Abstract
Background:
Children born prematurely may be at risk of developing osteopenia. This study investigated whether insulin-like growth factors (IGFs) in the early postnatal period influence bone mass and body composition in prematurely born children.
Methods:
A total of 74 control (gestational age >36 wk; n = 37) and preterm (gestational age <32 wk; n = 37) infants were investigated (mean age ± SD: 4.59 ± 0.31 y). Bone mineral density, body composition, and markers of bone and mineral metabolism were investigated in relation to postnatal IGF levels.
Results:
After adjusting for confounders, we found no differences in bone mass, but significantly less lean mass, increased fat mass, and increased osteocalcin levels in ex-preterm infants. Forward stepwise multiple analysis revealed that higher late postnatal IGF-II levels predict lumbar spine bone mineral content (P < 0.05) and lean mass (P < 0.05). When the birth weight standard deviation score was included in the analysis, higher early postnatal IGF-I levels predicted both lumbar spine bone mineral density and bone mineral content (P < 0.05). Higher early postnatal IGF binding protein-3 (P < 0.01) predicted increased fat mass at 4-y follow-up.
Conclusion:
Ex-preterm children have normal bone mass but different body composition compared with full-term controls. Higher early IGF-I and late postnatal IGF-II concentrations are positive predictors of lumbar spine bone mass.
Similar content being viewed by others
Main
Children’s bone health is an important issue with lifelong importance. Many factors and medical conditions are associated with an increased risk of a bone mineral disorder and future skeletal problems, including genetics, mechanical loading, activity level, longitudinal growth, puberty, hormones, cytokines, and nutritional status. Peak bone mass is achieved during early adulthood and serves as the “bone bank” for the remainder of life. Bone remodeling, the continuous process of bone formation and resorption, can be assessed and monitored by biochemical markers of bone turnover (1). Many studies have found that ex-preterm infants are shorter, lighter, and have lower bone mass (2,3,4,5) than their full-term peers, and ex-preterm infants who are small for gestational age at birth seem to have the most risk (6). However, several studies have found that the bone mass in ex-preterm infants is appropriate for their body size (7,8) and one study proposed that bone mineral density (BMD) in very-low-birth-weight infants is normalized at 2 y of age (9). During adolescence, children who were born prematurely do not have different bone mineral content (BMC ) (10) or BMD (11) (adjusted for height and weight) in comparison with normal-weight children born at full term. Supplementation with early diet benefits short-time growth and BMD. Positive outcomes of an early special diet have been shown on body composition and fat mass during the first 2 y of life, but the long-term effects on BMD and other morbidities are not yet known (12).
In full-term newborn infants, umbilical cord serum insulin-like growth factor (IGF)-I and IGF binding protein (IGFBP)-3 concentrations positively correlate with the gestational age (GA) (13,14), birth weight (BW) (13,14,15), and fat mass (16). IGF-I levels increase after a normal birth, primarily as a result of the onset of growth hormone–stimulated IGF-I production by the liver after ~6 mo of age (17). IGF-I has growth-promoting effects on almost every tissue, especially skeletal muscle, cartilage, and bone. Circulating IGF-I has also been suggested to regulate adipose tissue growth and the differentiation of preadipocytes into adipocytes (18). The influence or effect of IGF-II has been more difficult to establish, though IGF-II mutations seem to affect lean mass and fat mass distribution in pigs (19).
Circulating IGF-I and IGFBP-3 reflect the short-term growth velocity in very-low-birth-weight infants (20,21). In healthy pregnancies, cord serum IGF-I levels are related more to the size of the skeleton than to the degree of mineralization (17).
We hypothesized that children born prematurely have lower BMD, BMC, and unchanged body composition at 4 y of age compared with normal-weight full-term controls. This study was designed primarily to investigate whether children born prematurely have reduced bone mass compared with healthy full-term children at 4 y of age and whether BMD or BMC in former preterm children correlates with early postnatal IGF-I or IGF-II levels or whether these two factors are affected by differing body composition in children born prematurely compared with that in full-term children. Furthermore, we investigated whether low early postnatal IGF-I or IGF-II levels are associated with lower BMD and BMC levels and a difference in body composition during follow-up at 4 y of age. We also investigated different bone markers and their associations with current IGF-I concentrations and bone mass.
