Key Points
-
Awareness of dental therapists and their permitted duties in the UK is low.
-
Nearly two thirds of participants accepted the possibility of receiving fillings from therapists.
-
Fewer people were willing for their children to receive treatment from therapists.
-
Public education and reassurance is needed on the training and permitted duties of therapists and the rationale for skill-mix in dentistry.
Abstract
Objectives To investigate public awareness and the social acceptability of dental treatment provided by dental therapists in the UK.
Method A telephone survey of a representative quota sample of 1,000 UK adults.
Results 10.4% of participants were aware of dental therapists as a professional group, of whom none correctly identified their permitted duties. 61.3% were willing to receive simple restorative treatment from a therapist, with acceptability predicted by being male [OR 1.44 (95% CI 1.09-1.90)], being younger [OR 1.024 (1.016-1.032)] and having a perceived need for treatment [OR 1.49 (1.09-2.5)]. Fewer were willing to allow a therapist to restore a child's tooth (54.7%, p <0.001, McNemar's test) with acceptability predicted by being younger [OR 1.026 (1.018-1.034)]. Those receiving some private treatment were less likely to report acceptability of simple restorative treatment for themselves [OR 0.61 (0.46-0.81)] or for children [OR 0.54 (0.41-0.72)]. 48.2% of participants expected to pay less for treatment provided by therapists, with acceptability of equal costs predicted by the participant being male [OR 1.81 (1.50-2.40)].
Conclusion These findings identify a need for education and reassurance of the public on the training and permitted duties of dental therapists and the rationale for skill-mix in dentistry.
Similar content being viewed by others
Introduction
The use of skill-mix in dentistry, where different dental team members employ different skills, is now well established in the UK and elsewhere.1 Although the extent to which it is used varies internationally, the rationale for using skill-mix focuses on the potential for increasing access and efficiency of services.2,3,4,5,6,7 In the UK it has been estimated that 70% of all visits and 60% of all clinical time in primary care could be provided by dental therapists.8
This model of care has been given increasing prominence over the last two decades in the UK following positive published reports.9,10 Subsequent legislative changes permitted dual-trained dental hygienists and therapists (referred to as dental therapists in this paper) to work in all sectors of dentistry11 and the number of training places for dental therapists has increased significantly. Recently the General Dental Council (GDC) has defined the permitted duties of all members of the dental team. As well as describing the core treatments and procedures each professional group may conduct under the prescription of a dentist, a wide range of additional treatments that appropriately trained dental care professionals (DCPs) may perform was identified.12 Such skills potentially extend the list of permitted duties for each type of DCP.
Sequential UK studies indicate increasing acceptance by dentists of the use of skill-mix,13,14,15 although there is still ignorance of dental team members' roles.14,15 However, the views of patients and public are missing from any consideration of potential changes in service provision. US data suggest patient satisfaction with care provided by DCPs,16,17,18,19 however these cannot necessarily be generalised to the UK. Indeed, the acceptability of care provided by DCPs has been identified as a priority for research.20 Furthermore, little is known of the public awareness of dental therapists and their roles. This is particularly important now given recent recommendations to increase the use of skill-mix.21
The term 'acceptability' is often used synonymously with 'satisfaction'. However, the acceptability of a service or professional group should be conceptualised more broadly. People can only express satisfaction with a service or professional when they have experienced care. However, the views of people who have not experienced care become crucial if the use of a professional group is to be expanded. For example, healthcare quality assurance requires a service's social acceptability and legitimacy be considered as a key part of service quality assessment.22,23 Similarly, the psychology literature refers to the importance of assessing the social validity of healthcare interventions where the social acceptability of the goals, procedures and outcomes of treatment is assessed.24,25,26 Conceptually this can be applied to services or professional groups such as DCPs. In both, the views of those who have and have not experienced care should be sought.
A preliminary study of the social acceptability of skill-mix in South Yorkshire reported low levels of awareness of dental therapists as a professional group and of their permitted duties. Although the acceptability of some procedures was relatively high, more invasive procedures and those provided for children were regarded as less acceptable.27 In addition, qualitative data suggested a possible association between dental anxiety and lower levels of acceptability of skill-mix.28 However, nothing is known of the prevalence of these views at a national level. Therefore the aim of this study was to investigate public awareness and social acceptability of the use of dental therapists in the UK.
