Abstract
Background/objectives
Few studies have examined the effects of the weight status at birth and preschool age on the risk of elevated blood pressure (EBP) in early childhood, and whether the effects can be modified by breastfeeding duration remains unclear. We aimed to evaluate the effects of high birth weight (HBW) with overweight/obese or abdominal obesity on the risk of EBP in preschoolers, and further evaluate the effects classified by breastfeeding duration (<6 and ≥6 months).
Subjects/methods
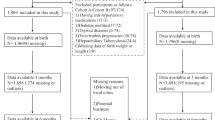
This cross-sectional study was conducted in 2018 in Zhuhai, China. Out of 2390 3–4-year-old preschoolers originally recruited, a total of 1899 were included in the analysis. Logistic regression analysis was performed to examine the effects of the weight status at the two age points and breastfeeding duration on the risk of EBP.
Results
Preschoolers with current overweight/obese had a 1.13-fold increased risk of EBP than those with persistent normal weight, irrespective of their birth weight. However, the preschoolers with HBW had no increased risk of EBP, when they became normal weight (OR 1.70, 0.78–3.72). Similar results were found for the current abdominal obesity and the risk of EBP. In addition, the EBP risk of obese status was minimized if preschoolers were breastfed for ≥6 months.
Conclusions
Obesity status at preschool age can increase the risk of EBP, irrespective of birth weight. However, this EBP risk can be mitigated if HBW changes to current normal weight. Longer breastfeeding duration can partially offset the risk of EBP in preschoolers with obesity status.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Juhola J, Magnussen CG, Berenson GS, Venn A, Burns TL, Sabin MA, et al. Combined effects of child and adult elevated blood pressure on subclinical atherosclerosis: the International Childhood Cardiovascular Cohort Consortium. Circulation. 2013;128:217–24. https://doi.org/10.1161/CIRCULATIONAHA.113.001614.
Berenson GS, Srinivasan SR, Bao W, Newman WP III, Tracy RE, Wattigney WA. Association between multiple cardiovascular risk factors and atherosclerosis in children and young adults. The Bogalusa Heart Study. N. Engl J Med. 1998;338:1650–6. https://doi.org/10.1056/NEJM199806043382302.
Dong B, Wang HJ, Wang Z, Liu JS, Ma J. Trends in blood pressure and body mass index among Chinese children and adolescents from 2005 to 2010. Am J Hypertens. 2013;26:997–1004. https://doi.org/10.1093/ajh/hpt050.
Zou ZY, Dong YH, Ma J. The endemic distribution and related factors of elevated blood pressure among Chinese children and adolescents aged 7–18 years in 2014. Chin J Prev Med. 2017;51:290–4. https://doi.org/10.3760/cma.j.issn.0253-9624.2017.04.003.
Edvardsson VO, Steinthorsdottir SD, Eliasdottir SB, Indridason OS, Palsson R. Birth weight and childhood blood pressure. Curr Hypertens Rep. 2012;14:596–602. https://doi.org/10.1007/s11906-012-0311-6.
Kuciene R, Dulskiene V, Medzioniene J. Associations between high birth weight, being large for gestational age, and high blood pressure among adolescents: a cross-sectional study. Eur J Nutr. 2018;57:373–81. https://doi.org/10.1007/s00394-016-1372-0.
Zhang Y, Li H, Liu SJ, Fu GJ, Zhao Y, Xie YJ, et al. The associations of high birth weight with blood pressure and hypertension in later life: a systematic review and meta-analysis. Hypertens Res. 2013;36:725–35. https://doi.org/10.1038/hr.2013.33.
Mu M, Wang SF, Sheng J, Zhao Y, Li HZ, Hu CL, et al. Birth weight and subsequent blood pressure: a meta-analysis. Arch Cardiovasc Dis. 2012;105:99–113. https://doi.org/10.1016/j.acvd.2011.10.006.
Li YY, Wu JQ, Yu JM, Rong F, Ren JC, Gao ES, et al. [The influence of high birth weight on the blood pressure during childhood—a cohort study]. Chin J Epidemiol. 2012;33:1213–7.
Parker ED, Sinaiko AR, Kharbanda EO, Margolis KL, Daley MF, Trower NK, et al. Change in weight status and development of hypertension. Pediatrics. 2016;137:e20151662 https://doi.org/10.1542/peds.2015-1662.