Results
Bone Mass
The bone mass data are provided in Table 1 . No differences were found in total body BMD, total body less head BMD, lumbar spine BMD, total body BMC, or total body less head BMC between the preterm and the control groups when adjusted for age, gender, current height, and current weight. A tendency for higher lumbar spine BMC was found in the preterm group ( Table 1 ).
Body Composition
The body composition data are provided in Table 1 . Lean mass and lean mass less head were lower (P < 0.01 and P < 0.05, respectively) and fat mass less head (P < 0.01) was higher in the preterm group when adjusted for age, gender, height, and weight ( Figure 1 ).
Lean mass less head and fat mass less head in ex-preterm children compared with full-term controls. DXA measurements for (a) lean mass less head and (b) fat mass less head in the preterm and control groups adjusted for corrected age, gender, height, and weight. The bars represent the 95% confidence intervals. *P < 0.05, **P < 0.01 compared with controls. DXA, dual-energy X-ray absorptiometry.
IGF-I, IGF-II, and IGFBP-3
Mean postnatal IGF-I, IGF-II, and IGFBP-3 levels during early and late postnatal weeks and mean current IGF-I and IGFBP-3 values in the preterm group are provided in Table 2 . Current IGF-I or IGFBP-3 levels did not correlate with total BMD (P = 0.80 and P = 0.37, respectively), total BMC (P = 0.46 and P = 0.20, respectively), BMD less head (P = 0.74 and P = 0.79, respectively), BMC less head (P = 0.75 and P = 0.83, respectively), or BMD L1–L4 (P = 0.56 and P = 0.26, respectively) but showed a tendency to correlate with BMC L1–L4 (P = 0.10 and P = 0.09, respectively). Current IGF-I and IGFBP-3 levels correlated with fat mass (r = 0.64; P = 0.001 and r = 0.56; P < 0.01, respectively), and IGF-I levels alone correlated with fat mass less head (r = 0.39; P < 0.05) but current IGF-I and IGF-BP3 did not correlate with lean mass (P = 0.41 and P = 0.31, respectively) or lean mass less head (P = 0.69 and P = 0.66, respectively). Current IGF-I levels did not correlate with BW standard deviation score (BWSDS; r = −0.14; P = 0.42).
Multiple Regression Analysis
The results of the forward stepwise multiple regression analysis are provided in Table 3 . Lean body mass (P < 0.001) and gestational age (P < 0.01) had an adjusted r2 of 57% for total body BMC in all subjects. For total body less head BMC, fat mass less head was also included as a significant predictor (P < 0.05) with lean mass less head (P < 0.0001) and gestational age (P < 0.001; adjusted r2: 43%; P = 0.0001). Higher late postnatal IGF-II level was found to be a positive predictor of BMC L1–L4 (P < 0.05; Table 3 ) and lean mass less head (P < 0.05; Table 3 ) in the preterm group with weight standard deviation score (WSDS) included in the analysis. In Figure 2 , the correlation between BMC L1–L4 and WSDS at follow-up in relation to mean late postnatal serum IGF-II levels is shown.
The correlation between lumbar spine BMC L1–L4 and WSDS at follow-up in children born preterm with high or low IGF-II levels at postmenstrual age of 34.7–37.3 wk. The regression line of children with late postnatal IGF-II >365 µg/l (filled circle) (y = 15.12 + 1.20x; r = 0.66; P = 0.014) (dashed line, ---) was significantly above the regression of those with IGF-II below 365 µg/l (unfilled circle (y = 13.34 + 1.15x; r = 0.58; P = 0.005)) (spaced dashed line, - - -) (P < 0.01). BMC, bone mineral content; IGF, insulin-like growth factor; WSDS, weight standard deviation score.
With BWSDS (P = 0.23) and WSDS (P < 0.05) included in the analysis, higher early postnatal IGF-I showed a positive contribution to BMD L1–L4 (P < 0.05, adjusted r2 = 0.24) and BMC L1–L4 (P < 0.05) in the preterm group ( Table 3 ). BWSDS did not add any further information on total body BMD, total body BMC, total body less head BMD, or total body less head BMC in the forward stepwise multiple regression analysis with WSDS (data not shown).
