using a standardized reporting methodology. Eur. Urol. 59, 213–218 (2011).
Gore, J. L. et al. Urinary diversion and morbidity after radical cystectomy for bladder cancer. Cancer 116, 331–339 (2010).
Lawrentschuk, N. et al. Prevention and management of complications following radical cystectomy for bladder cancer. Eur. Urol. 57, 983–1001 (2010).
Williams, O., Vereb, M. J. & Libertino, J. A. Noncontient urinary diversion. Urol. Clin. North Am. 24, 735–744 (1997).
Pernet, F. P. P. M. & Jonas, U. Ileal conduit urinary diversion: Early and late results of 132 cases in a 25-year period. World J. Urol. 3, 140–144 (1985).
Killeen, K. P. & Libertino, J. A. Management of bowel and urinary tract complications after urinary diversion. Urol. Clin. North Am. 15, 183–194 (1988).
Neal, D. E. Complications of ileal conduit diversion in adults with cancer followed up for at least five years. Br. Med. J. 290, 1695–1697 (1985).
Singh, G., Wilkinson, J. M. & Thomas, D. G. Supravesical diversion for incontinence: a long-term follow-up. Br. J. Urol. 79, 348–353 (1997).
Rinnab, L., Straub, M., Hautmann, R. E. & Braendle, E. Postoperative resorptive and excretory capacity of the ileal neobladder. BJU Int. 95, 1289–1292 (2005).
Kristjánsson A., Wallin, L. & Månsson, W. Renal function up to 16 years after conduit (refluxing or anti-reflux anastomosis) or continent urinary diversion. 1. Glomerular filtration rate and patency of uretero-intestinal anastomosis. Br. J. Urol. 7, 539–545 (1995).
Samuel, J. D., Bhatt, R. I., Montague, R. J., Clarke, N. W. & Ramani, V. A. The natural history of postoperative renal function in patients undergoing ileal conduit diversion for cancer measured using serial isotopic glomerular filtration rate and 99m technetium-mercaptoacetyltriglycine renography. J. Urol. 176, 2518–2522 (2006).
Thoeny, H. C., Sonnenschein, M. J., Madersbacher, S., Vock, P. & Studer, U. E. Is ileal orthotopic bladder substitution with an afferent tubular segment detrimental to the upper urinary tract in the long term? J. Urol. 168, 2030–2034 (2002).
Minervini, R. et al. Effects on renal function of obstructive and nonobstructive and dilatation of the upper urinary tract in ileal neobladders with refluxing ureteroenteric anastomoses. Eur. J. Surg. Oncol. 36, 287–291 (2010).
Mills, R. D. & Studer, U. E. Metabolic consequences of continent urinary diversion. J. Urol. 161, 1057–1066 (1999).
Waidelich, R., Rink, F., Kriegmair, M., Tatsch, K. & Schmeller, N. A study of reflux in patients with an ileal orthotopic bladder. Br. J. Urol. 81, 241–246 (1998).
Nesbit, R. M. Ureterosigmoid anastomosis by direct elliptical connection; a preliminary report. J. Urol. 61, 728–734 (1949).
Studer, U. E. et al. Twenty years experience with an ileal orthotopic low pressure bladder substitute—lessons to be learned. J. Urol. 176, 161–166 (2006).
Mattei, A., Birkhaeuser, F. D., Baermann, C., Warncke, S. H. & Studer U. E. To stent or not to stent perioperatively the ureteroileal anastomosis of ileal orthotopic bladder substitutes and ileal conduits? Results of a prospective randomized trial. J. Urol. 179, 582–586 (2008).
Perimenis, P., Burkhard, F. C., Kessler, T. M., Gramann, T. & Studer, U. E. Ileal orthotopic bladder substitute combined with an afferent tubular segment: long-term upper urinary tract changes and voiding pattern. Eur. Urol. 46, 604–609 (2004).
Steers, W. D. Voiding dysfunction in the orthotopic neobladder. World J. Urol. 18, 330–337 (2000).
Hautmann, R. E., Volkmer, B. G., Schumacher, M. C., Gschwend J. E. & Studer, U. E. Long-term results of standard procedures in urology: the ileal neobladder. World J. Urol. 24, 305–314 (2006).
Stein, J. P., Ginsberg, D. A. & Skinner, D. G. Indications and technique of the orthotopic neobladder in women. Urol. Clin. North Am. 29, 725–734 (2002).
Ali-El-Dein, B., Gomha, M. & Ghoneim, M. A. Critical evaluation of the problem of chronic urinary retention after orthotopic bladder substitution in women. J. Urol. 168, 587–592 (2002).
Hautmann, R. E. Urinary diversion: ileal conduit to neobladder. J. Urol. 169, 834–842 (2003).
