Abstract
Background
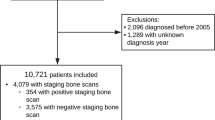
Up to 90% of men with metastatic castration-resistant prostate cancer (mCRPC) will have a distribution of disease that includes bone metastases demonstrated on a Technetium-99m (99mTc-MDP) bone scan. The Prostate Cancer Working Group 2 and 3 Consensus Criteria standardized the criteria for assessing progression based on the development of new lesions. These criteria have been recognized by regulatory authorities for drug approval. The bone scan index (BSI) is a method to quantitatively measure the burden of bony disease, and can assess both disease progression and regression. The automated BSI (aBSI) is a method of computer analysis to assess BSI, and is being qualified as a clinical trials endpoint.
Methods
Manual searching was used to identify the literature on BSI and aBSI. We summarize the most relevant aspects of the retrospective and prospective studies evaluating aBSI measurements, and provide a critical discussion on the potential advantages and caveats of aBSI.
Results
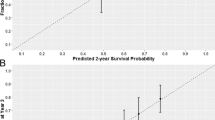
The development of neural artificial networks (EXINI boneBSI) to automatically determine the BSI reduces the turnaround time for assessing BSI with high reproducibility and accuracy. Several studies showed that the concordance between aBSI and BSI, as well as the interobserver concordance of aBSI, was >0.95. In a phase 3 assessment of aBSI, a doubling value increased the risk of death in 20%, pre-treatment aBSI values independently correlated with overall survival (OS) and time to symptomatic progression. Retrospective studies suggest that a decrease in aBSI after treatment may correlate with higher survival when compared with increasing aBSI.
Conclusions
aBSI provides a quantitative measurement that is feasible, reproducible, and in analyses to date correlates with OS and symptomatic progression. These findings support the aBSI to risk-stratify men with mCRPC for clinical trial enrollment. Future studies quantifying aBSI change over time as an intermediate endpoint for evaluating new systemic therapies are needed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Sartor O, de Bono JS. Metastatic prostate cancer. N Engl J Med. 2018;378:645–57.
Kirby M, Hirst C, Crawford ED. Characterising the castration-resistant prostate cancer population: a systematic review. Int J Clin Pract. 2011;65:1180–92.
Scher HI, Halabi S, Tannock I, Morris M, Sternberg CN, Carducci MA, et al. Design and end points of clinical trials for patients with progressive prostate cancer and castrate levels of testosterone: recommendations of the Prostate Cancer Clinical Trials Working Group. J Clin Oncol. 2008;26:1148–59.
Scher HI, Morris MJ, Stadler WM, Higano C, Basch E, Fizazi K, et al. Trial design and objectives for castration-resistant prostate cancer: Updated recommendations from the prostate cancer clinical trials working group 3. J Clin Oncol. 2016;34:1402–18.
Rathkopf DE, Beer TM, Loriot Y, Higano CS, Armstrong AJ, Sternberg CN, et al. Radiographic progression-free survival as a clinically meaningful end point in metastatic castration-resistant prostate cancer: the PREVAIL randomized clinical trial. JAMA Oncol. 2018;4:694–701.
Morris MJ, Molina A, Small EJ, de Bono JS, Logothetis CJ, Fizazi K, et al. Radiographic progression-free survival as a response biomarker in metastatic castration-resistant prostate cancer: COU-AA-302 results. J Clin Oncol. 2015;33:1356–63.
Ulmert D, Kaboteh R, Fox JJ, Savage C, Evans MJ, Lilja H, et al. A novel automated platform for quantifying the extent of skeletal tumour involvement in prostate cancer patients using the bone scan index. Eur Urol. 2012;62:78–84.
Montilla-Soler JL, Makanji R. Skeletal scintigraphy. Cancer Control. 2017;24:137–46.
Tryciecky EW, Gottschalk A, Ludema K. Oncologic imaging: interactions of nuclear medicine with CT and MRI using the bone scan as a model. Semin Nucl Med. 1997;27:142–51.
O’Sullivan GJ, Carty FL, Cronin CG. Imaging of bone metastasis: an update. World J Radiol. 2015;7:202–11.
McKillop JH, Williams ED, Harding LK. Consistency in nuclear medicine reporting--a pilot study using bone scans. Nucl Med Commun. 1990;11:253–7.