WSDS (P < 0.0001) and increased early postnatal IGFBP-3 levels (P < 0.01) were strong positive predictors of fat mass less head in the preterm group ( Table 3 ). If WSDS was replaced by current IGF-I levels, early postnatal IGFBP-3 (P < 0.001) and current IGF-I (P = 0.01) levels had an adjusted r2 of 45% for fat mass less head at 4 y of age (r2 = 0.49; P < 0.001) in the preterm group (n = 28).
Biochemical Markers of Bone and Mineral Metabolism
The median (range) serum levels of the different biochemical markers of bone and mineral metabolism are presented in Table 4 and compared with the reported pediatric age- and gender-specific reference intervals. For osteocalcin, significantly more values were above the reference range than within and below it (P < 0.001, Pearson’s χ2 test); otherwise the marker levels did not differ significantly compared with the reference material ( Table 4 ).
Subjects with elevated osteocalcin had significantly higher serum carboxy-terminal cross-linking telopeptide of type I collagen (CTX; P < 0.001, nonparametric Mann–Whitney test) and higher total body less head BMC (P < 0.05). We found no differences in WSDS, current IGF-I (P = 0.64), early IGF-I (P = 0.57), IGFBP-3 (P = 0.27), or late postnatal IGF-II (P = 0.31) levels compared with those in subjects within the reference interval for osteocalcin. In the group with elevated osteocalcin (i.e., above the reference value), a correlation with current IGF-I levels was present among females (P < 0.01), but a correlation was not found in the whole group of ex-preterm infants (r = 0.25; P = 0.20).
Lumbar spine BMC L1–L4 correlated significantly with total alkaline phosphatase (ALP; P < 0.05). ALP also significantly correlated with lumbar spine BMD L1–L4 (r = 0.43; P < 0.05). CTX correlated with total body less head BMC (r = 0.51; P = 0.01). CTX also correlated negatively with BWSDS in the preterm group (r = −0.49; P < 0.01). No correlations were observed for osteoprotegerin and Type I procollagen intact amino-terminal propeptide (PINP) with dual-energy X-ray absorptiometry bone mass measurements.
Current IGF-I levels positively correlated with CTX (r = 0.43; P = 0.01), tartrate-resistant acid phosphatase isoform 5b (TRACP5b; r = 0.47; P < 0.01), and ALP (r = 0.57; P < 0.001; Figure 3 ).
Current IGF-I levels in relation to some biochemical markers of bone and mineral metabolism. Current log-IGF-I levels correlated positively with ALP (r = 0.57, P<0.001; black unfilled triangles), log TRACP5b (r = 0.47, P=0.008; black filled triangles), and CTX (r = 0.43, P=0.014; black unfilled squares). ALP, alkaline phosphatase; CTX, carboxy-terminal cross-linking telopeptide of type I collagen; IGF, insulin-like growth factor; TRACP5b, tartrate-resistant acid phosphatase isoform 5b.
Discussion
In this group of 4-y-old prematurely born children, our main findings were lower lean mass and higher fat mass compared with those in an age- and height-matched control group, after correction for possible confounders. Osteocalcin levels were higher in the ex-preterm subjects, with more values above the median range compared with the reference material. Our preterm infants seemed to have normal BMD and BMC compared with the age- and height-matched control group at 4 y of age, which contradicted our initial hypothesis. Ex-preterm infants and adults have lower bone mass (2,3,4,5) than full-term controls, although other studies have found that the bone mass in ex-preterm infants either is appropriate for their body size or does not differ from normal-weight full-term infants (7,8,11). These findings might reflect different treatment strategies in modern neonatal intensive care units. In the current study, we found a tendency for higher lumbar spine BMC in the preterm group. Higher late postnatal IGF-II levels were found to correlate positively with lumbar spine BMC and lean mass in preterm infants at 4 y of age. Higher early postnatal IGF-I levels were predictive of both higher lumbar spine BMD and lumbar spine BMC when BWSDS was included in the analysis. A lower BWSDS positively correlated with lumbar spine BMD and BMC. Current IGF-I and early postnatal IGFBP-3 levels were both correlated with fat mass less head.