Hou Y, Wang M, Yang L, Zhao M, Yan Y, Xi B. Weight status change from childhood to early adulthood and the risk of adult hypertension. J Hypertens. 2018. https://doi.org/10.1097/HJH.0000000000002016.
Kagura J, Adair LS, Munthali RJ, Pettifor JM, Norris SA. Association between early life growth and blood pressure trajectories in black South African Children. Hypertension. 2016;68:1123–31. https://doi.org/10.1161/HYPERTENSIONAHA.116.08046.
Pluymen LPM, Wijga AH, Gehring U, Koppelman GH, Smit HA, van Rossem L. Breastfeeding and cardiometabolic markers at age 12: a population-based birth cohort study. Int J Obes. 2019;43:1568–77. https://doi.org/10.1038/s41366-018-0317-5.
Nobre LN, Lessa AD. Influence of breastfeeding in the first months of life on blood pressure levels of preschool children. J Pediatr. 2016;92:588–94. https://doi.org/10.1016/j.jped.2016.02.011.
Lawlor DA, Najman JM, Sterne J, Williams GM, Ebrahim S, Davey Smith G. Associations of parental, birth, and early life characteristics with systolic blood pressure at 5 years of age: findings from the Mater-University study of pregnancy and its outcomes. Circulation. 2004;110:2417–23. https://doi.org/10.1161/01.CIR.0000145165.80130.B5.
Zhai Y, Li WR, Shen C, Qian F, Shi XM. Prevalence and correlates of elevated blood pressure in Chinese children aged 6–13 years: a nationwide school-based survey. Biomed Environ Sci. 2015;28:401–9. https://doi.org/10.3967/bes2015.057.
Zong XN, Li H. Construction of a new growth references for China based on urban Chinese children: comparison with the WHO growth standards. PLoS ONE 2013;8:e59569. https://doi.org/10.1371/journal.pone.0059569.
Zong XN, Li H. Comparison of the China child growth standards and the WHO child growth standards from 0 to 7 years old. Chin J Child Heal Care. 2010;18:195–8.201.
Lurbe E, Agabiti-Rosei E, Cruickshank JK, Dominiczak A, Erdine S, Hirth A, et al. 2016 European Society of Hypertension guidelines for the management of high blood pressure in children and adolescents. J Hypertens. 2016;34:1887–920. https://doi.org/10.1097/HJH.0000000000001039.
Fan H, Yan YK, Mi J. Updating blood pressure reference for Chinese children aged 3-17 years. Chin J Hypertens. 2017;25:428–38.
Li H, Zong XN, Ji CY, Mi J. Body mass index cut-offs for overweight and obesity in Chinese children and adolescents aged 2–18 years. Chin J Epidemiol. 2010;31:616–20.
Freedman DS, Serdula MK, Srinivasan SR, Berenson GS. Relation of circumferences and skinfold thicknesses to lipid and insulin concentrations in children and adolescents: the Bogalusa Heart Study. Am J Clin Nutr. 1999;69:308–17. https://doi.org/10.1093/ajcn/69.2.308.
Anzo M, Inokuchi M, Matsuo N, Takayama JI, Hasegawa T. Waist circumference centiles by age and sex for Japanese children based on the 1978-1981 cross-sectional national survey data. Ann Hum Biol. 2015;42:56–61. https://doi.org/10.3109/03014460.2014.928368.
World Health Organization. Second-Hand Smoke, Women, and Children. https://www.who.int/tobacco/publications/gender/en_tfi_gender_women_second_hand_smoke_women_children.pdf-14mb. Accessed 15 Jul 2019.
Stekhoven DJ, Buhlmann P. MissForest–non-parametric missing value imputation for mixed-type data. Bioinformatics. 2012;28:112–8. https://doi.org/10.1093/bioinformatics/btr597.
Tang F, Ishwaran H. Random forest missing data algorithms. Stat Anal Data Min. 2017;10:363–77. https://doi.org/10.1002/sam.11348.
Lumley T, Diehr P, Emerson S, Chen L. The importance of the normality assumption in large public health data sets. Annu Rev Public Health. 2002;23:151–69. https://doi.org/10.1146/annurev.publhealth.23.100901.140546.