Method
A telephone survey was undertaken by a market research company (GfkNOP) using structured interviews on a representative quota sample (n = 1,000) of UK adults (18 years and over). Precision estimates were undertaken to calculate the desired sample size. These were based on data from the earlier study27 which identified that 15% of participants were aware of dental therapists as a professional group. A sample of 1,000 was selected to provide a 95% confidence interval that a population proportion of 15% would provide estimates ± 2.2%. This level of precision was regarded as sufficient for the study.
The content of the questionnaire was informed by a review of the literature, anecdotal reports and data from qualitative interviews.27,28 Areas of inquiry included the following explanatory variables: participants' age, sex, socio-economic29 and educational status; dental attendance patterns and access to care; perceived treatment need; and levels of dental anxiety (assessed by the Modified Dental Anxiety Scale).30 The outcome variables included awareness and knowledge of dental therapists and their permitted duties, acceptability of treatment provided by therapists for adults and children, and expectations of cost of treatment. Only closed questions were used. The questionnaire was piloted with 20 volunteers in face-to-face interviews and the market research company undertook further telephone piloting before commencement. Minimal modifications were requested.
Potential participants were then telephoned out of normal working hours (5.30pm-9.00pm) by random dialling in postcodes to obtain a quota sample that was representative of the Office for National Statistics mid-2005 population estimates for the UK.31 The sample was weighted to ensure appropriate proportional representation of England, Scotland, Wales and Northern Ireland. To achieve a quota sample of 1,000 UK adults, 6,937 unique telephone numbers were called. Of the numbers called, 1,704 were called back as they were either busy or engaged (n = 466) or the participant requested the interview take place at a different time (n = 1,238). Only 91 calls resulted in no contact being made (due to wrong numbers, no answer after a number of call attempts, or the number being out of service). Of those contacted, 5,828 declined to participate and a further 18 stopped the interview.
The subject matter, purpose and likely duration of the survey were explained. Potential participants were informed that they could decline involvement in the survey at any stage during or after the interview. Having been asked the questions about demographic data and the duties of a dental therapist, all participants were provided basic information about therapists indicating that they were professionally trained to undertake certain tasks once a dentist had examined the patient and prescribed particular treatments. All interviews took less than ten minutes to complete.
The analytical strategy aimed to identify putative associations between explanatory variables and the five outcome variables. Data were analysed in two phases. Initially descriptive and appropriate bivariate analyses (chi-square and McNemar tests) were undertaken to describe and compare key descriptor variables. The second phase identified explanatory variables that predicted the main outcome variables. As the key difference between dental hygienists' and dental therapists' competencies is the provision of simple restorative care, willingness to have simple fillings performed by a therapist was used as an outcome measure of the acceptability of care provided by them. Bivariate analyses (chi-square tests) of the possible predictors of the acceptability of providing this treatment were used to pre-select variables for forward stepwise logistic regression models. All variables with a relationship of p <0.2 were entered into the models. All analyses were performed using SPSS version 15 and alpha level was set to 0.05.
Ethical approval for the study was granted by the University of Sheffield, UK.
Results
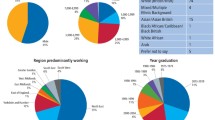
Of the 1,000 participants, 486 (48.6%) were male. Their mean age was 47.0 years and 28.7% had a child under 16 years of age. Seventy-one percent attended regularly for check-ups and 28.3% perceived they had treatment need. Of those reporting difficulty with access to a dentist (10.1%), 70.4% cited a lack of local availability of a National Health Service (NHS) dentist as the cause.
Overall, 10.4% of participants said they were aware of dental therapists as a professional group. Unsurprisingly, participants with relatives or friends who had worked in a dental team were more aware of dental therapists (42% v 13%, p <0.001, McNemar's test). No other variable predicted awareness.
Of those that had heard of a therapist (n = 104), only 38 (36.5%) thought that therapists were able to extract deciduous teeth and 69.2% that they could administer local anaesthetic (Table 1). No participant correctly predicted all the permitted duties of dental therapists.
Having received information on the role of therapists and their training, 61.3% of participants would be happy to receive simple restorative treatment but 20.4% would not be happy to receive any treatment from them (Table 2).
Overall, participants regarded dental therapists providing care for children as less acceptable (Table 3). Fewer participants regarded dental therapists providing fillings (54.7% v 61.3%, p <0.001, McNemar's test) and administering local anaesthetic (58.1 v 68.5%, p <0.001, McNemar's test) for children as acceptable than they did for themselves. More than half of participants found dental therapists extracting deciduous teeth to be unacceptable (Table 3).