Fosbøl MØ, Petersen PM, Kjaer A, Mortensen J. 223Ra therapy of advanced metastatic castration-resistant prostate cancer: quantitative assessment of skeletal tumor burden for prognostication of clinical outcome and hematologic toxicity. J Nucl Med. 2018;59:596–602.
Zacho HD, Manresa JAB, Mortensen JC, Bertelsen H, Petersen LJ. Observer agreement and accuracy in the evaluation of bone scans in newly diagnosed prostate cancer. Nucl Med Commun. 2015;36:445–51.
Sadik M, Suurkula M, Höglund P, Järund A, Edenbrandt L. Quality of planar whole-body bone scan interpretations - a nationwide survey. Eur J Nucl Med Mol Imaging. 2008;35:1464–72.
Bogaerts J, Ford R, Sargent D, Schwartz LH, Rubinstein L, Lacombe D, et al. Individual patient data analysis to assess modifications to the RECIST criteria. Eur J Cancer. 2009;45:248–60.
Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, et al. New response evaluation criteria in solid tumours: Revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45:228–47.
Sonpavde G, Pond GR, Berry WR, de Wit R, Eisenberger MA, Tannock IF, et al. The association between radiographic response and overall survival in men with metastatic castration-resistant prostate cancer receiving chemotherapy. Cancer. 2011;117:3963–71.
Sonpavde G, Pond GR, Plets M, Tangen CM, Hussain MHA, Lara PN, et al. Validation of the association of RECIST changes with survival in men with metastatic castration-resistant prostate cancer treated on SWOG Study S0421. Clin Genitourin Cancer. 2017;15:635–41.
Imbriaco M, Larson SM, Yeung HW, Mawlawi OR, Erdi Y, Venkatraman ES, et al. A new parameter for measuring metastatic bone involvement by prostate cancer: the Bone Scan Index. Am Assoc Cancer Res. 1998;4:1765–72.
Sabbatini P, Larson SM, Kremer A, Zhang ZF, Sun M, Yeung H, et al. Prognostic significance of extent of disease in bone in patients with androgen-independent prostate cancer. J Clin Oncol. 1999;17:948–57.
Meirelles GSP, Schoder H, Ravizzini GC, Gonen M, Fox JJ, Humm J, et al. Prognostic value of baseline [18F] fluorodeoxyglucose positron emission tomography and 99mTc-MDP bone scan in progressing metastatic prostate cancer. Clin Cancer Res. 2010;16:6093–9.
Dennis ER, Jia X, Mezheritskiy IS, Stephenson RD, Schoder H, Fox JJ, et al. Bone scan index: a quantitative treatment response biomarker for castration-resistant metastatic prostate cancer. J Clin Oncol. 2012;30:519–24.
Sadik M, Suurkula M, Hoglund P, Jarund A, Edenbrandt L. Improved classifications of planar whole-body bone scans using a computer-assisted diagnosis system: a multicenter, multiple-reader, multiple-case study. J Nucl Med. 2009;50:368–75.
Sadik M, Jakobsson D, Olofsson F, Ohlsson M, Suurkula M, Edenbrandt L. A new computer-based decision-support system for the interpretation of bone scans. Nucl Med Commun. 2006;27:417–23.
Anand A, Morris MJ, Kaboteh R, Reza M, Tragardh E, Matsunaga N, et al. A preanalytic validation study of automated bone scan index: effect on accuracy and reproducibility due to the procedural variabilities in bone scan image acquisition. J Nucl Med. 2016;57:1865–71.
Shintawati R, Achmad A, Higuchi T, Shimada H, Hirasawa H, Arisaka Y, et al. Evaluation of bone scan index change over time on automated calculation in bone scintigraphy. Ann Nucl Med. 2015;29:911–20.
Anand A, Morris MJ, Kaboteh R, Bath L, Sadik M, Gjertsson P, et al. Analytic validation of the automated bone scan index as an imaging biomarker to standardize quantitative changes in bone scans of patients with metastatic prostate cancer. J Nucl Med. 2016;57:41–5.
Reza M, Kaboteh R, Sadik M, Bjartell A, Wollmer P, Trägårdh E. A prospective study to evaluate the intra-individual reproducibility of bone scans for quantitative assessment in patients with metastatic prostate cancer. BMC Med Imaging. 2018;18:1–8.