We only found a tendency for current IGF-I and IGFBP-3 levels to correlate with lumbar spine BMC; otherwise we found no correlation between current IGF-I and IGFBP-3 levels with BMD or BMC. However, current IGF-I levels (at 4 y of age) positively correlated with several markers of bone turnover, specifically CTX, ALP, and TRACP5b.
The preterm group had a relatively lower lean body mass and increased fat mass compared with the control group after correcting for possible confounders. Increased total and abdominal adipose tissue has also been reported in adult ex-preterm subjects compared with the same in controls (22). In pigs, with IGF-II mutations that induce increased IGF-II levels, more lean body mass is generated; thus, IGF-II seems to influence lean body mass (19). Hernandez et al. (23) performed a similar study in which body composition was determined at 2 y of age in material from preterm infants (n = 26), and IGF-I, IGF-II, and leptin were followed longitudinally from birth. An influence of IGF-II on lean body mass was also found. In their study, leptin levels at 1 mo of age correlated with fat mass at 2 y of life (23). Higher leptin levels reflect more fat mass present at that period in neonatal life. Early postnatal IGFBP-3 levels were shown to be strongly predictive of later fat mass in the preterm group in our study. In our preterm group, increased IGFBP-3 levels corresponding to the mean level of IGFBP-3 at a postmenstrual age of 30–32.5 wk was the strongest predictor of fat mass at 4 y, not IGFBP-3 in late postnatal weeks (data not shown). Because IGFBP-3 circulates in the blood bound in a complex with either IGF-I or IGF-II, high IGFBP-3 most probably correlates with higher levels of one or both of these growth factors.
The increase in osteocalcin can be explained by the relatively increased fat mass in the preterm group. Osteocalcin is produced by osteoblasts and reflects bone formation, but recent studies have demonstrated an association between osteocalcin and metabolic syndrome (24), as well as indications of osteocalcin production and release by the adipose tissue (25). In a group of adult men, osteocalcin was found to be inversely related to fat mass and plasma glucose (26). In our ex-preterm infants with osteocalcin levels above the reference range, a correlation between osteocalcin and current IGF-I levels was present in females, which might indicate that preterm girls with elevated osteocalcin are more sensitive to the effects of IGF-I than are preterm boys. When comparing different osteocalcin studies and methods, the measured osteocalcin value can differ 10-fold depending on the applied method. The differences between assays are mostly due to different polyclonal and monoclonal antibodies recognizing different epitopes of circulating immunoreactive fragments of osteocalcin (27). We used the same assay as that reported by Tarallo et al. (28), who investigated biological variations and reference limits in 1,096 healthy individuals from 4 to 65 y of age.
Higher late postnatal IGF-II level was a significant positive predictor of lumbar spine BMC, and when BWSDS was included in the analysis, higher early postnatal IGF-I levels were predictive of both lumbar spine BMD and lumbar spine BMC. In experimental studies, IGF-I and IGF-II levels were shown to induce osteoclastogenesis and to affect osteoclast differentiation and bone resorption (29,30). Knockout mice with a loss of function in one of the promoter regions for the IGF-II gene have certain skeletal abnormalities associated with reduced mineralization and altered bone remodeling (31). The differentiation of osteoprogenitors into osteoblasts is impaired in these mice, and IGF-II has been suggested to be a regulator of the fate of mesenchymal progenitors during bone development (31). One may speculate that the higher IGF-II levels in late postnatal weeks associated with higher lumbar spine BMC in the preterm subjects may relate to early developmental programming of osteoclast/osteoblast formation by IGF-II. Another explanation for this positive association may be that the promotion of late postnatal cell proliferation by IGF-II is important for later lumbar spine BMD/BMC outcome. As osteoblasts and adipocytes are derived from the same progenitor cells, one may speculate that IGF-II or an interaction between IGF-I and IGF-II during certain time periods in fetal development could be important in directing the differentiation process of these progenitors to either adipocytes or osteoblasts. This interaction might be disturbed during early postnatal weeks in preterm infants, leading to differences in body composition at older ages.