Thirty-nine percent of participants expected to pay the same for treatment provided by dental therapists but 48.2% would expect to pay less.
Significant predictors of the acceptability of care provided by dental therapists and its cost are reported in Table 4. Male participants, younger participants and those with perceived treatment need were more likely to find having their tooth restored by a therapist acceptable. Younger participants were more likely to report a therapist restoring a child's tooth acceptable. Those receiving some private treatment were more likely to find treatment provided by dental therapists unacceptable for themselves and for children. Men were more likely to accept paying the same (rather than less) for care provided by a therapist. Although levels of acceptability varied in different socioeconomic groups, chi-square test for trends did not identify a clear association.
Discussion
The aim of this study was to investigate public awareness and social acceptability of the use of dental therapists in the UK. It found low levels of awareness of therapists as a professional group and of their permitted duties. Although more than half of participants accepted the prospect of being treated by therapists, significantly fewer were willing for them to treat children.
The low level of awareness of dental therapists reported here is similar to the findings of the South Yorkshire study.27,28 Before 2002, therapists were employed primarily in the salaried dental services. Consequently, despite the recent step change in the number of training places, it is unlikely that participants would have encountered them and this may explain the limited awareness. Indeed, no participant correctly identified all of their permitted duties. The findings of this and the South Yorkshire study suggest that participants were confusing dental therapists with dental hygienists.
Our earlier qualitative study also suggested that procedures perceived as more invasive were regarded as less acceptable when performed by DCPs, where more emphasis was placed on the importance of qualifications, familiarity and trust in the clinician performing the task.28 The proportions of participants in this study willing to accept local anaesthesia and simple restorative treatment were consistent with the South Yorkshire data27 (61.3% v 57.0% and 68.5% v 64.0%, respectively). However, the proportion of participants not willing to have any treatment provided by a therapist differed (20.4% v 7.0% respectively).
Younger participants were happier to receive treatment from dental therapists and for them to treat a child. The odds ratios (Table 4) indicate that approximately 2.6% more people found treatment provided by dental therapists for adults or children unacceptable for every year of life. Although high levels of satisfaction have been reported with skill-mix in general healthcare,32,33,34,35,36 some older patients have expressed a preference for seeing the doctor in particular circumstances.34 Lower acceptance of skill-mix in older age groups must be a consideration when delegating care.
The earlier qualitative study had suggested that lower levels of acceptability of skill-mix might be observed in the more dentally anxious.28 As previous studies have identified that those who do not access dental services are often dentally anxious,37,38,39 such an association would limit the use of skill-mix in increasing access to care. No association between dental anxiety and acceptability was found in this dataset.
Logistic regression identified that perceived need for treatment predicted acceptability of receiving dental therapy treatment (Table 4). Bivariate analyses had suggested that irregular attendance and perceived need were associated with acceptability, but lack of access to care was not, suggesting some confounding with irregular attendance. Taken together, these findings are encouraging if skill-mix is to be used in areas where access to dental services is poor and perceived needs are high.
The survey participants perceived that dental therapists providing treatment for children was less acceptable than for adults. This finding is consistent with the preliminary study,27,28 although levels of acceptability were slightly higher nationally. Almost half of participants would not want dental therapists to provide restorative care, administer local anaesthetic or extract a child's deciduous tooth. Given that dental therapists are often employed to treat children and adolescents in the UK and elsewhere,40,41 this finding is important. Our qualitative data suggest that more negative views about dental therapists treating children were related to assumptions of inexperience and questionable technical competence. However, positive experiences of being treated by therapists could modify views.28 Those within the dental profession opposed to the use of dental therapists have expressed concerns about DCPs treating children.42,43 If skill-mix is to be used to increase access to care for children, it is important that these views are considered. Reassurances about dental therapists' training, qualifications, regulation by the General Dental Council, competence and supervision requirements need to be carefully communicated, emphasising that the quality of care received should be at least as good as that provided by a dentist. Similarly, care in the communication of the rationale for the use of skill-mix is required. Significantly, both this study and the preliminary study found that younger participants were more likely to find dental therapists treating children as acceptable, which is encouraging if skill-mix is to be used more in the future, especially as older adults are less likely to have children.
