Abstract
Objective
To investigate if a hemodynamically significant patent ductus arteriosus (hsPDA) leads to elevated high-sensitivity troponin T (hsTnT) and NTproBNP levels in serum.
Study design
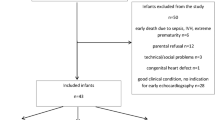
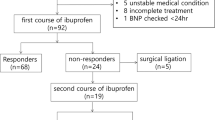
Infants <34 weeks and <1500 g were prospectively enrolled, except those with major congenital or chromosomal anomalies. An echocardiogram (ECHO) was performed and hsTnT and NTproBNP were measured within 5 days of life and repeated after treatment of hsPDA. Clinical, ECHO, and hsTnT data were analyzed using Student t-test, two proportion z-test, and regression analysis.
Results
Seventy infants were enrolled. Infants in the hsPDA group had lower gestation and birth weight. Mean hsTnT and NTproBNP levels in the hsPDA group were higher compared to the group without an hsPDA, with levels being 251.54 vs 161.6 pg/ml, p < 0.01 for hsTnT and 18181.02 vs 3149.23 pg/ml, p < 0.001 for NTproBNP.
Conclusion
HsPDA leads to increased hsTnT and NTproBNP levels in preterm infants without affecting cardiac function.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Hamrick SE, Hansmann G. Patent ductus arteriosus of the preterm infant. Pediatrics. 2010;125:1020–30.
Clyman RI. Mechanisms regulating the ductus arteriosus. Biol Neonate. 2006;89:330–5.
Wyllie J. Treatment of patent ductus arteriosus. Semin Neonatol. 2003;8:425–32.
Baylen BG, Ogata H, Oguchi K, Ikegami M, Jacobs H, Jobe A, et al. The contractility and performance of the preterm left ventricle before and after early patent ductus arteriosus occlusion in surfactant-treated lambs. Pediatr Res. 1985;19:1053–8.
Way GL, Pierce JR, Wolfe RR, McGrath R, Wiggins J, Merenstein GB. ST depression suggesting subendocardial ischemia in neonates with respiratory distress syndrome and patent ductus arteriosus. J Pediatr. 1979;95:609–11.
McNamara PJ, Sehgal A. Towards rational management of the patent ductus arteriosus: the need for disease staging. Arch Dis Child Fetal Neonatal Ed. 2007;92:F424–7.
Skeik N, Patel DC. A review of troponins in ischemic heart disease and other conditions. Int J Angiol. 2007;16:53–8.
Sharma S, Jackson PG, Makan J. Cardiac troponins. J Clin Pathol. 2004;57:1025–6.
Antman E, Bassand J-P, Klein W, Ohman M, Lopez Sendon JL, Rydén L, et al. Myocardial infarction redefined—a consensus document of The Joint European Society of Cardiology/American College of Cardiology committee for the redefinition of myocardial infarction. J Am Coll Cardiol. 2000;36:959–69.
Makikallio K, Vuolteenaho O, Jouppila P, Rasanen J. Association of severe placental insufficiency and systemic venous pressure rise in the fetus with increased neonatal cardiac troponin T levels. Am J Obstet Gynecol. 2000;183:726–31.
Szymankiewicz M, Matuszczak-Wleklak M, Hodgman JE, Gadzinowski J. Usefulness of cardiac troponin T and echocardiography in the diagnosis of hypoxic myocardial injury of full-term neonates. Biol Neonate. 2005;88:19–23.
Trevisanuto D, Zaninotto M, Altinier S, Plebani M, Zanardo V. High serum cardiac troponin T concentrations in preterm infants with respiratory distress syndrome. Acta Paediatr. 2000;89:1134–6.
Sherwood MW, Kristin Newby L. High-sensitivity troponin assays: evidence, indications, and reasonable use. J Am Heart Assoc. 2014;3:e000403.
Chenevier-Gobeaux C, Bonnefoy-Cudraz E, Charpentier S, Dehoux M, Lefevre G, Meune C, et al. High-sensitivity cardiac troponin assays: answers to frequently asked questions. Arch Cardiovasc Dis. 2015;108:132–49.