The current study has limitations, including a small cohort size and comparison of laboratory measurements with general reference values instead of a control group. However, the findings indicate that with today’s nutrition routines, former preterm infants can exhibit normal bone mass formation but can still have a different distribution of fat mass and lean mass than their full-term peers.
The association between neonatal laboratory findings, such as IGFBP-3 levels, and later body composition outcomes could be important for designing trials to improve future nutrition in preterm children. Studying these children at an older age, such as early adulthood, would be of interest in order to analyze the influence of puberty, study possible sex differences, and determine whether our findings are fixed or dynamic processes.
In summary, our preterm infants had normal BMC and BMD compared with age- and height-matched controls at 4 y of age. A difference in body composition was found between the groups, with an altered lean mass/fat mass ratio in the preterm group, which indicates that premature birth may have effects on body composition that persist throughout childhood. Differences in early postnatal levels of IGF may influence the outcome.
Methods
Subjects
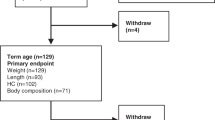
Patients were recruited from the year 2000 to the year 2002 from western Sweden at the Queen Silvia Children’s Hospital after informed consent was obtained from the children and their parents. The local research ethics committee of Göteborg University, Sweden, approved this study (no. 370-04). The study group comprised 71 preterm infants at baseline. Data regarding the initial IGF-I levels at birth are reported elsewhere (32). The current follow-up study was conducted after the initial study, and all patients were contacted for this follow-up study.
Only 39 prematurely born children and their parents were willing to participate in this follow-up assessment at 4 y of age, which was conducted in the period 2005–2008. Children from the initial study group who participated in the follow-up study did not differ from those who did not participate in regard to gestational age at birth (P = 0.59, analysis of variance t-test), BW (P = 0.34), and BWSDS (P = 0.73). Two children were excluded due to failure to undergo the bone mass scan, which resulted in a total of 37 children: 21 boys and 16 girls. The median (range) postmenstrual age at birth (based on ultrasonography performed at weeks 16–18) was 27.7 (24.4–31.1) weeks. All infants were hospitalized in the neonatal intensive care unit and nourished according to standardized routines. Enteral feeding was introduced early, with increasing amounts of breast milk (i.e., 2–48 h after birth). Supplementary parenteral nutrition with glucose, amino acids, and fat was used until full enteral feeding was possible. Breast milk was analyzed for protein content and fortified with Enfamil human milk fortifier (Mead Johnson, Glenview, IL) to obtain 3.5 g protein/kg/d. The initial IGF-I, IGF-II, and IGFBP-3 values were calculated as the mean during the postmenstrual age of 30–32.5 (early) and 34.7–37.3 (late) weeks. At the 4-y follow-up examination, IGF-I and IGFBP-3 were presented as a single value.
The control group comprised 45 healthy 4-y-old Swedish children from relatives or friends of the preterm children’s families or those randomly selected from pediatric health care units. These children were screened for any known disease and were not born prematurely. Eight children were excluded from the initial control group to obtain a better correlation with the age and height of the preterm group. The control children were examined in 2005–2008. Blood sampling was not performed in the control children and they were not analyzed for IGF-I levels for ethical reasons. Height was measured to the nearest 0.1 cm using a wall-mounted stadiometer. Weight was measured to the nearest 0.1 kg on an analogue scale.
Baseline and follow-up characteristics are presented in Table 5 . No significant differences were found between control and preterm children regarding gender, corrected age, height, height SDS, weight, weight SDS, BMI, or BMI SDS ( Table 5 ). Eight preterm infants and four control children were born small for gestational age (defined as less than −2 BWSDS).
Assessment of Bone Mass
The BMD and the BMC for the total body and lumbar spine (L1–L4) were assessed by dual-energy X-ray absorptiometry using the Lunar Prodigy (GE Lunar Corp., Madison, WI). Lean mass and fat mass were also measured. Only measurements of good quality were included in the analysis, and scans with movement artifacts were excluded ( Table 1 ).