Interestingly, those who received some private dental treatment were less likely to accept dental therapists. These findings converge with our qualitative data,28 which suggested a spectrum of views being held on the nature of dental services, ranging from a private service view of dentistry to a public service view. Those with a public service view tended to be more positive about skill-mix, seeing the potential for the efficient use of resources in an NHS service. Conversely, those with a private service view often took the standpoint of a consumer, preferring to be treated by a dentist if the cost for treatment would be unaltered. Such findings have profound implications for the employment of therapists in the treatment of adults and children if the proportion of care delivered on private contract continues to increase, but also in the NHS where charges relate to the treatment required rather than the dental team member providing care.
Such consumerist concerns have been expressed elsewhere in the belief that the use of dental therapists would lead to a two-tier dental service, where treatment by dentists is reserved for those that can afford it.43 Our earlier qualitative study28 suggested that dental and medical services are perceived differently – those with a public service view of medical services often held more consumerist views of NHS dentistry owing to the patient charges levied for treatment and some welcomed the introduction of a scale of fees relating to the clinician providing care. This study has identified that more participants would expect to pay less for treatment from therapists than those who would expect to pay the same. A similar finding was reported in the South Yorkshire study.
Evaluation of health services increasingly emphasises the importance of user views,22,23,44,45,46 the most contemporary of which go beyond evaluating patient satisfaction with services experienced. The concepts of social acceptability22 and social validity24 require a broader assessment of the social desirability and appropriateness of a service and its outcomes. The findings of this study, consistent with the earlier study, raise questions about the current social acceptability of the use of dental therapists in the UK. They have identified that awareness of dental therapists as a professional group and their permitted duties is low. Therefore, it is doubtful whether many would be able to give informed consent for treatment provided by therapists should perceptions remain unchanged. There is a role for both the Government and the profession to communicate the rationale for using skill-mix in terms of increasing efficiency and access while maintaining its effectiveness and thus improving the service's quality overall.23 Our qualitative data suggested that once the rationale for skill-mix is explained, views on the use of dental therapists were modified.28 Similar arguments could also be used by dentists solely working in the private sector, if efficiency improvements are reflected in patient charges to patients.28 Research into the potential for the use of skill-mix in private care would also be beneficial.
Telephone surveys have been used in national dental surveys47 and are frequently used in health and social surveys, particularly in North America.48,49,50 Although every effort was made by the market research company to achieve a representative sample, like all surveys, a risk of sampling bias exists which tends to result in an overrepresentation of the views of white participants of higher income and educational attainment.51 This telephone survey reported 26.6% of participants as having perceived need for treatment, which is similar to the proportion (25.4%) reporting perceived need in a recent large-scale postal survey of adults (n = 10,864),37 suggesting that the impact of any sampling and response bias was similar in both.
This study and the earlier preliminary study have identified a number of areas for future inquiry. Further research is needed into the broader aspects of the quality of services provided by dental therapists in terms of their efficiency, effectiveness, their impact on equity and accessibility and their acceptability.22,23 Research into their acceptability should include an investigation into the views of patients, parents/guardians and children on the experiential acceptability of care provided by dental therapists. The theoretical and methodological difficulties of such research are well documented52,53 and mixed-method approaches have been recommended.54,55 Given the increasing proportion of provision of dental services in the private sector, models of how skill-mix can be best employed in both NHS and private practice should be explored and how the delegation of care is best undertaken and communicated in both should be investigated.
Conclusion
This study confirmed that the awareness of dental therapists and their permitted duties was low across the UK. More than half of participants accepted the prospect of treatment provided by dental therapists; significantly fewer were willing for them to treat children. A fifth of participants would not be willing to receive any treatment from a therapist. Common predictors of acceptability were being younger and if the participant had a perceived need for treatment. More participants expected to pay less for treatment provided by dental therapists than those who expected equal costs. Such factors need to be considered, as skill-mix is to be increasingly used in the delivery of dental services.
References
FDI World Dental Federation. Facts and figures web resource. http://www.fdiworldental.org/resources/3_0facts.html (accessed 12 December 2008).
World Health Organization. Report of an expert committee on auxiliary dental personnel. Tech. Rep. Series No. 163. Geneva: WHO, 1959.
Department of Health. Modernising NHS dentistry - implementing the plan. London: The Stationery Office, 2000.
Department of Health. NHS dentistry: options for change. London: The Stationery Office, 2002.
Spencer J. Narrowing the inequality gap in oral health and dental care in Australia. Sydney, Australia: Australian Health Policy Institute, University of Sydney, 2004.
Khan A A. Oral health services in developing countries: a case for the primary health care approach. Developing Dentistry 2004; 5(2): 1–2.