Stein, J. P., Penson, D. F., Wu, S. D. & Skinner, D. Pathological guidelines for orthotopic urinary diversion in women with bladder cancer: a review of the literature. J. Urol. 178, 756–760 (2007).
Lee, K. S., Montie, J. E., Dunn, R. L. & Lee, C. T. Hautmann and Studer orthotopic neobladders: a contemporary experience. J. Urol. 169, 2188–2191 (2003).
Nagele, U. et al. Radical cystectomy and orthotopic bladder replacement in females. Eur. Urol. 50, 249–257 (2006).
Borirakchanyavat, S., Aboseif, S. R., Carroll, P. R., Tanagho, E. A. & Lue, T. F. Continence mechanism of the isolated female urethra: an anatomical study of the intrapelvic somatic nerves. J. Urol. 158, 822–826 (1997).
Hugonnet, C. L., Danuser, H., Springer, J. P. & Studer, U. E. Decreased sensitivity in the membranous urethra after orthotopic ileal bladder substitute. J. Urol. 161, 418–421 (1999).
Kessler, T. M., Studer, U. E. & Burkhard, F. C. Increased proximal urethral sensory threshold after radical pelvic surgery in women. Neurourol. Urodyn. 26, 208–212 (2007).
Hautmann, R. E., Paiss, T. & de Petriconi, R. The ileal neobladder in women: 9 years of experience with 18 patients. J. Urol. 155, 76–81 (1996).
Stenzl, A. et al. Rationale and technique of nerve sparing radical cystectomy before an orthotopic neobladder procedure in women. J. Urol. 154, 2044–2049 (1995).
Studer, U. E. et al. Twenty years experience with an ileal orthotopic low pressure bladder substitute—lessons to be learned. J. Urol. 176, 161–166 (2006).
Hautmann, R. E., de Petriconi, R., Kleinschmidt, K., Gottfried, H. W. & Gschwend, J. E. Orthotopic ileal neobladder in females: impact of the urethral resection line on functional results. Int. Urogynecol. J. Pelvic Floor Dysfunct. 11, 224–229 (2000).
Bhatta Dhar, N., Kessler, T. M., Mills, R. D., Burkhard, F. & Studer, U. E. Nerve-sparing radical cystectomy and orthotopic bladder replacement in female patients. Eur. Urol. 52, 1006–1014 (2007).
Stein, J. P., Penson, D. F., Wu, S. D. & Skinner, D. Pathological guidelines for orthotopic urinary diversion in women with bladder cancer: a review of the literature. J. Urol. 178, 756–760 (2007).
Simon, J. et al. Neobladder emptying failure in males: incidence, etiology and therapeutic options. J. Urol. 176, 1468–1472 (2006).
Burkhard, F. C. & Studer, U. E. Orthotopic bladder substitution. Curr. Opin. Urol. 10, 343–349 (2000).
Abol-Enein, H. & Ghoneim, M. A. Functional results of orthotopic ileal neobladder with serous-lined extramural ureteral reimplantation: experience with 450 patients. J. Urol. 165, 1427–1432 (2001).
Parekh, D. J., Gilbert, W. B. & Smith, J. A. Jr . Functional lower urinary tract voiding outcomes after cystectomy and orthotopic neobladder. J. Urol. 163, 56–58 (2000).
Porru, D. et al. Urodynamic analysis of voiding dysfunction in orthotopic ileal neobladder. World J. Urol. 17, 285–289 (1999).
Nesrallah, L. J., Srougi, M. & Dall'Oglio, M. F. Orthotopic ileal neobladder: the influence of reservoir volume and configuration on urinary continence and emptying properties. BJU Int. 93, 375–378 (2004).
Shaaban, A. A., Mosbah, A., El-Bahnassawy, M. S., Madbouly, K. & Ghoneim, M. A. The urethral Kock pouch: long-term functional and oncological results in men. BJU Int. 92, 429–435 (2003).
Stein, J. P., Dunn, M. D., Quek, M. L., Miranda, G. & Skinner, D. G. The orthotopic T pouch ileal neobladder: experience with 209 patients. J. Urol. 172, 584–587 (2004).
Carrion, R. et al. A multi-institutional study of orthotopic neobladders: functional results in men and women. BJU Int. 93, 803–806 (2004).
Kulkarni, J. N., Pramesh, C. S., Rathi, S. & Pantvaidya, G. H. Long-term results of orthotopic neobladder reconstruction after radical cystectomy. BJU Int. 91. 485–488 (2003).
Studer, U. E. & Zingg, E. J. Ileal orthotopic bladder substitutes. What we have learned from 12 years' experience with 200 patients. Urol. Clin. North Am. 24, 781–793 (1997).
Brendler, C. B., Steinberg, G. D., Marshall, F. F., Mostwin, J. L. & Walsh, P. C. Local recurrence and survival following nerve-sparing radical cystoprostatectomy. J. Urol. 144, 1137–1140 (1990).