Biochemical Determinations
A detailed description of the biochemical methods are reported elsewhere (33). All biochemical analyses were performed using serum samples. Briefly, osteocalcin was determined by radioimmunoassay using OSTK-PR (CIS Bio International, Gif-sur-Yvette, Cedex, France). Type I procollagen intact amino-terminal propeptide was also determined by radioimmunoassay (Orion Diagnostica, Oulunsalo, Finland). ALP was measured by a kinetic assay with 1.0 mol/l diethanolamine buffer (pH 9.8), 1.0 mmol/l MgCl2, and 10 mmol/l p-nitrophenylphosphate. Type I collagen degradation was assessed by measuring CTX using the CrossLaps enzyme-linked immunosorbent assay (Nordic Bioscience Diagnostics A/S, Herlev, Denmark), which is reported to measure a cathepsin K degradation product of trivalently cross-linked type I collagen. Osteoclast-derived TRACP5b was measured using a solid-phase immunofixed enzyme activity assay (SBA Sciences, Oulu, Finland). Pediatric age- and gender-specific reference intervals were reported elsewhere for osteoprotegerin, ALP, osteocalcin, type I procollagen intact amino-terminal propeptide, CTX, and TRACP5b (33).
The IGF-I, IGF-II, and IGFBP-3 assays are described in detail elsewhere (34). Briefly, serum samples were diluted 1:50 and IGF-I was measured in duplicate using IGFBP-blocked radioimmunoassay without extraction in the presence of an ~250-fold excess of IGF-II (Mediagnost GmbH, Tubingen, Germany). The IGFBP-3 samples were diluted 1:300. For IGF-I, the intraassay coefficient of variance was 15.7% at 10.2 µg/l and 9.6% at 34.5 µg/l. The interassay coefficient of variance was 23.9% at 10.2 µg/l and 12.1% at 34.5 µg/l. The intraassay coefficient of variance for IGFBP-3 was 10, 7, and 6% at 716, 1,750, and 3,929 μg/l, respectively (34).
Statistical Analysis
Anthropometric data are presented as median (range) and dual-energy X-ray absorptiometry measurements as mean (±SD). Normal distribution was achieved by log-transformation of early postnatal IGF-I, IGFBP-3, and IGF-II concentrations, as well as current IGF-I, IGFBP-3, and TRACP5b concentrations. Comparisons between two separate groups regarding anthropometric data were performed with the nonparametric Mann–Whitney U-test ( Table 5 ). Pearson’s χ2 test was used to compare numerical values ( Table 5 ) and the frequency of preterm infants with osteocalcin levels above that of a reference control material ( Table 4 ). To determine differences between preterm and full-term children with regard to bone mass and body composition, multiple regression analysis was corrected for current age, gender, height, and weight, and P values were also determined after correction for only age and gender ( Table 1 ). Forward stepwise multiple regression analysis was performed with total body BMC, total body less head BMD, total body less head BMC, spine BMD L1–L4, BMC L1–L4, lean mass less head, and adipose tissue mass less head as dependent variables ( Table 3 ). The difference between regression lines was calculated in a special model of multiple regression analysis with WSDS and spine BMC L1–L4 ( Figure 2 ). The level of significance was set to P < 0.05. P values between 0.10 and 0.05 were considered tendency. All statistical analyses were performed using Statistical Stat Soft, version 10 (Tulsa, OK).
Statement of Financial Support
This study was supported by grants from the Swedish Society of Medicine, the Göteborg Medical Society, the Capio Research Foundation, the County Council of Östergötland, and the Swedish Research Council K2006-75X-21144-01-3.
Disclosure
There is no conflict of interest to disclose.
References
Demers LM . Clinical usefulness of markers of bone degradation and formation. Scand J Clin Lab Invest Suppl 1997;227:12–20.
Farooqi A, Hagglof B, Sedin G, Gothefors L, Serenius F . Growth in 10- to 12-year-old children born at 23 to 25 weeks’ gestation in the 1990s: a Swedish national prospective follow-up study. Pediatrics 2006;118:1452–65.