Kaboteh R, Damber JE, Gjertsson P, Höglund P, Lomsky M, Ohlsson M, et al. Bone Scan Index: a prognostic imaging biomarker for high-risk prostate cancer patients receiving primary hormonal therapy. EJNMMI Res. 2013;3:1–6.
Reza M, Bjartell A, Ohlsson M, Kaboteh R, Wollmer P, Edenbrandt L, et al. Bone Scan Index as a prognostic imaging biomarker during androgen deprivation therapy. EJNMMI Res. 2014;4:1–9.
Poulsen MH, Rasmussen J, Edenbrandt L, Høilund-Carlsen PF, Gerke O, Johansen A, et al. Bone Scan Index predicts outcome in patients with metastatic hormone-sensitive prostate cancer. BJU Int. 2016;117:748–53.
Kaboteh R, Gjertsson P, Leek H, Lomsky M, Ohlsson M, Sjöstrand K, et al. Progression of bone metastases in patients with prostate cancer -automated detection of new lesions and calculation of bone scan index. EJNMMI Res. 2013;3:1–6.
Armstrong AJ, Kaboteh R, Carducci MA, Damber JE, Stadler WM, Hansen M, et al. Assessment of the bone scan index in a randomized placebo-controlled trial of tasquinimod in men with metastatic castration-resistant prostate cancer (mCRPC). Urol Oncol Semin Orig Invest. 2014;32:1308–16.
Reza M, Ohlsson M, Kaboteh R, Anand A, Franck-Lissbrant I, Damber J-E, et al. Bone Scan Index as an imaging biomarker in metastatic castration-resistant prostate cancer: a multicentre study based on patients treated with abiraterone acetate (Zytiga) in clinical practice. Eur Urol Focus. 2016;2:540–6.
Anand A, Morris MJ, Larson SM, Minarik D, Josefsson A, Helgstrand JT, et al. Automated Bone Scan Index as a quantitative imaging biomarker in metastatic castration-resistant prostate cancer patients being treated with enzalutamide. EJNMMI Res. 2016;6:23.
Reza M, Jones R, Aspegren J, Massard C, Mattila L, Mustonen M, et al. Bone Scan Index and progression-free survival data for progressive metastatic castration-resistant prostate cancer patients who received ODM-201 in the ARADES Multicentre Study. Eur Urol Focus. 2016;2:547–52.
Alva A, Nordquist L, Daignault S, George S, Ramos J, Albany C, et al. Clinical correlates of benefit from radium-223 therapy in metastatic castration resistant prostate cancer. Prostate. 2017;77:479–88.
Fosbøl MØ, Petersen PM, Kjaer A, Mortensen J. Radium-223 therapy of advanced metastatic castration-resistant prostate cancer: quantitative assessment of skeletal tumor burden for prognostication of clinical outcome and hematological toxicity. J Nucl Med. 2017;59:195677. jnumed.117.
Haupt F, Berding G, Namazian A, Wilke F, Böker A, Merseburger A, et al. Expert system for bone scan interpretation improves progression assessment in bone metastatic prostate cancer. Adv Ther. 2017;34:986–94.
Kothari S, Sharif-Tabrizi A, Attwood K, Lamonica DM, Levine EG, George Saby. Bone scan index at baseline as a tool for predicting hematologic toxicity in metastatic castration-resistant prostate cancer patients eligible for radium-223 treatment. J Clin Oncol. 2017;35:e16513.abstr.
Sternberg C, Armstrong A, Pili R, Ng S, Huddart R, Agarwal N, et al. Randomized, double-blind, placebo-controlled phase iii study of tasquinimod in men with metastatic castration-resistant prostate cancer. J Clin Oncol. 2016;34:2636–43.
Armstrong AJ, Anand A, Edenbrandt L, Bondesson E, Bjartell A, Widmark A, et al. Phase 3 assessment of the automated bone scan index as a prognostic imaging biomarker of overall survival in men with metastatic castration-resistant prostate cancer. JAMA Oncol. 2018;27710:1–8.
Araz M, Aras G, Küçük ÖN. The role of 18F-NaF PET/CT in metastatic bone disease. J Bone Oncol. 2015;4:92–7.