Cole, C. J. et al. Local control of muscle-invasive bladder cancer: preoperative radiotherapy and cystectomy versus cystectomy alone. Int. J. Radiat. Oncol. Biol. Phys. 32, 331–340 (1995).
Greven, K. M., Spera, J. A., Solin, L. J., Morgan, T. & Hanks, G. E. Local recurrence after cystectomy alone for bladder carcinoma. Cancer 69, 2767–2770 (1992).
Herr, H. W. Preoperative irradiation with and without chemotherapy as adjunct to radical cystectomy. Urology 25, 127–134 (1985).
Montie, J. E., Straffon, R. A. & Stewart, B. H. Radical cystectomy without radiation therapy for carcinoma of the bladder. J. Urol. 131, 477–482 (1984).
Skinner, D. G. & Lieskovsky G. Contemporary cystectomy with pelvic node dissection compared to preoperative radiation therapy plus cystectomy in management of invasive bladder cancer. J. Urol. 131, 1069–1072 (1984).
Skinner, D. G., Tift, J. P. & Kaufmann, J. J. High dose, short course preoperative radiation therapy and immediate single stage radical cystectomy with pelvic node dissection in the management of bladder cancer. J. Urol. 127, 671–674 (1982).
Westney, O. L. et al. Presentation, methods of diagnosis and therapy for pelvic recurrence following radical cystectomy for transitional cell carcinoma of the bladder. J. Urol. 159, 792–795 (1998).
Hautmann, R. E. & Simon, J. Ileal neobladder and local recurrence of bladder cancer: patterns of failure and impact on function in men. J. Urol. 162, 1963–1966 (1999).
Thurairaja, R., Burkhard, F. C. & Studer, U. E. The orthotopic neobladder. BJU Int. 102, 1307–1313 (2008).
Varol, C. & Studer, U. E. Managing patients after an ileal orthotopic bladder substitution. BJU Int. 93, 266–270 (2004).
Elting, L. S. et al. Correlation between annual volume of cystectomy, professional staffing, and outcomes: a statewide, population-based study. Cancer 104, 975–984 (2005).
Birkmeyer, J. D. et al. Hospital volume and surgical mortality in the United States. N. Engl. J. Med. 346, 1128–1137 (2002).
Birkmeyer, J. D. et al. Surgeon volume and operative mortality in the United States. N. Engl. J. Med. 349, 2117–2127 (2003).
Birkmeyer, J. D., Sun, Y., Wong, S. L. & Stukel, T. A. Hospital volume and late survival after cancer surgery. Ann. Surg. 245, 777–783 (2007).
Hollenbeck, B. K., Wei, Y. & Birkmeyer, J. D. Volume, process of care, and operative mortality for cystectomy for bladder cancer. Urology 69, 871–875 (2007).
Granberg, C. F. et al. Functional and oncological outcomes after orthotopic neobladder reconstruction in women. BJU Int. 102, 1551–1555 (2008).
Nesrallah, L. J., Almeida, F. G., Dall'Oglio, M. F., Nesrallah, A. J. & Srougi, M. Experience with the orthotopic ileal neobladder in women: a mid-term follow-up. BJU Int. 95, 1045–1047 (2005).
Ali-el-Dein, B. et al. Surgical complications following radical cystectomy and orthotopic neobladders in women. J. Urol. 180, 206–210 (2008).
Stenzl, A. et al. Urethra-sparing cystectomy and orthotopic urinary diversion in women with malignant pelvic tumors. Cancer 92, 1864–1871 (2001).
Author information
Authors and Affiliations
Contributions
R. E. Hautmann, S. H. Hautmann and O. Hautmann contributed equally to the researching of data, discussion of content and reviewing of this manuscript before submission. R. E. Hautmann wrote the article.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Hautmann, R., Hautmann, S. & Hautmann, O. Complications associated with urinary diversion. Nat Rev Urol 8, 667–677 (2011). https://doi.org/10.1038/nrurol.2011.147
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrurol.2011.147
This article is cited by
-
A modified ureteroileal anastomosis can reduce ureteroileal anastomotic stricture after ileal conduit
International Urology and Nephrology (2024)
-
Managing Pelvic Organ Prolapse After Urinary Diversion or Neobladder
Current Bladder Dysfunction Reports (2023)
-
Continent cutaneous urinary diversion with an ileal pouch with the Mitrofanoff principle versus a Miami pouch in patients undergoing cystectomy for bladder cancer: results of a comparative study
World Journal of Urology (2022)
-
A “mysterious ghost kidney stone” in an 8-year-old boy with a solitary right kidney, obstructive megaureter, and ureterostomy: Answers
Pediatric Nephrology (2021)