Wood NS, Costeloe K, Gibson AT, Hennessy EM, Marlow N, Wilkinson AR ; EPICure Study Group. The EPICure study: growth and associated problems in children born at 25 weeks of gestational age or less. Arch Dis Child Fetal Neonatal Ed 2003;88:F492–500.
Chan GM, Armstrong C, Moyer-Mileur L, Hoff C . Growth and bone mineralization in children born prematurely. J Perinatol 2008;28:619–23.
Zamora SA, Belli DC, Rizzoli R, Slosman DO, Bonjour JP . Lower femoral neck bone mineral density in prepubertal former preterm girls. Bone 2001;29:424–7.
van de Lagemaat M, Rotteveel J, van Weissenbruch MM, Lafeber HN . Small-for-gestational-age preterm-born infants already have lower bone mass during early infancy. Bone 2012;51:441–446.
Weiler HA, Yuen CK, Seshia MM . Growth and bone mineralization of young adults weighing less than 1500 g at birth. Early Hum Dev 2002;67:101–12.
Fewtrell MS, Prentice A, Jones SC, et al. Bone mineralization and turnover in preterm infants at 8-12 years of age: the effect of early diet. J Bone Miner Res 1999;14:810–20.
Ichiba H, Shintaku H, Fujimaru M, Hirai C, Okano Y, Funato M . Bone mineral density of the lumbar spine in very-low-birth-weight infants: a longitudinal study. Eur J Pediatr 2000;159:215–8.
Erlandson MC, Sherar LB, Baxter-Jones AD, et al. Preterm birth and adolescent bone mineral content. Am J Perinatol 2011;28:157–63.
Breukhoven PE, Leunissen RW, de Kort SW, Willemsen RH, Hokken-Koelega AC . Preterm birth does not affect bone mineral density in young adults. Eur J Endocrinol 2011;164:133–8.
Pittaluga E, Vernal P, Llanos A, et al.; Neonatology Collaborative Group. Benefits of supplemented preterm formulas on insulin sensitivity and body composition after discharge from the neonatal intensive care unit. J Pediatr 2011;159:926–32.e2.
Bennett A, Wilson DM, Liu F, Nagashima R, Rosenfeld RG, Hintz RL . Levels of insulin-like growth factors I and II in human cord blood. J Clin Endocrinol Metab 1983;57:609–12.
Gluckman PD, Johnson-Barrett JJ, Butler JH, Edgar BW, Gunn TR . Studies of insulin-like growth factor -I and -II by specific radioligand assays in umbilical cord blood. Clin Endocrinol (Oxf) 1983;19:405–13.
Lassarre C, Hardouin S, Daffos F, Forestier F, Frankenne F, Binoux M . Serum insulin-like growth factors and insulin-like growth factor binding proteins in the human fetus. Relationships with growth in normal subjects and in subjects with intrauterine growth retardation. Pediatr Res 1991;29:219–25.
Akcakus M, Koklu E, Kurtoglu S, Kula M, Koklu SS . The relationship among intrauterine growth, insulinlike growth factor I (IGF-I), IGF-binding protein-3, and bone mineral status in newborn infants. Am J Perinatol 2006;23:473–80.
Gluckman PD . Clinical review 68: The endocrine regulation of fetal growth in late gestation: the role of insulin-like growth factors. J Clin Endocrinol Metab 1995;80:1047–50.
Blüher S, Kratzsch J, Kiess W . Insulin-like growth factor I, growth hormone and insulin in white adipose tissue. Best Pract Res Clin Endocrinol Metab 2005;19:577–87.
Gardan D, Gondret F, Van den Maagdenberg K, Buys N, De Smet S, Louveau I . Lipid metabolism and cellular features of skeletal muscle and subcutaneous adipose tissue in pigs differing in IGF-II genotype. Domest Anim Endocrinol 2008;34:45–53.
Kajantie E, Dunkel L, Rutanen EM, et al. IGF-I, IGF binding protein (IGFBP)-3, phosphoisoforms of IGFBP-1, and postnatal growth in very low birth weight infants. J Clin Endocrinol Metab 2002;87:2171–9.