Xu RY, Zhu XF, Yang Y, Ye P. High-sensitive cardiac troponin T. J Geriatr Cardiol. 2013;10:102–9.
El-Khuffash AF, Molloy EJ. Influence of a patent ductus arteriosus on cardiac troponin T levels in preterm infants. J Pediatr. 2008;153:350–3.
Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr. 1978;92:529–34.
Shennan AT, Dunn MS, Ohlsson A, Lennox K, Hoskins EM. Abnormal pulmonary outcomes in premature infants: prediction from oxygen requirement in the neonatal period. Pediatrics. 1988;82:527–32.
Classification of Retinopathy of Prematurity revisited. The international classification of retinopathy of prematurity revisited. Arch Ophthalmol. 2005;123:991–9.
Bell MJ, Ternberg JL, Feigin RD, Keating JP, Marshall R, Barton L, et al. Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg. 1978;187:1–7.
Jain A, Shah PS. Diagnosis, evaluation, and management of patent ductus arteriosus in preterm neonates. JAMA Pediatr. 2015;169:863–72.
Apple FS. A new season for cardiac troponin assays: it’s time to keep a scorecard. Clin Chem. 2009;55:1303–6.
Freund Y, Chenevier-Gobeaux C, Bonnet P, Claessens YE, Allo JC, Doumenc B, et al. High-sensitivity versus conventional troponin in the emergency department for the diagnosis of acute myocardial infarction. Crit Care. 2011;15:R147.
Baum H, Hinze A, Bartels P, Neumeier D. Reference values for cardiac troponins T and I in healthy neonates. Clin Biochem. 2004;37:1079–82.
Clyman RI. The role of patent ductus arteriosus and its treatments in the development of bronchopulmonary dysplasia. Semin Perinatol. 2013;37:102–7.
Adamcova M, Kokstein Z, Palicka V, Vavrova J, Podholova M, Kost’al M. Cardiac troponin T in neonates after acute and long-term tocolysis. Biol Neonate. 2000;78:288–92.
Shelton SD, Fouse BL, Holleman CM, Sedor FA, Herbert WN. Cardiac troponin T levels in umbilical cord blood. Am J Obstet Gynecol. 1999;181(5 Pt 1):1259–62.
Kulkarni M, Gokulakrishnan G, Price J, Fernandes CJ, Leeflang M, Pammi M. Diagnosing significant PDA using natriuretic peptides in preterm neonates: a systematic review. Pediatrics. 2015;135:e510–525.
El-Khuffash AF, Slevin M, McNamara PJ, Molloy EJ. Troponin T, N-terminal pronatriuretic peptide and a patent ductus arteriosus scoring system predict death before discharge or neurodevelopmental outcome at 2 years in preterm infants. Arch Dis Child Fetal Neonatal Ed. 2011;96:F133–137.
Acknowledgements
We would like to acknowledge Catharine White Creech and Lacie Dixon who did the ECHOs of all subjects recruited in the study. The study would not be possible without their help. We would also like to acknowledge all the parents who allowed us to include their infants in the study. We want to acknowledge Roche pharmaceutical (Indianapolis, IN, USA) for their support in the measurement of hsTnT levels.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest. However, we have received support from Roche Diagnostics, Indianapolis, IN, USA, who provided us with the Elecsys 2010 assay for biomarker analysis for this study, but Roche Diagnostics was not involved in the analysis and interpretation of the research data.
Rights and permissions
About this article
Cite this article
Asrani, P., Aly, A.M., Jiwani, A.K. et al. High-sensitivity troponin T in preterm infants with a hemodynamically significant patent ductus arteriosus. J Perinatol 38, 1483–1489 (2018). https://doi.org/10.1038/s41372-018-0192-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-018-0192-x
This article is cited by
-
High-Sensitivity Troponin T Testing for Pediatric Patients in the Emergency Department
Pediatric Cardiology (2022)
-
The effect of patent ductus arteriosus on coronary artery blood flow in premature infants: a prospective observational pilot study
Journal of Perinatology (2020)
-
Cardiac Troponin T in Healthy Full-Term Infants
Pediatric Cardiology (2019)