Dong YH, Zou ZY, Yang ZP, Wang ZH, Jing J, Luo JY, et al. Association between high birth weight and hypertension in children and adolescents: a cross-sectional study in China. J Hum Hypertens. 2017;31:737–43. https://doi.org/10.1038/jhh.2017.22.
Mamun AA, Lawlor DA, O’Callaghan MJ, Williams GM, Najman JM. Effect of body mass index changes between ages 5 and 14 on blood pressure at age 14: findings from a birth cohort study. Hypertension. 2005;45:1083–7. https://doi.org/10.1161/01.HYP.0000166720.18319.51.
Ortiz-Pinto MA, Ortiz-Marron H, Ferriz-Vidal I, Martinez-Rubio MV, Esteban-Vasallo M, Ordobas-Gavin M et al. Association between general and central adiposity and development of hypertension in early childhood. Eur J Prev Cardiol. 2019; 2047487319839264. https://doi.org/10.1177/2047487319839264.
Forsyth JS, Willatts P, Agostoni C, Bissenden J, Casaer P, Boehm G. Long chain polyunsaturated fatty acid supplementation in infant formula and blood pressure in later childhood: follow up of a randomised controlled trial. BMJ. 2003;326:953 https://doi.org/10.1136/bmj.326.7396.953.
Marlin DW, Picciano MF, Livant EC. Infant feeding practices. J Am Diet Assoc. 1980;77:668–76.
Havas S, Roccella EJ, Lenfant C. Reducing the public health burden from elevated blood pressure levels in the United States by lowering intake of dietary sodium. Am J Public Health. 2004;94:19–22.
World Health Organization. UNICEF (2003) Global Strategy for Infant and Young Child Feeding. https://apps.who.int/iris/bitstream/handle/10665/42590/9241562218.pdf. Accessed 15 July 2019.
Duan Y, Yang Z, Lai J, Yu D, Chang S, Pang X et al. Exclusive breastfeeding rate and complementary feeding indicators in China: a national representative survey in 2013. Nutrients. 2018;10. https://doi.org/10.3390/nu10020249.
Schroder H, Ribas L, Koebnick C, Funtikova A, Gomez SF, Fito M, et al. Prevalence of abdominal obesity in Spanish children and adolescents. Do we need waist circumference measurements in pediatric practice? PLoS ONE 2014;9:e87549 https://doi.org/10.1371/journal.pone.0087549.
Wicklow BA, Becker A, Chateau D, Palmer K, Kozyrskij A, Sellers EA. Comparison of anthropometric measurements in children to predict metabolic syndrome in adolescence: analysis of prospective cohort data. Int J Obes. 2015;39:1070–8. https://doi.org/10.1038/ijo.2015.55.
Gillespie B, d’Arcy H, Schwartz K, Bobo JK, Foxman B. Recall of age of weaning and other breastfeeding variables. Int Breastfeed J. 2006;1:4. https://doi.org/10.1186/1746-4358-1-4.
Li R, Scanlon KS, Serdula MK. The validity and reliability of maternal recall of breastfeeding practice. Nutr Rev 2005;63:103–10. https://doi.org/10.1111/j.1753-4887.2005.tb00128.x.
Acknowledgements
We extend our sincere thanks to the healthcare staff from the Maternal and Child Health Center and the Community Health Service Centers in Zhuhai city that provided support in the project through data collection and services on the front lines. We also greatly appreciate the families who have been willing to be involved in this research project.
Funding
Source of funding: This study was supported by the Natural Science Foundation of China (Grant No. 81673182) and the Fundamental Research Funds for the Central Universities, HUST (Grant No. 2016YZXD041).
Author information
Authors and Affiliations
Contributions
JZ and WM designed the project; JZ, JS, LW, YZ, CL, YW, and WM conducted data collection; JS analyzed data or performed statistical analysis; JS wrote the paper; JZ and WM had primary responsibility for the final content. All authors read and approved the final paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sun, J., Wu, L., Zhang, Y. et al. Association of breastfeeding duration, birth weight, and current weight status with the risk of elevated blood pressure in preschoolers. Eur J Clin Nutr 74, 1325–1333 (2020). https://doi.org/10.1038/s41430-020-0608-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-020-0608-5