Hansen-Pupp I, Löfqvist C, Polberger S, et al. Influence of insulin-like growth factor I and nutrition during phases of postnatal growth in very preterm infants. Pediatr Res 2011;69(5 Pt 1):448–53.
Thomas EL, Parkinson JR, Hyde MJ, et al. Aberrant adiposity and ectopic lipid deposition characterize the adult phenotype of the preterm infant. Pediatr Res 2011;70:507–12.
Hernandez MI, Rossel K, Peña V, et al. Leptin and IGF-I/II during the first weeks of life determine body composition at 2 years in infants born with very low birth weight. J Pediatr Endocrinol Metab 2012;25:951–5.
Lee NK, Sowa H, Hinoi E, et al. Endocrine regulation of energy metabolism by the skeleton. Cell 2007;130:456–69.
Foresta C, Strapazzon G, De Toni L, et al. Evidence for osteocalcin production by adipose tissue and its role in human metabolism. J Clin Endocrinol Metab 2010;95:3502–6.
Kindblom JM, Ohlsson C, Ljunggren O, et al. Plasma osteocalcin is inversely related to fat mass and plasma glucose in elderly Swedish men. J Bone Miner Res 2009;24:785–91.
Masters PW, Jones RG, Purves DA, Cooper EH, Cooney JM . Commercial assays for serum osteocalcin give clinically discordant results. Clin Chem 1994;40:358–63.
Tarallo P, Henny J, Fournier B, Siest G . Plasma osteocalcin: biological variations and reference limits. Scand J Clin Lab Invest 1990;50:649–55.
Bosetti M, Sabbatini M, Nicolì E, Fusaro L, Cannas M . Effects and differentiation activity of IGF-I, IGF-II, insulin and preptin on human primary bone cells. Growth Factors 2013;31:57–65.
Hemingway F, Taylor R, Knowles HJ, Athanasou NA . RANKL-independent human osteoclast formation with APRIL, BAFF, NGF, IGF I and IGF II. Bone 2011;48:938–44.
Hardouin SN, Guo R, Romeo PH, Nagy A, Aubin JE . Impaired mesenchymal stem cell differentiation and osteoclastogenesis in mice deficient for Igf2-P2 transcripts. Development 2011;138:203–13.
Hellström A, Engström E, Hård AL, et al. Postnatal serum insulin-like growth factor I deficiency is associated with retinopathy of prematurity and other complications of premature birth. Pediatrics 2003;112:1016–20.
Swolin-Eide D, Hansson S, Larsson L, Magnusson P . The novel bone alkaline phosphatase B1x isoform in children with kidney disease. Pediatr Nephrol 2006;21:1723–9.
Blum WF, Breier BH . Radioimmunoassays for IGFs and IGFBPs. Growth Regul 1994;4 Suppl 1:11–9.
Acknowledgements
We thank all of the patients and parents for participating in this study. We are grateful to Anne Dohse and Cecilia Halling Linder for excellent technical assistance. We want to express our gratitude for the excellent statistical advice given by Mattias Molin and Anders Pehrsson. We also want to express our gratitude to Agneta Hilding, Karolinska Institute, for fruitful discussions.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Stigson, L., Kistner, A., Sigurdsson, J. et al. Bone and fat mass in relation to postnatal levels of insulin-like growth factors in prematurely born children at 4 y of age. Pediatr Res 75, 544–550 (2014). https://doi.org/10.1038/pr.2014.4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pr.2014.4
This article is cited by
-
Body composition in preterm infants: a systematic review on measurement methods
Pediatric Research (2023)
-
Increased risk of rickets but not fractures during childhood and adolescence following necrotizing enterocolitis among children born preterm in Sweden
Pediatric Research (2019)
-
Diminished growth and lower adiposity in hyperglycemic very low birth weight neonates at 4 months corrected age
Journal of Perinatology (2016)
-
Preterm Children Born Small for Gestational Age are at Risk for Low Adult Bone Mass
Calcified Tissue International (2016)
-
Dietary proteins and IGF I levels in preterm infants: determinants of growth, body composition, and neurodevelopment
Pediatric Research (2015)