Even-Sapir E, Metser U, Mishani E, Lievshitz G, Lerman H, Leibovitch I. The detection of bone metastases in patients with high-risk prostate cancer: 99mTc-MDP Planar bone scintigraphy, single- and multi-field-of-view SPECT, 18F-fluoride PET, and 18F-fluoride PET/CT. J Nucl Med. 2006;47:287–97.
Beheshti M, Vali R, Waldenberger P, Fitz F, Nader M, Loidl W, et al. Detection of bone metastases in patients with prostate cancer by 18F fluorocholine and 18F fluoride PET-CT: a comparative study. Eur J Nucl Med Mol Imaging. 2008;35:1766–74.
Minamimoto R, Loening A, Jamali M, Barkhodari A, Mosci C, Jackson T, et al. Prospective comparison of 99mTc-MDP scintigraphy, combined 18F-NaF and 18F-FDG PET/CT, and whole-body MRI in patients with breast and prostate cancer. J Nucl Med. 2015;56:1862–8.
Harmon SA, Perk T, Lin C, Eickhoff J, Choyke PL, Dahut WL, et al. Quantitative assessment of early [18F]sodium fluoride positron emission tomography/computed tomography response to treatment in men with metastatic prostate cancer to bone. J Clin Oncol. 2017;35:2829–37.
Ryan CJ, Shah S, Efstathiou E, Smith MR, Taplin M-E, Bubley GJ, et al. Phase II study of abiraterone acetate in chemotherapy-naive metastatic castration-resistant prostate cancer displaying bone flare discordant with serologic response. Clin Cancer Res. 2011;17:4854–61.
Thomas L, Balmus C, Ahmadzadehfar H, Essler M, Strunk H, Bundschuh RA. Assessment of bone metastases in patients with prostate cancer-a comparison between 99mTc-bone-scintigraphy and [68Ga]Ga-PSMA PET/CT. Pharmaceuticals (Basel). 2017;10:pii: E68.
Rathke H, Afshar-Oromieh A, Giesel FL, Kremer C, Flechsig P, Haufe S, et al. Intra-individual comparison of Tc-99m-MDP bone scan and the PSMA-ligand Tc-99m-MIP-1427 in patients with osseous metastasized prostate cancer. J Nucl Med. 2018; 59:1373–79.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We declare the following conflicts of interest. Dr. Mota: none relevant to this manuscript. Dr. Armstrong: none relevant to this manuscript. Dr. Larson reports receiving commercial research grants from Genentech, Inc., WILEX AG, Telix Pharmaceuticals Limited, and Regeneron Pharmaceuticals, Inc.; holding ownership interest/equity in Voreyda Theranostics Inc. and Elucida Oncology Inc., and holding stock in ImaginAb, Inc. SML is the inventor and owner of issued patents both currently unlicensed and licensed by MSK to Samus Therapeutics, Inc. and Elucida Oncology, Inc. SML is or has served as a consultant to Cynvec LLC, Eli Lilly & Co., Prescient Therapeutics Limited, Advanced Innovative Partners, LLC, Gerson Lehrman Group, Progenics Pharmaceuticals, Inc., and Janssen Pharmaceuticals, Inc. Dr. Fox: None relevant to this manuscript. Dr. Morris reports unpaid consultant for Bayer, Endocyte, Progenics, Janssen; paid consultant for Oric Pharmaceuticals and Advance Acclerator Applications; research funding: Genentech/Roch, Endocyte, Bayer, Progenics, Astellas, Corcept.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mota, J.M., Armstrong, A.J., Larson, S.M. et al. Measuring the unmeasurable: automated bone scan index as a quantitative endpoint in prostate cancer clinical trials. Prostate Cancer Prostatic Dis 22, 522–530 (2019). https://doi.org/10.1038/s41391-019-0151-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-019-0151-4
This article is cited by
-
Comparison of skeletal segmentation by deep learning-based and atlas-based segmentation in prostate cancer patients
Annals of Nuclear Medicine (2022)
-
The role of MRI in prostate cancer: current and future directions
Magnetic Resonance Materials in Physics, Biology and Medicine (2022)
-
The prognostic power of 18F-FDG PET/CT extends to estimating systemic treatment response duration in metastatic castration-resistant prostate cancer (mCRPC) patients
Prostate Cancer and Prostatic Diseases (2021)
-
Prognostic value of the bone scan index in patients with metastatic castration-resistant prostate cancer: a systematic review and meta-analysis
BMC Cancer (2020)