New Zealand Ministry of Health. Implementing the New Zealand Health Strategy 2005: the Minister of Health's fifth report on progress on the New Zealand Health Strategy, and the second report on actions to improve quality. Wellington, New Zealand: Ministry of Health, 2005.
Evans C, Chestnutt, I G, Chadwick B L. The potential for delegation of clinical care in general dental practice. Br Dent J 2007; 203: 695–699.
Nuffield Foundation. Education and training of personnel auxiliary to dentistry. London: Nuffield Foundation, 1993.
General Dental Council. Report of the Dental Auxiliaries Review Group. London: General Dental Council 1998.
United Kingdom Parliament. Statutory Instrument 2002 No. 1671. The Dental Auxiliaries (Amendment) Regulations 2002. London: HMSO, 2002.
General Dental Council. Scope of practice. London: General Dental Council, 2009.
Gallagher J L, Wright D A. General dental practitioners' knowledge of and attitudes towards the employment of dental therapists in general practice. Br Dent J 2003; 194: 37–41.
Dyer T A, Robinson P G. General health promotion in general dental practice - the involvement of the dental team. Part 2: a qualitative and quantitative investigation of the views of practice principals in South Yorkshire. Br Dent J 2006; 201: 45–51.
Ross M K, Ibbetson R J, Turner S. The acceptability of dually-qualified dental hygienist-therapists to general dental practitioners in South-East Scotland. Br Dent J 2007; 202: E8.
Chaffin J G, Chaffin S D, Mangelsdorff A D, Finstren K. Patient satisfaction with dental hygiene providers in US military clinics. J Dent Hygiene 2007; 81: 9.
Lotzkar S, Johnson D W, Thompson M B. Experimental program in expanded functions for dental assistants: phase 1 base line and phase 2 training. J Am Dent Assoc 1971; 82: 101–122.
Lotzkar S, Johnson D W, Thompson M B. Experimental program in expanded functions for dental assistants: phase 3 experiment with dental teams. J Am Dent Assoc 1971; 82: 1067–1081.
Sisty N L, Henderson W G. A comparative study of patient evaluations of dental treatment performed by dental and expanded-function dental hygiene students. J Am Dent Assoc 1974; 88: 985–996.
Galloway J, Gorham J, Lambert M, Richards D, Russell D, Welshman J. The professionals complementary to dentistry: a systematic review and synthesis. London: UCL Eastman Dental Hospital Dental Team Studies Unit, 2003.
Department of Health. NHS dental services in England: an independent review led by Professor Jimmy Steele. London: Department of Health, 2009. http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_101137 (accessed 25 November 2009).
Donabedian A. An introduction to quality assurance in healthcare. Oxford: Oxford University Press, 2003.
Maxwell R J. Quality assessment in health. Br Med J (Clin Res Ed) 1984; 288: 1470–1472.
Wolf M M. Social validity, the case for subjective measurement of how applied behaviour analysis is finding its heart. J Appl Behav Anal 1978; 11: 203–214.
Finney J W. On further development of the concept of social validity. J Appl Behav Anal 1991; 24: 245–249.
Foster S L, Mash E J. Assessing the social validity in clinical treatment research: issues and procedures. J Consult Clin Psychol 1999; 67: 309–319.
Dyer T A, Robinson P G. Public awareness and social acceptability of dental therapists. Int J Dent Hyg 2009; 7: 108–114.
Dyer T A, Robinson P G. Exploring the social acceptability of skill-mix in dentistry. Int Dent J 2008; 58: 173–180.
Market Research Society. Occupation groupings: a job dictionary. 6th ed. London: Market Research Society, 2006.
Humphris G M, Morrison T, Lindsay S J. The Modified Dental Anxiety Scale: validation and United Kingdom norms. Community Dent Health 1995; 12: 44–50.
Office for National Statistics. National Statistics online. Population mid year estimates 2005. http://www.statistics.gov.uk/statbase/Product.asp?vlnk=14204 (accessed 25 November 2009).
Spitzer W O, Sackett D L, Sibley J C et al. The Burlington randomized trial of the nurse practitioner. N Engl J Med 1974; 290: 251–256.
Mundinger M O, Kane R L, Lenz E R et al. Primary care outcomes in patients treated by nurse practitioners or physicians: a randomized trial. JAMA 2000; 280: 59–68.
Roblin D W, Becker E R, Adams E K, Howard D H, Roberts M H. Patient satisfaction with primary care: does type of practitioner matter? Med Care 2004; 42: 579–590.
Horrocks S, Anderson E, Salisbury C. Systematic review of whether nurse practitioners working in primary care can provide equivalent care to doctors. BMJ 2002; 324: 819–823.
Laurant M, Reeves D, Hermens R, Braspenning J, Grol R, Sibbald B. Substitution of doctors by nurses in primary care. Cochrane Database Syst Rev 2005; (2): CD001271.
Wyborn C, Marshman Z, Dyer T A, Beal J, Godson J. The dental health of adults in Yorkshire and Humber 2008. York: Yorkshire and Humber Public Health Observatory, 2009.
Finch H, Keegan J, Ward K, Sanyal S B. Barriers to the receipt of dental care. London: British Dental Association, 1988.
Kelly M, Steele J, Nuttall N et al. Adult dental health survey - oral health of adults in the United Kingdom 1998. London: The Stationery Office, 2000.
Teusner D N, Spencer A J. Dental labour force, Australia 2000. AIHW cat. no. DEN 116. Canberra: Australian Institute of Health and Welfare, 2000. (Dental Statistics and Research Series No. 28).
New Zealand Ministry of Health. School dental service facilities discussion document. Wellington: Ministry of Health, 2003.
Burt B A, Eklund S A. Dentistry, dental practice and the community. 6th ed. pp 111–127. Philadelphia: WB Saunders Company, 2006.
Bramson J B, Guay A H. Comments on the proposed pediatric oral health therapist. J Public Health Dent 2005; 65: 123–127.
Department of Health. Standards for better health. London: Department of Health, 2004.
Arah O A, Westert G P, Hurst J, Klazinga N S. A conceptual framework for the OECD Health Care Quality Indicators Project. Int J Qual Health Care 2006; 18 (Suppl 1): 5–13.
Department of Health. High quality care for all. London: Department of Health, 2008.
AIHW Dental Statistics and Research Unit. Oral health and access to dental care – the gap between the “deprived” and the “priveleged” in Australia. Canberra: Australian Institute of Health and Welfare, 2001.
Simon T R, Mercy J A, Barker L. Can we talk? Importance of random-digit-dial surveys for injury prevention research. Am J Prev Med 2006; 31: 406–410.
Link M W, Kresnow M-J. The future of random-digit-dial surveys for injury prevention and violence research. Am J Prev Med 2006; 31: 444–450.
Statistics Canada. General social survey – access to and use of information communication technology (GSS). Detailed information for 2000 (Cycle 14). http://www.statcan.gc.ca/cgi-bin/imdb/p2SV.pl?Function=getSurvey&SDDS=4505&lang=en&db=imdb&adm=8&dis=2 (accessed 25 November 2009).
Link M W, Battaglia M P, Frankel M R, Osborn L, Mokdad A H. A comparison of address-based sampling (ABS) versus random-digit dialing (RDD) for general population surveys. Public Opin Q 2008; 72: 6–27.
Locker D, Dunt D. Theoretical and methodological issues in sociological studies of consumer satisfaction with medical care. Soc Sci Med 1978; 12: 283–292.
Calnan M. Towards a conceptual framework of lay evaluation of health care. Soc Sci Med 1988; 27: 927–933.
Sitzia J, Wood N. Patient satisfaction: a review of issues and concepts. Soc Sci Med 1997; 45: 1829–1843.
Schneider H, Palmer N. Getting to the truth? Researching user views of primary health care. Health Policy Plan 2002; 17: 32–41.
Acknowledgements
The authors would like to thank Irene Quoico of GfkNOP and Dr Sarah Baker for her support with the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed paper
Rights and permissions
About this article
Cite this article
Dyer, T., Humphris, G. & Robinson, P. Public awareness and social acceptability of dental therapists. Br Dent J 208, E2 (2010). https://doi.org/10.1038/sj.bdj.2010.1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2010.1
This article is cited by
-
The perceptions and attitudes of qualified dental therapists towards a diagnostic role in the provision of paediatric dental care
British Dental Journal (2022)
-
Perceptions of dental therapists within dental schools: a brief exploration
BDJ Team (2021)
-
Assessing the efficacy and social acceptability of using hygienist-therapists as front-line clinicians
BDJ Team (2017)
-
Feasibility study: assessing the efficacy and social acceptability of using dental hygienist-therapists as front-line clinicians
British Dental Journal (2016)
-
Alternative scenarios: harnessing mid-level providers and evidence-based practice in primary dental care in England through operational research
Human Resources for Health (2015)